Adolescent Mental Health Care: Time for Revolution
Stefano Marini1*, Lucia D'Agostino1, Carla Ciamarra1, Roberto De Lena2, Mara Giacomodonato2,3, Maddalena Molinero2, Lucia Corsi3, Alessandro Gentile1 and Tiziano Acciavatti4
1National Health System, Department of Mental Health, Termoli, Italy
2Cooperativa Progetto Popolare, Montescaglioso, Italy
3Cooperativa Sociale DiversaMente, Larino, Italy
4National Health Service, Department of Mental Health, Pescara, Italy
Submission: January 19, 2024; Published: February 06, 2024
*Corresponding author: Stefano Marini, National Health Service, Department of Mental Health, Termoli, Italy, Email ID: JOJ Case, Email: sfnmarini@gmail.com
How to cite this article: Stefano M, Lucia D, Carla C, Roberto De L, Mara G, et al. Adolescent Mental Health Care: Time for Revolution. JOJ Case Stud. 2024; 14(4): 555893. DOI: 10.19080/JOJCS.2023.14.555891.
Abstract
Compared to the mental health of adults, the mental health of young people is often disproportionately affected by disasters. The transitional phase from adolescence into young adulthood represents a window of opportunity to prevent new onset and to improve the outcomes of mental disorders. To a worldwide estimate, in the year 2020 between 10-20% of adolescents would have suffered from mental health problems for the first time. The main aim of this paper is to critically review the unmet needs necessary for developing integrated mental health services for adolescents and young people and to provide recommendations to be implemented in mental health services after the COVID-19 pandemic. The COVID-19 pandemic has been a global disaster that has affected the lives of adolescents and their families on multiple levels. Adolescents must receive the physical and mental care they need to develop, grow and enjoy a satisfying quality of life. Furthermore, both vertical, horizontal and longitudinal integration should be promoted.
Keywords: Youth mental health; Innovation; Mental health services; Integrated care; Multidisciplinary
Introduction
The COVID-19 pandemic has been a global disaster that has affected the lives of adolescents and their families on multiple levels. While physical health is understandably the priority during a pandemic, the impact of the COVID-19 pandemic and resulting measures on mental health has also been a major concern [1]. Indeed, the scientific literature provides clear evidence of the psychological and psychiatric impact that general health conditions have had on the general population [2,3].
Since the beginning of the COVID-19 epidemic, researchers around the world have focused more on the impact on mental health in the children and adult population, while, in our opinion, little attention has been paid to the effects of COVID-19 on adolescent mental health.
Adolescence usually includes people aged between 10 and 19 years [4], while people from 19 to 25 years old are considered young adulthood [5].
Adolescence has often been labeled by developmental theorists as a time of storm and stress [6] both due to physical and chemical changes [7] and the regulatory system still largely underdeveloped until early adulthood [8]. Another distinctive feature of adolescence is the marked increase in social sensitivity and the importance of peers [9]. These essential characteristics of adolescence have been severely threatened by the pandemic. Indeed, Gruber et al. [1] conceptualized the COVID-19 pandemic as a multidimensional stressor [1].
Furthermore, adolescence is a developmental stage in which many psychological symptoms increase in prevalence and numerous psychological problems may emerge for the first time [10].
On the other hand, adolescence, with its ongoing changes in behavioral functions and underlying neural circuits represents a "window of opportunity" to carry out early interventions in the prevention of the development of psychopathologies [11].
It is important to highlight that possible psychopathological alterations are not equally likely in all adolescents. Disasters tend to amplify pre-existing social (education, income, access to healthcare, access to other support services including psychological support) and personal (aspects relating to resilience) inequalities, resulting in an unequal impact on young people [12,13].
If we take into consideration that approximately a quarter of the world's population is represented by adolescents [14] and that about 75% of mental disorders begin before the age of 25 [15], the mental health of adolescents becomes an aspect of primary global importance.
Moreover, developing a serious mental disorder at a crucial time in life is an important predictor of persistent negative socioeconomic and health outcomes, such as economic disengagement, unemployment, low income, welfare dependency, low education and illness [16-18].
However, available evidence suggests that relatively mild mental disorders that develop during adolescence often do not persist into early adulthood [19]. Therefore, youth-focused interventions designed to reduce the risk of symptom onset or prevent progression from relatively mild mental health problems to more serious mental health problems can have a significant impact on long-term economic, educational and health outcomes.
Although past literature reported a growing trend of psychopathological aspects in adolescents before 2019 [20,21], according to the global estimate, in the year 2020 between 10-20% of adolescents would have suffered from mental health problems [22]. Numerous studies have established an association between the COVID-19 pandemic and rates of anxiety [23-27]. Other research has identified a high association between the pandemic and depression [28-31]. The study conducted by Duan et al. [24] identified an association between depression and social media use, such as smartphone addiction and Internet addiction. Guo et al. [32] identified an association between COVID-19-related stress and depression.
Surveys of young people's use of psychoactive substances report an initial decrease in alcohol and drug use, perhaps partly due to fewer opportunities for social use [33]. Other studies suggest that frequent and problematic substance use during the pandemic has increased in some high-risk youth, such as those with comorbid psychopathology [34-37].
Studies on suicide risk and/or attempted suicide have reported no increased rates of death by suicide [38,39]. Regarding emergency room visits for suicide attempts, the data are conflicting. One study reported a decrease in hospital attendance for self-harm behavior in the early months of the pandemic [40], while others reported small increases in suicidal ideation and suicide attempts among young people presenting to children's hospitals [41] and those admitted for a psychiatric condition [42].
During the COVID-19 pandemic, adolescents with a previous diagnosis of anorexia nervosa reported a 70% increase in poor eating habits and an increase in thoughts associated with eating disorders [43]. Furthermore, an unprecedented increase in the number of hospitalizations for restrictive eating disorders has been reported [44,45].
Pre-pandemic maltreated adolescents experienced higher rates of post-traumatic stress disorder (PTSD) and higher rates of anxiety [31]. The study [46] which evaluated various groups of young people, including adolescents diagnosed with OCD, established a worsening of symptoms (44.6%). Adolescents suffering from conduct disorders and Attention-deficit/hyperactivity disorder (ADHD) presented an increase in externalizing symptoms [47]. Furthermore, observed increases in externalizing symptoms were highly associated with lower levels of socialization and parental and peer support [48].
Regarding gender, studies have established higher rates of COVID-19-related anxiety among women [29,49].
Few studies have been conducted on marginalized groups [50] and adolescents with neurodevelopmental disorders such as autism, intellectual disability and ADHD [51].
For the mental well-being of adolescents, it appears important to also consider the effects that the restrictive measures linked to the pandemic have had on young people's family relationships. Some studies highlight the worsening of intra-family conflicts between parents and adolescent children in different ways at different times of the lockdown [52,53]. Other evidence suggests that spending more time with family during the pandemic was a protective factor for young people's mental health while spending more time online and more time connected virtually with friends were positively associated with depression [28].
The effect of the pandemic and the resulting restrictive measures on the use of social media by young people is important but still unclear. Although pre-pandemic literature has established a link between adolescents' excessive use of social media and poorer psychological well-being, such as depressive symptoms [54], risky behaviors [55], and body image disturbances [56], studies carried out during the pandemic led to ambiguous results [57].
Furthermore, recent reviews classified risk and protective factors for the mental health effects of the COVID-19 pandemic [58-60].
The main aim of this paper is to critically review the unmet needs necessary for developing integrated mental health services for adolescents and young people and to provide recommendations to be implemented in mental health services.
Materials and Methods
A literature search was conducted on major databases to find useful studies for the purposes of this paper.
Discussion
The effects of the COVID-19 pandemic on adolescent well-being have reinforced the importance of putting systems in place to support adolescent well-being. The Partnership for Maternal, Newborn & Child Health, and the World Health Organization (WHO) in collaboration with the United Nations H6+Technical Working Group on Adolescent Health define children and youth well-being as “having the support, confidence, and resources to thrive in contexts of secure and healthy relationships, realizing their full potential and rights” [61]. In 2020, Ross et al. [62] proposed five interconnected well-being domains with subdomains and requirements (e.g., good health and optimum nutrition, learning and competence, connectedness, safety and supportive environment, agency and resilience).
In 2002, the WHO identified five key points to promote the delivery of quality health care for young people consisting of accessibility, acceptability, appropriateness, effectiveness, and equity of care [63]. Moreover, six different groups of youth-friendly health services have been delineated:
a) health service specialized in children and adolescent care in a hospital setting;
b) similar specialized service located in the community;
c) school or college-based and stakeholders connected with schools or universities;
d) community-based center providing health services and other services (e.g., help with literacy and numeracy skills);
e) pharmacies and shops that sell health products but do not provide health services;
f) outreach information and service provision.
O’Brien et al. [64] reported the gap between the prevalence of mental disorders in young people and the rates of access to treatments (25-35%), highlighting an important paradox: people with the highest level of need have the worst chance of treatment.
Many factors must be taken into consideration regarding the difficulties and barriers that young people encounter in accessing mental health services, which in our opinion, can be summarized in three factors: service, personal and social factors.
The discussion of barriers related to service factors should start from the original bifurcation of pediatric services and adult services, still leaving a gap for services for adolescents [65]. Primary care professionals experience difficulties in the recognition of youth mental health problems [64] and have already expressed a need for better training in adolescent health [66,67]. Furthermore, poorly trained health professionals encounter difficulties in communicating with young people and their parents [68]. Young people often are unhappy with the consultation resulting in high dropout rates [69]. There are difficulties in receiving the first visit [70] and delays in starting treatment [71]. Some services are inaccessible for reasons relating to cost, where they are located, limited opening hours or lack of advertising and visibility [72-74].
A recent systematic review [75] showed young people's stigmatizing beliefs about mental healthcare, mental health professionals, and access to care. Many adolescents report fear of a lack of confidentiality from health workers [76], about being recognized in a clinic waiting room and about being scolded or carrying out unpleasant procedures [77].
Social determinants frameworks appear to be related to many health inequalities and differential access to resources around the world, such as economic stability, education access and quality, healthcare access and quality, neighborhood and built environment, and social and community context [78]. Extensive evidence supports the impact of social determinants on mental health [79,80]. In some developing countries, restrictive laws and policies limit access to services for some groups of young people [81]. Moreover, during the pandemic, marginalized groups have been less able to engage with telehealth ser-vices [82].
Currently, mental health services are still predominantly organized around diagnostic categories diagnoses of adult mental disorders [83] that are poorly adapted to the developmental characteristics of adolescents. Indeed, the current diagnostic systems for mental disorders (DSM-5 and ICD-11) do not allow a diagnosis to be made if symptom expression is below a certain cut-off value.
Over the years, alternative approaches that reflect psychopathological dimensions have been advocated such as the Research Domain Criteria [84] and the Hierarchical Taxonomy of Psychopathology (HiTOP) [85], but proposals for an evolutionary perspective on emerging psychopathology have been rare [85,86].
Dimensional approaches are certainly necessary for the clinical evaluation of sub-threshold or prodromal symptoms that allow early interventions and preventions to be carried out.
The cornerstone of early intervention in psychiatry was certainly represented by early intervention for psychotic disorders [87] based on the clinical stage model of mental disorders [88]. Subsequently, similar interventions have been proposed for bipolar dis-orders [89] and major depressive disorders [90].
On the other hand, according to Rose’s Strategy for Preventive Medicine [91] “a large number of people exposed to a small risk may generate many more cases than a small number exposed to a high risk”. From this perspective "the high-risk strategy" could be less effective in reducing the prevalence of the disease than "the population strategy".
Public health is a term “coined in the early 19th century to distinguish actions governments and societies - as opposed to private individuals - should take to preserve and protect the people’s health” [92]. Therefore, if we wanted to intervene in public mental health, we should dedicate more resources to prevention rather than treating the individual through “the population strategy”.
Regarding adolescents, “the population strategy” translates into interventions aimed at the multiple factors that can influence the mental health of young people.
Recently, Fazel and Soneson [93] have proposed a new conceptual framework of interventions entitled “the Interactional Schema” of child and adolescent public mental health. This schema places an enhanced emphasis on the interactional nature of three factors influencing child and adolescent mental health: interpersonal, community and institutional. The framework de-emphasizes individual-focused interventions by encouraging public health and prevention approaches especially with interventions de-livered outside specialist mental health settings.
To address the shortcomings of the health system for the mental health of young people, since the beginning of this century, broad-spectrum approaches have emerged [94,95] with models of integrated primary mental health care [96].
Literature provides multiple definitions of integrated healthcare [97], but the one that best suits the purposes of this article is “…changes to health or both health and health-related service delivery which aim to increase integration or coordination” [98].
Starting from the project called “Headspace” founded in Australia [99], we are witnessing a global renewal in youth mental healthcare characterized by multidisciplinary, integration and delivery in a single setting that constitutes a soft entry point to mental healthcare. Numerous nations all around the world are now adopting an integrated youth primary care model [100].
Common features of these models include:
a) clear separation of services for young people from those of children and adults with particular attention to the transition phase;
b) greater participation of young people in service planning and reduction of stigma;
c) single healthcare location with high visibility in the local community;
d) flexible and soft approach to diagnosis especially in the early stages of mental ill-health.
A growing literature is highlighting the improvement in the possibility of accessing services, short-term clinical improvements and high levels of satisfaction among families [101-103].
Due to the negative outcomes of the COVID-19 pandemic on mental health among adolescents, it is imperative to provide strategies to prevent the onset of even serious psychopathological alterations today and in the future [104].
The COVID-19 pandemic has certainly represented a global disaster, but it may also have created countless possibilities for changes in youth mental health services and interventions. In this sense, the restrictive measures adopted to stem the COVID-19 pandemic could represent an issue to reflect on for future public health interventions.
In our opinion, the revolution of the youth care system should include two fundamental macro-areas integrated with each other: re-think public health institutions and promote prevention/early interventions.
Public health institutions include national and international organizations (e.g., the WHO), Ministry of Health, governments, local administrations, national health systems (where present), mental health services, primary, secondary, tertiary care, schools, etc.
Greater cooperation and integration between institutions appear necessary, to reduce the marginalization of minority groups, promote equality of rights and social security policy, address poverty and socioeconomic inequality and greater equity in the possibility of access to care. So far, the effects of these policies on mental health appear mixed [105-107].
An important aspect of the implementation of the care system is represented by the incorporation of the point of view of adolescents. Co-production experiences have shown positive results [108,109].
For about fifteen years, the WHO has recognized primary care as the heart of mental health care [110] as numerous advantages are using this approach (i.e. reduced stigma and barriers, feasibility across most healthcare contexts, etc.). Previous reviews have reported positive data on primary [111,112], secondary and tertiary integration interventions [113] in terms of better accessibility to health services, reduction of waiting times and better early detection of health problems and treatment. Furthermore, health services should have a more widespread presence throughout the territory, particularly primary care, even in the most rural areas, with the possibility of carrying out home interventions.
To reduce barriers, improve the engagement of young people and make the first contact with institutions more accessible, there are some experiences with voluntary youth or paid peer workers [114,115].
The integration of new digital technologies could on the one hand improve accessibility and engagement to care and on the other be used to carry out therapeutic interventions [116-119]. This has been especially true during the COVID-19 pandemic [120]. Digital technologies can also be used in population-based prevention approaches and to help prevent relapse [121,122].
As regards health specialists, and in particular mental health, more training should be carried out for the recognition of the first stages of psychopathological alterations, but also to improve the relationship with young people. A new model of youth mental health care should be fostered with the establishment of a new subspecialty of youth psychiatry, separated from the medical model of pediatrics and in close collaboration with adult psychiatry.
The literal meaning of the term “prevention” is “the act of preventing something from happening” [123]. Based on the moment in which it acted during the pathology, the prevention phases were classified as primary, secondary and tertiary [124]. For the purposes of this article, we will not take into consideration the phases of the disease to be prevented, but the areas in which to act and in particular: the family and peers, the community, the school and the individual.
Family and peer relationships play a key role in youth well-being [125-127]. Scientific literature supports strong evidence on the health of young people with parenting interventions [128]. Moreover, treatment of parental mental illness can reduce the risk of new diagnoses in children [129]. Friendship interventions reported limited evidence on adolescents’ mental health [130].
Social and independent activities in the natural environment can improve mental health outcomes, but there is little evidence that these interventions may have on the incidence of new psychopathological disorders [131-133]. Social cohesion may help protect against the development of anxiety and depression among adolescents and young adults [134]. Important opportunities for intervention in the community are represented by participation in artistic and recreational activities [131,135,136].
Awareness, anti-stigma and mental health promotion campaigns are of fundamental importance for raising awareness among the general population, but most are generic or for adults [137].
The school, even if it is considered an institution, represents a focal point of prevention interventions as a place of relationships between individuals, peers, families and communities. It also represents a fundamental place in the recognition of non-clinically significant symptoms, where preventive interventions can be carried out constantly and systematically. Numerous prevention interventions have been carried out within schools for suicide, self-harming behaviors, substance misuse and bullying with variable efficacy data on young people's well-being [138-142]. Furthermore, good evidence supports the positive effects of physical activity during school hours on students’ mental health [143,144].
For interventions on the individual, the first step to take is to focus on new diagnostic approaches, facilitating interventions for subthreshold expressions of emerging psychopathology as early as possible. As already demonstrated, younger age of onset is a predictor of longer duration of symptoms, comorbidities and worse outcomes [145].
Even if the literature highlights the greater effectiveness of indicated prevention interventions [146,147], in our opinion, we should first focus more on universal and selective prevention interventions through primary care and school and only subsequently, on indicated interventions provided by secondary care systems and tertiary.
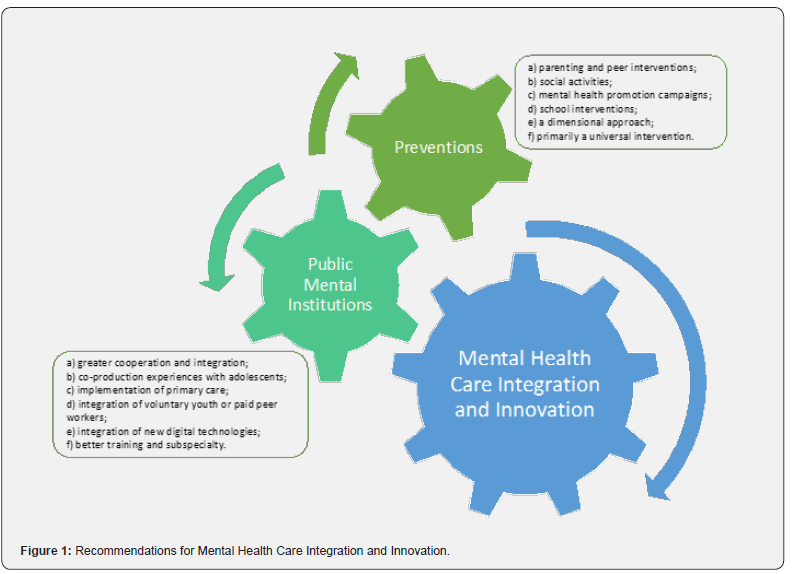
In summary (Figure 1), the key recommendations for implementing public health institutions include:
a) Greater cooperation and integration;
b) Co-production experiences with adolescents;
c) Implementation of primary care;
d) Integration of voluntary youth or paid peer workers;
e) Integration of new digital technologies;
f) Better training and subspecialty.
On the other hand, the key recommendations for prevention include:
a) Parenting and peer interventions;
b) Social activities;
c) Mental health promotion campaigns;
d) School interventions;
e) Dimensional approach;
f) Primarily a universal intervention.
Lastly, we completely agree with Fazel and Soneson's statement “…mental health interventions are not necessarily confined to an individual psychological and/or pharmacological approach, and many children and adolescents could stand to benefit from interventions that take a broader view of the multitude of interpersonal-, community- and institutional-level factors that influence mental health”.
Conclusion
Due to dramatic and sudden changes in their lives during the pandemic, thousands of teenagers around the world could still be at risk for psychopathological disorders creating a mental health “pandemic” scenario.
We believe they deserve an inclusive response in terms of global health measures to avert potentially serious and long-lasting effects in terms of marginalization, stigma and psychopathological developments. Vertical, horizontal and longitudinal integration should be promoted. Despite scientific evidence, the institutions that deal with the mental health of young people are still inefficient even with new approaches that are still not widespread in the world.
The current lack of an adequate care system requires an absolute priority in carrying out a conceptual and practical revolution of health services for the current and future well-being of young people. On the other hand, broader prevention campaigns should be implemented to intercept potentially serious dimensional clinical aspects from a longitudinal perspective.
Thinking of the mental health of young people as a common good to be protected, the fundamental changes to be made are in the internal world and the external world of the individual, of the community, of public health institutions.
Acknowledgement
This paper was entirely funded by the authors, and no pharmaceutical companies were informed of or were involved in the paper. The authors have no potential conflict of interests that are directly relevant to the contents of the paper. All authors have contributed to this paper with equal efforts.
References
- Gruber J, Prinstein MJ, Clark LA, Rottenberg J, Abramowitz JS, et al. (2021) Mental health and clinical psychological science in the time of COVID-19: Challenges, opportunities, and a call to action. Am Psychol 76(3): 409-426.
- Fiorillo A, Gorwood P (2020) The consequences of the COVID‐19 pandemic on mental health and implications for clinical practice. Eur Psychiatry 63(1): e32.
- Rossi R, Socci V, Talevi D, Mensi S, Niolu C, et al. (2020) COVID‐19 pandemic and lockdown measures impact on mental health among the general population in Italy. Front Psychiatry 11: 790.
- (2003) Age limits and adolescents. Paediatr Child Health 8(9): 577-578.
- Jones PB (2013) Adult mental health disorders and their age at onset. Br J Psychiatry Suppl 54: s5-s10.
- Casey BJ, Jones RM, Levita L, Libby V, Pattwell SS, et al. (2010) The storm and stress of adolescence: insights from human imaging and mouse genetics. Dev Psychobiol 52(3): 225-235.
- Bailen NH, Green LM, Thompson RJ (2019) Understanding Emotion in Adolescents: A Review of Emotional Frequency, Intensity, Instability, and Clarity. Emotion Review 11(1): 63-73.
- Somerville LH, Jones RM, Casey B (2010) A time of change: behavioral and neural correlates of adolescent sensitivity to appetitive and aversive environmental cues. Brain Cogn 72(1): 124-133.
- Somerville LH (2013) The teenage brain: sensitivity to social evaluation. Curr Dir Psychol Sci 22(2): 121-127.
- Rapee RM, Oar EL, Johnco CJ, Forbes MK, Fardouly J, et al. (2019) Adolescent development and risk for the onset of social-emotional disorders: a review and conceptual model. Behav Res Ther 123: 103501.
- Uhlhaas PJ, Davey CG, Mehta UM, Shah J, Torous J, et al. (2023) Towards a youth mental health paradigm: a perspective and roadmap. Mol Psychiatry 28(8): 3171-3181.
- Ambrose AJH (2020) Inequities During COVID-19. Pediatrics 146(2): e20201501.
- Ioannidis JPA (2020) Global perspective of COVID-19 epidemiology for a full-cycle pandemic. Eur J Clin Invest 50(12): e13423.6
- Dasgupta M, Engelman R, Levy J, Luchsinger G, Merrick TW, et al. (2014) State of world population 2014: the power of 1.8 billion adolescents, youth and transformation of the future. New York: United Nations Population Fund, 2014.
- Kessler RC, Berglund P, Demler O, Jin R, Merikangas KR, et al. (2005) Lifetime prevalence and age-of-onset distributions of DSM-IV disorders in the National Comorbidity Survey Replication. Arch Gen Psychiatry 62(6): 593-602.
- Gibb SJ, Fergusson DM, Horwood LJ (2010) Burden of psychiatric disorder in young adulthood and life outcome satage 30. Br J Psychiatry 197(2): 122-127.
- Hakulinen C, Elovainio M, Arffman M, Lumme S, Pirkola S, et al. (2019) Mental disorders and long-term labour market outcomes: nationwide cohort study of 2 055 720 individuals. Acta Psychiatr Scand 140(4): 371-381.
- Leone M, Kuja-Halkola R, Leval A, D'Onofrio BM, Larsson H, et al. (2021) Association of youth depression with subsequent somatic diseases and premature death. JAMA Psychiatry 78(3): 302-310.
- Patton GC, Coffey C, Romaniuk H, Mackinnon A, Carlin JB, et al. (2014) The prognosis of common mental disorders in adolescents: a 14-year prospective cohort study. Lancet 383(9926): 1404-1411.
- Mojtabai R, Olfson M, Han B (2016) National Trends in the Prevalence and Treatment of Depression in Adolescents and Young Adults. Pediatrics 138(6): e20161878.
- Wiens K, Bhattarai A, Pedram P, Dores A, Williams J, et al. (2020) A growing need for youth mental health services in Canada: examining trends in youth mental health from 2011 to 2018. Epidemiol Psychiatr Sci 29: e115.
- Bruining H, Bartels M, Polderman TJC, Popma A (2021) COVID-19 and child and adolescent psychiatry: an unexpected blessing for part of our population? Eur Child Adolesc Psychiatry 30(7): 1139-1140.
- Oosterhoff B, Palmer CA, Wilson J, Shook N (2020) Adolescents' Motivations to Engage in Social Distancing During the COVID-19 Pandemic: Associations with Mental and Social Health. J Adolesc Health 67(2): 179-185.
- Duan L, Shao X, Wang Y, Huang Y, Miao J, et al. (2020) An investigation of mental health status of children and adolescents in China during the outbreak of COVID-19. J Affect Disord 275: 112-118.
- McElroy E, Patalay P, Moltrecht B, Shevlin M, Shum A, et al. (2020) Demographic and health factors associated with pandemic anxiety in the context of COVID-19. Br J Health Psychol 25(4): 934-944.
- Tang S, Xiang M, Cheung T, Xiang YT (2021) Mental health and its correlates among children and adolescents during COVID-19 school closure: The importance of parent-child discussion. J Affect Disord 279: 353-360.
- Zhang C, Ye M, Fu Y, Yang M, Luo F, et al. (2020) The Psychological Impact of the COVID-19 Pandemic on Teenagers in China. J Adolesc Health 67(6): 747-755.
- Ellis WE, Dumas TM, Forbes LM (2020) Physically isolated but socially connected: Psychological adjustment and stress among adolescents during the initial COVID-19 crisis. Can J Behav Sci Rev Can Sci du Comport 52: 177-187.
- Tee ML, Tee CA, Anlacan JP, Aligam KJG, Reyes PWC, et al. (2020) Psychological impact of COVID-19 pandemic in the Philippines. J Affect Disord 277: 379-391.
- Barendse MEA, Flannery J, Cavanagh C, Aristizabal M, Becker SP, et al. (2023) Longitudinal Change in Adolescent Depression and Anxiety Symptoms from before to during the COVID-19 Pandemic. J Res Adolesc 33(1): 74-91.
- Newlove-Delgado T, McManus S, Sadler K, Thandi S, Vizard T, et al. (2021) Child mental health in England before and during the COVID-19 lockdown. Lancet Psychiatry 8(5): 353-354.
- Guo J, Fu M, Liu D, Zhang B, Wang X, et al. (2020) Is the psychological impact of exposure to COVID-19 stronger in adolescents with pre-pandemic maltreatment experiences? A survey of rural Chinese adolescents. Child Abuse Negl 110(Pt 2): 104667.
- White HR, Stevens AK, Hayes K, Jackson KM (2020) Changes in Alcohol Consumption Among College Students Due to COVID-19: Effects of Campus Closure and Residential Change. J Stud Alcohol Drugs 81(6): 725-730.
- Dumas TM, Ellis W, Litt DM (2020) What Does Adolescent Substance Use Look Like During the COVID-19 Pandemic? Examining Changes in Frequency, Social Contexts, and Pandemic-Related Predictors. J Adolesc Health 67(3): 354-361.
- Naughton F, Ward E, Khondoker M, Belderson P, Marie Minihane A, et al. (2021) Health behaviour change during the UK COVID-19 lockdown: Findings from the first wave of the C-19 health behaviour and well-being daily tracker study. Br J Health Psychol 26(2): 624-643.
- Pinkham AE, Ackerman RA, Depp CA, Harvey PD, Moore RC (2020) A Longitudinal Investigation of the Effects of the COVID-19 Pandemic on the Mental Health of Individuals with Pre-existing Severe Mental Illnesses. Psychiatry Res 294: 113493.
- Bartel SJ, Sherry SB, Stewart SH (2020) Self-isolation: A significant contributor to cannabis use during the COVID-19 pandemic. Subst Abus 41(4): 409-412.
- Isumi A, Doi S, Yamaoka Y, Takahashi K, Fujiwara T (2020) Do suicide rates in children and adolescents change during school closure in Japan? The acute effect of the first wave of COVID-19 pandemic on child and adolescent mental health. Child Abuse Negl 110(Pt 2): 104680.
- Leske S, Kõlves K, Crompton D, Arensman E, de Leo D (2021) Real-time suicide mortality data from police reports in Queensland, Australia, during the COVID-19 pandemic: an interrupted time-series analysis. Lancet Psychiatry 8(1): 58-63.
- Hawton K, Casey D, Bale E, Brand F, Ness J, et al. (2021) Self-harm during the early period of the COVID-19 pandemic in England: Comparative trend analysis of hospital presentations. J Affect Disord 1(282): 991-995.
- Hill RM, Rufino K, Kurian S, Saxena J, Saxena K, et al. (2021) Suicide Ideation and Attempts in a Pediatric Emergency Department Before and During COVID-19. Pediatrics 147(3): e2020029280.
- Thompson EC, Thomas SA, Burke TA, Nesi J, MacPherson HA, et al. (2021) Suicidal thoughts and behaviors in psychiatrically hospitalized adolescents pre- and post- COVID-19: A historical chart review and examination of contextual correlates. J Affect Disord Rep 4: 100100.
- Schlegl S, Maier J, Meule A, Voderholzer U (2020) Eating disorders in times of the COVID-19 pandemic-Results from an online survey of patients with anorexia nervosa. Int J Eat Disord 53(11): 1791-1800.
- Haripersad YV, Kannegiesser-Bailey M, Morton K, Skeldon S, Shipton N, et al. (2021) Outbreak of anorexia nervosa admissions during the COVID-19 pandemic. Arch Dis Child 106(3): e15.
- Solmi F, Downs JL, Nicholls DE (2021) COVID-19 and eating disorders in young people. Lancet Child Adolesc Health 5(5): 316-318.
- Nissen JB, Højgaard DRMA, Thomsen PH (2020) The immediate effect of COVID-19 pandemic on children and adolescents with obsessive compulsive disorder. BMC Psychiatry 20(1): 511.
- Fitzpatrick O, Carson A, Weisz JR (2021) Using Mixed Methods to Identify the Primary Mental Health Problems and Needs of Children, Adolescents, and Their Caregivers during the Coronavirus (COVID-19) Pandemic. Child Psychiatry Hum Dev 52(6): 1082-1093.
- Rodman AM, Rosen ML, Kasparek SW, Mayes M, Lengua L, et al. (2022) Social experiences and youth psychopathology during the COVID-19 pandemic: A longitudinal study. Dev Psychopathol 12: 1-13.
- Qi H, Liu R, Chen X, Yuan XF, Li YQ, et al. (2020) Prevalence of anxiety and associated factors for Chinese adolescents during the COVID-19 outbreak. Psychiatry Clin Neurosci 74(10): 555-557.
- Hawke LD, Hayes E, Darnay K, Henderson J (2021) Mental health among transgender and gender diverse youth: An exploration of effects during the COVID-19 pandemic. Psychology of Sexual Orientation and Gender Diversity 8(2): 180-187.
- Summers J, Baribeau D, Mockford M, Goldhopf L, Ambrozewicz P, et al. (2021) Supporting Children with Neurodevelopmental Disorders During the COVID-19 Pandemic. J Am Acad Child Adolesc Psychiatry 60(1): 2-6.
- Donker MH, Mastrotheodoros S, Branje S (2021) Development of parent-adolescent relationships during the COVID-19 pandemic: The role of stress and coping. Dev Psychol 57(10): 1611-1622.
- Bülow A, Keijsers L, Boele S, van Roekel E, Denissen JJA (2021) Parenting adolescents in times of a pandemic: Changes in relation-ship quality, autonomy support, and parental control? Dev Psychol 57(10): 1582-1596.
- Ivie EJ, Pettitt A, Moses LJ, Allen NB (2020) A meta-analysis of the association between adolescent social media use and depressive symptoms. J Affect Disord 275: 165-174.
- Vannucci A, Simpson EG, Gagnon S, Ohannessian CM (2020) Social media use and risky behaviors in adolescents: A meta-analysis. J Adolesc 79: 258-274.
- Saiphoo AN, Vahedi Z (2019) A meta-analytic review of the relationship between social media use and body image disturbance. Computers in Human Behavior 101: 259-275.
- Tillman G, March E, Lavender AP, Braund TA, Mesagno C (2023) Disordered Social Media Use during COVID-19 Predicts Perceived Stress and Depression through Indirect Effects via Fear of COVID-19. Behav Sci 13(9): 698.
- Wolf K, Schmitz J (2023) Scoping review: longitudinal effects of the COVID-19 pandemic on child and adolescent mental health. Eur Child Adolesc Psychiatry 21: 1-56.
- Panchal U, Salazar de Pablo G, Franco M, Moreno C, Parellada M, et al. (2023) The impact of COVID-19 lock-down on child and adolescent mental health: systematic review. Eur Child Adolesc Psychiatry 32(7): 1151-1177.
- Rosen ML, Rodman AM, Kasparek SW, Mayes M, Freeman MM, et al. (2021) Promoting youth mental health during the COVID-19 pandemic: A longitudinal study. PLoS One 16(8): e0255294.
- WHO (2016) Promoting health through the life-course. H6: Harnessing the collective strengths of the UN system to reach every woman, child and adolescent. Geneva: World Health Organization.
- Ross DA, Hinton R, Melles-Brewer M, Engel D, Zeck W, et al. (2020) Adolescent Well-Being: A Definition and Conceptual Framework. J Adolesc Health 67(4): 472-476.
- World Health Organization. Making Health Services Adolescent Friendly. Geneva, Switzerland: 2002.
- O'Brien D, Harvey K, Howse J, Reardon T, et al. (2016) Barriers to managing child and adolescent mental health problems: a systematic review of primary care practitioners' perceptions. Br J Gen Pract 66(651): e693-707.
- Signorini G, Singh SP, Boricevic-Marsanic V, Dieleman G, Dodig-Ćurković K, et al. (2017) Architecture and functioning of child and adolescent mental health services: a 28-country survey in Europe. Lancet Psychiatry 4(9): 715-724.
- Kraus B, Stronski S, Michaud PA (2003) Training needs in adolescent medicine of practising doctors: a Swiss national survey of six disciplines. Med Educ 37(8): 709-714.
- Foreman D (2001) General practitioners and child and adolescent psychiatry: awareness and training of the new commissioners. Psychiatr Bull 25(3): 101-104.
- Elster AB, Marcell AV (2003) Health care of adolescent males: overview, rationale, and recommendations. Adolesc Med 14(3): 525-540.
- de Haan AM, Boon AE, de Jong JT, Hoeve M, Vermeiren RR (2013) A meta-analytic review on treatment dropout in child and adolescent outpatient mental health care. Clin Psychol Rev 33(5): 698-711.
- Wang PS, Angermeyer M, Borges G, Bruffaerts R, Tat Chiu W, et al. (2007) Delay and failure in treatment seeking after first onset of mental disorders in the World Health Organization's World Mental Health Survey Initiative. World Psychiatry 6(3): 177-185.
- Dagani J, Signorini G, Nielssen O, Bani M, Pastore A, et al. (2017) Meta-analysis of the Interval between the Onset and Management of Bipolar Disorder. Can J Psychiatry 62(4): 247-258.
- Royal College of Paediatrics and Child Health (2003) Bridging the gaps: health care for adolescents: Intercollegiate Adolescent working party report. Royal College of Paediatrics and Child Health 2003: 60.
- Society for Adolescent Medicine (2004) Access to health care for adolescents and young adults. J Adolesc Health 35(4): 342-344.
- Kefford CH, Trevena LJ, Willcock SM (2005) Breaking away from the medical model: perceptions of health and health care in sub-urban Sydney youth. Med J Aust 183(8): 418-421.
- Goodwin J, Savage E, Horgan A (2016) Adolescents' and Young Adults' Beliefs about Mental Health Services and Care: A Systematic Review. Arch Psychiatr Nurs 30(5): 636-644.
- Sanci LA, Sawyer SM, Kang MS, Haller DM, Patton GC (2005) Confidential health care for adolescents: reconciling clinical evidence with family values. Med J Aust 183(8): 410-414.
- Gleeson C, Robinson M, Neal R (2002) A review of teenager’s perceived needs and access to primary health care: implications for health services. Prim Health Care Res Dev 3: 184-193.
- Alegría M, NeMoyer A, Falgàs Bagué I, Wang Y, Alvarez K (2018) Social Determinants of Mental Health: Where We Are and Where We Need to Go. Curr Psychiatry Rep 20(11): 95.
- Becerra MB, Becerra BJ (2020) Psychological Distress among College Students: Role of Food Insecurity and Other Social Determinants of Mental Health. Int J Environ Res Public Health 17(11): 4118.
- Allen J, Balfour R, Bell R, Marmot M (2014) Social determinants of mental health. Int Rev Psychiatry 26(4): 392-407.
- WHO (2001) Global consultation on adolescent health services a consensus statement. Geneva: Department of Child and Adolescent Health and Development, World Health Organization.
- Shah JL, Scott J, McGorry PD, Cross SPM, Keshavan MS, et al. (2020) Transdiagnostic clinical staging in youth mental health: a first international consensus statement. World Psychiatry 19(2): 233-242.
- Insel T, Cuthbert B, Garvey M, Heinssen R, Pine DS, et al. (2010) Research domain criteria (RDoC): toward a new classification framework for research on mental disorders. Am J Psychiatry 167(7): 748-751.
- Kotov R, Krueger RF, Watson D, Achenbach TM, Althoff RR, et al. (2017) The Hierarchical Taxonomy of Psychopathology (HiTOP): A dimensional alternative to traditional nosologies. J Abnorm Psychol 126(4): 454-477.
- Durbin CE, Wilson S, MacDonald AW (2022) Integrating development into the Research Domain Criteria (RDoC) framework: Introduction to the special section. J Psychopathol Clin Sci 131(6): 535-541.
- Casey BJ, Oliveri ME, Insel T (2014) A neurodevelopmental perspective on the research domain criteria (RDoC) framework. Biol Psychiatry 76(5): 350-353.
- McGorry PD, Hickie IB, Yung AR, Pantelis C, Jackson HJ (2006) Clinical staging of psychiatric disorders: a heuristic framework for choosing earlier, safer and more effective interventions. Aust N Z J Psychiatry 40(8): 616-622.
- Fava GA, Kellner R (1993) Staging: a neglected dimension in psychiatric classification. Acta Psychiatr Scand 87(4): 225-230.
- Berk M, Post R, Ratheesh A, Gliddon E, Singh A, et al. (2017) Staging in bipolar disorder: from theoretical framework to clinical utility. World Psychiatry 16(3): 236-244.
- Verduijn J, Milaneschi Y, van Hemert AM, Schoevers RA, Hickie IB, et al. (2015) Clinical staging of major depressive disorder: an empirical exploration. J Clin Psychiatry 76(9): 1200-1208.
- Rose G, Khaw KT, Marmot M (2008) Rose’s strategy of preventive medicine: The complete original text. Oxford: Ox-ford University Press.
- Krieger N, Birn AE (1998) A vision of social justice as the foundation of public health: commemorating 150 years of the spirit of 1848. Am J Public Health 88(11): 1603-1606.
- Fazel M, Soneson E (2023) Current evidence and opportunities in child and adolescent public mental health: a research review. J Child Psychol Psychiatry 64(12): 1699-1719.
- McGorry PD, Mei C (2018) Early intervention in youth mental health: progress and future directions. Evid Based Ment Health 21(4): 182-184.
- Settipani CA, Hawke LD, Cleverley K, Chaim G, Cheung A, et al. (2019) Key attributes of integrated community-based youth service hubs for mental health: a scoping review. Int J Ment Health Syst 13: 52.
- Hetrick SE, Bailey AP, Smith KE, Malla A, Mathias S, et al. (2017) Integrated (one-stop shop) youth health care: best avail-able evidence and future directions. Med J Aust 207(10): S5-S18.
- Goodwin N (2016) Understanding Integrated Care. Int J Integr Care 16(4): 6.
- Baxter S, Johnson M, Chambers D, Sutton A, Goyder E, et al. (2018) The effects of integrated care: a systematic review of UK and international evidence. BMC Health Serv Res 18(1): 350.
- McGorry PD, Tanti C, Stokes R, Hickie IB, Carnell K, et al. (2007) headspace: Australia's National Youth Mental Health Foundation-where young minds come first. Med J Aust 187(S7): S68-S70.
- McGorry PD, Mei C, Chanen A, Hodges C, Alvarez-Jimenez M, Killackey E (2022) Designing and scaling up integrated youth mental health care. World Psychiatry 21(1): 61-76.
- Hilferty F, Cassells R, Muir K, et al. (2015) Is headspace making a difference to young people’s lives? Final report of the independent evaluation of the headspace program. Sydney: University of New South Wales, 2015.
- Muir K, McDermott S, Gendera S, Flaxman S, Patulny R, et al. (2009) Independent evaluation of head-space: the National Youth Mental Health Foundation. Sydney: University of New South Wales.
- Rickwood DJ, Mazzer KR, Telford NR, Parker AG, Tanti CJ, et al. (2015) Changes in psychological distress and psychosocial functioning in young people visiting headspace centres for mental health problems. Med J Aust 202(10): 537-542.
- Kar SK, Menon V, Yasir Arafat SM, Kabir R (2020) Research in Mental Health During the COVID-19 Pandemic: Quality versus quantity. Sultan Qaboos Univ Med J 20(4): e406-e407.
- Boccia D, Maritano S, Pizzi C, Richiardi MG, Lioret S, et al. (2023) The impact of income-support interventions on life course risk factors and health outcomes during childhood: a systematic review in high income countries. BMC Public Health 23(1): 744.
- Burley J, Samir N, Price A, Parker A, Zhu A, et al. (2022) Connecting Healthcare with Income Maximisation Services: A Systematic Review on the Health, Wellbeing and Financial Impacts for Families with Young Children. Int J Environ Res Public Health 19(11): 6425.
- Simpson J, Albani V, Bell Z, Bambra C, Brown H (2021) Effects of social security policy reforms on mental health and inequalities: A systematic review of observational studies in high-income countries. Soc Sci Med 272: 113717.
- Maina G, Mclean M, Mcharo S, Kennedy M, Djiometio J, King A (2022) A scoping review of school-based indigenous substance use prevention in preteens (7-13 years). Subst Abuse Treat Prev Policy 15(1): 74.
- Grande AJ, Elia C, Peixoto C, Jardim PTC, Dazzan P, et al. (2022) Mental health interventions for suicide prevention among indigenous adolescents: a systematic review. Sao Paulo Med J 140(3): 486-498.
- Funk M, Ivbijaro G (2008) Integrating mental health into primary care: a global perspective. Geneva: World Health Organiza-tion/WONCA, 2008.
- Wolfe I, Satherley RM, Scotney E, Newham J, Lingam R (2020) Integrated Care Models and Child Health: A Meta-analysis. Pediatrics 145(1): e20183747.
- Yonek J, Lee CM, Harrison A, Mangurian C, Tolou-Shams M (2020) Key Components of Effective Pediatric Integrated Mental Health Care Models: A Systematic Review. JAMA Pediatr 174(5): 487-498.
- Pygott N, Hartley A, Seregni F, Ford TJ, Goodyer IM, et al. (2023) Research Review: Integrated healthcare for children and young people in secondary/tertiary care - a systematic review. J Child Psychol Psychiatry 64(9): 1264-1279.
- Simmons MB, Coates D, Batchelor S, Dimopoulos-Bick T, Howe D (2018) The CHOICE pilot project: Challenges of implementing a combined peer work and shared decision-making programme in an early intervention service. Early Interv Psychiatry 12(5): 964-971.
- Simmons MB, Batchelor S, Dimopoulos-Bick T, Howe D (2017) The Choice Project: Peer Workers Promoting Shared Decision Making at a Youth Mental Health Service. Psychiatr Serv 68(8): 764-770.
- Conley CS, Raposa EB, Bartolotta K, Broner SE, Hareli M, et al. (2022) The Impact of Mobile Technology-Delivered Interventions on Youth Well-being: Systematic Review and 3-Level Meta-analysis. JMIR Ment Health 9(7): e34254.
- Mohr DC, Riper H, Schueller SM (2018) A Solution-Focused Research Approach to Achieve an Implementable Revolution in Digital Mental Health. JAMA Psychiatry 75(2): 113-114.
- Rodriguez-Villa E, Rauseo-Ricupero N, Camacho E, Wisniewski H, Keshavan M, et al. (2020) The digital clinic: Implementing technology and augmenting care for mental health. Gen Hosp Psychiatry 66: 59-66.
- Cross S, Piper SE, Davenport TA, Milton AC, Iorfino F, et al. (2019) Implementation study of a prototypic e-clinic being integrated into youth mental health services: staff experiences and reported service quality improvements. Med J Aust 211: S30-S36.
- Torous J, Jän Myrick K, Rauseo-Ricupero N, Firth J (2020) Digital Mental Health and COVID-19: Using Technology Today to Accelerate the Curve on Access and Quality Tomorrow. JMIR Ment Health 7(3): e18848.
- Fusar-Poli P, Sullivan SA, Shah JL, Uhlhaas PJ (2019) Improving the Detection of Individuals at Clinical Risk for Psychosis in the Community, Primary and Secondary Care: An Integrated Evidence-Based Approach. Front Psychiatry 10: 774.
- Cohen A, Naslund JA, Chang S, Nagendra S, Bhan A, et al. (2023) Relapse prediction in schizophrenia with smartphone digital phenotyping during COVID-19: a prospective, three-site, two-country, longitudinal study. Schizophrenia 9(1): 6.
- Prevention Meaning in the Cambridge English Dictionary.
- Baumann LC, Karel A (2013) Prevention: primary, secondary, tertiary. In: Gellman MD, Turner JR (Eds.), Encyclopedia of Behavioral Medicine. New York, NY: Springer (2013), pp. 1532-1534.
- Hughes K, Bellis MA, Hardcastle KA, Sethi D, Butchart A, et al. (2017) The effect of multiple adverse childhood experiences on health: a systematic review and meta-analysis. Lancet Public Health 2(8): e356-e366.
- Yap MB, Pilkington PD, Ryan SM, Jorm AF (2014) Parental factors associated with depression and anxiety in young people: a systematic review and meta-analysis. J Affect Disord 156: 8-23.
- Lereya ST, Patalay P, Deighton J (2022) Predictors of mental health difficulties and subjective wellbeing in adolescents: A longitudinal study. JCPP Adv 2(2): e12074.
- Arango C, Díaz-Caneja CM, McGorry PD, Rapoport J, Sommer IE, et al. (2018) Preventive strategies for mental health. Lancet Psychiatry 5(7): 591-604.
- Siegenthaler E, Munder T, Egger M (2012) Effect of preventive interventions in mentally ill parents on the mental health of the off-spring: systematic review and meta-analysis. J Am Acad Child Adolesc Psychiatry 51(1): 8.e8-17.e8.
- Manchanda T, Stein A, Fazel M (2023) Investigating the Role of Friendship Interventions on the Mental Health Outcomes of Adolescents: A Scoping Review of Range and a Systematic Review of Effectiveness. Int J Environ Res Public Health 20(3): 2160.
- Moula Z, Palmer K, Walshe N (2022) A Systematic Review of Arts-Based Interventions Delivered to Children and Young People in Nature or Outdoor Spaces: Impact on Nature Connectedness, Health and Wellbeing. Front Psychol 13: 858781.
- Bray I, Reece R, Sinnett D, Martin F, Hayward R (2022) Exploring the role of exposure to green and blue spaces in preventing anxiety and depression among young people aged 14-24 years living in urban settings: A systematic review and conceptual framework. Environ Res 214(Pt 4): 114081.
- Fyfe-Johnson AL, Hazlehurst MF, Perrins SP, Bratman GN, Thomas R, et al. (2021) Nature and Children's Health: A Systematic Review. Pediatrics 148(4): e2020049155.
- Breedvelt JJF, Tiemeier H, Sharples E, Galea S, Niedzwiedz C, et al. (2022) The effects of neighbourhood social cohesion on preventing depression and anxiety among adolescents and young adults: rapid review. BJPsych Open 8(4): e97.
- Glew SG, Simonds LM, Williams EI (2021) The effects of group singing on the wellbeing and psychosocial outcomes of children and young people: a systematic integrative review. Arts Health 13(3): 240-262.
- Lee RLT, Lane S, Brown G, Leung C, Kwok SWH, et al. (2020) Systematic review of the impact of unstructured play interventions to improve young children's physical, social, and emotional wellbeing. Nurs Health Sci 22(2): 184-196.
- Henderson C, Robinson E, Evans-Lacko S, Thornicroft G (2017) Relationships between anti-stigma programme awareness, disclosure comfort and intended help-seeking regarding a mental health problem. Br J Psychiatry 211(5): 316-322.
- Brann KL, Baker D, Smith-Millman MK, Watt SJ, DiOrio C (2021) A meta-analysis of suicide prevention programs for school-aged youth. Children and Youth Services Review 121: 105826.
- Gijzen MWM, Rasing SPA, Creemers DHM, Engels RCME, Smit F (2022) Effectiveness of school-based preventive programs in suicidal thoughts and behaviors: A meta-analysis. J Affect Disord 298(Pt A): 408-420.
- Walsh EH, McMahon J, Herring MP (2022) Research Review: The effect of school-based suicide prevention on suicidal ideation and suicide attempts and the role of intervention and contextual factors among adolescents: a meta-analysis and meta-regression. J Child Psychol Psychiatry 63(8): 836-845.
- Guzman-Holst C, Zaneva M, Chessell C, Creswell C, Bowes L (2022) Research Review: Do antibullying interventions reduce internalizing symptoms? A systematic review, meta-analysis, and meta-regression exploring intervention components, moderators, and mechanisms. J Child Psychol Psychiatry 63(12): 1454-1465.
- Fraguas D, Díaz-Caneja CM, Ayora M, Durán-Cutilla M, Abregú-Crespo R, et al. (2021) Assessment of School Anti-Bullying Interventions: A Meta-analysis of Randomized Clinical Trials. JAMA Pediatr 175(1): 44-55.
- Leahy AA, Mavilidi MF, Smith JJ, Hillman CH, Eather N, et al. (2020) Review of High-Intensity Interval Training for Cognitive and Mental Health in Youth. Med Sci Sports Exerc 52(10): 2224-2234.
- Wang X, Cai ZD, Jiang WT, Fang YY, Sun WX, et al. (2022) Systematic review and meta-analysis of the effects of exercise on de-pression in adolescents. Child Adolesc Psychiatry Ment Health 16(1): 16.
- Caspi A, Houts RM, Ambler A, Danese A, Elliott ML, et al. (2020) Longitudinal Assessment of Mental Health Disorders and Comorbidities Across 4 Decades Among Participants in the Dunedin Birth Cohort Study. JAMA Netw Open 3(4): e203221.
- Fusar-Poli P, Correll CU, Arango C, Berk M, Patel V, et al. (2021) Preventive psychiatry: a blueprint for improving the mental health of young people. World Psychiatry 20(2): 200-221.
- Skinner A, Occhipinti JA, Song YJC, Hickie IB (2023) Population-level effectiveness of alternative approaches to preventing mental disorders in adolescents and young adults. Sci Rep 13(1): 19982.






























