Cervical Length and Posterior-Cervical Angle in Prediction of Successful Induction of Labor
Sabry Sayed Mohamed Hassan, Ahmed Elsayed Ahmed Omar* and Ahmed Mohamed Essam El-Din Mahmoud Mansour
Department of Obstetrics and Gynecology, Faculty of Medicine, Ain Shams University, Egypt
Submission: April 20, 2022; Published: April 29, 2022
*Corresponding author: Dr. Ahmed Elsayed Ahmed Omar, Department of Obstetrics and Gynecology,
Faculty of Medicine, Ain Shams University, Egypt
How to cite this article: Sabry S M H, Ahmed E A O, Ahmed M E El-Din M M. Cervical Length and Posterior-Cervical Angle in Prediction of Successful Induction of Labor. J Gynecol Women’s Health 2022: 23(3): 556112. DOI: 10.19080/JGWH.2022.23.556112
Abstract
Background: Owing to limitations of Bishop’s score to evaluate labor induction, transvaginal ultrasound variables over that traditional Bishop’s score are recommended.
Purpose: Evaluating the reliability of measuring the length of the cervix and posterior cervical angle with the transvaginal ultrasonography compared to traditional Bishop’s scores to predict labor induction success.
Patients and Methods: A prospective observational study has been performed on 100 pregnant females with 37-41 weeks’ gestational age who had been acclaimed to undergo labor induction during the period from October 2019 to October 2020. Cervix length, posterior cervical angle, and Bishop’s score were assessed also their relations to successful induction of labor were evaluated.
Results: The posterior cervical angle sensitivity, specificity, and accuracy for predicting successful labor induction were 92%, 89%, and 89% respectively, which were superior to those of Bishop’s score as well as cervical length. Moreover, both posterior cervical angle and cervical length combined use for predicting the successful labor induction show sensitivity 94%, specificity 91%, and accuracy 91%. The assessment by ROC curve demonstrates that area under curve (AUC) sound to be higher using combined ultrasonographic parameters (0.940, 95% CI 0.823 – 0.901), comparing with Bishop’s Scores.
Conclusion: For predicting the labor induction outcome the combined use of both cervix length and post cervix angle was superior to the Bishop’s score.
Keywords: Induction of labor; Cervical length; Posterior cervical angle
Introduction
Induction of labor (IOL) is a popular obstetrical procedure, accounting for about 20–30% of all deliveries [1]. In females with an unfavorable (unripe) cervix, IOL by cervical helps to avoid the possibility of problems for the mother and even the fetus [2]. Despite the fact that following IOL, vaginal delivery (VD) is the preferable option of labor, complications may hinder the delivery, resulting in an unsuccessful IOL. Low Bishop’s scores (<6), maternal obesity, nulliparity, additionally to gestation age less than 41 weeks, all are considered as possible causes of unsuccessful IOL [3].
In clinical practice, the Bishop’s score [4] is the most commonly used system to evaluate the cervical condition [5]. However, some investigators demonstrated that using Bishop’s Score system for predicting IOL success is poor. This is because of the imprecise nature of cervical assessment due to difficulties in evaluating the internal os changes, especially while the external os is closed. In addition, this is considered a subjective measurement with abroad range of uncertainty influenced by the clinical experience of the physician [6].
Prior to IOL, transvaginal ultrasound (TVUS) is suggested to be superior to the conventional Bishop’s scores for evaluating the cervix due to the reproducibility of TVUS parameters and its easy learning [7]. Cervical length (CL) and posterior-cervical angle (PCA) are two ultrasound parameters that have been identified to evaluate the clinical functionality of the cervix, that assess the quality of cervix integrity [8].
Measurement of CL and finding of cervical funneling may have a role in predicting and managing preterm labor, and cervical incompetence [9]. A large number of studies found an inverse relation between the uterine CL during pregnancy and the frequency of preterm labor. The relative risk of preterm birth increases with decreasing CL [10,11].
During pregnancy, PCA, described as the angle between both the posterior uterine wall and the endocervical canal, is measured by TVUS. It was supposed that large PCA has been linked to a more direct, linear exit of uterine contents onto the cervix. Otherwise, smaller PCA leads to a lesser direct force on the inner os, which can protect against cervical distortion [12].
Studies in the literature [13-16] reported that PCA may be a useful parameter to monitor the progression of the cervix towards a labor phenotype [13], and the premature labor’s danger rises with increasing PCA [14]. In addition, one small sample-sized study has shown that PCA is a reliable indicator of IOL [17]. However, it was suggested that PCA is closely associated with the age of gestation at delivery [15,16]. This study purposed to assess the reliability of measuring both PCA and CL using TVU in comparison with Bishop’s score to predict the success of IOL.
Methods and Patients
Study design: A prospective observational study (Accuracy of diagnostic test study) was carried out at Ain Shams University Maternity Hospital during the period from October 2019 to October 2020.
Study Population: 100 pregnant females with gestational age from 37-41 weeks were admitted for IOL. All women included in the study were primigravida, with one live fetus in cephalic presentation, with active labor absence (cervical dilatation > 4-cm or cervical effacement > 80 %) [18]. However, all pregnant women with confirmed fetal anomalies, amniotic fluid disorders, Bishop score > 8, antepartum hemorrhage, cephalopelvic disproportion, previous cervical operation, previous cesarean delivery and myomectomy (previous uterine scar), and those who are morbidly obese (Body Mass Index (BMI) over 40, fetal macrosomia, fetal distress, or uterine anomalies were excluded from the study.
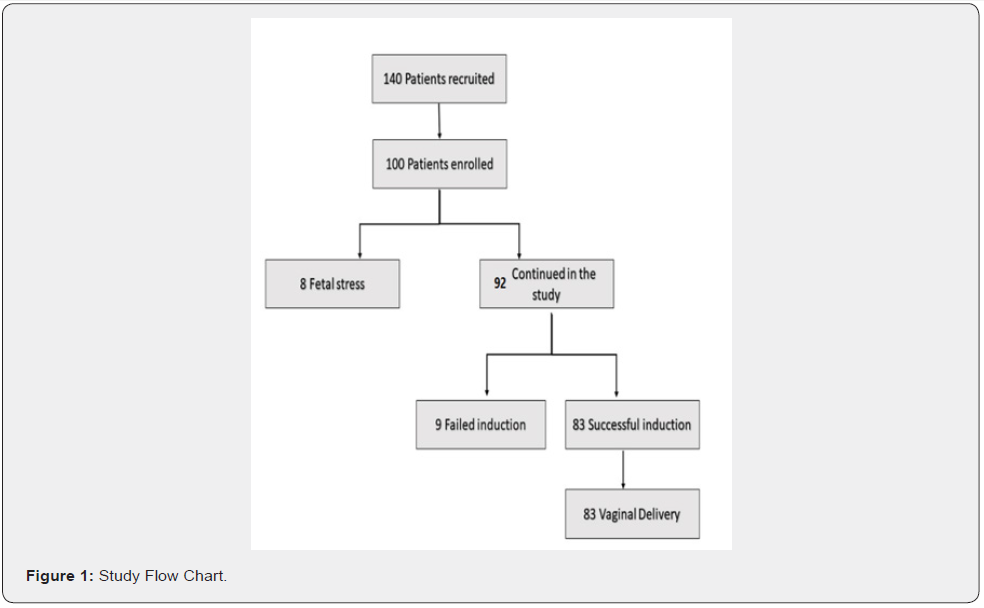
Methods: The study scheme is demonstrated in Figure 1. Informed consent was received from all participants, after counseling them on the nature of the study and its benefits. All women were subjected to full history taking, physical examination, ultrasonography examination by two ultrasound experts; a) Abdominal ultrasound was done by Samsung (Seoul, South Korea) ultrasound system by frequency 7 MHZ to determine fetal viability, weight, number, amniotic fluid, and placental site, b) Transvaginal ultrasound (TVUS) was performed with an empty bladder in the lithotomy position with a frequency 4 -9 MHZ by Samsung (Seoul, South Korea) ultrasonography machine. Gently, the vaginal probe was introduced into the vagina till the back of the fornix was reached. A sagittal cervix plane has been obtained, ensuring proper visualization of the full length of the cervical canal. The calipers were put between both the inner and outer cervical openings for the CL measurement. We measured the angle between the line used in measuring the CL and the back of the uterine wall for the PCA measurement [19]. Finally, to calculate the Bishop’s score, a digital examination was done [20]. Measurements of both CL and PCA were kept blinded from the investigator who performed the Bishop scoring.
Induction of Labor: The IOL protocol was following the protocol of the local university hospital. We gave cervical ripening agents in the form of a vaginal tablet containing 25 μg misoprostol (Vagiprost; Adwia, Cairo, Egypt) to those cases that have a firm or closed cervix to be repeated at least after 4 hours up to 5 doses. In comparison, females who have a flexible cervix and others that improved by Misoprostol were given an oxytocin intravenous infusion (Syntocinon; Novartis, Basel, Switzerland). The initial dosage was 5 units (in 500 ml Ringer solution) average of 12 drops per minute. Each half an hour, we doubled the dosage till we reach effective constrictions; the maximum dose up to 96 drops per minute. We compared the measured PCA and CL with bishop score for evaluation of successful IOL that was defined as the time interval for induction to active labor (according to ACOG[18]) where cervical dilatation >4-cm or cervical effacement > 80 %). In addition, we determined which angle compared with CL and bishop score was followed by unsuccessful IOL which was defined as not progressing to active labor within 24 hours.
Statistical analysis of the data: IBM SPSS software package version 20.0 supplied information to the computer [21]. Numbers and percentages were used to describe quality information. Also, medium and normal divergence for regularly distributing information was utilized to characterize quantity information whilst irregularly distributing information was demonstrated by the medium, minimal and extreme. In the case of information with normal distribution, a comparison between two independent populations was made through an independent t-test whilst over two populations F-test (ANOVA) was utilized. The outcomes of the significant tests are classified as two-tail possibilities. The acquired findings’ importance was assessed at the 5% level.
Result
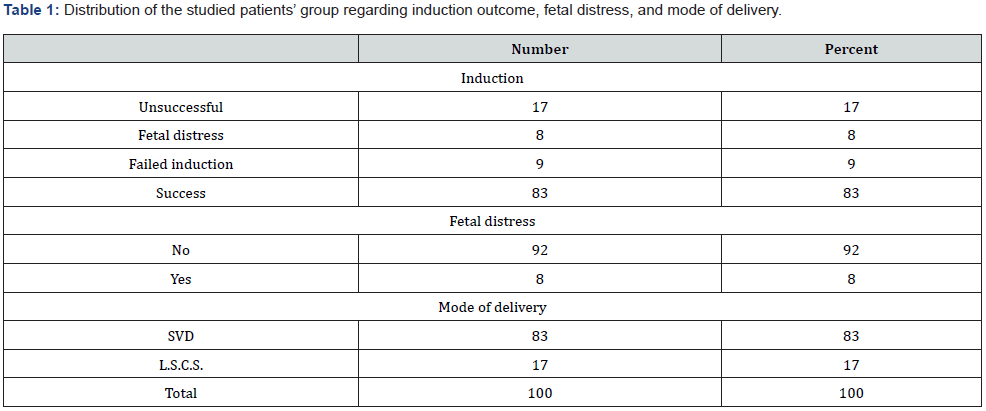
Regarding induction of Labor, unsuccessful induction was recorded in 17 women (17%), including 8 women (8%) with fetal distress and 9 women (9%) with failed induction. whereas successful induction was reported in 83 women (83%). Regarding mode of delivery, 83 women (83%) were delivered via spontaneous vaginal delivery (SVD) and 17 (17%) were delivered via lower segment Cesarian section (LSCS) (Table 1).
In the current study, induction time ranged from 4-18 with a mean value of 8.44±3.15 and induction to delivery time ranged from 6-24 with a mean value of 12.16±4.06. regarding the time from induction to delivery. Time < 24 hrs was recorded in 79 women (95.2%) while time > 24 hrs was recorded in 4 women (4.8%). Our results show no statistically significant differences between failed versus successful induction outcomes regarding maternal age, gestational age, and BMI.
Vagiprost in failed cases, all the patients had 5 Vagiprost, while in success cases ranged from 1-4 with a mean value of 2.39±0.95. There was a highly significant increase in Vagiprost in failed cases more than success cases (P < 0.01).
Bishopscore in failed cases ranged from 2-4 with a mean value of 3.11±0.93 and in success cases ranged from 3-8 with a mean value of 5.64±1.14. CL in failed cases ranged from 29-37 with a mean value of 34.67±2.40 while success cases ranged from 21- 37 with a mean value of 28.76±3.93. PCA in failed cases ranged from 78-110 with a mean value of 91.56±9.96 and in success cases ranged from 70-150 with a mean value of 108.35±17.94. A significant statistical difference was recorded between failed versus successful induction outcomes concerning Bishop score, CL, and PCA (P < 0.001*) (Table 2). In addition, the Bishop’s score additionally to PCA demonstrated a significant positive correlation to successful IOL outcome. Whereas LC showed a negative correlation with successful induction outcome.
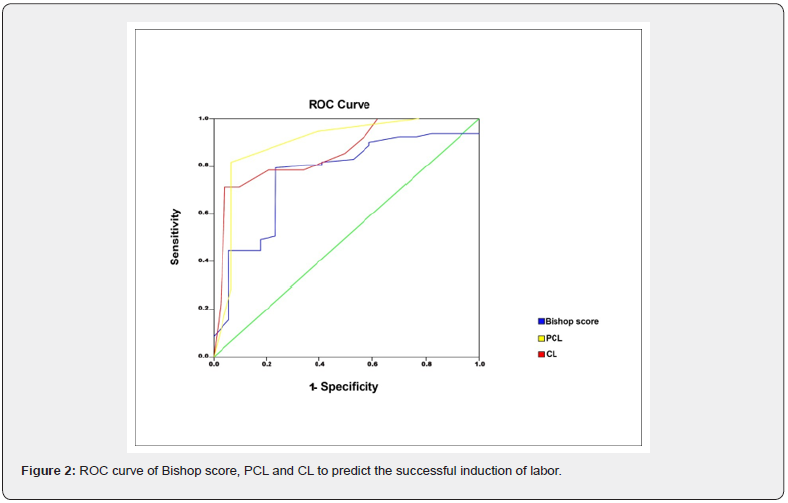
ROC curves of Bishop score, CL, and PCA were performed. The AUC was higher for PCA (AUC 0.905, 95% CI 0.80 – 0.96), in comparison with Bishop’s Score and CL (Figure 2).
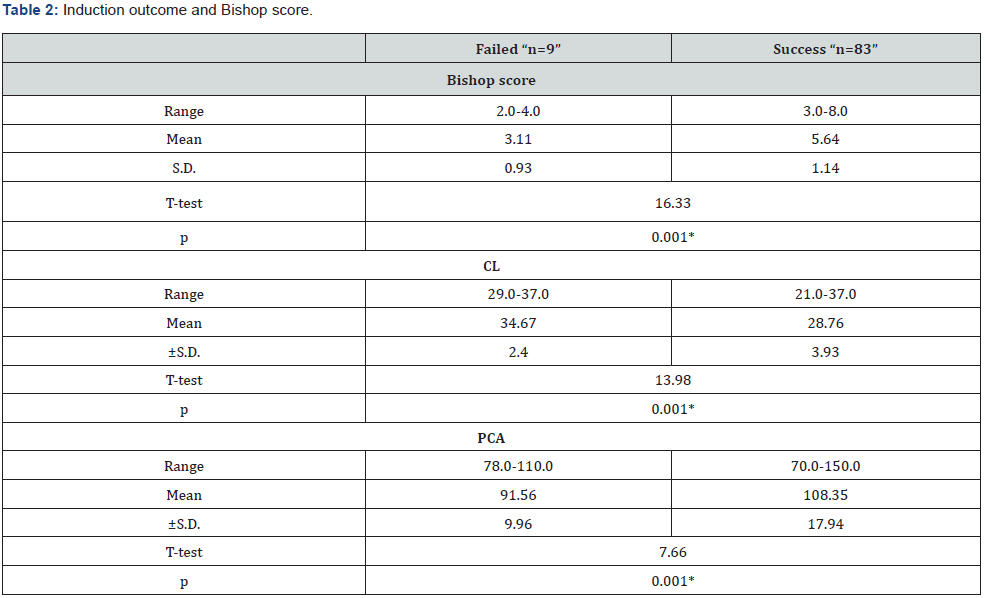
P was significant if < 0.05
S.D. = Standard deviation
*.= significant at level 0.05
T-test=student t-test
The assessed cut-off value of Bishop score in predicting successful IOL consequences was 5. The cut-off value of Bishop score had a sensitivity of 61.0% and a specificity of 83.0% and an accuracy of 78.0. The sensitivity of CL to predict successful induction of labor was 91.0, specificity was 83.0, and accuracy was 86.0 for the CL cut-off value of 34.0. The sensitivity, specificity, and accuracy of PCA cut-off value at 99.0 to predict successful induction of labor was 92.0, 89.0, and 89.0, respectively (Table 3).
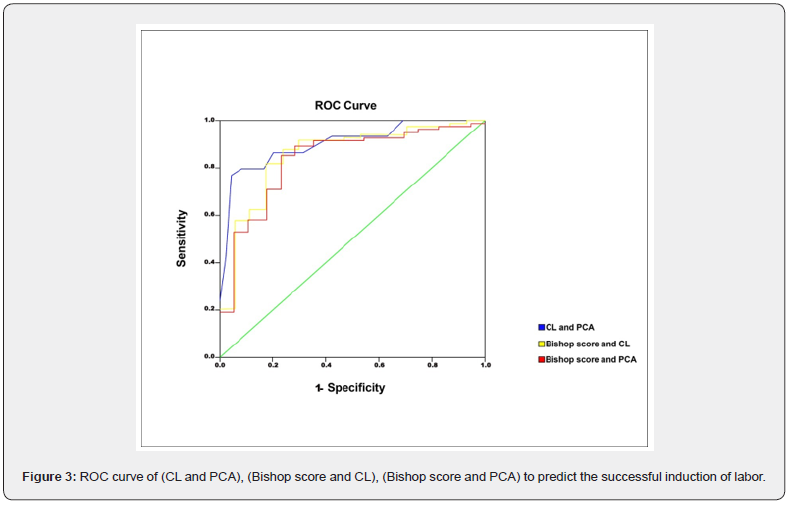
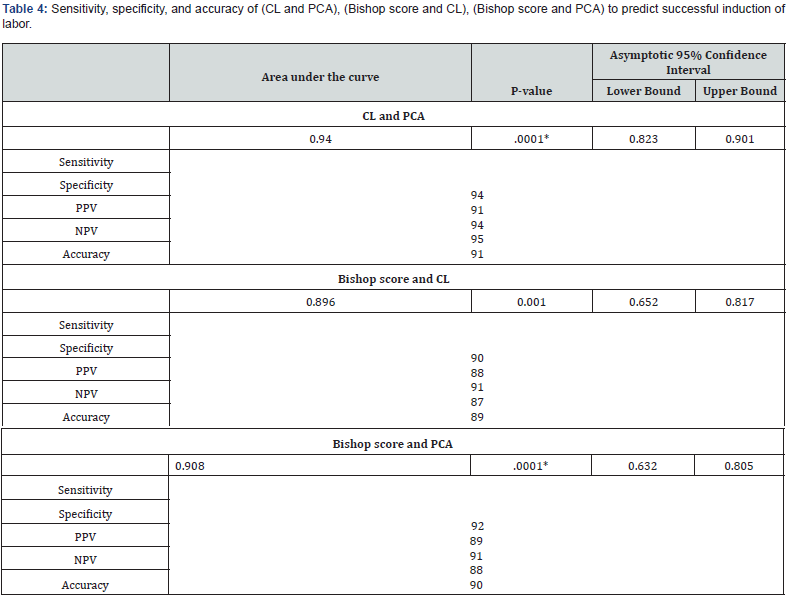
ROC curve for combined CL and PCA was conducted where AUC was 0.940, 95% CI 0.823– 0.901. The combined CL and PCA for predicting successful IOL sensitivity, specificity, and accuracy have been estimated. Sensitivity was 94.0, specificity was 91.0, and accuracy was 91.0 (Figure 3) (Table 4).
ROC curve for combined Bishop score and CL was performed where AUC was 0.896, 95% CI 0.652– 0.817. The sensitivity, specificity, and accuracy of Bishop score and CL to predict successful IOL were 90.0, 88.0, and 89.0, respectively (Figure 3) (Table 4).
ROC curve of combined Bishop score and PCA was done where AUC was 0.908, 95% CI 0.632– 0.805. The sensitivity combined Bishop score and PCA to predict successful induction of labor was 92.0, specificity was 89.0, and accuracy was 90.0 (Figure 3) (Table 4).

PPV = positive predictive value
NPV = Negative predictive value
The bishop score shows a negative significant correlation with cervical length, induction time, induction to delivery time, and Vagiprost, while there was a positive significant correlation with cervical angle. The CL shows a negative correlation with cervical angle, and a positive significant correlation with induction time, induction to delivery, and Vagiprost. The PCA shows a negative significant correlation with induction time, induction to delivery, and Vagiprost. The induction time shows a positive significant correlation with induction to delivery and Vagiprost, final the induction to delivery shows a positive significant correlation with Vagiprost (Table 5).

**. Correlation is significant at the 0.01 level
*. Correlation is significant at the 0.05 level
Discussion
In some fetal and maternal conditions, IOL is done when labor is more beneficial than waiting for spontaneous labor [2]. Bishop score was introduced in practice as a predictor of successful IOL and it is considered the most important and useful scoring system [22]. However, as alternatives for the conventional Bishop’s score, some ultrasound parameters were recommended. The most used parameters are measuring CL and PCA measurement by using TVUS [23].
In the current study, PCA and the CL measurements are assessed using TVUS in comparison with the Bishop’s scoring to predict the effectiveness of IOL. This study was carried out at Ain Shams University Maternity Hospital on 100 pregnant admitted for IOL. The females’ age ranged from 18-39 years with a mean of 24.17±3.94 and with gestational age from 37-41 weeks. Through this study, IOL was unsuccessful in 17 cases (17%) where 8 (8%) of them had fetal distress. In addition, after IOL 83 cases (83%) delivered by SVD while 17 cases (17%) delivered by LSCS.
Jing study included 475 cases indicated for IOL. Out of all cases, 393 (82.7%) had VD in addition to 82 (17.3%) had urgent CS; 40 from those were failed to access the active phase of labor, 20 because of fetal hypoxia, 19 caused by progression failure, additionally to 3 for different causes [24].
That vaginal dose of 50-μ5 of misoprostol was studied widely, results demonstrated that such dose is more effective but not secure, unlike a 25-μg dosage (related to high uterine tachysystole levels, uterine hyperstimulation, also cesarean because of the abnormal cardiotocographic outcome as well as meconium [25]. In the present study, 25-μg misoprostol tablets in failed cases, all the patients had 5 tablets. While in success cases ranged from 1-4 with a mean value of 2.39±0.95. There was a highly significant increase in Vagiprost in failed cases more than success cases (P < 0.01).
Silva study was carried out on 412 pregnant females who were indicated for IOL. The IOL has been performed in females with Bishop’s Score < 6 using vaginal 25-μg Misoprostol tablets. 69% of the pregnant females with IOL progressed to VD, but 31% of the females progressed to CS. In 244 cases (59.2%) 1 or 2 misoprostol tablets have been utilized. From 412 cases, 197 (47.8%) needed oxytocin after that within the labor procedure, after induction by misoprostol. Thus, high Bishop’s score, as well as prior VD, seemed to be the greatest indicators of successful IOL by vaginal 25-μg misoprostol tablets [26].
The current study showed induction time ranged from 4-18 with a mean value of 8.44±3.15 and induction to delivery time ranging from 6-24 with a mean value of 12.16±4.06 where 79 cases (95.2%) it takes < 24 hrs was and 4 cases (4.8%) takes > 24 hrs. The induction time showed a positive significant correlation with induction to delivery and Vagiprost, final the induction to delivery time show a positive significant correlation with Vagiprost.
Parvin Bastani stated a positive correlation between the time of induction to birth and the CL with a P-value of <0.01. They concluded the superiority of CL over the Bishop score and PCA [27]. In a study conducted by Mohamed S. Abouzeid on 100 females, aged between 18 and 35, with gestational ages between 37 and 42 weeks, a positive correlation with high statistical significance (HS) between Vagiprost dosage with CL and induction time (p-value <0.001) was found throughout the whole cases with medical indications for IOL. Additionally, a negative correlation with high statistical significance (HS) between both Vagiprost dosage with Bishop’s scores and PCA has been demonstrated [28].
Due to the status of the cervix before labor was identified as the most significant indicator of successful IOL, a number of studies have assessed the relation between the Bishop’s score and sonographic cervical measurement with IOL consequence [29].
In the current study, CL in failed IOL cases ranged from 29- 37 with a mean value of 34.67±2.40 while successful IOL cases ranged from 21-37 with a mean value of 28.76±3.93. A statistically significant difference was recorded between both failed and successful induction outcome concerning CL (P < 0.05). It showed a negative correlation with successful induction outcome.
For the prediction of successful IOL at cut-off 34 mm, the CL showed sensitivity, specificity, and accuracy of 91.0, 83.0, and 86.0 respectively with PPV of 86.0 and NPV of 80.0. In addition, CL showed a negative correlation with PCA, and a positive significant correlation with induction time, induction to delivery, and Vagiprost.
The meta-analysis of Verhoeven’s study involved 31 analyses that reported both CL and delivery outcome. For cesarean deliveries, summary estimates of both sensitivity/specificity for CL were 0.82/0.34, 0.64/0.74, and 0.13/0.95 for different cutoffs 20, 30, and 40 mm, respectively. They concluded that CL and cervical wedging by sonography at or near term are able to predict the outcome of delivery after IOL [5].
The Anikwe Study30 on 1333 pregnant women where 60 females have been selected for IOL with a success rate was 100%. The mean induction delivery time for all participants was 8.1 ± 3.0 hours and a mean labor duration of 7.4 ± 2.9 hours. Pre-induction CL is a good predictor of a short labor duration (P = 0.001).
In the present study regarding the relation between Bishop’s score and IOL outcome in failed cases ranged from 2-4 with a mean value of 3.11±0.93 while success cases ranged from 3-8 with a mean value of 5.64±1.14. A difference with a statistical significance was recorded between failed versus successful induction outcome regarding Bishop Score (P < 0.05). Bishop Score showed a positive correlation with successful induction outcome.
For the prediction of successful IOL, Bishop’s score at the cut-off point 5 demonstrated sensitivity, specificity, and accuracy of 90.0, 88.0, and 89.0 respectively with PPV of 91.0 and NPV of 87.0. Thus, our study showed that the CL has better sensitivity, specificity, and accuracy in predicting successful IOL over Bishop’s score.
This was concurrent with Kolkman’s study [30,31], which concluded that the Bishop score seems to be a weak predictor for the induced labor result at term. IOL has also succeeded in 86.9% of cases, in Bajpai’s study [32] on 131 women who underwent IOL at term with intact membranes and live fetuses, successful IOL was in 86.9% of patients. At cut-off values of ≥ 4, TVUS cervical parameters were better than Bishop score (Sensitivity 77% vs. 65%, Specificity 93% vs. 86%) in predicting successful IOL. ROC analysis illustrated that AUC was higher for TVUS Score (0.90, 95% CI 0.84 – 0.95), in comparison to Bishop score. Also, Kanwar’s study on 110 nulliparous term pregnant women admitted for IOL showed CL by TVUS is a valuable predictor of successful IOL. When CL < 3.5 cm, 88% (66/75) delivered vaginally and when CL > 3.5 cm only 11.42% (4/35) delivered vaginally. Concluding that within 24 hours of induction, CL is a powerful predictor of vaginal delivery in comparison to Modified Bishop’s score [33].
Our results were in disagreement with Khandelwal study [34] on 62 nulliparous women who underwent IOL. In comparison with CL (P = 0.004), in the prediction of the active phase of labor, the Bishop score had a high significance (P-value < 0.0001). For Bishop’s scores, the optimum cut-off point for predicting IOL through 6 hours was > 4 having a 69% sensitivity and 79% specificity. Likewise, CL better cut-off point for IOL prediction in 6 hours was < 25 mm by 51% sensitivity and 70% specificity. For predicting induction-to-delivery interval within 12 h, Bishop scores (P = 0.001) were also superior to CL (P = 0.01). Also, Bahadori [35] found a more significant correlation of Bishop (0.001) than of CL (0.04) for predicting cervical ripening in 12 hours. Cut off for Bishop score was ≥4 had a sensitivity and specificity of 57.9% and 28.7% respectively, whereas cut off for CL ≥19 mm had a sensitivity of and a specificity of 66.7% and 65% respectively.
In the current study, PCA in failed IOL cases ranged from 78-110 with a mean value of 91.56±9.96 and in success IOL cases ranged from 70-150 with a mean value of 108.35±17.94. A difference with a statistical significance was found between both failed and successful induction finding concerning PCA (P < 0.05). PCA showed a positive correlation with successful induction outcome.
To predict the success of IOL at a cut-off value of 99.0, PCA presented sensitivity, specificity, and accuracy of 92, 89.0, and 89.0, respectively with PPV of 90 and NPV of 88. In addition, PCA showed a negative significant correlation with induction time, induction to delivery, and Vagiprost.
PCA > 99.5°, CL < 34 mm, and a Bishop’s score > 5 were suggested as cut-offs for the prediction of successful IOL by Al‐ Adwy [17]. There was no significant difference among the AUC of those three measurements. However, the PCA > 99.5° had the highest sensitivity (91.84%), specificity (90.48), positive prediction value (95.7%), negative prediction value (82.6%), positive probability rate (9.64), in addition to negative probability rate (0.09) comparing to the other two indicators.
The study conducted by Gokturk that included multi-variate regression analyses of variables showed that multiparity, CL, PCA, and Bishop’s score had a significant statistical prediction for the success of IOL [36].
The CL and post PCA sensitivity, specificity, and accuracy to predict successful induction were 94.0, 91.0, 91.0 respectively. While both Bishop score and CL sensitivity, specificity, and accuracy for predicting the success of induction were 90.0, 88.0, 89 respectively. In addition, the Bishop’s score and PCA’s sensitivity, specificity, and accuracy for the prediction of successful induction were 92.0, 89.0, 90 respectively.
Ahmed’s study on 200 pregnant women indicated IOL. Overall sensitivity, specificity, ultrasound measures (CL and PCA) were 89.55, and 63.64 respectively, while sensitivity, specificity, of bishop score, were 78.87, and 82.76, respectively [37].
Conclusion
Our data concluded that ultrasonographic cervical assessment and Bishop’s score are good indicators of successful IOL but sonographic parameters including CL and PCA seemed to be better compared to the Bishop’s score in predicting the labor induction finding especially when used combined. Overall, PCA showed the best sensitivity and specificity as an indicator for IOL outcome especially in the combination with CL measurement.
Acknowledgement
The authors of this study possess no acknowledgments to make with regards to this study and this manuscript’s content.
Ethical Approval
The study was presented for approval from the Ethical Committee of the Department of Obstetrics and Gynecology, Faculty of Medicine, Ain Shams University.
Author Contributions
Ahmed E. Omar designed the study and performed data collection and analysis. Ahmed E. Mansour, Sabry S. Hassan supervised all procedures and data interpretation. Ahmed Elsayed Ahmed Omar wrote the manuscript. All authors were involved in the revision of the manuscript and approved the final version for submission.
References
- Marconi AM (2019) Recent advances in the induction of labor. F1000Res 8: F1000 Faculty Rev-1829.
- De Vivo V, Carbone L, Saccone G, Magoga G, De Vivo G, et al. (2020) Early amniotomy after cervical ripening for induction of labor: a systematic review and meta-analysis of randomized controlled trials. American journal of obstetrics and gynecology 222(4): 320-329.
- Parkes I, Kabiri D, Hants Y, Ezra Y (2016) The indication for induction of labor impacts the risk of cesarean delivery. J Matern Fetal Neonatal Med 29(2): 224-228.
- Bishop EH (1964) Pelvic scoring for elective induction. Obstet Gynecol 24: 266-268.
- Verhoeven CJ, Opmeer BC, Oei SG, Latour V, van der Post JA, et al. (2013) Transvaginal sonographic assessment of cervical length and wedging for predicting outcome of labor induction at term: a systematic review and meta-analysis. Ultrasound Obstet Gynecol 42(5): 500-508.
- Navve D, Orenstein N, Ribak R, Daykan Y, Shechter-Maor G, et al. (2017) Is the Bishop-score significant in predicting the success of labor induction in multiparous women? Journal of Perinatology 37(5): 480-483.
- Vayssière C, Morinière C, Camus E, Le Strat Y, Poty L, et al. (2002) Measuring cervical length with ultrasound: evaluation of the procedures and duration of a learning method. Ultrasound Obstet Gynecol 20(6): 575-579.
- Myers KM, Feltovich H, Mazza E, Vink J, Bajka M, et al. (2015) The mechanical role of the cervix in pregnancy. J Biomech 48(9): 1511-1523.
- Jafari-Dehkordi E, Adibi A, Sirus M (2015) Reference range of the weekly uterine cervical length at 8 to 38 weeks of gestation in the center of Iran. Adv Biomed Res 4: 115.
- Slager J, Lynne S (2012) Assessment of cervical length and the relationship between short cervix and preterm birth. J Midwifery Womens Health 57 Suppl 1: S4-S11.
- Vaisbuch E, Romero R, Mazaki-Tovi S, Erez O, Kusanovic JP, et al. (2010) The risk of impending preterm delivery in asymptomatic patients with a nonmeasurable cervical length in the second trimester. Am J Obstet Gynecol 203(5): 446.e1-9.
- Al-Azzawi F, Webster S (2018) Childbirth & Obstetrics Techniques. In: (3rd edn), JP Medical Ltd, India.
- Knight JC, Tenbrink E, Sheng J, Patil AS (2017) Anterior uterocervical angle measurement improves prediction of cerclage failure. J Perinatol 37(4): 375-379.
- Sepúlveda-Martínez A, Díaz F, Muñoz H, Valdés E, Parra-Cordero M (2017) Second-Trimester Anterior Cervical Angle in a Low-Risk Population as a Marker for Spontaneous Preterm Delivery. Fetal Diagn Ther 41(3): 220-225.
- Sochacki-Wójcicka N, Wojcicki J, Bomba-Opon D, Wielgos M (2015) Anterior cervical angle as a new biophysical ultrasound marker for prediction of spontaneous preterm birth. Ultrasound Obstet Gynecol 46(3): 377-378.
- Lynch TA, Szlachetka K, Seligman NS (2017) Ultrasonographic Change in Uterocervical Angle is not a Risk Factor for Preterm Birth in Women with a Short Cervix. Am J Perinatol 34(11): 1058-1064.
- Al-Adwy AM, Sobh SM, Belal DS, Omran EF, Hassan A, et al. (2018) Diagnostic accuracy of posterior cervical angle and cervical length in the prediction of successful induction of labor. Int J Gynaecol Obstet141(1): 102-107.
- Neal JL, Lowe NK, Ahijevych KL, Patrick TE, Cabbage LA, et al. (2010) “Active labor” duration and dilation rates among low-risk, nulliparous women with spontaneous labor onset: a systematic review. Journal of midwifery & women's health 55(4): 308-318.
- Gokturk U, Cavkaytar S, Danısman N (2015) Can measurement of cervical length, fetal head position and posterior cervical angle be an alternative method to Bishop score in the prediction of successful labor induction? J Matern Fetal Neonatal Med 28(11): 1360-1365.
- ACoPB (2009) (ACOG Committee on Practice Bulletins -- Obstetrics). ACOG practice bulletin no. 107: induction of labor. Obstet Gynecol. 114(2 Pt 1): 386-397.
- IBM Corp9 (2011) IBM SPSS Statistics for Windows, Version 20.0. Armonk, NY: IBM Corp, USA.
- Ivars J, Garabedian C, Devos P, Therby D, Carlier S, et al. (2016) Simplified Bishop score including parity predicts successful induction of labor. Eur J Obstet Gynecol Reprod Biol 203: 309-314.
- Papillon-Smith J, Abenhaim HA (2015) The role of sonographic cervical length in labor induction at term. J Clin Ultrasound 43(1): 7-16.
- Lu J, Cheng YKY, Ho SYS, Sahota DS, Hui LL, et al. (2020) The predictive value of cervical shear wave elastography in the outcome of labor induction. Acta Obstet Gynecol Scand 99(1): 59-68.
- McMaster K, Sanchez-Ramos L, Kaunitz AM (2015) Balancing the efficacy and safety of misoprostol: a meta-analysis comparing 25 versus 50 micrograms of intravaginal misoprostol for the induction of labour. Bjog 122(4): 468-476.
- Silva TAG, Borges Júnior LE, Tahan LA, Costa TFA, Magalhães FO, et al. (2017) Induction of Labor using Misoprostol in a Tertiary Hospital in the Southeast of Brazil. Rev Bras Ginecol Obstet 39(10): 523-538.
- Bastani P, Hamdi K, Abasalizadeh F, Pourmousa P, Ghatrehsamani F (2011) Transvaginal ultrasonography compared with Bishop score for predicting cesarean section after induction of labor. Int J women's health 3: 277-280.
- Mohamed S Abouzeid YAW, Nabil F Mohamed (2018) Comparative Study between 2D and 3D Ultrasound Cervicometry and Digital Assessment of the Cervix before Induction of Labour. Egypt J Hosp Med 71(5): 3261-3372.
- Baños N, Migliorelli F, Posadas E, Ferreri J, Palacio M (2015) Definition of Failed Induction of Labor and Its Predictive Factors: Two Unsolved Issues of an Everyday Clinical Situation. Fetal Diagn Ther 38(3): 161-169.
- Anikwe CC, Okorochukwu BC, Uchendu E, Ikeoha CC (2020) The Effect of Ultrasound-Measured Preinduction Cervical Length on Delivery Outcome in a Low-Resource Setting. Sci World J 2020: 8273154.
- Kolkman DG, Verhoeven CJ, Brinkhorst SJ, van der Post JA, Pajkrt E, et al. (2013) The Bishop score as a predictor of labor induction success: a systematic review. Am J Perinatol 30(8): 625-630.
- Bajpai N, Bhakta R, Kumar P, Rai L, Hebbar S (2015) Manipal Cervical Scoring System by Transvaginal Ultrasound in Predicting Successful Labour Induction. J Clin Diagn Res 9(5): Qc04-9.
- Kanwar SN, Reena P, Priya BK (2015) A comparative study of trans vaginal sonography and modified Bishop's Score for cervical assessment before induction of labour. Sch J App Med Sci 3(6B): 2284-2288.
- Khandelwal R, Patel P, Pitre D, Sheth T, Maitra N (2018) Comparison of Cervical Length Measured by Transvaginal Ultrasonography and Bishop Score in Predicting Response to Labor Induction. J Obstet Gynaecol India 68(1): 51-57.
- Bahadori F, Ayatollahi H, Naghavi-Behzad M, Khalkhali H, Naseri Z (2013) Predicting factors on cervical ripening and response to induction in women pregnant over 37 weeks. Med Ultrason 15(3): 191-198.
- Gokturk U, Cavkaytar S, Danısman N (2015) Can measurement of cervical length, fetal head position and posterior cervical angle be an alternative method to Bishop score in the prediction of successful labor induction? J Matern-fetal Neo M 28(11): 1360-1365.
- Ahmed IB, Ashraf HM, Abd El-Moneim MZ (2020) Bishop score versus ultrasonographic techniques for prediction of successful induction of labor. Al-Azhar Med J 49(4):1703-1712.






























