Breast Ultrasonography: Old or New?
Di Grezia G1*, Gatta G1, Pignata S2, Grassi Roberta3 and Grassi Roberto1
1Radiology Department, Second University of Naples, Italy
2Tricarico Private Hospital - Belvedere M.Mo, Cosenza, Italy
3Radiologya and Radiotherapy Department, University of Sassari, Italy
Submission: September 26, 2016; Published: October 03, 2016
*Corresponding author: Di Grezia G, Radiology Department, Second University of Naples, 312, Vittorio Emanuele Street, 83100 Avellino, Italy.
How to cite this article: Di Grezia G, Gatta G, Pignata S, Grassi R, Grassi R. Breast Ultrasonography: Old or New?. J Gynecol Women’s Health. 2016; 1(4): 555566. DOI: 10.19080/JGWH.2016.01.555566
Abstract
Harmonic Imaging, Frequency compound, Superb microvascular Imaging, Elastosonography, 3/4D ultrasonography, Authomatized breast ultrasonography and High frequency Sonography are only some of the advanced technology in breast ultrasonography imaging. Although the high operator-dependence and despite of the presence of new methods, at the state, there is no technique that can replace the handle 2D B mode ultrasonography, not only for the detection but also to guide interventional procedures, like fine needle aspiration or biopsies. In detail, automatized breast ultrasonography could be used as a useful tool in the completion of breast cancer screening in dense breasts and HFU can be helpful in the evaluation of superficial lesions or in nipple discharge.
Keywords: Breast cancer; Ultrasonography; 3D Ultrasonography; ABUS, Elastosonography; HFU
Introduction
In the last years, many techniques are developed to increase the performance of breast ultrasonography and to improve cost/effectiveness ratio. Harmonic Imaging, Frequency compound, Superb microvascular Imaging, Elastosonography, 3/4D ultrasonography, Authomatized breast ultrasonography and High frequency Sonography are only some of the advanced technology in under forty first level breast cancer screening [1]. Although the advancement of these new technologies that can improve the accuracy of the diagnosis and reduce the patient anxiety [2], dedicated breast training during residency or in specialized radiologist is required. Breast ultrasonography can distinguish cystic from solid masses and is a valid help to guide interventional procedures, such as US-guided fine needle cytology or biopsies [3,4]; is a cheap, non-invasive, quick and safe diagnostic tool used as a complementary exam in over forty women and as the main exam in under forty patients. However, the main limitation of breast ultrasonography is operator dependent nature and its low specificity, leading to a high rate of false positive results [5].
2D Breast Ultrasonography with 3D and 4D Reconstruction
Modern breast US systems have broad-band high frequency probes (6-16 MhZ) with high multidimensional imaging level; 3D ultrasonography allows the study of the surrounding studies in three orthogonal planes with an update also of BIRADS system [6]. A composed imaging reduces shadowing artifacts and avoids overlapping scans; it allows to visualize the lesion in more than one plans, thanks to the rotation of the y-axis, with the availability of more standardized images such as in coronal plane [7] and to have the more accurate measure of the long axis; in adjunct the volume evaluation is possible [8]. Four dimensional breast ultrasonography is able to demonstrate the elasticity of the lesion elasticity, thanks to movement of compression and decompression of breast tissue. Four-D grey scale ultrasonography do not enhance true-positive results or reduce false-positive ones [9]. The add of ev contrast further improves the diagnostic accuracy in 3D imaging, even if is not of common use because of the lack of spread and the cost of the exam [10].
Harmonic Imaging – Frequency Compound
Tissue harmonic imaging is an automatized tissue optimization that enhances contrast to optimize the image quality; so it can be considered an adjunct to conventional breast ultrasound with an improving of detectability and characterization [11]. It improves also the visualization of the needle against fatty background during breast interventional procedures [12]. Even if the tissue imaging plays a role in fatty breasts, compound imaging improves lesion echo texture assessment. The combination between this too methods could be a useful tool in the detection and in the characterization of breast lesions [13].
Superb Microvascular Imaging (SMI)
The development of Colour Doppler Flow Imaging (CDFI) consists in the detection of cery small or micro blood flow states, the SMI that use an algorithm that allows the visualization of minute vessels with slow velocity without using an ev contrast media. The limitations are due to the high sensitivity of the technique due to extraneous Doppler signals (motion artifacts) indistinguishable from blood flow; to increase the specificity, SMI associated to CDFI is preferable [14].
Elastosonography
The implementation of 2D ultrasonography takes advantages of the hardening of malignant breast tissues. Elastosonography can measure the degrees of stiffness in different tissues. The exam is composed by three phases: a) low-frequency vibration; b) colour mapping of stiffness; c) stiffness parameters. However, the manual compression could modify the elastography results, even if the methods are able to increase sensitivity in BI-RADS 3 lesions and to increase the detection rate of malignant lesions [15]. The acoustic radiation force impulse (ARFI) is a freehand compression technique that allows standardizing the technique; however the overlapping of benign and malignant lesions hardness causes a limited actual clinical application; to date, only combining conventional ultrasonography with elastosonography can direct the decision of interventional procedures [15]. Indeed, more prospective trials are necessary to determine if quantitative analysis of images can help to overcome some pitfalls of this method [16] (Figure 1).
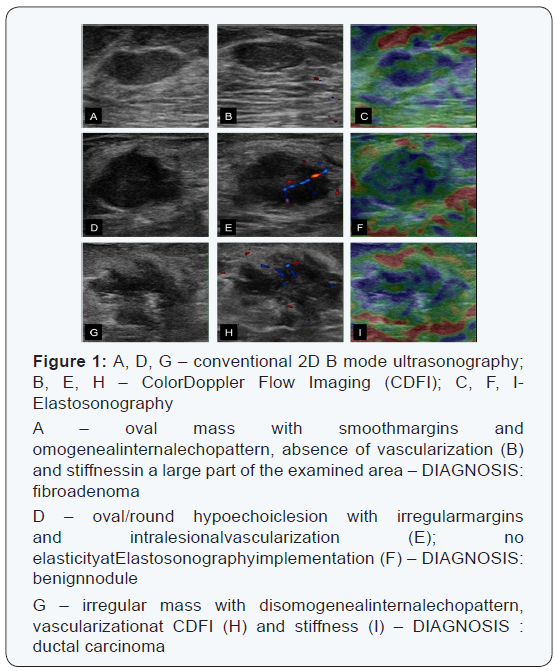
Automatized Breast Ultrasonography (ABUS)
ABUS was introduced more than 10 years ago and it has evolved and improved until the new models are disseminated. The standardize technique, the reproducibility, and the operator – independence gave to ABUS a role as a complementary exam after screening mammography in dense breasts [17]. ABUS scanner of new generation are supine water-coupled scanning with 4 to 7 Mhz transducers that can acquire until 2000-5000 images and some of these equipments can also do 3D reconstructions; despite the width of the probe (from 12 to 26 cm), in some cases of large breasts, more than one scan could be necessary. The time of the execution of the exam is about 15 minutes, less than the time necessary for handle breast ultrasonography (about 19 minutes) [18]. ABUS can minimize the number of recalls in mammography screening, even if a second handle breast ultrasonography could be necessary for the BI-RADS judgment and to guide interventional procedures, such as fine needle aspiration or core biopsies. Indeed, the irreplaceable breast training demonstrates also that automated breast ultrasonography cannot be preferred to a manual US examination [19] in clinical senology, but only in breast cancer screening.
Very High Frequency Ultrasonography (HFU)
The high frequency ultrasonography probes (until 70 MHz) allows an evaluation within the first centimeter of the skin surface with high spatial resolution although reduced the low depth of penetration with a good assessment of skin [20], first order ducal involvement and nipple-area complex. That is exactly why HFU represents a valid complement of a conventional breast ultrasonography also in hereditary syndromes with breast involvement [21,22]. HFU allows also the evaluation of dermatologic diseases of the breast, the skin thickness, the retraction assessment, papillary lesions, inflammatory carcinoma or Paget disease and could have a role in the assessment of nipple discharge. In our institution, are in progress some experimental studies with the first ultra-high-frequency US system (Vevo MD; FUJIFILM Visual Sonics, Amsterdam, the Netherlands; 48–70- MHz linear-array transducer). Preliminary results consist of the different layers of the skin with the differentiation of the superficial layer of the superficial fascia and of the cutaneous and subcutaneous structures [23].
Conclusion
At the state, in our experience, according to literature, there is no technique that can replace the conventional 2D B mode ultrasonography; all these methods presented could be considered as an implementation of the standard exam, associated to the patient history and the clinical breast exam in under forty patients; mammography is mandatory in over forty females. The evaluation of the semiotic signs of the lesion in conventional exam, associated to adjunct signs, determined by SMI, Harmonic Imaging, 3D reconstructions could direct but not replace an interventional procedure. Automatized breast ultrasonography could be used as a useful tool in the completion of breast cancer screening in dense breasts and HFU can be helpful in the deepening of the superficial breast lesions or skin diseases with breast involvement or in nipple discharge. In conclusion the “new” breast ultrasonography can only put beside the conventional breast ultrasonography but not replace it.
References
- Di Grezia G, Somma F, Serra N, Reginelli A, Cappabianca S, et al. (2016) Reducing Costs of Breast Examination: Ultrasound Performance and Inter-ObserverVariability of Expert Radiologists Versus Residents. Cancer Invest 34(7): 355-360.
- Di Grezia G, Prisco V, Iannaccone T, Grassi R, Serra N, et al. (2016) Personality disorder and temperamental traits in patients with breast disease: preliminary results Minerva Psichiatrica 57(3): 85-89.
- Gatta G, Iaselli F, Parlato V, Di Grezia G, Grassi R, et al. (2011) Differential diagnosis between fibroadenoma, giant fibroadenoma and phyllodestumour: sonographicfeatures and core needlebiopsy. Radiologia Medica 116(6): 905-918.
- Gatta G, Di Grezia G, Ancona A, Capodieci M, Coppolino F, et al. (2013) Underestimation of a typical lobular hyperplasia and lobular carcinoma in situ at stereotaxic 11-gauge vacuum-assisted breast biopsy. European Journal of Inflammation 11(3): 825-835.
- Leconte I, Fellah L (2008) US and dense breasts: where do we stand? J Radiol 89(9 Pt 2): 1169-1179.
- American College of Radiology: illustratedbreastimaging reporting data and system (BI-RADS): Ultrasound (1st edn), Reston, American College of Radiology, 2003.
- Weismann C, Hergan K (2007) Current status of 3D/4D volume ultrasound of the breast. Ultraschall Med 28(3): 273-282.
- Scherzer O (2002) A fast and robust algorithm for 2D/3D panorama ultrasound. Realtime Imaging 8: 53-60.
- Weismann CF, Datz L (2007) Diagnosticalgorithm: how to make use of new 2D, 3D and 4D ultrasound technologies in breast imaging. Eur J radiol 64(2): 250-257.
- Li MH, Liu Y, Liu LS, Li PX, Chen Q (2016) Differential diagnostic value of real-time elastography and three dimensional ultrasound imaging in breast lumps. Zhongua Yi Xue Za Zhi 96(19): 1515-1518.
- Szopinski KT, Pajk AM, Wysocki M, Amy D, Szopinska M, et al. (2003) Tissue harmonic imaging: utility in breast sonography. J Ultrasound Med 22(5): 479-487.
- Mesurolle B, Bining HJ, El Khoury M, Barhdadi A, Kao E, et al. (2006) Contribution of tissue harmonic imaging and frequency compound imaging in interventional breast sonography. Ultrasound Med 25(7): 845-855.
- Mesurolle B, Helou T, El-Khoury M, Edwardes M, Sutton EJ (2007) Tissue harmonic imaging, frequency compound imaging and conventional imaging: use and benefit in breast sonography. J Ultrasound Med 26(8): 1041-1051.
- Yan M, Li G, Li J, Ren WD (2015) The Diagnostic Value of Superb Microvascular Imaging (SMI) in Detecting Blood Flow Signals of Breast Lesions: A Preliminary Study Comparing SMI to Color Doppler Flow Imaging. Medicine 94(36): 1-6.
- Ebnerl (2014) Diagnostic Performance and Additional Value of Elastosonography in Focal Breast Lesions: Statistical Correlation between Size-Dependant Strain Index Measurements Multimodality- BI-RADS Score, and Histopathology in a Clinical Routine Setting ISNR Radiology Article ID 396368.
- Landoni V, Francione V, Marzi S, Pasciuti K, Ferrante F, et al. (2012) Quantitativeanalysis of elastography images in the detection of breastcancer. Eur J Radiol 81(7): 1527-1531.
- U.S. Food and Drug Administration (FDA) (2012) Medicaldevices: somo-v Automated Breast Ultrasound System (ABUS): P110006 [Internet]. Silver Spring, MD: U.S. Food and Drug Administration.
- Shin HJ, Kim HH, Cha JH (2015) Current status of automated breast ultrasonography. Ultrasonography 34(3): 165-172.
- Kan L, Olivotto IA, Warren Burhenne LJ, Sickles EA, Coldman AJ (2000) Standardized abnormal interpretation and cancer detection ratios to assess reading volume and reader performance in a breast screening program. Radiology 215(2): 563-567.
- Gatta G, Di Grezia G, Lieto R, Ancona A, Laieta MT, et al. (2012) No evidence for an association between trauma and breast carcinoma: A retrospective cohort study. Global Advanced Journal of Medicine and Medical Sciences 1(7): 172-180.
- Ferraro GA, Romano T, De Francesco F, Grandone A, D’Andrea F, et al. (2013) Management of prepubertalgynecomastia in two monozygotic twins with Peutz-Jeghers syndrome: from aromatase inhibitors to subcutaneous mastectomy. Aesthetic Plast Surg 37(5): 1012-1022.
- Di Grezia G, Romano T, De Francesco F, Somma F, Rea G, et al. (2014) Breast ultrasound in the management of gynecomastia in Peutz- Jeghers Syndrome: a case report. J Med Case Rep 8: 440.
- Allemann N, Silverman RH, Reinstein DZ, Coleman DJ (1993) High frequency ultrasound imaging and spectral analysis in traumatic hyphema. Ophtalomology 100(9): 1351-1357.







