Relationship Between Body Adiposity Indices and Lung Function Parameters of Young Nigerian Women
Taofeek Oluwole Awotidebe1*, Olufesola Motunrayo Fasakin2, Jubril Mohammed3, Olayemi Fehintola Awopeju4,5, Adekola B Adeoyegun6, Halimah Adenike Salahudeen1 and Rufus Adesoji Adedoyin1
1Department of Medical Rehabilitation, College of Health Sciences, Obafemi Awolowo University, Nigeria
2Nursing Services Department, Veterans Affairs Medical Center, USA
3Department of Physiotherapy, Bayero University Kano, Nigeria
4Department of Medicine, College of Health Sciences, Obafemi Awolowo University, Nigeria
5Chest Clinic Unit, Obafemi Awolowo University Teaching Hospitals Complex, Nigeria
5Department of Physiotherapy, Bayero University Kano, Nigeria
6Department of Physiotherapy, Osun State University Teaching Hospital, Nigeria
Submission: November 16, 2023; Published: December 01, 2023
*Corresponding author: Taofeek Oluwole Awotidebe (PT, Ph. D), Department of Medical Rehabilitation, College of Health Sciences, Obafemi Awolowo University, Ile - Ife, Nigeria
How to cite this article: Taofeek Oluwole Awotidebe*, Olufesola Motunrayo Fasakin, Jubril Mohammed, Olayemi Fehintola Awopeju, Adekola B Adeoyegun, Halimah Adenike Salahudeen and Rufus Adesoji Adedoyin. Relationship Between Body Adiposity Indices and Lung Function Parameters of Young Nigerian Women. Int J Pul & Res Sci. 2023; 6(5): 555700. DOI: 10.19080/IJOPRS.2023.06.555700
Abstract
Purpose: Increasing body adiposity (BA) has been reported to predispose individuals to developing pulmonary diseases. However, the link between BA measures and lung function (LF) parameters of young women remains controversial. This study investigated the relationships between BA indices and LF parameters among Nigerian young women.
Methods: Two hundred and twenty (220) female undergraduate students at a Nigerian university participated in this cross-sectional study using purposive sampling. The participant’s age and measures of BA including body mass index percentage fat mass (FM), and percent body fat (%BF) were measured using standard procedures. Lung function parameters of forced vital capacity (FVC), forced expiratory volume in first second (FEV1), percent FEV1 (%FEV1) and peak expiratory flow rate (PEFR) were also measured using a spirometer. Data were analyzed using descriptive and inferential statistics. Alpha level was set at p≤ 0.05.
Results: The mean age and BMI of participants were 20.2±2.3 years and 21.8±3.8 kg/m2, respectively. More than a quarter, (29.5%) of participants were either overweight or obese. Age had significant inverse correlation with FVC (r=-0.143; p=0.034). Similarly, significant inverse correlations were found between BMI and FVC (r=-0.145; p=0.032) and FEV1(r=-0.150; p=0.026). Additionally, significant inverse correlations were found between %BF and FVC (r=-0.208; p=0.002) and FEV1 (r=-0.211; p=0.002). The predictive risks for poor lung function among underweight and overweight/obese individuals were 6.8 and 12.2%, respectively.
Conclusion: It was concluded that young Nigerian women presented with high rates of abnormal BMI categories and body adiposity measures that contribute negatively to their lung function parameters.
Keywords: Bodyweight status; Pulmonary function; Undergraduates; Young adults; Abdominal adiposity
Abbreviations: FM: Fat Mass; BMI: Body Mass Index; PEFR: Peak Expiratory Flow Rate; FVC: Forced Vital Capacity; LF: Lung Function; BA: Body Adiposity; OSA: Obstructive Sleep Apnea; COPD: Chronic Obstructive Pulmonary Disease; FFM: Fat Free Mass; FEVI: Forced Expiratory Volume in First Second; BIA: Bioelectrical Impedance Analysis; TLC: Total Lung Capacity; FRC: Functional Residual Capacity; RC: Residual Capacity; ANOVA: Analysis of Variance; SPSS: Statistical Package for Social Sciences; CARTA: Consortium for Advanced Research Training in Africa
Introduction
Overweight/obesity-related pulmonary dysfunction has been reported to be on the rise globally [1,2]. Whilst the relationship between obesity and pulmonary dysfunction is becoming progressively distinct, there is still a dearth of information regarding whether the prevalence and pattern occurs similarly in all population groups [3]. Moreover, the pathophysiology of some complex/chronic respiratory disorders such as asthma, obstructive sleep apnea (OSA), and chronic obstructive pulmonary disease (COPD)have been reported to involve interactions among several factors that may include environmental, genetic, behavioral and anthropometric (body adiposity) variables [4]. Body adiposity and growth are principal elements of health that require regular monitoring with the view to preventing future chronic diseases [5]. There has been an increasing interest among researchers in ascertaining the relationships between body adiposity measures and lung function parameters to have better insight into the adiposity-related pulmonary diseases prevention and rehabilitation [6,7].
For example, upper body obesity has been found to predispose individuals to a higher risk of cardiovascular and metabolic disease compared to lower body obesity [8]. Some studies have even suggested that upper body fat distribution and abdominal adiposity are better predictors of lung function than body weight or BMI [9,10]. Body fat distribution, body fat percentage and fat free mass (FFM) indices are known to influence lung function parameters such as forced vital capacity (FVC) and of changes in forced expiratory volume in first second (FEV1) [11]. Lastly, Müller et al. [12] stated that the association between body composition and lung function has both a muscular and an obesity effect component that is “u-shaped”.
Currently, there are neither universally accepted norms for body composition nor a consensus regarding the percentage of body fat that is associated with optimal health risk. Nevertheless, the lowest statistical health risk is associated with body fat percentages of range between12% to 20% for males and 20% to 30% for females. Males and females differ in terms of how and where their body fat is stored, how various hormones are secreted in proportion to body fat, and the way the brain regulate body fat [13] (Shi and Clegg). Undoubtedly, women have a higher proportion of body fat compared to men [14]. Over the last three decades, despite the reported negative consequences of overweight/obesity on pulmonary functions, none or limited studies have investigated the influence of body adiposity indices such as fat distribution and body mass on the pulmonary functions of young women [15] (Peters and Dixon).
Previous reports have not distinguished fat from fat free mass, and this has resulted in an underestimation of the importance of body adiposity as a factor influencing pulmonary function in women. There is dearth of information on the relationships between body adiposity indices and lung function parameters among young women in Nigeria. As a priori, we hypothesized that there would be no significant difference in the lung function parameters and different body mass index categories of young undergraduate women Hence, the aim of the present study was to investigate the relationships between body adiposity measures and lung function parameters among apparently healthy young Nigerian female university students.
Methods
Participants
The participants of this study were young female students selected from different faculties of the Obafemi Awolowo University, Ile-Ife, Osun State, Nigeria. They were recruited using purposive sampling technique. Recruitment was carried out in the various halls of residence of female students in the university campus. Eligibility for inclusion criteria included being a female undergraduate student at the university, with age ranged between 18-28 years old and evidence of residing in the halls of residence. Participants were excluded from the study if they were presented with any self-reported medical condition such as asthma, cardiovascular disease, clinical diagnosis of pulmonary disease, or type-2 diabetes. Individuals with history or current smoking of cigarette were excluded. Pregnant women were also excluded from the study. The sample size for this study was based on a sample size formula, n = z2*p* (1-p)/d2, where n = the desired sample size of the study group, z = 1.96 at 95% confidence interval, p = pre study estimate of proportion = total width of expected confidence interval [16]. Hence, a minimum sample size of 196 participants was required. However, 10% was added to the estimated sample size to obtain a total of about 220 participants. This was done to accommodate for incomplete or missing data and possible attrition.
Procedure
The protocol to conduct this study was approved by the Health Research and Ethics Committee of the Institute of Public Health, College of Health Sciences, Obafemi Awolowo University, Ile-Ife, Nigeria (Protocol number: IPHOAU/12/1339). The purpose of the study was explained to each participant and written informed consent was sought and obtained. The participant’s age was recorded, while their anthropometric characteristics and indices of adiposity were measured using standard procedures. Lung function parameters were recorded using a standard spirometer in accordance with the recommendations of the American Thoracic Society.
Assessment of body adiposity measures
Body weight and height: Weight of the participants was measured using a standardized weighing scale. The body weight was measured in kilograms (kg) to the nearest 0.1kg, with the participants in standing position, barefoot and putting on only light clothing. The height of the participants was measured using a standardized height meter that is calibrated from 0 to 200cm. Participants’ heels, back and occiput were made to touch the scale with the participant looking straight ahead during measurement. The height of each participant was measured to the nearest 0.1m. Body mass index (BMI): BMI was calculated by dividing the body weight in kilograms by the height in meters squared (kg/m2). The calculated BMI for each participant were classified as follows: underweight (≤ 18.5kg/m2), normal (18.5-24.9 kg/m2), overweight (25.0-29.9 kg/m2) and obesity (≥ 30kg/m2) [17]. Waist and hip circumference: The waist and hip circumference was measured using an inelastic tape measure. The waist circumference was measured using the anatomical landmark situated 2.5cm above the umbilicus. The hip circumference was taken using the surface marking of the greater trochanter as the reference point [18]. Both waist and hip circumference for each participant was expressed in centimeters to the nearest 0.1cm. The waist to hip ratio was calculated by dividing waist circumference by hip circumference.
Percent Body Fat: Bioelectrical Impedance Analysis (BIA) machine was used to assess the percent body fat (% BF) using the manufacturer’s instruction as guide (Camry HF 10, Taiwan). All participants were instructed to remove all metal objects (such as earrings, necklaces, wrist watches and mobile phones) away from their body. Dryness of the palm was ensured by using a dry towel for cleaning. Parameters such as height, weight, age and sex for each participant were imputed into the micro data processor of the instrument before switching on the start button. Each participant was instructed to stand erect with the 2 feet together, while holding the handles of the BIA machine in both hands such that the palms adequately cover the metal surface situated in the handles of the instrument [19]. Thereafter, the participants were then instructed to hold out their arms straight at 90 degrees of shoulder flexion and stand still until a new set of data is displayed on the display. The percentage body fat was approximated to the nearest one decimal place.
Fat and fat free mass: Fat mass was estimated using the product of weight in kilograms and percent body fat (weight × % BF). Fat free mass was calculated as the difference between measured body mass and predicted fat mass [20].
Assessment of lung function parameters
The lung function testing was done using a standard spirometer (Moose PFT system; Cybermedic, Louisville, Co, USA, softwarev3.8D). Three spirometry or lung function test trials were performed in accordance with the American Thoracic Society criteria to ensure uniformity [21]. Initially, participants were first instructed on the lung function maneuver would be performed, with appropriate demonstration of the technique for proper understanding. For the main test, each participant was instructed to take a deep breath up to total lung capacity (TLC) from functional residual capacity (FRC). Thereafter, the participant will then insert the mouthpiece of the spirometer and make sure their lips are tightly sealed around the mouthpiece before starting the forced exhalation maneuver. The forced exhalation involves a sudden blowing (blasting) of all the air in their lungs as fast and as complete as possible through the mouthpiece of the spirometer and until residual capacity (RC). Lung function parameters including forced expiratory volume in first second (FEV1), % FEV1, forced vital capacity (FVC) and peak expiratory flow rate (PEFR) were then recorded from the spirometer display. All lung function tests were conducted in the chest clinic by a pulmonologist (OF) to limit test variability. Finally, the spirometer was calibrated on a daily basis, and weekly quality control measures were obtained to ensure accuracy and precision of test equipment.
Data analysis
Data obtained was summarized using descriptive statistics of frequency, percentage, mean and standard deviation. Analysis of variance (ANOVA) was used to test for the differences in different BMI groups (weight-status) with respect to body adiposity and lung function parameters. Multiple regression analysis was used to determine the risk of having poor lung function according to weight-status. Physical characteristics and body adiposity measures that correlated with lung function parameters were included in the model to predict poor lung function among underweight and overweight/obese individuals. Data obtained was found to be normally distributed using the Kolmogorov–Smirnov test. Furthermore, the dissimilarities in the data were tested using homoscedasticity before performing regression analysis. The International Business Machine (IBM) Statistical Package for Social Sciences (SPSS) Statistics version21.0 (IBM Co., Armonk, NY, USA) was used to perform statistical analyses. The alpha level was set at p≤0.05.
Results
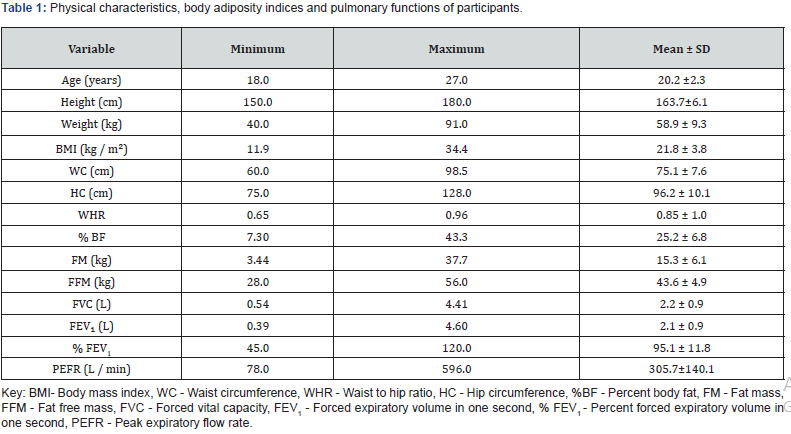
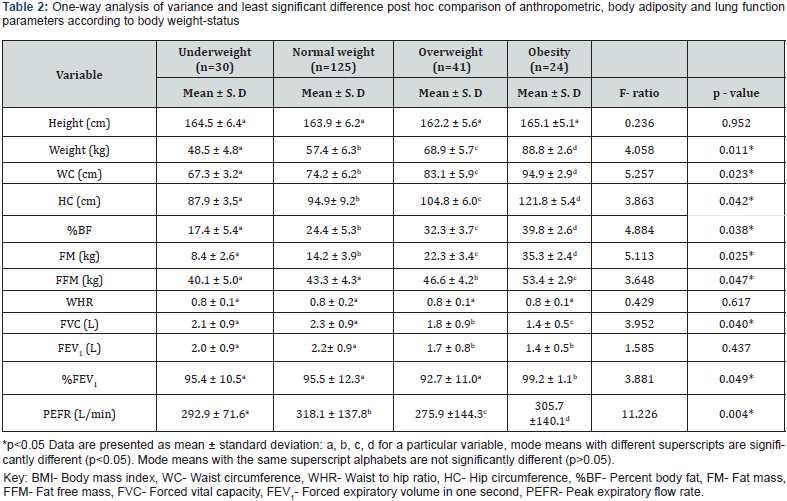
The findings of this study as presented in indicated that the means (and standard deviation) of age, BMI, %BF, FM and FFM of the participants were 20.2 ± 2.3 years and 21.8 ± 3.8kg/m2, 25.2 ± 6.8, 15.3 ± 6.1 kg and 43.6 ± 4.9, respectively. Furthermore, the means (and standard deviation) for the lung function parameters of FVC, FEV1, and %FEV1were 2.2 ± 0.9L, 2.1 ± 0.9L and 95.1 ± 11.8, respectively. (Table 1) (Table 2) shows results of the one-way analysis of variance (ANOVA) and Least Significant Difference post hoc comparison of anthropometric variables, body adiposity measures and lung function parameters according to bodyweight status (different BMI category). The results among others show that more than a quarter, (29.5%) of participants were overweight/obese. Higher BMI, %BF and FM were recorded among individuals with overweight/obese BMI category compared to individuals with normal weight (P<0.05).
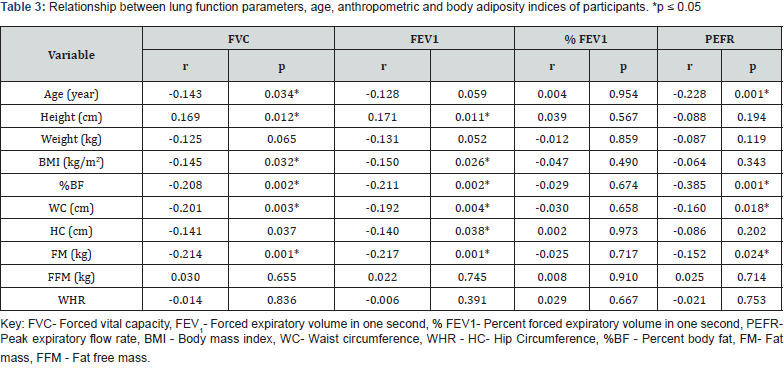
Contrastingly, significantly lower levels of lung function parameters were reported among individuals in both the underweight (FVC: 2.1 ± 0.9L), overweight ((FVC: 1.8 ± 0.9 L) and obese (FVC: 1.4 ± 0.5L) category compared to individuals with normal weight (FVC: 2.3 ± 0.9 L) (F = 3.952; p = 0.040). However, all participants were comparable in height, WHR, FEV1 and %FEV1 (p > 0.05). Lastly, there were significant differences in weight (F = 4.058; p = 0.011), %BF (F = 4.884; p = 0.038), FM (F = 5.113; p = 0.025), FVC (F = 3.952; p = 0.040) and PEFR (F = 11.226; p = 0.004) across bodyweight status of participants. The results of the study further showed that the age of participants was significantly and inversely correlated with FVC (r = -0.143; p = 0.034) and PEFR (r=-0.228; p = 0.001). Similarly, BMI had an inverse significant correlation with FVC (r = -0.145; p = 0.032) and FEV1(r = -0.150; p = 0.026). Likewise, significantly inverse correlations were also reported between FM and FVC (r = -0.214; p = 0.001), FEV1 (r = -0.217; p = 0.001) and PEFR (r = -0.152; p = 0.024) as represented in (Table 3).
The results from the multiple regression analysis for the prediction of poor lung function among individuals with underweight with respect to age, height, body adiposity measures and lung function parameters is presented in (Table 4). For the prediction of poor lung function with respect to age; the study revealed that the unstandardized coefficient beta was 0.418, t = 5.796 and confidence interval at 95% (CI = 0.276-0.560). The FVC value also had an unstandardized coefficient beta was 0.440, t = 1.469 and confidence interval at 95% (CI = -0.148-1.029). The prediction equation for poor lung function among individuals with underweight with respect to age, body adiposity measures and lung function parameters is presented as:
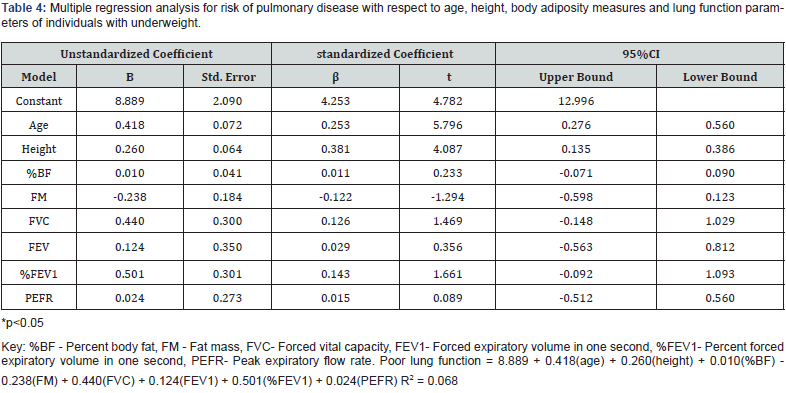
Poor lung function = 8.889 + 0.418(age) + 0.260(height) + 0.010(%BF) - 0.238(FM) + 0.440(FVC) + 0.124(FEV1) + 0.501(%FEV1) + 0.024(PEFR) and R2 = 0.068, contributing approximately about 6.8%.
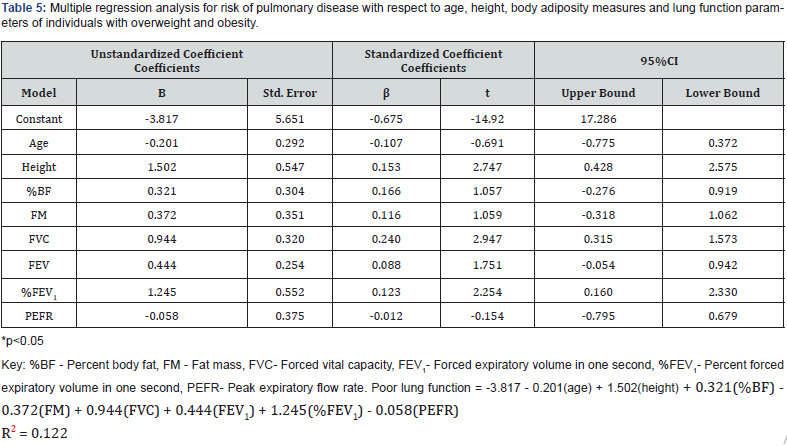
(Table 5) presents findings from the multiple regression analysis for the risk of pulmonary disease among individuals with overweight/obesity with respect to age, height, body adiposity measures and lung function parameters. For the prediction of risk of pulmonary disease with respect to age; an unstandardized coefficient beta of -0.201, t = -0.691 and confidence interval at 95% (C.I = -0.775-0.372). The results further showed that FEV1had an unstandardized coefficient beta of 0.254, t = 1.751 and confidence interval at 95% (C.I = -0.054-0.942). The prediction equation for poor lung function among individuals with overweight/obesity with respect to age, body adiposity measures and lung function parameters is presented as: Poor lung function = -3.817 - 0.201(age) + 1.502(height) + 0.321(%BF) - 0.372(FM) + 0.944(FVC) + 0.444(FEV1) + 1.245(%FEV1) - 0.058(PEFR)
R2 = 0.122
Discussion
The objective of this study was to assess the body adiposity measure, bodyweight status, lung function parameters and their relationships among young Nigerian women. Findings from the present study revealed that close to a third of participants in this study were either overweight or obese. This is consistent with findings of previous studies that citing increasing prevalence of overweight or obesity especially among young women [22,23]. Another plausible explanation for this may be the unprecedented changes in lifestyle factors among young people globally. The proliferation of fast-food outlets and consumption of large portions of food with high calories as well as reduced physical activity is presumed to contribute to the intake-output imbalance, which invariably lead to accumulation of fat and consequently resulting to obesity [24]. Moreover, several studies have reported gender differences in the level of physical activity between male and female gender at several points in life [25,26].
Findings from our study showed that measures of body adiposity were higher among individuals with overweight/obesity compared to those with normal weight. This is like findings of previous study that have shown that BMI, %BF and FM tend to be higher among individuals with overweight/obesity [4,27]. Excessive fat tissue is more likely to increase among individuals with sedentary lifestyle and those who also consume fatty food. And this may cause a decrease in chest wall compliance due to adipose tissue encasing the chest and abdomen. Thus, the effects of obesity could result to reduced lung functions and subsequently the development of pulmonary dysfunction.
Lung function parameters commonly used for the estimation of lung function are FVC, FEV1 and PEFR. Findings from our study revealed that reduced values were obtained when compared the norm reference value for female adults of similar age and physical characteristics. Already, previous studies have indicated that lung function is usually reduced among individuals with increased deposit of adipose tissue [28,29]. Furthermore, racial and ethnic differences in the values of lung function have been widely established. Generally, Caucasians tend to have higher lung function parameters than black Africans [30,31], with factors such as low socioeconomic status, low level of education, higher body fat, and marital status often cited as been responsible for these differences [32]. Additionally, body weight which may differ across racial and ethnic groups is known to have influence on lung volume and flow rates. Consequently, application of prediction formulae derived for outside the population of interest may lead to the over or under estimation of the values [33].
The results of this study also revealed that pulmonary function had a significant inverse relationship with variables such age, BMI, %BF, WC, HC and FM. We anticipate that an increased body fat is most likely a cause of lung function decline. This is because lung function is determined by the interactions between the lungs, chest wall compliance, respiratory muscle function, and peripheral airway size [34,35]. In this present study, participant’s height was significantly correlated with both FVC and FEV1. Expectedly, this finding is consistent with both old and recent reports that have indicated that height linearly correlates with lung size [36]. In contrast, variables such as the WC and HC were shown to have a significant, but negative correlation with the lung function parameters assessed. Most adiposity measures of this study were negatively correlated with lung function, especially among men [9].
Our findings have also shown that FVC is significantly reduced in underweight, overweight or obese individuals compared to individuals with normal BMI. This is consistent with the findings of Alaagib et al. [37], which states that underweight and obese individuals have significant reductions in FEV1 and FVC compared to individuals with normal weight. The WC has also been described to be negatively correlated with lung function, which is consistent with our findings. Another explanation may be that during normal respiration, mechanical contraction of the diaphragm leads to downward and forward movements of the abdominal content, while the external intercostal muscles contract to pull up the ribs upward and forward [38]. However, in individuals with obesity, this mechanism is impaired because the excess body fat that lines the chest and occupies the abdomen limits the action of the respiratory muscles. These structural changes in the thoracic-abdominal area tend to restrict diaphragmatic mobility and rib movement, which promotes changes in the dynamics of the respiratory system and reduces its compliance, leading to mechanical impairment of the respiratory muscles [39].
Finally, the findings of this study resulted in reference equations generated for young Nigerian women. This might be helpful in identifying young women at risk of pulmonary diseases especially, where facilities to perform lung function test are not readily available. More importantly, these equations might help rehabilitation programmers design appropriate preventive strategies for these patients. It is noteworthy to mention a few limitations in this study. This study utilized a cross-sectional design; hence inference cannot be made, and generalizability may be limited. Furthermore, lack of data regarding physical activity level, quality of air, housing living environment and socio-economic status are potentially external variables that are known to affect the outcome of studies of this nature. However, our study participants were university undergraduate young women who have similar conditions, i.e., were mostly within the same age range and residing within the university campus with better environmental condition.
Conclusion
It was concluded that young Nigerian women presented with high rates of abnormal bodyweight categories (underweight, overweight or obese) body adiposity measures that contributes negatively to their lung function parameters. These findings are of clinical significance in proposing preventive strategies that is relevant in the rehabilitation of young women with abnormal adiposity measures.
Acknowledgments
This research was supported by the Consortium for Advanced Research Training in Africa (CARTA). CARTA is jointly led by the African Population and Health Research Center and the University of the Witwatersrand and funded by the Carnegie Corporation of New York (Grant No. G-19-57145), Sida (Grant No:54100113), Uppsala Monitoring Center, Norwegian Agency for Development Cooperation (Norad), and by the Wellcome Trust [reference no. 107768/Z/15/Z] and the UK Foreign, Commonwealth & Development Office, with support from the Developing Excellence in Leadership, Training and Science in Africa (DELTAS Africa) programme. The statements made and views expressed are solely the responsibility of the Fellow.
References
- Hodgson LE, Murphy PB, Hart N (2015) Respiratory management of the obese patient undergoing surgery. J Thorac Dis 7(5): 943-952.
- World Health Organization. (2021) Obesity and overweight.
- Mafort TT, Rufino R, Costa CH, Lopes AJ (2016) Obesity: systemic and pulmonary complications, biochemical abnormalities, and impairment of lung function. Multidiscip Respir Med 11: 28.
- Sutherland TJT, McLachlan CR, Sears MR, Poulton R, Hancox RJ (2016) The relationship between body fat and respiratory function in young adults. Eur Respir J 48(3): 734-747.
- Global Burden of Disease Collaborative Network, Global Burden of Disease Study 2019 (GBD 2019) Results (2020, Institute for Health Metrics and Evaluation – IHME).
- Mohammed J, Adedoyin RA, Awotidebe TO, Onigbinde TA (2012) Influence of parental socioeconomic status on lung function indices of children in Ile - Ife. J Niger Soc Physiother 20: 67-72.
- Zammit C, Liddicoat H, Moonsie I, Makker H (2010) Obesity and respiratory diseases. Int J Gen Med 3: 335-343.
- Amirabdollahian F, Haghighatdoost F (2018) Anthropometric Indicators of Adiposity Related to Body Weight and Body Shape as Cardiometabolic Risk Predictors in British Young Adults: Superiority of Waist-to-Height Ratio. J Obes 2018: 8370304.
- Chen Y, Rennie D, Cormier Y F, Dosman J (2007) Waist circumference is associated with pulmonary functions in normal-weight, overweight, and obese subjects. Am J Clin Nutr 85(1): 35-39.
- Costa D, Barbalho MC, Miguel GP, Eli Maria PF, João Luiz Moreira CA (2008) The impact of obesity on pulmonary function in adult women. Clinics (Sao Paulo) 63(6): 719-724.
- Cortés-Télles A, Torre-Bouscoulet L, Silva-Cerón M, Mejía-Alfaro R, Syed N, et al. (2015) Combined effects of mild-to-moderate obesity and asthma on physiological and sensory responses to exercise. Respir Med 109(11):1397-1403.
- Müller MJ,BaracosV, Bosy-Westphal A, Dulloo A, Eckel J, Fearon KCH, Hall KD, et al. (2014) Functional Body Composition and Related Aspects in Research on Obesity and Cachexia. Obes Rev 15(8): 640-656.
- Shi H, Clegg DJ (2009) Sex differences in the regulation of body weight. Physiol Behav 97(2): 199-204.
- Peters U, Dixon AE (2018) The effect of obesity on lung function. Expert Rev Respir Med12(9): 755-767.
- Blaak E (2021) Gender differences in fat metabolism Curr Opin Clin Nutr Metab Care 4(6): 499-502.
- Kasiulevicius V, Sapoka V, Filipaviciute˙ R (2006) Sample size calculation in epidemiological studies. Gerontologija 7: 225-231.
- Awotidebe TO, Adeyeye VO, Ogunyemi SA, Bisiriyu LA, Adedoyin RA, et al. (2017) Joint predictability of physical activity and bodyweight status on health-related quality of life of patients with hypertension. J Exerc Rehabil 13(5): 588-598.
- Choy CS, Chan WY, Chen TL, Shih CC, Wu LC, et al. (2011) Waist circumference and risk of elevated blood pressure in children: a cross-sectional study. BMC Public Health 11: 613.
- Mbada CE, Adedoyin RA, Oluwasanmi A, Awotidebe TO (2015) Bioelectric impedance analysis versus prediction equations for percent body fat in healthy Nigerian adults: correlation or conflict. Arch Physiother Glob Res 19(2): 27-33.
- He H, Pan L, Du J, Jin Y, Wang L, et al. (2021) Effect of fat mass index, fat free mass index and body mass index on childhood blood pressure: a cross-sectional study in south China. Transl Pediatr 10(3): 541-551.
- American Thoracic Society (ATS) (1995) Standardization of spirometry. Am J Resp Crit Care Med 152(3): 1107-1136.
- Steyn NP, Mchiza ZJ (2014) Obesity and the nutrition transition in Sub-Saharan Africa. Ann NY Acad Sci 1311(1): 88-101.
- Adeloye D, Ige-Elegbede JO, Ezejimofor M, Owolabi EO, Nnenna E, et al. (2021) Estimating the prevalence of overweight and obesity in Nigeria in 2020: a systematic review and meta-analysis Ann Med 53(1): 495-507.
- Bhurosy T, Jeewon R (2014) Overweight and obesity epidemic in developing countries: A problem with diet, physical activity, or socioeconomic status? Sci World J 2014: 964236.
- Azevedo MR, Araujo CLP, Reichert FF, Siqueira FV, Da Silva MC, et al. (2007) Gender differences in leisure-time physical activity. Int J Public Health 52(1): 8-15.
- Awotidebe TO, Adedoyin RA, Olukoju IO, Adegbesan OA, Babalola JF, et al. (2014) Psychosocial correlates of physical activity participation among Nigerian University Students. Int J Sports Sci 4(6): 205-211.
- Ojoawo AO, Adeniran SA, Fatiregun O, Onagbiye S, Bamiwuye S (2013) Relationship between body circumferences and lung function tests among undergraduate students at a Nigerian university. Pak J Physiol 9(1): 3-6.
- Koziel S, Ulijaszek SJ, Szklarska A, Tadeusz B (2007) The effects of fatness and fat distribution on respiratory functions. Ann Hum Biol 34(1): 123-131.
- Littleton SW (2012) Impact of obesity on respiratory function. Respirology 17(1): 43-49.
- Braun L (2015) Race, ethnicity and lung function: A brief history. Can J Respir Ther 51(4): 99-101.
- Menezes AMB, Wehrmeister FC, Hartwig FP, Perez-Padilla R, Gigante DP, et al. (2015) African ancestry, lung function and the effect of genetics. Eur Respir J 45(6): 1582-1589.
- Johannessen A, Eagan TM, Omenaas ER, Bakke PS, Gulsvik A (2010) Socioeconomic risk factors for lung function decline in a general population. Eur Respir J 36(3): 480-487.
- Collen J, Greenburg D, Holley A, King C, Roop S, et al. (2010) Racial discordance in spirometry comparing four commonly used reference equations to the National Health and Nutrition Examination Study III. Resp Med 104(5): 705-711.
- Rubinstein I, Zamel N, DuBarry L, Hoffstein V (1990) Airflow limitation in morbidly obese, non-smoking men. Ann Intern Med 112(11): 828-832.
- Roman MA, Rossiter HB, Casaburi R (2016) Exercise, ageing and the lung. Eur Respir J 48(5): 1471-1486.
- Suzanne MB, David AA, Mark WC (1994) Pulmonary function test outcome in healthy Nawajo native American adolescents. Am J Resp Crit Care Med 150(4): 1150-1153.
- Alaagib NA, Sukkar MY (2017) Effect of Body Composition on Ventilation Parameters in a Group of Young Sudanese Females. Sudan J Med Sci 12(2): 78-88.
- Koo P, Gartman EJ, Sethi JM, McCool FD (2015) Physiology in Medicine: physiological basis of diaphragmatic dysfunction with abdominal hernias implications for therapy. Appl Physiol 118(2): 142-147.
- Unterborn J (2001) Pulmonary function testing in obesity, pregnancy, and extremes of body habitus. Clin Chest Med 22(4): 759-767.






























