P-Glycoprotein Inhibition Improves Imipramine Transport Across the Blood– Brain Barrier: Micro Dialysis Experiments in Conscious, Free-Moving Rats
Hari Prasad Sonwani*
Apollo College of Pharmacy, Anjora Durg C.G 491001, India
Submission: December 17, 2023; Published: January 05, 2024
*Corresponding Address: Hari Prasad Sonwani, Apollo College of Pharmacy, Anjora Durg CG, India
How to cite this article: Hari Prasad Sonwani*. P-Glycoprotein Inhibition Improves Imipramine Transport Across the Blood– Brain Barrier: Micro Dialysis Experiments in Conscious, Free-Moving Rats. Canc Therapy & Oncol Int J. 2024; 25(5): 556174. DOI:10.19080/CTOIJ.2024.25.556174
Abstract
Overview and Goals According to recent research, treatment-resistant depression (TRD) may be exacerbated by the multidrug resistance transporter P-glycoprotein (P-gp) at the blood-brain barrier (BBB) restricting intracerebral antidepressant efflux concentrations. Furthermore, clinical experience suggests that verapamil, a P-gp inhibitor, may be used as an adjuvant medication to enhance clinical outcomes in TRD. Consequently, the goal of the current investigation was to ascertain how P-gp inhibition affected the passage of imipramine, a tricyclic antidepressant, and its active metabolite, desipramine, across the blood-brain barrier.
An Experimental Method The levels of imipramine and desipramine in the rats’ brains were measured by intracerebral micro dialysis after imipramine was administered intravenously (IV), either with or without prior treatment with cyclosporin A (CsA) or verapamil, two P-gp inhibitors. Drug levels in plasma were also measured on a regular basis KEY RESULTS: Iripramine concentrations in the microdialysis samples increased significantly after pretreatment with either verapamil or CsA, but imipramine plasma pharmacokinetics remained unchanged. Furthermore, there was a significant increase in desipramine levels in the brain and plasma following pretreatment with verapamil, but not with CsA. SUMMARY AND IMPLICATIONS The current investigation supported the idea that P-gp activity limits the amounts of some antidepressants in the brain, including imipramine, by showing that P-gp inhibition increased the intracerebral concentration of imipramine. These findings may help to explain reports of a beneficial response to adjunctive therapy with verapamil in TRD.
Keywords: P-glycoprotein; Imipramine; Desipramine; Antidepressant; Blood-Brain barrier; Micro dialysis; Treatment-resistant, Depression
Introduction
Several antidepressants may be substrates of the multidrug resistance transporter P-glycoprotein (P-gp) at the blood–brain barrier (BBB), according to recent preclinical research [1,2]. P-gp, which the ABCB1 gene encodes in is expressed throughout the human body, including the brain’s capillary endothelial cells’ luminal membrane, which forms the blood-brain barrier (BBB) [3]. P-gp-mediated drug efflux at the blood-brain barrier (BBB) is a significant barrier to the brain’s uptake of pharmaceutical chemicals that are P-gp substrates. It has also been connected to treatment failure for several brain conditions, including brain cancer and epilepsy [4,5]. Numerous useful SNPs, or single nucleotide polymorphisms, in the It has been determined that the ABCB1 gene influences P-gp expression and/or function [6]. Therefore, the capacity of P-gp substrate medications to reach therapeutic concentrations in the brain may be impacted by these functional SNPs. According to newly available clinical data, the ABCB1 genotype may be linked to the response rate to antidepressant treatment, especially for those drugs that have been demonstrated to be P-gp substrates at the BBB in vivo [7-9]. This implies that by limiting antidepressant concentrations at their intracerebral site of action, P-gpmediated efflux may be a factor in the high prevalence of treatment-resistant depression (TRD) [1].
Furthermore, early clinical research indicates that co-administration of the P-gp inhibitor verapamil may be advantageous in treating TRD [10]. The relative contributions of P-gp-mediated efflux and passive permeability on the transport of these antidepressant drugs across the BBB have not yet been conclusively determined, and the significance of putative P-gp efflux to the BBB transport of antidepressants remains contentious, despite numerous in vivo studies showing enhanced brain levels of several antidepressants in P-gp knockout mice, compared with wild-type controls [1]. However, not all antidepressants are substrates of P-gp. Interestingly, the clinical response to mirtazapine is not linked to the ABCB1 genotype [7]. Mirtazapine is one such example [7,11]. It’s also important to recognize the complexity of the connection between antidepressants and P-gp and the challenges associated with extrapolating findings from one different experimental context [1]. The Pariante group’s work serves as an example of this point. There in vitro research suggested that P-gp activity at the BBB could be a target of antidepressant action [12,13], but more recent in vivo findings seem to refute this theory [14].
Only three such studies have been published to date, to our knowledge [10,15,16]. While many studies have examined the distribution of antidepressants to the brain in P-gp knockout mice relative to wild-type controls, there is a dearth of research investigating the effect of pharmacological P-gp inhibition on the ability of antidepressants to penetrate the BBB. It has been previously demonstrated that in some brain regions, pretreatment with verapamil increases the brain-to-serum ratios of imipramine, a tricyclic antidepressant, and its active metabolite, desipramine [10]. On the other hand, inconsistent results about the P-gp substrate status of imipramine have been obtained from in vitro transport studies utilizing several P-gp expressing cell lines [17,18]. Consequently, it is yet unknown if P-gp restricts imipramine’s capacity to cross the BBB. The time-dependent effect of P-gp inhibition on the distribution of these antidepressants into the brain has not been clarified by this earlier research in normal animals since they only looked at brain-to-serum ratios at a single (terminal) period after antidepressant treatment. The current investigation made use of an integrated intracerebral Using a micro dialysis technique, researchers examined how pretreatment with one of two different P-gp inhibitors - cyclosporin A (CsA) or verapamil - affected the concentrations of free imipramine and desipramine in the extracellular fluid (ECF) of the brain over time in wild-type Sprague Dawley rats. When it comes to the analysis of drug transporters in the central nervous system, intracerebral micro dialysis is a valuable investigative tool that may be used to evaluate drug permeability across the blood-brain barrier as a function of time [19] (Figures 1 & 2).

Discussion and Conclusion
Recent research indicates a possible connection between the therapeutic response of antidepressants, which have been demonstrated to be P-gp substrates, and functional SNPs in the ABCB1 gene, despite some contradictory results in the literature. encodes P-gp in humans, according to research conducted by Gex- Fabry et al. [20], Kato et al. [21], Nikisch et al. [22], Uhr et al. [7], Sarginson et al. [8], and Lin et al. [9]. The current investigation showed that, without altering imipramine levels in plasma, pretreatment with either of the well-known P-gp inhibitors verapamil or CsA dramatically raised levels of the tricyclic antidepressant imipramine in brain ECF. This suggests that because there may be species-specific variations in P-gp substrate, care should be used when extrapolating findings from preclinical rodent research to the clinical environment. particularity [23,24]. The increases in brain antidepressant levels mediated by P-gp inhibition happened without any notable changes to imipramine’s plasma pharmacokinetics. Clinical studies have shown that coadministration of verapamil after oral administration of imipramine in healthy volunteers increased imipramine bioavailability; this effect may have resulted from decreased imipramine clearance [24]. Iripramine’s plasma clearance was unaffected by verapamil pretreatment in the current investigation. A notable but slight rise in serum imipramine concentration was previously documented at a solitary (final) time-point after verapamil therapy [10].

The lack of observation of this effect in the current investigation may be attributed to the distinct routes of imipramine administration utilized in the two studies (i.p. from earlier research vs. i.v. in this study) or the various techniques for collecting samples (blood from the trunk after previous decapitation vs. indwelling catheter in the current investigation). Animals in the IMI + CsA group had an 84% greater dialysate: plasma imipramine AUC ratio than those in the IMI only group. The statistical significance of the observed difference indicates that rats treated with CsA have improved imipramine transport across the blood-brain barrier. The dialysate: plasma imipramine AUC ratio did not reach statistical significance, even though the IMI + VERAP group’s dialysate imipramine AUC was significantly higher than that of the IMI alone group. This is likely because of the increased variability observed when plasma concentrations were considered. Given that both P-gp inhibitors like CsA and verapamil are well-established [25]. These findings support our earlier research [10] and the theory that P-gp restricts the ability of some antidepressants, like imipramine, to cross the BBB [1].
Furthermore, it is important to remember that CsA is a more effective P-gp inhibitor than verapamil, as evidenced by the higher increase in brain imipramine levels seen in the CsA pretreatment group compared with verapamil pretreated animals [26]. To the best of our knowledge, this study is the first to use the microdialysis method to examine how P-gp inhibition affects antidepressant absorption and brain penetration across the blood-brain barrier. The method of microdialysis provides many benefits over conventional techniques that examine drug concentrations in brain homogenate samples [27,28]. First off, samples made from brain homogenates contain drug remaining in the blood in the network of capillaries throughout the brain, but samples made using the microdialysis technique only contain drug that has crossed the blood-brain barrier. Second, although the classic brain homogenate approach often does not distinguish between pharmacologically inactive bound and active unbound drug, microdialysis measures only free drug molecules in the brain ECF. Thirdly, the microdialysis methodology provides temporal resolution not achievable with homogenate-based methods by tracking changes in brain drug concentrations in individual animals over time with or without P-gp inhibition. Furthermore, we may use microdialysis to investigate how P-gp inhibition affects drug concentrations in a particular target brain region, such the PFC. Although brain homogenate techniques can be utilized for region-specific analysis [10], most of the prior research has concentrated on total brain concentrations of antidepressant drugs rather than examining effects that are particular to a given region. Given that P-gp expression and function vary throughout several brain anatomical regions, this is a significant research restriction [10,29].
Therefore, it’s possible that significant region-specific variations in drug concentrations were hidden by the earlier use of whole brain analysis. When comparing amounts of dialysate that have not been adjusted for in vivo probe recovery in It is crucial to keep in mind that changing drug clearance by P-gp inhibition is probably going to have an impact on probe recovery in microdialysis experiments examining the impact of P-gp efflux on the net BBB transport of a drug [12]. Nevertheless, in vivo probe recovery should be less in rats receiving a P-gp inhibitor than in animals not receiving treatment [30], and this has been demonstrated in experiments [31,32]. Consequently, we would probably observe an even more pronounced increase in brain imipramine if it were able to adjust our dialysate concentrations for in vivo recovery and so determine actual brain ECF imipramine concentrations. levels in the animals medicated with verapamil and CsA compared to the untreated controls. It is challenging to compare the magnitude of increases in brain imipramine concentrations reported here with those previously reported in other studies that have investigated the effect of P-gp inhibition on the BBB transport of antidepressants because of the different methodology used in this study. It will also be interesting to examine the implications of these findings for human patients receiving long-term antidepressant treatment. It’s interesting to note that pretreatment with verapamil significantly raised the levels of desipramine in plasma, which is an active metabolite of imipramine and an independent antidepressant. Compared to the IMI only group, the IMI + VERAP group’s mean AUC for desipramine in plasma was more than four times higher. metabolic enzymes, transporters, and receptors [33-36].
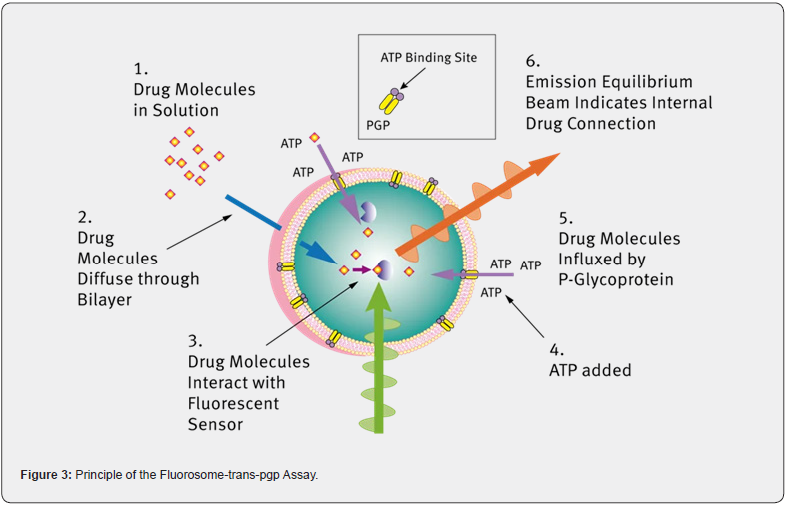
Furthermore, pharmacokinetics of several medications has been demonstrated to be altered by verapamil [37-40]. Therefore, rather than via P-gp inhibition, it appears plausible that one of these alternative interactions may be the mechanism mediating the increase in plasma desipramine levels. Verapamil has been specifically identified as an inhibitor of cytochrome P450 enzymes [36], which are primarily involved in the metabolism of imipramine and desipramine in humans [41]. Although imipramine plasma clearance was unaffected by co-administration of verapamil the rise in The IMI + VERAP group’s plasma desipramine levels may have been caused by verapamil-mediated inhibition of desipramine metabolism. Furthermore, it is important to remember that the brain has a functioning cytochrome P450 monooxygenase system [42-44]. Verapamil’s alleged suppression of these enzymes may therefore have an impact on drug levels in the brain. Desipramine levels in micro dialysis samples could only be accurately measured in animals’ pretreatment with verapamil, indicating higher levels in these animals [45-50]. These results were consistent with the elevated levels of desipramine in the brain seen in the IMI + VERAP group. It is unclear if the therapeutic advantages of verapamil augmentation in TRD [10] are related to this rise in brain desipramine concentrations. But it’s important to remember that after oral imipramine treatment, verapamil co-administration had no influence on desipramine concentrations in plasma, according to clinical research conducted in healthy volunteers [24,51- 57]. As a result, the rise in desipramine levels after verapamil pretreatment in rats given imipramine intravenously may not apply to people taking imipramine orally. It was not feasible to ascertain if pretreatment with either P-gp inhibitor altered the BBB transport of desipramine since desipramine concentrations in dialysate samples from the IMI only or IMI + CsA groups could not be quantified (Figure 3).
In summary
The current investigation unequivocally showed that pretreatment with P-gp inhibitors, verapamil or CsA, raised the levels of the antidepressant imipramine in the brains of normal rats. This demonstrates Overpass the BBB. These results add to the growing body of clinical data suggesting P-gp blocks several antidepressants from acting at their sites of action in the brain by preventing them from reaching effective concentrations. Such outcomes may be a factor in the increased incidence of TRD. Given these results, one could be tempted to hypothesize that P-gp inhibitor supplementary medication could be beneficial for treating depression clinically.
Conflicts of Interest
None.
References
- O’Brien FE, Dinan TG, Griffin BT, Cryan JF (2012) Interactions between antidepressants and P-glycoprotein at the blood-brain barrier: Clinical significance of in vitro and in vivo findings. Br J Pharmacol 165(2): 289-312.
- Alexander SPH, Mathie A, Peters JA (2011) Guide to Receptors and Channels (GRAC), (5th). Br J Pharmacol 164(Suppl. 1): S1-S324.
- Cordoncardo C, O’Brien JP, Casals D, Rittmangrauer L, Biedler JL, et al. (1989) Multidrug-resistance gene(P-glycoprotein) is expressed by endothelial-cells at blood-brainbarrier sites. Proc Natl Acad Sci U S A 86(2): 695-698.
- Siddiqui A, Kerb R, Weale ME, Brinkmann U, Smith A, et al. (2003) Association of multidrug resistance in epilepsy with a polymorphism in the drug-transporter gene ABCB1. N Engl J Med 348(15): 1442-1448.
- Pauwels EKJ, Erba P, Mariani G, Gomes CMF (2007) Multidrug resistance in cancer: its mechanism and its modulation. Drug News Perspect 20(6): 371-377.
- Cascorbi I (2006) Role of pharmacogenetics of ATP-binding cassettetransporters in the pharmacokinetics of drugs. Pharmacol Ther 112(2): 457-473.
- Uhr M, Tontsch A, Namendorf C, Ripke S, Lucae S, et al. (2008) Polymorphisms in the drug transporter gene ABCB1 predict antidepressant treatment response in depression. Neuron 57(2): 203-209.
- Sarginson JE, Lazzeroni LC, Ryan HS, Ershoff BD, Schatzberg AF, et al. (2010) ABCB1 (MDR1) polymorphisms andantidepressant response in geriatric depression. Pharmacogenet Genomics 20(8): 467-475.
- Lin KM, Chiu YF, Tsai IJ, Chen CH, Shen WW, et al. (2011) ABCB1 gene polymorphisms are associated with the severity of major depressive disorder and its response to escitalopram treatment. Pharmacogenet Genomics 21(4): 163-170.
- Clarke G, O’Mahony SM, Cryan JF, Dinan TG (2009) Verapamil intreatment resistant depression: a role for the P-glycoproteintransporter? Hum Psychopharmacol 24(3): 217-223.
- Uhr M, Grauer MT, Holsboer F (2003) Differential enhancement of antidepressant penetration into the brain in mice with abcb1ab (mdr1ab) P-glycoprotein gene disruption. Biol Psychiatry 54(8): 840-846.
- Pariante CM, Kim RB, Makoff A, Kerwin RW (2003) Antidepressant fluoxetine enhances glucocorticoid receptor function in vitro by modulating membrane steroid transporters. Br J Pharmacol 139(6): 1111-1118.
- Pariante CM, Thomas SA, Lovestone S, Makoff A, Kerwin RW (2004) Do antidepressants regulate how cortisol affects the brain? Psychoneuroendocrinology 29(4): 423-447.
- Mason BL, Thomas SA, Lightman SL, Pariante CM (2011) Desipramine treatment has minimal effects on the brain accumulation of glucocorticoids in P-gp-deficient and wild-type mice. Psychoneuroendocrinology 36(9): 1351-1360.
- Ejsing TB, Linnet K (2005) Influence of P-glycoprotein inhibitionon the distribution of the tricyclic antidepressant nortriptyline over the blood-brain barrier. Hum Psychopharmacol 20(2): 149-153.
- Ejsing TB, Hasselstrom J, Linnet K (2006) The influence of P-glycoprotein on cerebral and hepatic concentrations ofnortriptyline and its metabolites. Drug Metabol Drug Interact 21: 139-162.
- Mahar Doan KM, Humphreys JE, Webster LO, Wring SA, Shampine LJ, Serabjit-Singh CJ et al. (2002) Passive permeabilityand P-glycoprotein-mediated efflux differentiate central nervoussystem (CNS) and non-CNS marketed drugs. J Pharmacol Exp Ther 303(3): 1029-1037.
- Faassen F, Vogel G, Spanings H, Vromans H (2003) Caco-2permeability, P-glycoprotein transport ratios and brain penetration of heterocyclic drugs. Int J Pharm 263: 113-122.
- Sawchuk RJ, Elmquist WF (2000) Microdialysis in the study of drugtransporters in the CNS. Adv Drug Deliv Rev 45: 295-307.
- Gex-Fabry M, Eap CB, Oneda B, Gervasoni N, Aubry JM, et al. (2008) CYP2D6 and ABCB1 genetic variability: influence onparoxetine plasma level and therapeutic response. Ther Drug Monit 30(4): 474-482.
- Kato M, Fukuda T, Serretti A, Wakeno M, Okugawa G, et al. (2008) ABCB1 (MDR1) gene polymorphisms are associatedwith the clinical response to paroxetine in patients with majordepressive disorder. Prog Neuropsychopharmacol Biol Psychiatry 32(2): 398-404.
- Nikisch G, Eap CB, Baumann P (2008) Citalopram enantiomers in plasma and cerebrospinal fluid of ABCB1 genotyped depressive patients and clinical response: a pilot study. Pharmacol Res 58: 344-347.
- Yamazaki M, Neway WE, Ohe T, Chen I, Rowe JF, et al. (2001) In vitro substrate identification studies for p-glycoprotein-mediated transport: species difference and predictability of in vivo results. J Pharmacol Exp Ther 296(3): 723-735.
- Hermann DJ, Krol TF, Dukes GE, Hussey EK, Danis M, et al. (1992) Comparison of verapamil, diltiazem, and labetalol on thebioavailability and metabolism of imipramine. J Clin Pharmacol 32(2): 176-183.
- Baumert C, Hilgeroth A (2009) Recent advances in the development of P-gp inhibitors. Anticancer Agents Med Chem 9(4): 415-436.
- Hsiao P, Bui T, Ho RJ, Unadkat JD (2008) In vitro-to-in vivoprediction of P-glycoprotein-based drug interactions at the humanand rodent blood-brain barrier. Drug Metab Dispos 36(3): 481-484.
- De Lange ECM, De Boer AG, Breimer DD (2000) Methodological issues in microdialysis sampling for pharmacokinetic studies. Adv Drug Deliv Rev 45: 125-148.
- Hammarlund-Udenaes M (2010) Active-site concentrationsof chemicals - are they a better predictor of effect thanplasma/organ/tissue concentrations? Basic Clin Pharmacol Toxicol 106(3): 215-220.
- Kwan P, Sills GJ, Butler E, Gant TW, Brodie MJ (2003) Differential expression of multidrug resistance genes in naive rat brain. Neurosci Lett 339(1): 33-36.
- Bungay PM, Morrison PF, Dedrick RL (1990) Steady-state theory forquantitative microdialysis of solutes and water in vivo and in vitro. Life Sci 46(2): 105-119.
- De Lange EC, De Bock G, Schinkel AH, De Boer AG, Breimer DD (1998) BBB transport and P-glycoprotein functionality using MDR1A (-/-) and wild-type mice. Total brain versus microdialysisconcentration profiles of rhodamine-123. Pharm Res 15(11): 1657-1665.
- Xie R, Hammarlund-Udenaes M, De Boer AG, De Lange EC (1999) The role of P-glycoprotein in blood-brain barrier transport of morphine: transcortical microdialysis studies in mdr1a (-/-) and mdr1a (+/+) mice. Br J Pharmacol 128(3): 563-568.
- Auguet M, Delaflotte S, Clostre F, Defeudis FV (1986) Verapamil asan apparent competitive antagonist of the serotonin receptor ofrabbit isolated aorta. Gen Pharmacol 17(2): 133-135.
- Cole SPC, Loe DW, Deeley RG (2000) Verapamil stimulatesglutathione transport by the 190-kDa multidrug resistance protein1 (MRP1). J Pharmacol Exp Ther 293(2): 530-538.
- Paxinos G, Watson C (1998) The Rat Brain in Stereotaxic Coordinates, (4th) Academic Press: San Diego. Polasek TM, Elliot DJ, Lewis BC, Miners JO (2004) Mechanism based inactivation of human cytochrome P4502C8 by drugs invitro. J Pharmacol Exp Ther 311(3): 996-1007.
- Wang YH, Jones DR, Hall SD (2004) Prediction of cytochrome P450 3A inhibition by verapamil enantiomers and their metabolites. Drug Metab Dispos 32(2): 259-266.
- Backman JT, Olkkola KT, Aranko K, Himberg JJ, Neuvonen PJ (1994) Dose of midazolam should be reduced during diltiazem andverapamil treatments. Br J Clin Pharmacol 37(3): 221-225.
- Kantola T, Kivisto KT, Neuvonen PJ (1998) Erythromycin andverapamil considerably increase serum simvastatin and simvastatincid concentrations. Clin Pharmacol Ther 64(2): 177-182.
- Fleishaker JC, Sisson TA, Carel BJ, Azie NE (2000) Pharmacokinetic interaction between verapamil and almotriptan in healthyvolunteers. Clin Pharmacol Ther 67(5): 498-503.
- Kovarik JM, Beyer D, Bizot MN, Jiang Q, Allison MJ, et al. (2005) Pharmacokinetic interaction between verapamil andeverolimus in healthy subjects. Br J Clin Pharmacol 60(4): 434-437.
- Lemoine A, Gautier JC, Azoulay D, Kiffel L, Belloc C, et al. (1993) Major pathway of imipramine metabolism is catalyzed by cytochromes P-450 1A2 and P-450 3A4 in human liver. Mol Pharmacol 43(5): 827-832.
- Baltes S, Gastens AM, Fedrowitz M, Potschka H, Kaever V, et al. (2007) Differences in the transport of the antiepilepticdrugs phenytoin, levetiracetam and carbamazepine by human andmouse P-glycoprotein. Neuropharmacology 52(2): 333-346.
- Ravindranath V (1998) Metabolism of xenobiotics in the centralnervous system: implications and challenges. Biochem Pharmacol 56(5): 547-551.
- Bart J, Willemsen AT, Groen HJ, Van Der Graaf WT, et al. (2003) Quantitative assessment of P-glycoproteinfunction in the rat blood-brain barrier by distribution volume of[11C] verapamil measured with PET. Neuroimage 20(3): 1775-1782.
- Colabufo NA, Berardi F, Cantore M, Contino M, Inglese C, et al. (2010) Perspectives of P-glycoprotein modulating agents inoncology and neurodegenerative diseases: pharmaceutical, biological, and diagnostic potentials. J Med Chem 53(5): 1883-1897.
- Evrard PA, Ragusi C, Boschi G, Verbeeck RK, Scherrmann JM (1998) Simultaneous microdialysis in brain and blood of the mouse: Extracellular and intracellular brain colchicine disposition. Brain Res 786: 122-127.
- Frahnert C, Rao ML, Grasmader K (2003) Analysis of eighteenantidepressants, four atypical antipsychotics and active metabolitesin serum by liquid chromatography: a simple tool for therapeuticdrug monitoring. J Chromatogr B Analyt Technol Biomed Life Sci 794(1): 35-47.
- Friedl W, Propping P (1984) 3H-imipramine binding in humanplatelets: a study in normal twins. Psychiatry Res 11(4): 279-285.
- Heiser A (2007) Rat Jugular Vein and Carotid ArteryCatheterization for Acute Survival Studies: A Practical Guide, (1st) Springer: New York.
- Huang C, Yoshimoto M, Miki K, Johns EJ (2006) The contribution of brain angiotensin II to the baroreflex regulation of renalsympathetic nerve activity in conscious normotensive and hypertensive rats. J Physiol 574: 597-604.
- Liow JS, Lu S, McCarron JA, Hong J, Musachio JL, et al. (2007) Effect of a P-glycoprotein inhibitor, Cyclosporin A, on the disposition in rodent brain and blood of the 5-HT1A receptor radioligand, [11C] (R)- (-) -RWAY. Synapse 61(2): 96-105.
- Page ME, Lucki I (2002) Effects of acute and chronic reboxetine treatment on stress-induced monoamine efflux in the rat frontal cortex. Neuropsychopharmacology 27: 237-247.
- Page ME, Bao L, Andre P, Pelta-Heller J, Sluzas E, et al. (2010) Cell-autonomous alteration of dopaminergic transmission by wild type and mutant (DeltaE) TorsinA in transgenic mice. Neurobiol Dis 39(3): 318-326.
- Sato Y, Shibanoki S, Sugahara M, Ishikawa K (1994) Measurement and pharmacokinetic analysis of imipramine and its metabolite by brain micro dialysis. Br J Pharmacol 112(2): 625-629.
- Syvanen S, Blomquist G, Sprycha M, Hoglund AU, Roman M, et al. (2006) Duration and degree of cyclosporin induced P-glycoprotein inhibition in the rat blood-brain barrier can be studied with PET. Neuroimage 32(3): 1134-1141.
- Thrivikraman KV, Huot RL, Plotsky PM (2002) Jugular vein catheterization for repeated blood sampling in the unrestrained conscious rat. Brain Res Brain Res Protoc 10(2): 84-94.
- Tsai TH, Liu SC, Tsai PL, Ho LK, Shum AY, et al. (2002) The effects of cyclosporin A, a P-glycoprotein inhibitor, on the pharmacokinetics of baicalein in the rat: a microdialysis study. Br J Pharmacol 137(8): 1314-1320.






























