Evaluation of PreTBI (Total Body Irradiation) and PosTBI Fatigue Severity Scale Scores in the ALL (Acute Lymphocytic Leukemia) Patients Preparing for Stem Cell Transplant
Bora Uysal*, Hakan Gamsiz and Murat Beyzadeoglu
University of Health Sciences, Gulhane Medical Faculty, Department of Radiation Oncology, Ankara, Turkey
Submission: July 28, 2022; Published: August 15, 2022
*Corresponding Address: Bora Uysal, MD, Asc. Professor of Radiation Oncology, University of Health Sciences, Gulhane Medical Faculty, Department of Radiation Oncology, 06010, Ankara, Turkey
How to cite this article: Bora U, Hakan G, Murat B. Evaluation of PreTBI (Total Body Irradiation) and PosTBI Fatigue Severity Scale Scores in the ALL (Acute Lymphocytic Leukemia) Patients Preparing for Stem Cell Transplant. Canc Therapy & Oncol Int J. 2022; 22(2): 556081. DOI:10.19080/CTOIJ.2022.22.556081
Abstract
TBI is used before stem cell transplantation for conditioning in ALL patients. We aimed to analyze the FSS scores before and after TBI for the patients consulted to our department between 2015 and 2020. Patients were asked to reply 9 questions before and after TBI with verbal or written form. 60 patients received TBI in 3 days without interruptions. 24 (40%) patients were male and 36 (60%) of all were female. Median age was 11 (6-17) years. The score over 36 means that the patient is needed to be evaluated by physician. The fatigue score of all group before TBI was median 42 (36-50). Post TBI score of all patients was 55 (48-61) and this was statistically significant (p<0.05).
Keywords: Fatigue; ALL; TBI
Abbreviations: ALL: Acute Lymphocytic Leukemia; TBI: Total Body Irradiation; FSS: Fatigue severity scale
Introduction
TBI (total body irradiation) was used without stem cell support for chronic lymphocytic leukemia or follicular lymphomas historically. Cytotoxic and immunological effects are the main goal of TBI for the hematopoietic transplantation. Allogeneic or autologous transplantation mean donor cells coming from another patient or patient’s pool respectively. Syngeneic transplantation means stem cells coming from identical twins. Hemibody irradiation is used for palliation of metastatic disease whereas stem cell support not needed. TBI has been used for malignant diseases in early 1900’s but lethal dose with radiation exposure limited its use only along with hematopoietic stem cell transplantation. Cytotoxicity, immunsuppresion are the major functions of TBI for conditioning regimen in hematopoietic stem cell transplantation. Eradicating bone marrow gains recovery of new cells. Immunsuppresion causes preventing rejection.
Fractionated TBI was found less effective than single dose TBI in a study by Storb et al. DNA damage was repaired by lymphoid cells during fractionation. Salomon analyzed three different models including 8.5 Gy single dose, 2 Gy times 6 fractions TBI and 1.2 Gy times hyperfractionated TBI. Single dose TBI was better in terms of immunsuppresion compared to other modalities. More graft rejections might occur after fractionated TBI. 10 Gy single dose TBI is roughly equivalent to 13-15 Gy fractionated TBI according to the literature. Dose rate, fractional dose, dose scheme, comorbid diseases and other diseases may be the factors that change the hematological variation in the preparing population for stem cell transplant. Acute toxicities of TBI are fatigue, nausea, vomiting, diarrhea, xerostomia, headache, fever, hypertension, dry mouth, oral mucositis, parotidis, alopecia. Delayed toxicities are interstitial pneumonitis, veno-occlusive disease of liver, cataract, renal toxicity, growth hormone deficiency, thyroid dysfunction, secondary cancers.
Materials and Methods
Between 2015 and 2020, 60 patients whose diagnosis was ALL (acute lymphocytic leukemia) were asked to tell their fatigue severity scale scores before and after TBI. They all received 12 Gy hyperfractionated TBI in 6 fractions, 2 Gy in 3 days with 6-hour gap between daily 2 fractions at a low dose rate of 1.59- 7.95 cgy/min with co60 1.25 mev teletherapy machine at SAD equal to 370-413.5 cm and diagonal field sizes 174.5-195 cm. The target volume was the entire body fitting into the limited size radiation field. Homogeneous dose distributions to all sites and limiting dose to the critical organs were the major challenging issues about treatment planning and radiation delivery. Daily positioning was reproducible over optimal dose distribution with technique that include thin body sites such as head, neck and legs. Bolus was used for homogenization. Patients lied supine with legs on a mobile couch. The head and neck were supported, and partial lung shielding was established.
Fatigue Severity Scale (FSS)
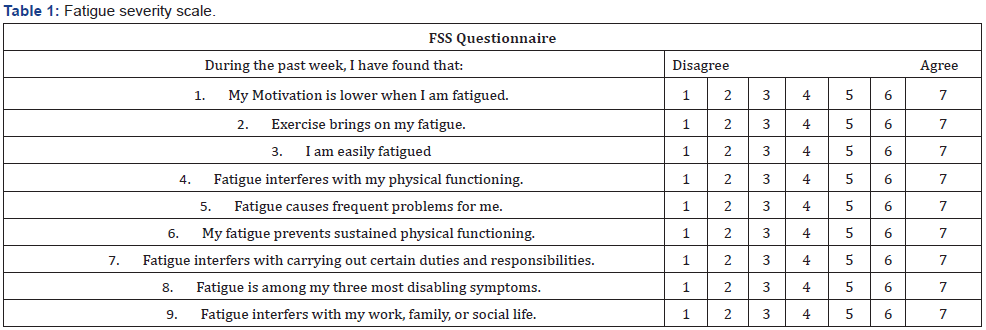
Fatigue Severity Scale (FSS) is a method of evaluating the impact of fatigue on patients. The FSS is a short questionnaire that requires the patient to rate the level of fatigue. The FSS questionnaire contains nine statements that rate the severity of fatigue symptoms. Patients read each statement and circle a number from 1 to 7, based on how accurately it reflects their condition during the past week and the extent to which they agree or disagree that the statement applies to them. A low value (e.g., 1) indicates strong disagreement with the statement, whereas a high value (e.g., 7) indicates strong agreement. All patients were given fatigue severity scale questionnaire before and after TBI. The results get from their verbal or written consent were recorded for analysis. Informed consent was provided for each patient in the study along with Helsinki Declaration.
Statistical Analysis
All statistical analyses were performed using standard software (SPSS version 22; SPSS Inc. Chicago, IL, USA). The primary outcomes of interest were association of fatigue severity scores with fractionated radiotherapy. The x2 test or students t-test were used to analyze the differences in clinical and pathological factors. Univariate analysis was performed via the log-rank test. Multivariate analysis was performed using the Cox proportional hazards model, using covariates with a p<0.10 based on univariate analysis. All p<0.05 were considered statistically significant.
Results
60 patients received TBI in 3 days without interruptions. 24 (40%) patients were male and 36 (60%) of all were female. Median age was 11 (6-17) years. The score over 36 means that the patient is needed to be evaluated by physician. The fatigue score of all group before TBI was median 42 (36-50). Post TBI score of all patients was 55 (48-61) and this was statistically significant (p<0.05). 90 % (54) of patients were answered 1st., 4th, 8th and 9th questions with a score of 7 points before and after TBI (Table 1). The scores of the questions’ 2nd, 5th, 6th and 7th were increased from median 3 (2-6) to median 6 (5-7) before TBI and after TBI respectively. The 3rd question ‘I am easily fatigued’ was answered with 7 points before and after TBI by all participants (100 %-60).
Discussion
Only chemotherapeutic option for conditioning in Acute Lymphoblastic Leukemia was recently analyzed recently in 2021. It was also an option to select TBI or conditioning chemotherapy for immunesuppresion and bone marrow ablation. Long term effects including secondary malignancies, cardiac or metabolic effects guided researchers to use myeloablative regimens such as busulfan or treosulfan. Encouraging but not 100 % similar results were shown after this study [1]. Pulmonary, ocular, cardiac, neurological or renal toxicities may be seen after TBI but these are manageable. 12 Gy regimen is suitable and long term sequelaes are grade 1 or 2 and limited with ocular or mucosal [2]. In a study with 110 patients, no secondary malignancies and acute or late cardiac effects were seen but menopausal syndrome, lung fibrosis and erectile dysfunction were shown in this population. Most frequent late reaction was actually GVHD (graft versus host disease) of the skin. Sophisticated radiation modalities will allow for decreasing organ toxicity for the stem cell transplant patients [3].
Animal study by Jackson et al was managed in 20 white rabbits. The hematological parameters 1 week after TBI showed thrombocytopenia and hemorrhagic syndrome with severe acute anemias. Efficacy screening, blood parameter follow-up should be done for TBI patients [4]. TBI is superior to chemotherapy about conditioning regimen with better leukemia free survival and overall survival. Its worst adverse effect is increased pulmonary toxicity [5]. Reduced toxicity myeloablative conditioning consisting of 8 Gy TBI, fludarabine and cyclophosphamide was used for pediatric patients. It offers high probability of survival and less toxicity with 80 % and 71 % 5-year overall survival and relapse free survival respectively [6]. TMI (total marrow irradiation) is a viable alternative to TBI. Helical tomotherapy uses its advantage of delivering intensity modulated radiotherapy to entire bone marrow. Acute toxicity was low and graft versus host disease free survival was higher than literature [7-9].
Biological results of the absorbed dose are dependent on type of radiation exposure and total volume irradiated [10]. A younger age <6 and the sequence of chemotherapy regimen before radiotherapy were associated with acute hematological toxicity in a study population treated at the M.D. Anderson Cancer Center. No treatment interruptions were seen, and all finished their schemes. CSI (craniospinal irradiation) with the electron technique was similar and alternative to photon CSI in younger patients [11]. The fatigue severity scale was used in our study to evaluate the patients’ physical discomfort before and after TBI. The literature actually focused on acute and chronic effects on TBI and stem cell transplantation. We aimed to analyze patients’ fatigue scores along with radiation. Fatigue scoring scale should be applied with more center and patient to guide and give recommendations for physical discomfort.
Conflict of Interest
No
References
- Hassine K, Powys M, Svec P, Miroslava Pozdechova, Birgitta Versluys et al. (2021) Total body irradiation forever? Optimising chemotherapeutic options for irradiation free conditioning for paediatric acute lymphoblastic leukemia. Front Pediatr 9: 775485.
- Oertel M, Martel J, Mikesch J, Sergiu Scobioala, Christian Reicherts, et al. (2021) The burden of survivorship on hematological patients long term analysis of toxicities after total body irradiation and allogeneic stem cell transplantation. Cancers 13(22): 5640.
- Marnitz S, Zich A, Martus P, Volker Budach, Ulrich Jahn, et al. (2014) Long term results of total body irradiation in adults with acute lymphoblastic leukemia. Strahlenther Onkol 190(5): 453-458.
- Jackson I, Gurung G, Poirier Y, Mathangi Gopalakrishnan, Eric P Cohen, et al. (2021) A New Zealand white rabbit model of thrombocytopenia and coagulopathy following total body irradiation across the dose range to induce the hematopoietic subsyndrome of acute radiation syndrome. Int J Radiat Biol 97(1): S19-S31.
- Stephens S, Thomas S, Rizzieri D, Mitchell E Horwitz, Nelson J Chao, et al. (2016) Myeloablative conditioning with total body irradiation for AML: balancing survival and pulmonary toxicity. Adv Radiat Oncol 1(4): 272-280.
- Hirabayashi K, Nakazawa Y, Sakashita K, Takashi Kurata, Shoji Saito, et al. (2014) Reduced toxicity myeloablative conditioning consisting of 8 Gy total body irradiation, cyclophosphamide and fludarabine for pediatric hematological malignancies. Sci Rep 4: 6942.
- Haraldsson A, Wichert S, Engstrom P, Stig Lenhoff, Dominik Turkiewicz, et al. (2021) Organ sparing total marrow irradiation compared to total body irradiation prior to allogeneic stem cell transplantation. Eur J Haematol 107(4): 393-407.
- Konishi T, Ogawa H, Najima Y, Shinpei Hashimoto, Atsushi Wada, et al. (2020) Safety of total body irradiation using intensity modulated radiation therapy by helical tomotherapy in allogeneic hematopoietic stem cell transplantation: a prospective pilot study. J Radiat Res 61(6): 969-976.
- Shinde A, Yang D, Frankel P, An Liu, Chunhui Han, et al. (2019) Radiation related toxicities using organ sparing total marrow irradiation transplant conditioning regimens. Int J Radiat Oncol Biol Phys 105(5): 1025-1033.
- Jackson I, Gibbs A, Poirier Y, Lynne Wathen, John Eley, et al. (2019) Hematological effects of nonhomogenous ionizing radiation exposure in a nonhuman primate model. Radiat Res 191(5): 428-438.
- Chang E, Allen P, Wu C, Joann Ater, John Kuttesch, et al. (2002) Acute toxicity and treatment interruption related to electron and photon craniospinal irradiation in pediatric patients treated at the University of Texas M.D. Anderson Cancer Center. Int J Radiat Oncol Biol Phys 52(4): 1008-1016.






























