Imaging of Herpetic Meningoencephalitis. A Short Illustrated Focus
Chérif Mohamadou Aidara1*, Abdoulaye Dione Diop1, Géro Akpo2, Hamidou Deme2, Nfally Badji2, Abdoulaye Ndoye Diop2, Sokhna Ba2 and El Hadji Niang2
1Radiology Office of Fann University Hospital, Dakar-Fann, Sénégal
2Radiology Office of Aristide Le Dantec University Hospital, Dakar Plateau Senegal
Submission: February 07, 2019; Published: February 28, 2019
*Corresponding author:Chérif Mohamadou Aidara, Radiology Office of Fann University Hospital, Dakar-Fann, Sénégal, West Africa
How to cite this article:Chérif Mohamadou Aidara, Abdoulaye Dione Diop, Géro Akpo, Hamidou Deme, et al. Imaging of Herpetic Meningoencephalitis.A Short Illustrated Focus. Curr Trends Clin Med Imaging. 2019; 2(5): 555601. DOI: 10.19080/CTCMI.2019.02.555601
Intrоductiоn
Herpetic meningo encephalitis (HME) is a sporadic, non-epidemic acute disease with an incidence of approximately 1 to 3 cases per million [1,2]. 95% of fatal cases in adults are due to Herpes Simplex Virus type 1. In neonatal period and children Herpes Simplex Virus type 2 is most often the culprit (80 to 90%).

The virus reaches the nervous system via the respiratory tract and then the trigeminal ganglion where it becomes latent in non immunocompromise patients [1,3]. The reactivation of the virus would be secondary to a decrease immunity due to genetic mutation on neurons and oligidendrocytes altering interferon production which normally inhibits viral replication [3,4]. This situation probably explains the preferential involvement of internal temporal lobe (early in the course) because of the anatomical proximity with the meckel’s cavum that houses the trigeminal ganglion (Figure 1) [1,5]. Extratemporal involvement only is also possible [2].
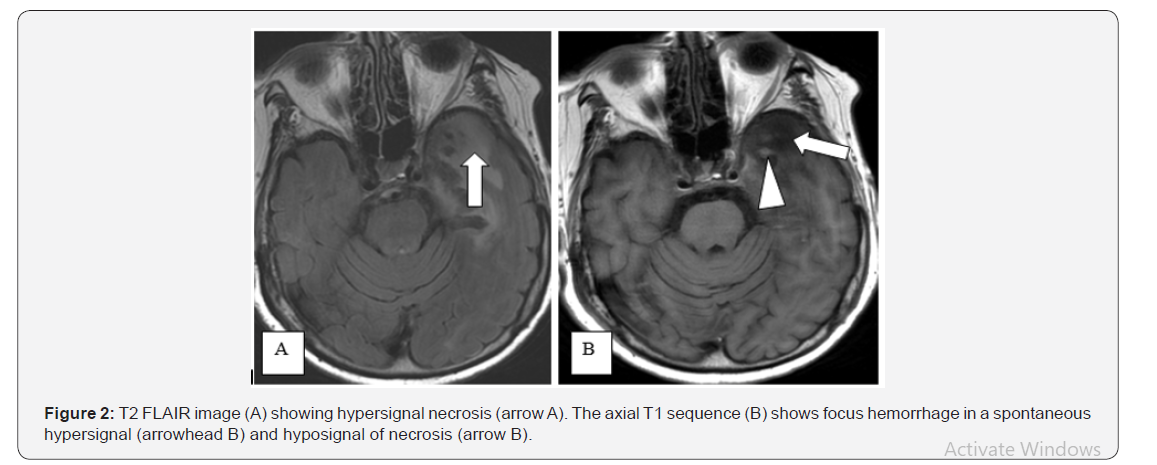
HME is an infectious, necrotizing and haemorrhagic (Figure 2) involvement of the brain parenchyma that is classically bilateral and asymmetrical. It may be associated with a meningeal involvement [2] (Figure 3). The usual clinical presentation associates acute or subacute behavioral disturbances, focal or generalized convulsions, focal neurological signs, cognitive disorders with headaches and infectious syndrome [2,3,6]. Aseptic meningitis can also be revealing. Signs of bradycardia, hypotension, syncope and hypothermia are related to hypothalamic involvement [5]. MRI is the most sensitive imaging current technique and plays a key role in diagnostic and follow-up. MRI imaging can guide the diagnosis early. It typically shows bilateral, asymmetrical involvement of the brain predominantly in the limbic system (medial temporal lobe, insular cortex, cingular gyrus, infero-lateral frontal lobe), with or without extension to the basal ganglia and the other lobes (Figure 3). Diencephalon and brain stem involvement are possible [1] Bonnici-Malia reported a case of hypothalamic and opto-chiasmatic involvement. Extra temporal involvement only can also be observed. CT is normal or the early course in 19% and shows the same aspects with a lower resolution than the MRI [2]Due to the high mortality rate despite the treatment (20 to 30%), the diagnosis must be rapidly evoked in the presence of cytotoxic (early) or vasogenic edema associated with hemorrhage and meningeal enhancement [7]. According to some authors, MRI can distinguish an HSV lesion from that caused by HHV6 or Japanese encephalitis [5,8].

Herpetic meningoencephalitis due to HSV is rapidly progressive compared to HHV6 lesions. This distinction is important because HHV6 is not sensitive to acyclovir. Japanese encephalitis involves the thalamus firstly.
However, aetiologies of limbic infectious lesions are numerous, apart from the HSV1 and 2 ; such as listeriosis, tuberculosis, varicella zoster virus, mycoplasma pneumoniae, enteroviruses, HHV6, Creutzfeldt-Jacob disease, West Nile virus, Influenza virus, Rocky Mountain spotted fever [2,8]. The gold standard diagnosis examination is virus detection in the cerebrospinal fluid by PCR (Polymerase Chain Reaction) with a high sensitivity and specificity ; 96 and 99% respectively. False negatives are possible early in the course. Repetition of the exam is then recommended. Mendes et al. reported a case with a repeated false negative PCR examination. Diagnosis was confirmed at autopsy. This illustrates the value of the associated clinical presentation [9,10] in the management. Acyclovir treatment initiated early is the only prognosis factor that can improve the prognosis of this condition. Survival is usually at the cost of significant cognitive sequelae. Complete recovery without sequelae is also possible [2].
References
- Bonnici Malia M, Kanodia AK, Rae N, Marwick C (2016) Herpes simplex encephalitis: Anusual imaging appeareances. BMJ Case Rep.
- Rashilas F, Wolff M, Delatour F, Chaffaut C, De Broucker T, Chevret S et al. (2002) Outcome of and prognostic factors for herpes simplex encephalitis in adult patients : results of a multicenter study. Clin Infect Dis 35(3): 254-260.
- Israel S, Kennedy PGE, Pachner AR (2007) The neurotopic herpes viruses : herpes simplex and varicella-zoster. The Lancet Neurology 6 (11): 1015-1028.
- Brinkmann MM, Spooner E, Hoebe K, Butler B, Ploeghe HL, et al. (2007) The interaction between the ER membrane protein UNC93B and TLR3, 7 and 9 is crucial for TLR signaling. JCB 177 (2): 265-275.
- Mehra S, Garga UC (2012) Role of imaging in herpes and Japenese encephalitis. Two cases and review of litterature. JIACM 13(4): 338-343.
- Sabah M, Mulcahy J, Zeman A (2012) BMJ 344: e3166.
- Chow FC, Glaser CA, Sheriff H, Xia D, Messenger S, Venkatesan WA, et al. (2015) Use of Clinical and Neuroimaging Characteristics to Distinguish Temporal Lobe Herpes Encephalitis From its mimics. Clinical - Infectious Diseases 60(9): 1377-1383.
- Noguchi T, Yoshiura T, Hiwatashi A, Togao O, Yamashita K, et al. (2010) CT and PMRI findings of Human Herpes virus 6 - Associated Encephalitis : Comparisaon With Findings of Herpes Simplex Virus Encephalitis. AJR 194.
- Mendez AA, Bosco A, Abdel Wahed L, Palmer K, Jones KA, et al. (2018) A Fatal Case of Herpes Simplex Encephalitis with Two False-Negative Polymerase Chain Reactions. Case Rep Neurol 10(2): 217–222.
- Weil AA, Glaser CA, Amad Z, Forghani B (2002) Patients with suspected herpes simplex encephalitis : rethinking an initial negative polymerase chain reaction result.Clin Infect Dis 34(8): 1154-1157.






























