Glycemic Control and its Associated Factors among Elderly Diabetic Patients in a Tertiary Hospital in Lagos, Nigeria
Ayonote, Uzoramaka Angela1*, Ogbonna, Adaobi Nneamaka1 and Akujuobi, Obianuju Mirian2
1Department of Family Medicine, Lagos University Teaching Hospital, Nigeria
2Department of Counselling Psychology, Yorkville University, Canada
Submission: July 13, 2022; Published: August 01, 2022
*Corresponding author: Ayonote Uzoramaka Angela, Department of Family Medicine, Lagos University Teaching Hospital, Lagos, Nigeria
How to cite this article: Ayonote, U A, Ogbonna, A N, Akujuobi, O.M. Glycemic Control and its Associated Factors among Elderly Diabetic Patients in a Tertiary Hospital in Lagos, Nigeria. Curre Res Diabetes & Obes J 2022; 16(1): 555928.DOI: 10.19080/CRDOJ.2022.16.555928
Abstract
Background: Glycaemic control in the elderly diabetic patient is highly individualized and achieving desired targets in the presence of comorbid conditions could be very challenging. This study was conducted to assess the glycemic control of elderly diabetics and identify associated factors at the Lagos University Teaching Hospital (LUTH).
Methodology: A hospital-based, cross-sectional descriptive study involving 199 randomly selected elderly diabetic patients receiving care at LUTH. A pretested, interviewer-administered questionnaire was used in data collection, which include sociodemographic characteristics, clinical history, and glycaemic control. Glycemic control was assessed using glycated haemoglobin (HBA1C). HBA1C<7.0% was tight; 7-8% targeted and >8% poor glycaemic control. Associations between glycemic control and independent variables was assessed using the chi-square test and its predictors identified by logistic regression analysis. Level of significance was set at p<0.05.
.Results: The mean age of the participants was 68.6 years ± 6.7 years. Tight and poor glycemic control was seen in 35.1% and 34.2% respectively. Significant associations existed between glycemic control, age (ꭓ2=9.310; p – 0.010), and marital status (ꭓ2 = 9.934; p – 0.007). Independent predictors include >2 antidiabetic medication (aOR – 2.55; p – 0.048)
Conclusion: Poor glycaemic control was high among the elderly and there was a negative correlation between age and glycaemic control among the participants. Statistically significant association was also found between glycaemic control and marital status of the participants as well as the number of diabetic medications, the presence of co-morbid conditions and adherence to medications. The need for individualized care among elderly diabetics cannot be overemphasized in order to reduce the risk of hypoglycaemia, improve clinical outcome, while considering other factors which could have an impact on glycaemic control among the elderly.
Keywords: Elderly; Diabetic; Glycaemic control; Related factors; Nigeria
Introduction
Non-communicable diseases are major causes of morbidity and mortality among the elderly [1]. Cardiovascular diseases and diabetes mellitus (DM) have been predicted as leading causes of mortality in Africa within the next ten years [2]. Diabetes mellitus is a metabolic disease characterized by hyperglycaemia resulting from pathological defects in insulin secretion, insulin action, or both [3]. The long-term exposure to hyperglycaemia has been shown to result in long term damage and failure of major organs [4]. Type 2 Diabetes Mellitus is the most prevalent form of Diabetes and it accounts for about 90% of all cases [5]. There is a global pandemic of DM due to the increasing numbers of older people, growing population of the elderly worldwide, rising levels of obesity and inactivity [6,7]. Also, as much as 80% of individuals living with DM reside within low and middle income countries [8]. The prevalence of DM has been shown to increase with age across all regions with a global prevalence among the elderly of 18.8% [9] and highest prevalence occurring among those aged between 60 and 79 years [8]. Research has shown that it is pertinent to ensure adherence to medication regimens among this group of individuals considering that it is crucial to achieving successful treatment outcomes [10,11].
The United Nations describes elderly persons as individuals who are aged 60-years and above [12] and persons within this age group are known to manifest higher rates of health complications including functional decline, neurological defects, visual impairments and so on. This could create a challenge in the management of diabetes among the elderly as well as achieving target glycaemic control [10,13]. Glycaemic control can be assessed by measuring the glycated haemoglobin (HbA1C) and HbA1c values less than 7.0% indicates adequate glycaemic control in general populations, however, several guidelines recommend less stringent glycaemic control targets ranging between 7.5% to 8.0% for elderly diabetic patients [14-16]. This is because of increased susceptibility to hypoglycaemia and other health comorbidities among geriatric individuals [16].
Some studies have shown that glycaemic control among the elderly can be affected by the presence of comorbid conditions as well as life expectancy of the individual hence, target glycaemic control among the elderly should be individualized [16-18]. Considering the challenges posed by having to take daily medications, polypharmacy and medications cost, frequent needle pricks, the reduced capacity for self-care and so on; the task of achieving glycaemic control among elderly diabetics can be tedious [10,11]. The elderly persons living with diabetes mellitus also suffer higher rates of complications due to longer periods of exposure to the disease hence, the need for achieving glycaemic control cannot be over emphasized [13].
The estimated prevalence of diabetes among the elderly in different regions of the world include North America and the Caribbean- 26.3%, Middle East and North Africa- 20.4%, Western Pacific- 20.0% Europe 19.4%, South and Central America-19.0%, Southeast Asia- 13.5%, and Africa 5.2% [19]. Kirkman et al. [20] found that about 22.0% to 33.0% of elderly in the United States were diagnosed with diabetes. Jain et al. [21] in India reported a prevalence of DM among the elderly to be 30.4%. In Brazil the prevalence of diabetes among the elderly has been reported to be 22.4% following a cross sectional study [22]. A hospital based study in Cotonou, Republic of Benin found the prevalence of diabetes among elderly persons aged 65 years and above, to be 15.9% [23]. Gatimu et al. [24] in Ghana following a cross sectional study among older adults aged 50 years and above, also reported the prevalence of DM among elderly 60 years and above to be 9.38%. Another study in Nigeria reported a DM prevalence rate of 8.9% among the elderly [25]. In 2017, about 60% of deaths from DM among individuals aged 18-99years worldwide occurred amongst the elderly [19].
Studies assessing glycaemic control among elderly diabetic patients considering the unique characteristics of elderly diabetics are not widespread and requires more evidence. Considering majority of studies among diabetics were conducted among the general population, the increase in the population of the elderly, the rising prevalence of diabetes mellitus as well as higher burden of the disease among the elderly; there was a need for the conduct of this study focusing strictly on elderly diabetics [26]. This study thus assessed glycaemic control among geriatric diabetics receiving care at a tertiary health facility in Lagos, Nigeria as well as identifying factors associated with glycaemic control. The information generated from this study provided empirical data regarding glycaemic control among elderly diabetics as well as the socio-demographic and clinically associated factors. It also provided a basis for advocacy targeted at improving the clinical care of geriatric individuals affected by diabetes mellitus.
Materials And Methods
Study area
The study was carried out in Lagos state at the Endocrinology Clinic of Lagos University Teaching Hospital (LUTH). Lagos state is located in the south-western region of Nigeria. It is an urban city and comprises 20 Local Government Areas (LGA) and 37 Local Council Development Areas [27]. It is one of the most populous states in Nigeria with a population of about 21 million people. The inhabitants of Lagos State are of different tribes and ethnicity, but the Yoruba ethnic group is predominant. They also vary in occupation ranging from professionals to unskilled workers.
Lagos University Teaching Hospital is one of the tertiary health care facilities within the state. It is located at Idi-Araba community of Mushin LGA. The hospital was established in 1962 by the Federal Government of Nigeria to provide secondary and tertiary health care services to the general public and training for different cadres of health care professionals. It currently has a capacity of 811 bed/admission spaces for inpatient care. The Endocrinology clinic of the Department of Medicine, LUTH, offers specialist care to adult diabetic patients. It offers follow up care to previously diagnosed diabetic patients on Tuesday, 8am to 4pm. The newly diagnosed diabetic patients are seen on Mondays (1pm to 4pm). Individuals who have been diagnosed with diabetes mellitus at various health centers are also referred to this clinic for further care. About 124 elderly diabetic patients are seen for follow-up in the clinic monthly giving an average of 31 elderly diabetic patients during the weekly clinic on Tuesdays.
Study design
This study utilized a cross sectional, descriptive study design which adopted a hospital-based approach and was carried out at the Endocrinology clinic of the Lagos University Teaching Hospital (LUTH).
Study population and selection criteria
The study population consisted of elderly diabetic patients aged 60years. The United Nations’ definition of the elderly was used for this study. Inclusion criteria were elderly diabetic patients aged 60 years and above, who had been on follow up at the Endocrinology clinic of LUTH for a minimum of six months and who have normal cognitive function. Cognitive function was tested using the six-item cognitive impairment test (6-item CIT) tool [28,29]. A score of 0-7 was considered as normal; 8-9 as mild cognitive impairment and score ≥ 10 as severe cognitive impairment.28,29 Patients with score ≥ 8 were not recruited for the study. Non-consenting and acutely ill elderly patients were also excluded from the study [28].
Sample size calculation
Sample size was calculated using the sample size formula for
calculating single proportions in a population shown below [30]: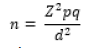 n is the minimum sample size required for the study, p is the
prevalence of good glycaemic control was reported as 40.0%
(0.40) by Osuji et al in South-west [31], q is the complementary
proportion given as 1 – p (1 – 0.40 = 0.60) and d is the level of
precision (margin of error) in the study set at 5.0% (0.05) for
this study. Minimum sample size was adjusted for non-response
using a non-response rate of 10% to account for possible
missing or incomplete data. After substitution a sample size of
406 participants was obtained after adjusting for non-response.
However, the total population of elderly diabetes expected in a
period of 3 months in the Endocrinology clinic is 372 patients
(124 patients monthly X 3; obtained from the Health Information
Management System of the hospital), hence the formula for
correcting for finite population (population < 10,000) was applied
and sample size of 195 participants was obtained. A total of 199
participants eventually commenced and completed the study.
n is the minimum sample size required for the study, p is the
prevalence of good glycaemic control was reported as 40.0%
(0.40) by Osuji et al in South-west [31], q is the complementary
proportion given as 1 – p (1 – 0.40 = 0.60) and d is the level of
precision (margin of error) in the study set at 5.0% (0.05) for
this study. Minimum sample size was adjusted for non-response
using a non-response rate of 10% to account for possible
missing or incomplete data. After substitution a sample size of
406 participants was obtained after adjusting for non-response.
However, the total population of elderly diabetes expected in a
period of 3 months in the Endocrinology clinic is 372 patients
(124 patients monthly X 3; obtained from the Health Information
Management System of the hospital), hence the formula for
correcting for finite population (population < 10,000) was applied
and sample size of 195 participants was obtained. A total of 199
participants eventually commenced and completed the study.
Sampling technique
Participants for this study were recruited from Endocrinology clinic of LUTH using a simple random sampling technique (using computer generated random numbers). About 12 – 15 elderly diabetic patients were recruited weekly over a period of 14 weeks between September and December 2021.
Study questionnaire
A pre-tested, semi-structured, interviewer-administered questionnaire with 5 sections was used; Section A-C of this questionnaire was adapted from the WHO STEPS 26 questionnaire and collected data on the socio-demographic characteristics, lifestyle and medical history of the participants including age, gender, marital status, occupation, income, and medical history [32]. The monthly income of participants included all sources of money available to the individual because a large proportion of the elderly in Nigeria are retired and lack a steady flow of income [33,34]. Section D assessed Medication adherence using the eight item Morisky Medication Adherence Scale (MMAS-8). The Morisky Medication Adherence scale has a total of eight questions. The responses to the first seven items are either ‘Yes’ or ‘No’ and a response of ‘Yes’ was scored 1, while ‘No’ was scored 0 except question 5 which was negatively worded and thus the scoring was reversed. The last item, question 8 had a 5-point Likert response. A response indicating ‘never/rarely’ attracts a score of 1 while choosing any of the other options on the scale attracts 0 point [35]. All scores obtained were summed up to a total score, which ranged from 0 to 8. The total score for each participant gave a measure of the level of their adherence to medications. A score of 8 represented high adherence, a score of 6-7 represented medium adherence while a score 5 and below represented low adherence [36]. The glycated haemoglobin result was recorded in Section E.
Study procedure
Data collection was done together with two research assistants who received pre-requisite training on the essential components of the research and the entire data collection process. Interview was conducted at the Endocrinology clinic every Tuesday. On all research day, using Microsoft EXCEL software, 15 random numbers were generated from between 1 and 31. (since average weekly attendance of the 60 years and above is 31. Elderly patients were arranged in selected rows of chairs and given serial numbers as they arrive to the clinic. Participants with numbers selected randomly by the computer were called and the study was introduced to them while they were also assessed for eligibility in the study. Those eligible and who gave consent to participate were recruited for the study. When an eligible selected patients declined participation, the number of persons who declined is added to the number to be recruited on the next research day. After recruitment and consent was obtained, participants are taken to a separate consulting room where the questionnaire was administered. Thereafter, venipuncture was performed according to the WHO guidelines on venipuncture [37]. The procedure was conducted at a side room set-up close to the clinics and was done under optimal conditions necessary to maintain a sterile procedure. The blood sample was then analyzed at a laboratory also located close to the clinics. Analysis was done using the automated CLOVER HbA1c machine by Infopia and results of each participant was obtained. These results were shared with the respective participants and appropriate counselling was given afterwards.
Data analysis
Data collected was entered and analyzed using the Statistical package for Social Sciences (SPSS) version 23. Descriptive statistics such as socio-demographic (age-group, sex, marital status, income level etc) and clinical characteristics (such as presence of comorbidity, number of medication) of the respondents were summarized using frequencies and percentages. Monthly income was classified into those living below the poverty line ≤ 21, 00 naira monthly and those living above the poverty line > 21,000 naira monthly using the national poverty line of living on ≤1.9USD per capita per day [38]. At an exchange rate of 1USD to 360 Naira as at the time of the study, this was equivalent to 684 naira/day and 20,520 naira per month (approximately N21,000 monthly). Glycaemic control (the dependent variable) was categorized as ‘very tight’ glycaemic control (HbA1c < 7%), ‘recommended’ glycaemic control for the elderly (HbA1C 7-8%) and ‘poor’ glycaemic control (HbA1c > 8%) [39-41]. A test for association between the independent variables (sociodemographic and clinical characteristics of participants as well as medication adherence and the dependent variable (glycaemic control) was done using the Chi-square or Fisher’s exact tests (where appropriate). Logistic regression was conducted to assess the independent predictors of glycaemic control and the level of statistical significance was set at p < 0.05.
Ethical considerations
Approval for this study was granted by the Lagos University Teaching Hospital Health Research and Ethics Committee. A written informed consent was obtained from each participant at recruitment using a consent form while, ensuring the privacy of each participant and confidentiality of their responses during the data collection process. The participants were also informed that they were free to opt out from the study as the decision to participate was entirely voluntary.
Results
Sociodemographic characteristics of participants
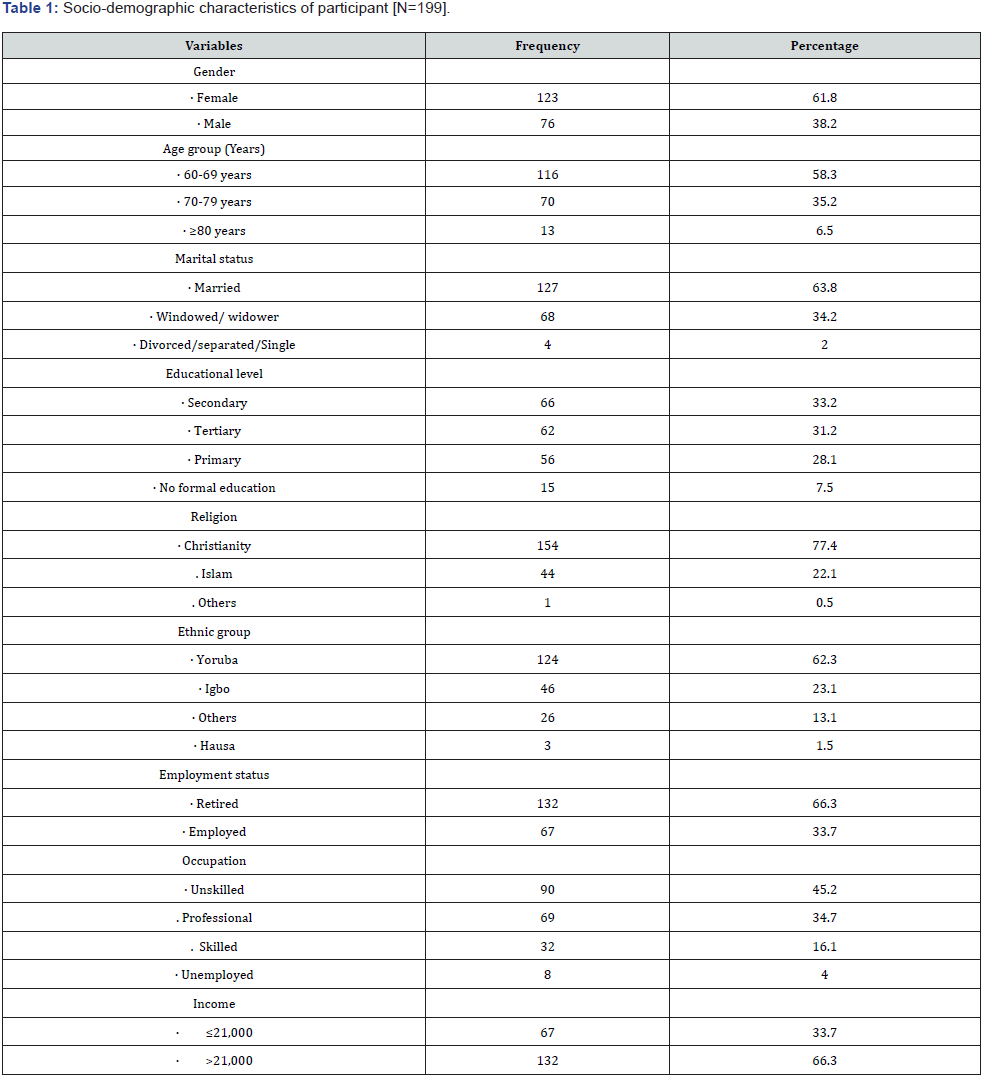
As seen in table 1 of the 199 participants, 116(58.3%), 70(35.2%) and 13(6.5%) of the participants were in the seventh, eighth and ninth decade of life respectively. The mean age of participants was 68.6±6.7 years. Most of the participants were married (63.8%), with post-primary education (64.4%), belong to the Christian faith (77.4%), retired (66.3%) and of the Yoruba ethnic nationality (62.3%). Table 1 also shows that two-third of participants (66.3%) were classified as living above the poverty line (>21,000/month).
Clinical history and medication adherence among the participants
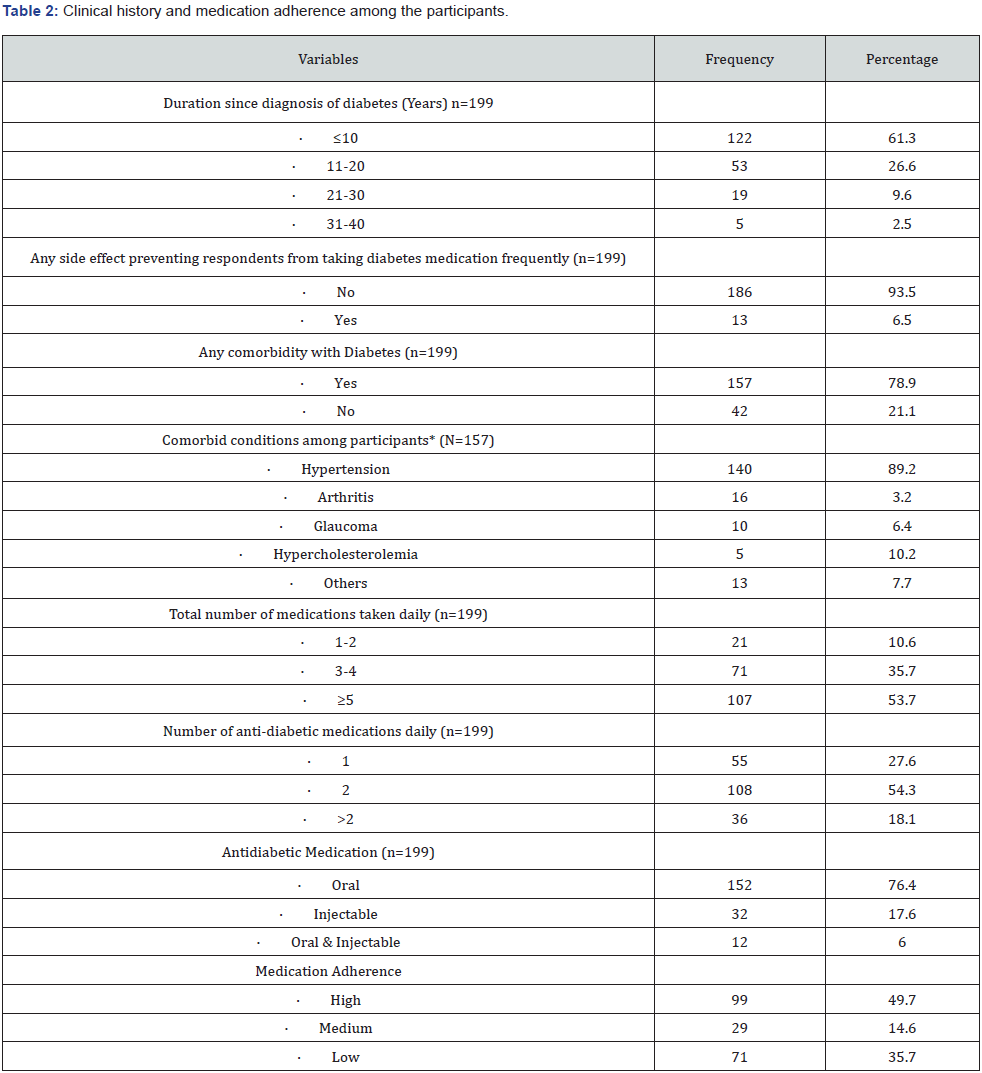
*Multiple responses
Table 2 reveals that 122 (61.3%) of the participants had been diagnosed with diabetes for ten years or less. Thirteen participants (6.5%) reported having side effects from the medication which negatively influenced taking their medications frequently. About 3 in every 4 participants (78.9%) reported comorbid condition(s) with diabetes. The most common co-morbid condition among the participants was hypertension (89.2%). Also shown in table 2, over half of the participants reported taking five or more medications daily (53.7%) and were on a combination of at least two antidiabetic medications (54.3%). Regarding the type of antidiabetic medications used by the participants, 152 participants (76.4%) used oral anti-diabetic medications, 35 (17.6%) used injectables and 12 (6.0%) used both oral and injectable medications. About half of study participants, however, had high medication adherence (Table 2).
Pattern of glycaemic control among the participants

Figure 1 shows the pattern of glycaemic control among the participants using HbA1c. Seventy participants (35.1%) had ‘very tight’ glycaemic control (HbA1c < 7%) while 68 (34.2%) had ‘poor’ glycaemic control with HBA1C > 8%. Only 61(30.7%) of them had their HBA1C between 7-8% which is the recommended targets for elderly diabetics. The overall mean HbA1C was 7.78% ± 1.7%.
Association between socio-demographic characteristics and glycemic control
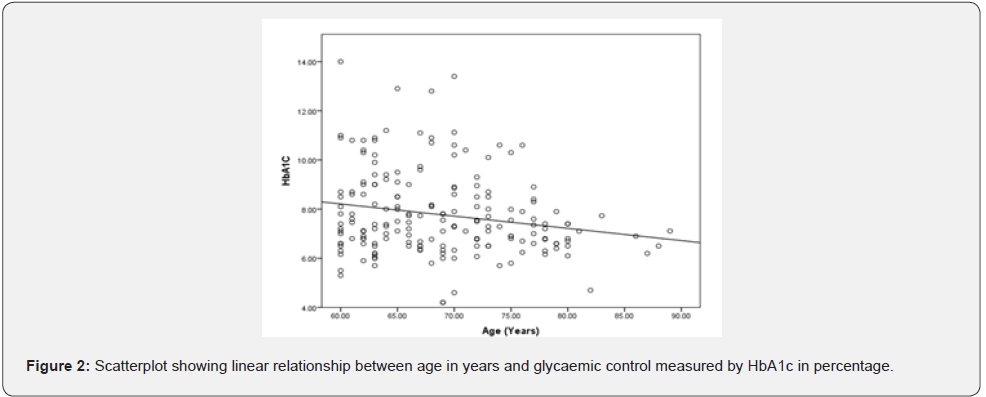
Table 3 shows the association between sociodemographic characteristics and glycaemic control of the study participant. There was a statistically significant association between age (ꭓ2=9.310; p – 0.010), marital status (ꭓ2 = 9.934; p – 0.007), and glycaemic control of the study participants. In figure 2, a negative correlation between age in years and glycaemic control assessed by glycated haemoglobin in percantage was demonstrated. It was seen that as the age of participants increased their HBA1C values decreased (ɼ = 0.197; p – 0.007).
Association between the clinical characteristic and glycaemic control
Statistically significant associations were found to exist between the presence of co-morbid conditions (ꭓ2=4.385, p – 0.039), the number of anti-diabetic medications taken daily (ꭓ2=12.328, p – 0.015) and glycaemic control. Medication adherence also showed a statistically significant (ꭓ2 =4.20; p – 0.049) relationship with glycaemic control (Table 4).
Predictors of poor glycaemic control among study participants
The number of anti-diabetic medication used daily (>2 medication: aOR = 2.555; p – 0.048) and medication adherence (Low adherence: OR = 2.026; p – 0.047) were independent predictors of poor glycaemic control among participants in this study. Participants who were on more than two antidiabetic medications were two times more likely to have poor glycemic control compared to those on ≤ 2 medications. Similarly, participants with low medication adherence had an increased odd of poor glycaemic control than those with high adherence. Other factors found to be associated with poor glycemic control in the bivariate analysis including age, marital status, presence of comorbid conditions, were not found to be independent predictors of poor glycaemic control following multivariate logistic regression analysis (Table 5).
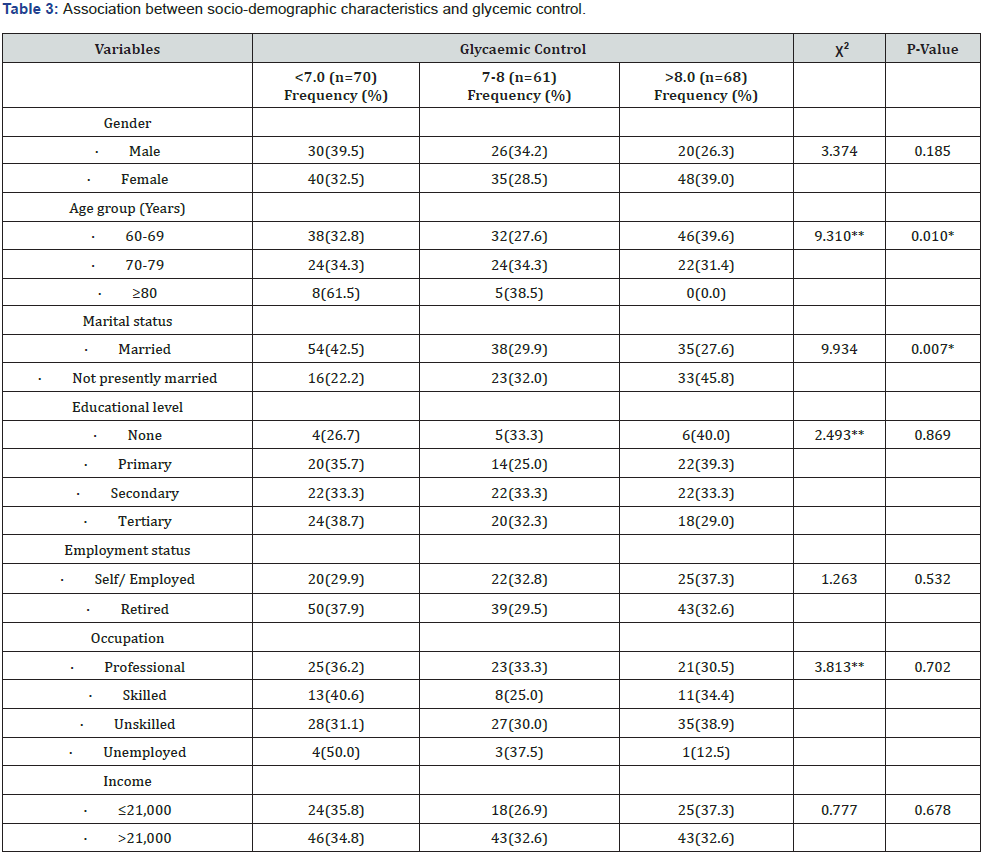
ꭓ2 = Chi square, *Significant p< 0.05, ** Fisher exact test, % = percentage in row bracket
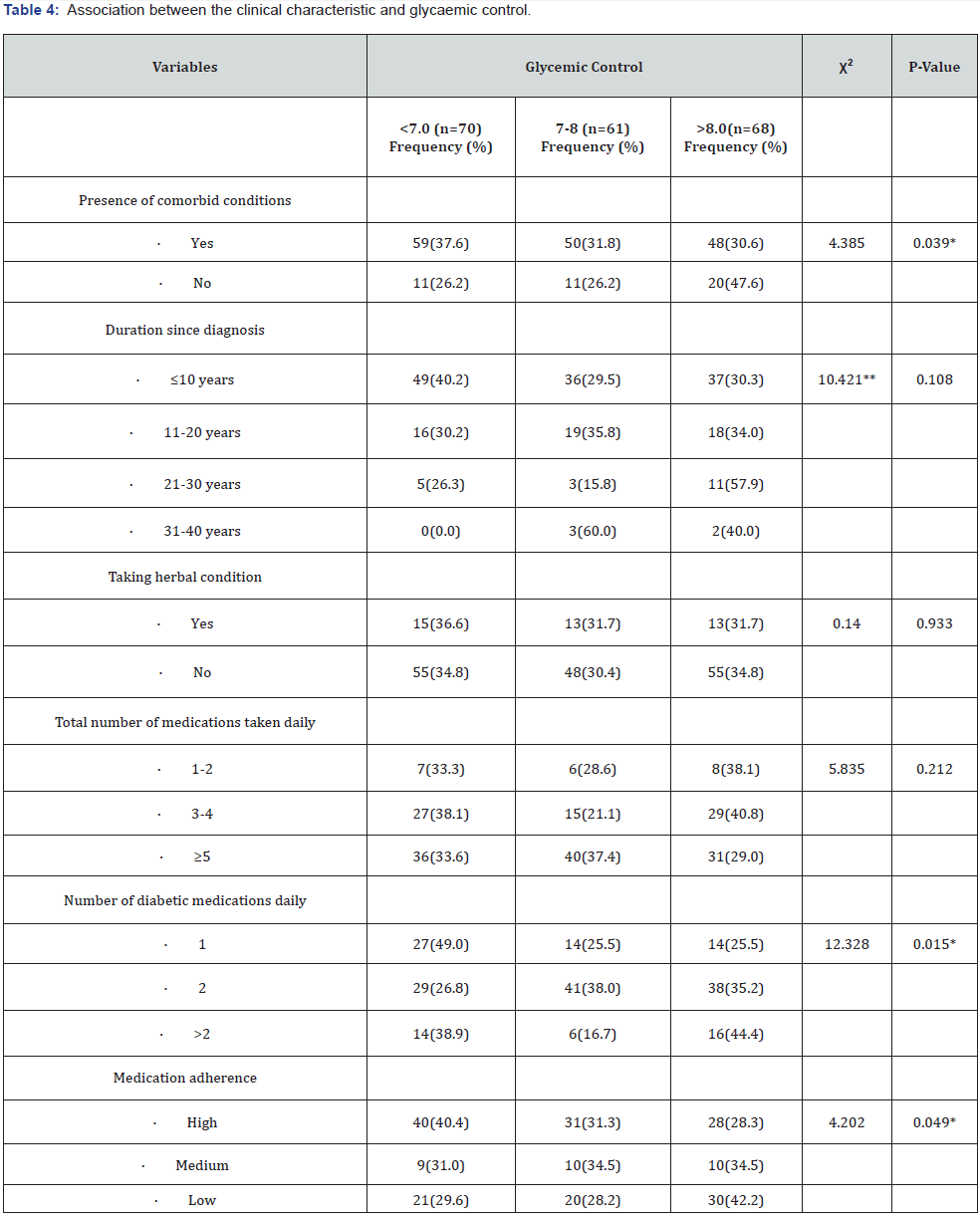
ꭓ2 = Chi square, *Significant P< 0.05, ** Fisher exact test, % = percentage in row bracket
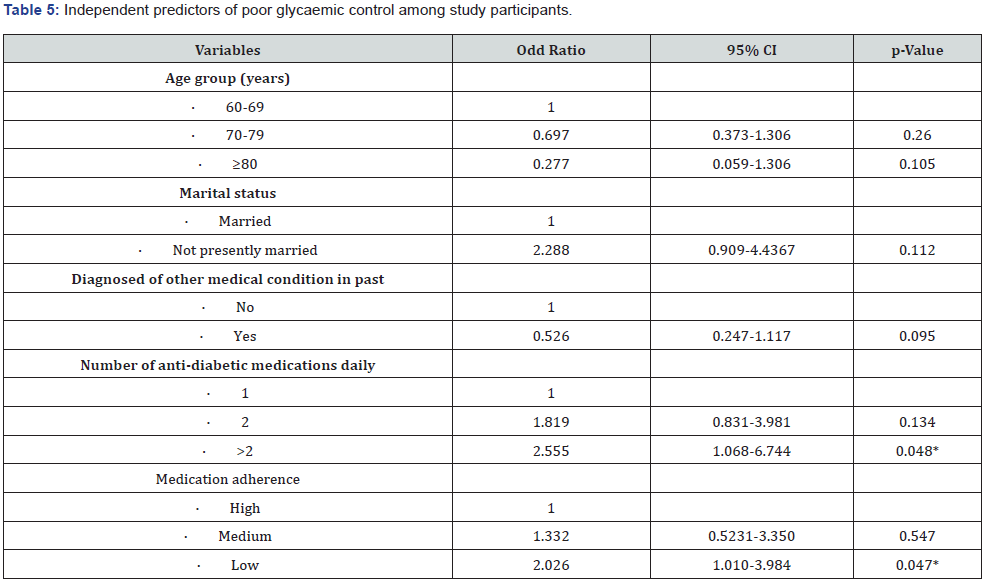
Reference category = 1
Discussion
This study found a statistically significant relationship between glycaemic control and age, as well as marital status of the participants. Scatter plot showing the linear relationship between age and glycaemic control of the participants showed a negative correlation implying that as their ages increased, HbA1c values reduced. This may suggest that with increasing age, the patients and their relatives are gaining more experience with managing diabetes and achieving a better glycaemic control. This is likely since the study is a hospital-based study that involved a large number (about 40%) who have been on follow up for more than 10 years. The susceptibility of the elderly to hypoglycaemia may have also contributed to this trend and, this buttresses the need for individualized care in the management of diabetes among the elderly [16-20]. A significant association between marital status and glycaemic control was also observed in our study which is probably due to the effect of spousal support and care. Spousal support may include activities such as peculiarities with meal preparation for diabetics, reminders for drug use and support at ensuring regular clinic visits which impact directly on the glycaemic status of the patients. However, logistic regression showed that age and marital status were not independent predictors of poor glycaemic control. This implies that although, age and marital status played a role in ensuring better glycaemic control among the participants, the level of influence cannot stand independent from other factors for achieving good glycaemic control [10,11].
The studies by Musenge & Osuji et al. [31,42] respectively, corroborated the present study’s finding of significant association existing between glycaemic control and age of respondents. The reason for the similarity could be the use of HBA1C values in assessing glycaemic control in the studies as well as the hospitalbased approach adopted in the study by Osuji et al. in 2018. There were however contrasting views to the findings of this study as the relationships identified in the present study were not found in some other studies [43-45]. The reason for this difference could be due to the different method used to access glycaemic control when compared with the present study where glycated haemoglobin was used. In one of such studies, glycaemic control of the participants was assessed by obtaining past results of their fasting blood glucose from the respective case notes of the respondents. Their method may not have given a true representation of the glycaemic control of the participants [43].
In addition, it was observed that a larger proportion of the participants in this study who had other co-morbid conditions had lower HBA1C values while, larger proportions of the participant who did not have any comorbid condition had higher HBA1C values. The reason for this observation may be because patients who have co-morbidities tend to be more concerned about their health and may adhere better to their medications, to improve their health. However, following logistic regression, the presence of co-morbidities was not found to be an independent predictor of glycaemic control. This implies that the association that was found between glycaemic control and the presence of co-morbid conditions may have been influenced by other factors [11,17,18].
This study also found that a larger proportion of the participants with duration of diagnosis above 20 years had higher HbA1c values although this was not found to be statistically significant. However, Ufuoma et al. [46] found a statistically significant association between glycaemic control and duration of diseases. This finding may be attributed to the age distribution of the study participants. A larger proportion (69%) of the participants in the study by Ufuoma et al. [46] were less than 60 years while for this study all the participants were above 60 years. Another reason could be because of the different HBA1C cut-off thresholds that were used both studies. Participants in the study by Ufuoma et al who had HBA1C >7% were categorized as having poor control, while for this study, participants with HBA1C >8% were considered as having poor glycaemic control. Lastly, the different geographical location of each study may have also contributed to the difference observed.
This study also found that the number of antidiabetic medications used by the participants was significantly associated with glycaemic control. It was observed that a larger proportion of the participants who used only one antidiabetic medication had better glycaemic control than those who used more than two diabetic medications daily. The reason for this may have been because patients with poor glycaemic control are more likely to be placed on combination therapy in accordance to clinical guidelines in management of diabetes. However, the combination therapy is also associated with challenges of adherence and finance. Lack of finances to procure multiple medications, could make adherence difficult which in turn makes good glycaemic control difficult to achieve. However, better medication adherence is most likely among participants who were placed on one antidiabetic medication.
Findings from studies buttress the fact that medication adherence facilitates glycaemic control. The studies by Alqami & Osei-Yeboah et al. [47,48] found an association between glycaemic control and medication adherence. These studies demonstrate the importance of medication adherence even in the elderly diabetic patient. However, from a study by Onwuchuluba et al. [49] no association was found between medication adherence and good glycaemic control. This difference may be a reflection of the fact that adherence to medication may not be the only factor that contributes to improved glycaemic control even among elderly patients; a concept that gave rise to this study which aimed at identifying other factors that may be associated with improved glycaemic control aside from medication adherence.
Conclusion
In this study, the highest proportion of the participants had very tight glycaemic control which was significantly associated with age and marital status of the participants as well as the number of diabetic medications used by the participants and the presence of co-morbid conditions. It was thus recommended in this study that the need for individualized care among elderly diabetics cannot be overemphasized in order to reduce their risk of hypoglycaemia and improve their clinical outcome while considering other factors that could affect glycaemic control. There is also a need for community-based studies to be conducted to assess the prevalence of glycaemic control among the general populace which may be more representative. Future studies can also conduct focused research on the effect of the diverse local diet available in West Africa and glycaemic control among diabetics.
References
1. Mini GK, Thankappan KR (2017) Pattern, correlates and implications of non-communicable disease multi-morbidity among older adults in selected Indian states: a cross-sectional study. BMJ Open 7(3): e013529.
- Aikins AD, Unwin N, Agyemang C, Allotey P, Campbell C, et al. (2010) Tackling Africa's chronic disease burden: from the local to the global. Globalization and Health 6(1): 5-13.
- Kharroubi AT, Darwish HM (2015) Diabetes mellitus: The epidemic of the century. World J Diabetes 6(6): 850-867.
- Dal-Canto DE, Ceriello A, Rydén L, Ferrini M, Hansen TB, et al. (2019) Diabetes as a cardiovascular risk factor: An overview of global trends of macro and micro vascular complications. Eur J Prev Cardiol 26(2): 25-32.
- Olokoba AB, Obateru OA, Olokoba LB (2012) Type 2 diabetes mellitus: A review of current trends. Oman Medical Journal 27(4): 269-273.
- Dieren SV, Beulens JW, Van-der Schouw YT, Grobbee DE, Nealb B (2010) The global burden of diabetes and its complications: An emerging pandemic. Eur J Cardiovasc Prev Rehabil 17(1): 3-8.
- Thibault V, Bélanger M, LeBlanc E, Babin L, Halpine S, et al. (2016) Factors that could explain the increasing prevalence of type 2 diabetes among adults in a Canadian province: A critical review and analysis. Diabetol Metab Syndr 8(1): 71-81.
- Guariguata L, Whiting DR, Hambleton I, Beagley J, Linnenkamp U, et al. (2014) Global estimates of prevalence of diabetes in adults for 2013 and projections to 2035. Diabetes Res Clin Pract 103(2): 137-149.
- (2017) International diabetes federation (8th edn.), Diabetes atlas. Available at www. diabetesatlas.org. Assessed on 16/12/19.
- Yap AF, Thirumoorthy T, Kwan YH (2016) Medication adherence in the elderly. Journal of Clinical Gerontology and Geriatrics 7(2): 64-67.
- Bazargan M, Smith J, Yazdanshenas H, Movassaghi M, Martins D, et al. (2017) non-adherence to medication regimens among older African-American adults. BMC Geriatr 17(1): 163-175.
- (2013) United Nations, Department of Economic and Social Affairs, Population Division. World Population Ageing 2013. ST/ESA/SER.A/348, 2013. Available at http://www.un.org/en/development/desa/population/publications/pdf/ageing/WorldPopulationAgeing2013.pdf. Assessed on 16/12/19.
- Corriere M, Rooparinesingh N, Kalyani RR (2013) Epidemiology of diabetes and diabetes complications in the elderly: An emerging public health burden. Current Diabetes Reports 13(6): 805-813.
- Huang ES, Liu JY, Moffet HH, John PM, Karter AJ (2011) Glycemic control, complications, and death in older diabetic patients: The diabetes and aging study. Diabetes Care 34(6): 1329-1336.
- Huang ES, Davis AM (2015) Glycemic control in older adults with diabetes mellitus. JAMA 314(14): 1509-1510.
- (2013) Guidelines abstracted from the American Geriatrics Society guidelines for improving the care of older adults with diabetes mellitus: 2013 update. J Am Geriatr Soc 61(11): 2020-2026.
- Yakaryılmaz FD, Öztürk ZA (2017) Treatment of type 2 diabetes mellitus in the elderly. World Journal of Diabetes 8(6): 278-285.
- Abdelhafiz AH, Sinclair AJ (2017) Management of type 2 diabetes in older people. Diabetes Therapy. 2013;4(1):13-26.
- (2017) International diabetes federation. IDF Diabetes atlas (8th), Available at www. diabetesatlas.org. Assessed on 16/12/19.
- Kirkman MS, Briscoe VJ, Clark N, Florez H, Haas LB, et al. (2012) Diabetes in older adults: A consensus report. J Am Geriatr Soc 60(12): 2342-2356.
- Jain A, Paranjape S (2013) Prevalence of type 2 diabetes mellitus in elderly in a primary care facility: An ideal facility. Indian J Endocrinol Metab 17(1): 318-322.
- Vitoi NC, Fogal AS, Nascimento CD, Franceschini SD, Ribeiro AQ (2015) Prevalence and associated factors of diabetes in the elderly population in Viçosa, Minas Gerais, Brazil. Revista Brasileira de Epidemiologia 18(4): 953-965.
- Djrolo F, Adoukonou T, Houehanou C, Houinato JD, Houinato D (2015) Diabetes in Borgou Department in Benin: Prevalence and associated factors. Journal of Diabetes Mellitus 5(2): 90-96.
- Gatimu SM, Milimo BW, San Sebastian M (2016) Prevalence and determinants of diabetes among older adults in Ghana. BMC Public Health 16(1): 1174.
- Balogun WO, Gureje O (2013) Self-reported incident type 2 diabetes in the Ibadan study of ageing: Relationship with urban residence and socioeconomic status. Gerontology 59(1): 3-7.
- Aboagye E, Agyemang OS, Tjerbo T (2014) Elderly demand for family-based care and support: Evidence from a social intervention strategy. Global Journal of Health Science 6(2): 94-104.
- (2019) Lagos population. World population review. Available from http://world populationreview.com/world-cities/lagos-population/. Assessed on 18/12/2019.
- O'Sullivan D, O'Regan NA, Timmons S (2016) Validity and reliability of the 6-item cognitive impairment test for screening cognitive impairment: A review. Dementia and Geriatric Cognitive Disorders 42(1-2): 42-49
- Apóstolo JL, Paiva DD, Silva RC, Santos EJ, Schultz TJ (2018) Adaptation and validation into Portuguese language of the six-item cognitive impairment test (6CIT). Aging & Mental Health 22(9): 1190-1195.
- Charan J, Biswas T (2013) How to calculate sample size for different study designs in medical research. Indian J Psychol Med 35(2): 121-126.
- Osuji NA, Ojo OS, Malomo SO, Sogunle PT, Egunjobi AO (2018) Relationship between glycaemic control and perceived family support among people with type 2 diabetes mellitus seen in a rich kinship network in South-West Nigeria. Family Medicine and Community Health 6(4): 168-177.
- Riley L, Guthold R, Cowan M, Savin S, Bhatti L, et al. (2016) The World Health Organization STEPwise approach to non-communicable disease risk-factor surveillance: Methods, challenges, and opportunities. Am J Public Health 106(1): 74-81.
- Ojagbemi A, Bello T, Luo Z, Gureje O (2016) Living conditions, low socioeconomic position, and mortality in the Ibadan study of aging. Journals of Gerontology Series B: Psychological Sciences and Social Sciences 72(4): 646-655.
- Animasahun VJ, Chapman HJ (2017) Psychosocial health challenges of the elderly in Nigeria: A narrative review. Afr Health Sci 17(2): 575-583.
- Yuvaraj K, Gokul S, Sivaranjini K, Manikandanesan S, Murali S, et al. (2019) Prevalence of medication adherence and its associated factors among patients with non-communicable disease in rural Puducherry, South India – A facility-based cross-sectional study. J Family Med Prim Care 8(2): 701-705.
- Egunjobi AO, Ojo OS, Malomo SO, Sogunle PT (2018) Medication adherence and perceived family support among patients with type 2 diabetes mellitus seen at a primary care clinic in Southwest Nigeria. Nigerian Journal of Family Practice 9(2): 21-31.
- (2010) WHO guidelines on drawing blood: best practices in phlebotomy. World Health Organization, Geneva, Switzerland.
Available from: https://www.ncbi.nlm.nih.gov/books/ NBK138665/. Accessed on 18/12/2019.
- (2019) The world-bank. Poverty and equity data portal. Available at http://povertydata. worldbank.org/poverty/country/NGA.
- Huang ES, Davis AM (2015) Glycemic control in older adults with diabetes mellitus. JAMA 314(14): 1509-1510.
- (2013) Guidelines abstracted from the American Geriatrics Society guidelines for improving the care of older adults with diabetes mellitus: 2013 update. J Am Geriatr Soc 61(11): 2020-2026.
- Alramadan MJ, Magliano DJ, Almigbal TH, Batais MA, Afroz A, et al. (2018) Glycaemic control for people with type 2 diabetes in Saudi Arabia–An urgent need for a review of management plan. BMC Endocrine Disorders 18(1): 62-74.
- Musenge EM, Manankov A, Mudenda B, Michelo C (2014) Glycaemic control in diabetic patients in Zambia. The Pan African Medical Journal 19: 354.
- Kamuhabwa AR, Charles E (2014) Predictors of poor glycemic control in type 2 diabetic patients attending public hospitals in Dar es Salaam. Drug Healthc Patient Saf 6(1): 155-165.
- Ashur ST, Shah SA, Bosseri S, Fah TS, Shamsuddin K (2016) Glycaemic control status among type 2 diabetic patients and the role of their diabetes coping behaviours: A clinic-based study in Tripoli, Libya. Libyan J Medi 11(1): 31086.
- Odume BB, Ofoegbu OS, Aniwada EC, Okechukwu EF (2015) The influence of family characteristics on glycaemic control among adult patients with type 2 diabetes mellitus attending the general outpatient clinic, national hospital, Abuja, Nigeria. South African Family Practice 57(6): 347-352.
- Ufuoma C, Godwin YD, Kester AD, Ngozi JC (2016) Determinants of glycemic control among persons with type 2 diabetes mellitus in Niger Delta. Sahel Med J 19(4): 190-195.
- Alqami AM, Alrahbeni T, Al Qarni A, Al Qarni HM (2019) Adherence to diabetes medication among diabetic patients in the Bisha governorate of Saudi Arabia– A cross-sectional survey. Patient Preference and Adherence 13: 63-71.
- Osei-Yeboah J, Owiredu W, Norgbe G, Obirikorang C, Lokpo S, et al. (2019) Physical activity pattern and its association with glycaemic and blood pressure control among people living with diabetes (PLWD) in the Ho Municipality, Ghana. Ethiopian Journal of Health Sciences. 29(1): 819-830.
- Onwuchuluba EE, Soremekun RO, Oyetunde OO (2019) Medication adherence and influencing factors in patients with type 2 diabetes attending a tertiary hospital in South-West Nigeria. J Clin Sci 16(4): 138-143.






























