Functional Abdominal Pain (FAP) in Children: Knowledge, Attitude, and Practice of Pediatricians in India
Bhaswati Acharyya1, Sanjeev Joshi2, Sanjay Wazir3, AG Karthikeyan4, Vyankatesh M Chavan5, I Shrikanth Rao6, Chaitanya Balloji7, Neha8, Seema Vikas Bhagat8, Krishna Chaitanya Veligandla8, Rahul Rathod8, Bhavesh Kotak8, Manipa Saha9, Akash Bararia9 and Monjori Mitra10*
1Institute of Child Health, India
2Chirayu Criticare and Joshi Bal Rugnalay, India
3Neonatology at Cloud nine hospital, India
4Sai Mother and Child Health Care, India
5Bhagwaan Mahaveer Jain Hospital, India
6Chetana Hospital, Puttur, Udupi, India
7Clinic in Ramachandra Rao Pet, India
8Dr. Reddy’s Laboratories Ltd., India
9Medclin Research Pvt. Ltd., India
10Institute of Child Health, India
Submission:September 19, 2023; Published:November 02, 2023
*Corresponding author: Monjori Mitra, Professor Pediatrics, Institute of Child Health, 11 Biresh Guha Street Kolkata – 700017, India, Email: monjori.mitra@medclinsearch.com
How to cite this article: Bhaswati Acharyya, Sanjeev Joshi, Sanjay Wazir, AG Karthikeyan, Vyankatesh M C, et al. Functional Abdominal Pain (FAP) in Children: Knowledge, Attitude, and Practice of Pediatricians in India. Adv Res Gastroentero Hepatol, 2023; 20(2): 556031. DOI: 10.19080/ARGH.2023.20.556031.
Abstract
Background: Functional Abdominal Pain (FAP) is prevalent among children; diagnosis and management are challenging due to poorly understood etiology and lack of guidelines. We investigated pediatricians’ current knowledge, attitude, and practice with respect to FAP.
Methods: A survey was conducted between December 2022 and March 2023 via a validated questionnaire, comprising 29 pertinent questions on general characteristics of pediatricians, and diagnosis and treatment of FAP, shared with ~2000 Indian pediatricians.
Results: Responses were received from 302 pediatricians, predominantly male (68.9%), aged 40–50 years (31.1%), from Tier-I (40.9%) places, practicing in private clinics (54.8%). Most respondents identified FAP definition (74.6%) and site of pain (78.1%). Confirmatory diagnosis was mostly done on the second or third visit (90.7%); vomiting was considered the predominant red flag (86.8%). FAP was believed to be a ‘diagnosis of exclusion’ (76%). Most respondents used ROME IV criteria (53%), ordered ultrasonography (USG) (74.3%), advised antispasmodics (75.6%), and agreed that investigations in up to 30% FAP cases were ordered due to parental pressure (79%). Most respondents expected ≤30% FAP patients to improve with non-pharmacological or pharmacological approaches, or with diet modification, and preferred combinatorial management strategy (60.1%). Probiotics were advised by 67.3% respondents in ≤20% patients, mostly using single strains (67.3%). Referral rate to cross-specialties was low (<10%). Most respondents considered reduction in intensity and pain frequency as therapeutic success (61.8%).
Conclusion: A general awareness about FAP exists among Indian pediatricians; however, a consensus in diagnosis and management is lacking. Most respondents stated that guidelines might be helpful.
Keywords: Functional abdominal pain; Knowledge; Attitude; Practice; Pediatricians
Abbreviations: FAP: Functional Abdominal Pain; KAP: Knowledge, Attitude, Practice; FGIDs: Functional Gastrointestinal Disorders; FAP-NOS: Functional Abdominal Pain-not Otherwise Specified; IBS: Irritable Bowel Syndrome; FD: Functional Dyspepsia
Introduction
Functional Gastrointestinal Disorders (FGIDs) are prevalent among children due to changes in ecosystem and lifestyle. FGIDs are considered as morphological and physiological abnormalities originating from dysmotility and/or visceral hypersensitivity due to changed mucosal and immune function, microbiota, central nervous system processing, or genetic causes [1]. Functional Abdominal Pain (FAP) is a common childhood FGID with clinical features including abdominal pain accompanied by vomiting, dyspepsia, headache, bloating, constipation, or diarrhea. There is increasing evidence to suggest that the underlying etiology of FAP involves complex interactions within the ‘microbiota–gut– brain axis’ [2]. The worldwide prevalence of FAP is estimated to be 13.5% (range: 1.6% - 41.2%) with Asia reporting a pooled prevalence of 16.5% [3].
FGIDs are usually diagnosed based on symptoms since there are no specific tests or biomarkers for the same. It was in this backdrop that the symptom-based ROME criteria were developed by a group of experts in the 1990s and have ever since been revised to integrate the improved understanding about the diseases. The most recent of the ROME criteria, ROME IV, came into effect in 2016 and included revisions to the definition and diagnostic criteria of FGIDs. As per ROME IV, a patient with any of the FGIDs is defined as one for whom ‘after appropriate medical evaluation, the symptoms cannot be attributed to another medical condition’. Based on this, clinicians now have a choice of making a diagnosis without any tests or through selective clinical criteria. The categories of ‘functional abdominal pain’ and ‘functional abdominal pain syndrome’ in ROME III have been replaced by the term ‘Functional abdominal pain-not otherwise specified’ (FAPNOS) in ROME IV. Thus, patients who do not meet the criteria for irritable bowel syndrome (IBS), functional dyspepsia (FD), or abdominal migraine criteria, are now categorized as FAP-NOS [4].
In the absence of any obvious organic pathology, the ROME criteria describe FAP as ‘a dysfunction in the mechanisms involved in pain perception’ [5]. Management of FAP is challenging as patients come from different psychosocial backgrounds and vary in their responses to different treatment regimen [2]. Despite the high prevalence of FAP, there is no documented literature, to the best of our knowledge, on the approach of pediatricians to the diagnosis and treatment of this indication in India, although studies have been published elsewhere [6].
We felt that it was required to understand the knowledge, attitude, and practice of Indian pediatricians towards FAP following the latest revision of the ROME criteria, and therefore, this survey was designed based on a self-administered questionnaire for collecting pediatricians’ responses to various aspects of FAP diagnosis and management.
Methods
After obtaining approval from an Independent Ethics Committee (IEC), this survey was conducted between December 2022 and March 2023 on practicing Indian pediatricians (including few pediatric gastroenterologists) with MD/DCH/DNB degree and who provide care to patients with FAP in healthcare setups/clinics/ hospitals/colleges located across various regions of India (no minimum experience was mandatory). The survey was performed in compliance with the Indian Council for Medical Research (ICMR) and Indian Good Clinical Practice (GCP) guidelines for clinical research. A set of 29 pertinent questions (Supplementary Table 1) was designed based on a survey of literature and suggestions from an expert committee of pediatricians. This validated questionnaire was shared with ~2000 pediatricians using electronic survey administered through Google Form. Responses were analyzed to assess knowledge, attitude, and practice of pediatricians regarding FAP in children. The survey was performed using anonymized information; confidentiality of pediatricians was maintained.
Results
General characteristics of respondents
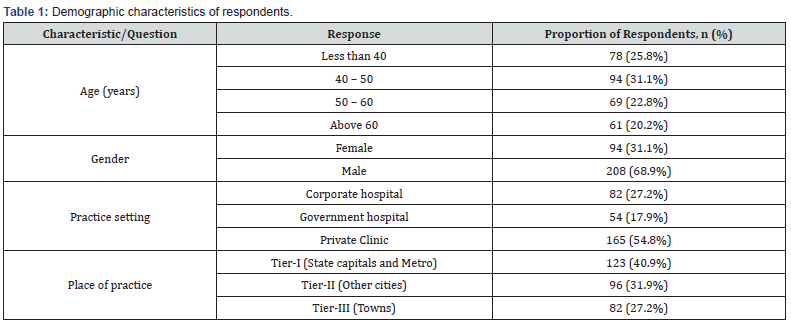
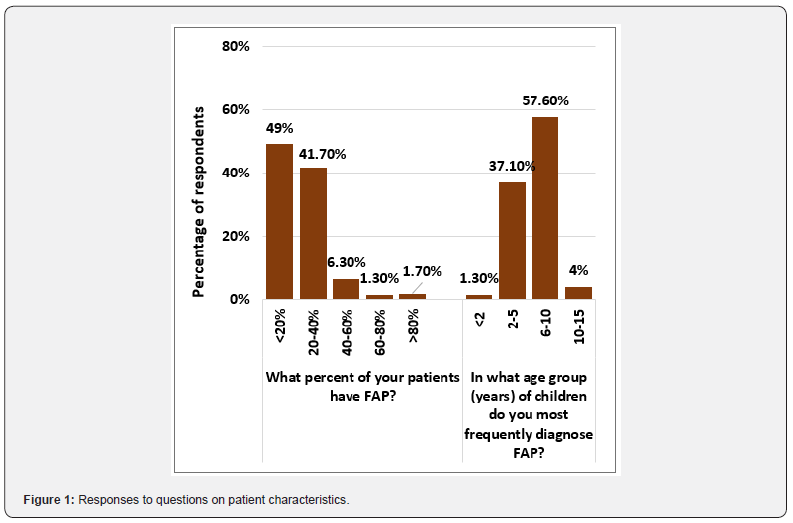
Responses to the self-administered questionnaire were received from a total of 302 pediatricians (henceforth referred to as ‘respondents’). Of these, a few chose not to respond to all questions. The actual number of respondents to each question was, therefore, used as the denominator to evaluate the percentage of responses in each case. Respondents were predominantly male (68.9%), aged 40 – 50 years (31.1%), from Tier-I places such as state capitals and metro cities (40.9%), and practicing mostly in private clinics (54.8%) (Table 1). According to 90.7% respondents, the percentage of FAP patients that they encounter is ≤40%; the most-affected age-group being 6 – 10 years, as stated by over half of the respondents (57.6%) (Figure 1).
Knowledge about FAP
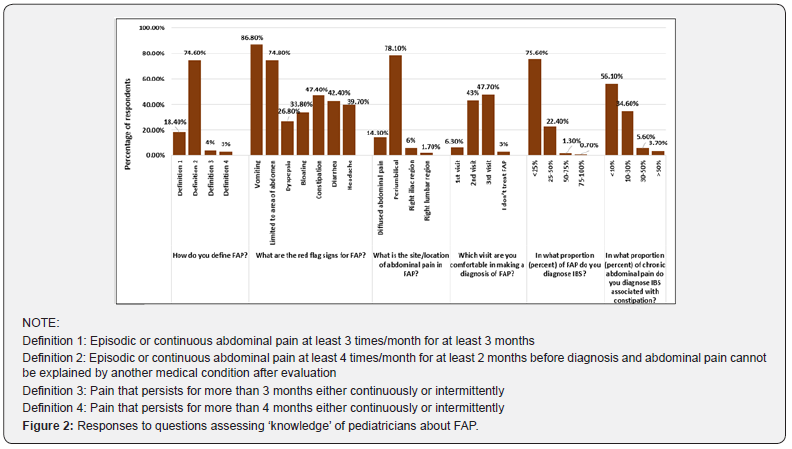
Most respondents were aware of the definition of FAP as per ROME IV criteria (74.6%) and identified the periumbilical region (78.1%) as the site of abdominal pain in FAP. Vomiting was considered as a red flag for FAP diagnosis followed by pain in limited area of abdomen by a majority of respondents (86.8% and 74.8%, respectively). Most respondents were comfortable with making a diagnosis of FAP on the second (43%) or third (47.7%) visit; very few respondents (6.30%) were confident of making a FAP diagnosis on the first visit by a patient. Most respondents believed that there is minimal overlap between the indications of FAP and Irritable Bowel Syndrome (IBS): 75.6% respondents said that they diagnose IBS in <25% FAP patients and 56.1% respondents said that they diagnose IBS associated with constipation in <10% cases of chronic abdominal pain (Figure 2).
Attitude towards FAP
Most respondents (76%) agreed or strongly agreed that FAP is a ‘diagnosis of exclusion’, that is, FAP can be confirmed only after closely related disorders are ruled out. The first line of therapy for FAP, according to most respondents (60.1%), was a combinatorial approach comprising of behavior modification, analgesics/ antispasmodics and laxatives (singly or in combination), and probiotics. These treatment modalities, individually, were considered as first line therapy by very few respondents (25.9%, 11%, and 3%, respectively). Along similar lines, most respondents (67.8%) preferred a combination of pharmacological and nonpharmacological approaches for FAP management (Figure 3).
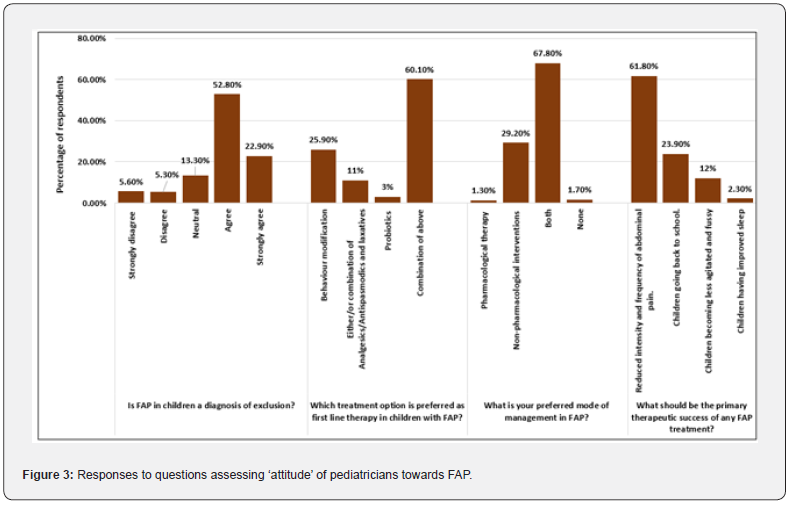
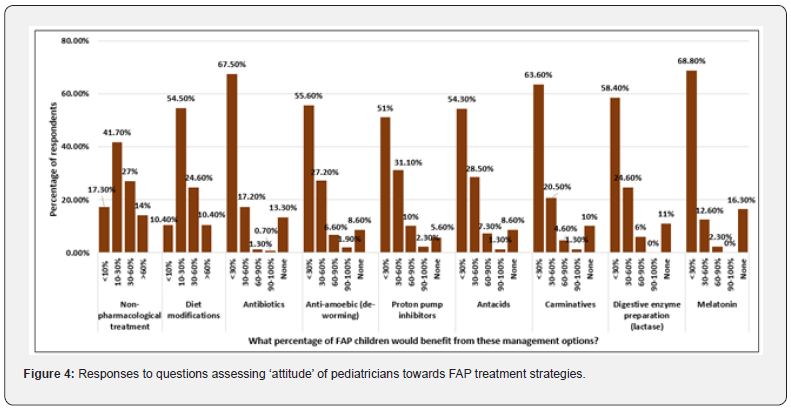
Around 10% – 30% of children with FAP were expected to get better with non-pharmacological approaches by 41.7% respondents and with diet modifications by 54.5% respondents. More than half of the respondents believed that <30% FAP patients would get better with any of the following pharmacological approaches: antibiotics, de-worming medications, proton pump inhibitors (PPIs), antacids, carminatives, lactase, or melatonin (Figure 4). Irrespective of the approach preferred, most respondents (61.8%) believed that the yardstick of a therapeutically successful FAP treatment should be ‘reduced intensity and frequency of abdominal pain’. Improved sleep, reduced agitation, and lesser absenteeism from school might be indicators of children getting better but were not considered as the ultimate goal of treatment (Figure 3). Around 98% respondents perceived a necessity of Indian guidelines for FAP.
Practice of FAP diagnosis and management
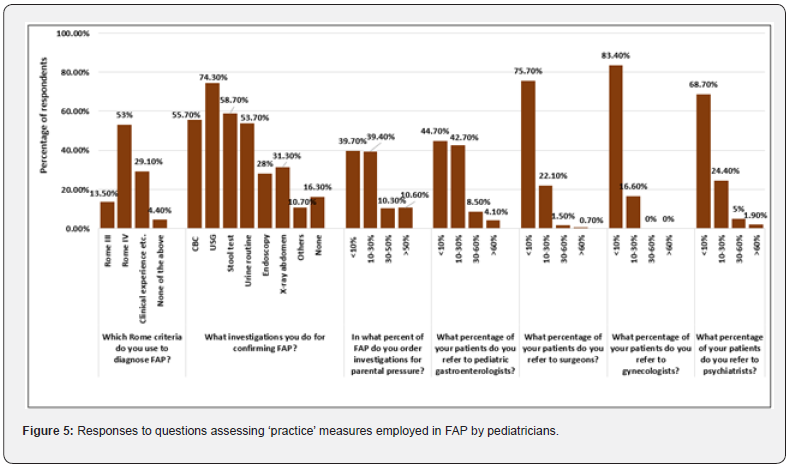
Most respondents (53%) stated that they used ROME IV criteria to diagnose FAP. Among the investigations requested for confirming FAP, ultrasonography (USG) was preferred by most respondents (74.3%), followed by stool test (58.7%), complete blood count (55.7%), routine urine test (53.7%), and others, while 16.3% respondents stated that they did not order for any investigation. Among the respondents, 79% mentioned that investigations were ordered due to parental pressure in only up to 30% FAP cases (Figure 5).
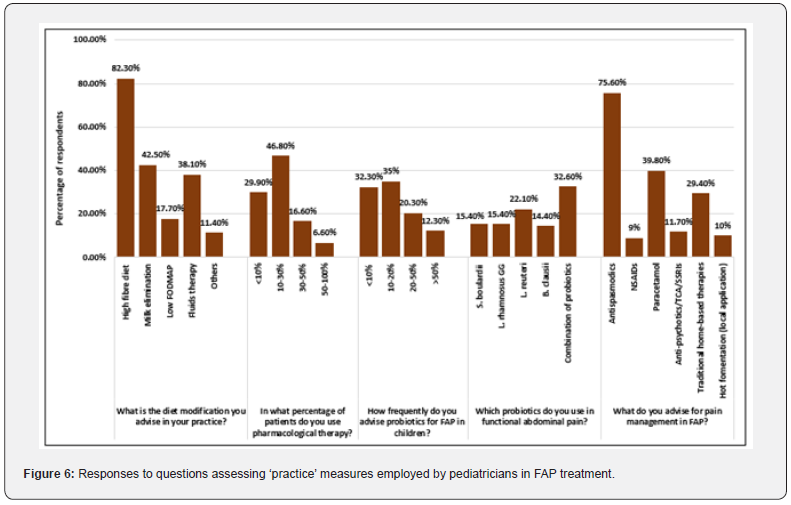
For FAP management, the diet modification most commonly advised by respondents was inclusion of high fiber food (82.3%). Other approaches opted for were milk elimination (42.5%), fluids therapy (38.1%), etc. Pharmacological therapy was used by 77% of respondents in up to 30% of children diagnosed with FAP. Probiotics were advised by 67.3% respondents in ≤20% patients, and most respondents (67.3%) used single strains. The percentage of respondents who prescribed L. reuteri, S. boulardii, L. rhamnosus GG, and B. clausii was 22.1%, 15.4%, 15.4%, and 14.4%, respectively. Combination of probiotics was prescribed by 32.6% respondents. For pain management, most respondents (75.6%) advised antispasmodics. Referral to specialists such as pediatric gastroenterologists, surgeons, gynecologists, or psyhciatrists was done for very few (<10%) FAP patients by most respondents (Figure 6).
Discussion and Conclusion
Despite the magnitude of the problem of FAP in children, there is limited literature on its diagnosis and treatment in India. With ROME IV criteria coming into effect, definition and diagnostic criteria for FAP were revised [4]. We conducted this survey hoping to gain insight into the current state of knowledge, attitude, and practice of pediatricians towards FAP. We analyzed responses of a total of 302 pediatricians to a set of 29 questions pertaining to diagnosis and management of FAP. The respondents hailed from Tier-I/II/III places and practiced in private clinics/government hospitals/corporate hospitals. No appreciable difference in response to any of the questions was evident when respondents were classified based on age, place of practice, and practice setting (data not shown).
This survey revealed that 74.6% of respondents were aware of the ROME IV criteria for diagnosis of FAP and differentiated between FAP and IBS in practice. However, only 53% used ROME IV criteria in practice. Although only <20% of patients visiting most respondents (49%) had FAP, 41.7% respondents said that 20% – 40% of their patients had FAP. Further studies on evaluating the prevalence of FAP might be useful in determining the actual incidence in India.
FAP diagnosis is made on the first visit by a very few respondents (6.3%). It is plausible that specialists such as pediatric gastroenterologists among the respondents required less time to confirm FAP diagnosis than others. This might be a possible reason why a few respondents were confident of diagnosing FAP in the first visit itself. Most respondents (90.7%) were comfortable in making a FAP diagnosis in second or third visit. Furthermore, the rate of referral to cross-specialties – in case of FAP – was found to be low in India (<10% patients are referred by most respondents to the specialists mentioned in the questionnaire). We believe that clinical practice guidelines might improve pediatricians’ approach to FAP diagnosis and perhaps make the diagnosis quicker. Varied investigations are requested in pursuit of a definitive diagnosis, some due to parental pressure as observed in this survey as well as a study from Australia [6]. Guiding principles, for instance, in the form of a flowchart, might enable a consensus amongst pediatricians in this regard. Stepwise delineation of investigations might be useful in selecting the most appropriate investigations customized for a patient based on symptoms and prognosis. This is also important since we have limited data to ascertain if the number of investigations done currently for FAP diagnosis poses any burden on healthcare services and on expenses incurred by the patients’ families. Further studies are required to assess the same.
While most respondents agreed that the primary goal of FAP treatment should be a reduction in intensity and frequency of abdominal pain, the approaches of pediatricians varied alongside their attitude towards the approaches. For instance, according to most respondents, only up to 30% of patients are expected to improve with any diet modifications, pharmacological interventions, or non-pharmacological approaches. Probiotics were advised by most respondents in only ≤20% patients. Since these multiple treatment modalities exist for FAP management, we believe that evidence-based guidelines might make the process streamlined and more efficient for pediatricians as well as patients. Similar conclusions were drawn by an earlier KAP study conducted for FAP in Australia [6].
This survey provides an overview of the general awareness about FAP among Indian pediatricians and the common approaches used in clinical practice currently. The information presented here might guide the development of evidence-based recommendations for FAP diagnosis and management by experts.
Funding
Funding for this study was provided by Dr. Reddy’s Laboratories Ltd.
Acknowledgements
The authors would like to thank all pediatricians who participated in this study. The authors would like to acknowledge the support of Medclin Research in study conduct, statistical analysis, and manuscript development.
Conflict of Interest
N, SVB, KCV, RR, and BK are employees of Dr. Reddy’s Laboratories Ltd. The other authors declare no conflict of interest.
References
- Drossman DA (2016) Functional Gastrointestinal Disorders: History, Pathophysiology, Clinical Features and Rome IV. Gastroenterology.
- Thapar N, Benninga MA, Crowell MD, Di Lorenzo C, Mack I, et al. (2020) Pediatric functional abdominal pain disorders. Nat Rev Dis Primer 6(1): 89.
- Korterink JJ, Diederen K, Benninga MA, Tabbers MM (2015) Epidemiology of pediatric functional abdominal pain disorders: a meta-analysis. PloS One 10(5): e0126982.
- Hyams JS, Di Lorenzo C, Saps M, Shulman RJ, Staiano A, et al. (2016) Functional Disorders: Children and Adolescents. Gastroenterology.
- Benninga MA, Faure C, Hyman PE, St James Roberts I, Schechter NL, et al. (2016) Childhood Functional Gastrointestinal Disorders: Neonate/Toddler. Gastroenterology.
- Heinsch ML, Nightingale S (2019) Functional gastrointestinal disorders in children and adolescents: Knowledge, practice and attitudes of Australian paediatricians. J Paediatr Child Health 55(9): 1063-1069.






























