In Search of an Exact and Cheap, Radiation and Intervention-Free Method Diagnosis of HCC and Malignant Tumors of the Liver Doppler Study of HCC and Conclusions
Muhammad Anwar1*and Ayesha Anwar Raza2
11University of Lahore, Pakistan
22Department of Allied Health Sciences University of Lahore, Pakistan
Submission:March 17, 2022; Published:March 31, 2022
*Corresponding author:Muhammad Anwar, University of Lahore, Pakistan
How to cite this article:Muhammad A, Ayesha Anwar R. In Search of an Exact and Cheap, Radiation and Intervention-Free Method Diagnosis of HCC and Malignant Tumors of the Liver Doppler Study of HCC and Conclusions. Adv Res Gastroentero Hepatol, 2022; 18(4): 555991. DOI: 10.19080/ARGH.2022.18.555991.
Abstract
Introduction: Nevascularization develops around the HCC and malignant tumours of liver in basket form. This leads to increased blood supply via hepatic artery. We have tried to do quantification of hepatic artery, basket vessels and feeding vessels wherever it is found. We have accumulated data of liver tumours (malignant) from 2013 to sep.2021 from our colour Doppler centre. Our centre is located in Punjab province of Pakistan. Here prevalence of hepatitis C in 6.5% which is very high [1]. China has the highest burden of HCV infection cases. Pakistan has the second highest burden of HCV positive cases [2] This is a retrospective study.
Objective: The purpose of this study was to establish the peak systolic velocity of hepatic artery of hepatis malignant lesion which are found hepatitis c and hepatitis B related complication.
Materials and Method: Study comprises of 120 patients with almost equal females & males of age 40 to 70 years. It began in April 2013 and continues. Verbal consent was taken to include in this study. I have studied liver cancers a specially HCC and I am of the opinion that PSV 80cms/sec should be a cut off value between benign and malignant tumours. Can we set it a gold standard.
Subjects & Methods: Study comprises of 120 patients with almost equal females & males of age 40 to 70 years. It began in April 2013 and continues, in our outdoor during their USG consultation, with convex probe. The multifrequency transducer 2.5 to 6.0mHz was used. Hepatic artery was interrogated (seldom) at the head of pancreas with angle correction or in liver along with portal vein without angle correction (as at this naturally angle is corrected) in fasting state to keep the measurements uniform as food intake profoundly increases the PSV. Basket or circumferential vessels and feeding vessels were also studied. Results: The normal PSV in normal subjects is 25 to 40cm/sec. It goes upto 60cm/sec, he normal PSV in normal subjects is 25 to 40cm/sec. It goes upto 60 cm/sec in cirrhotic, if it goes beyond that, portal vein tumor or HCC will be suspected.we can take PSV of 80 cms/sec a cut off between benign and malignant tumours. Future and further research and validation is requested to other colleagues.
Keywords:HCC; Color doppler; Duplex scan; PSV of hepatic artery; PSV of basket pattern; Feeding vessels
Introduction
We wanted to find a near sure method of identifying HCC in a non-invasive and radiation-free way. As in our country, a Triassic CT Scan is available at district headquarters hospitals only and biopsy is invasive, I used PSV of the hepatic artery to find a cut-off for a malignant tumor. Furthermore, basket pattern vessels and feeding vessels were also studied for duplex scan and important results were drawn.
As we know that neovascularization is the hallmark of HCC and this leads to increased blood supply via the hepatic artery which leads to an increase in caliber and PSV of Doppler signal,basket vessels and feeding vessels in HCC also show a peculiar pattern. We have accumulated data of liver tumors (malignant) from 2013 to Sep. 2020, from our color Doppler center. Our center is located in the Punjab province of Pakistan. Here prevalence of hepatitis C is 6.5% which is very high [1]. China has the highest burden of HCV infection. Pakistan has the second-highest burden of HCV-positive cases [2].
Study design and study participants
This is a prospective, single-centered, randomized, observational study. Participants were adult’s patients of both sexes. They presented voluntarily at our color Doppler center and verbal consent was taken, patients were informed about the possible use of data for research purposes.
Background
Malignant tumors grow in an uncontrolled fashion with the propensity to spread into the surrounding tissues. Both these critical features are closely dependent on the tumor vascular network [1-3]. The development of neo-formed vessels is essential for tumor growth [4]. An increased number of unpaired arteries detected defines the vascular profile which differentiates hepatocellular growth as neoplastic rather than hyperplastic in small nodules of the cirrhotic liver with undefined malignant potential [5,6].
Tumor vascularization shows some peculiar biological and morphological features. Firstly, it is not self-limited and tends to grow indefinitely according to the biological behavior of the tumor. Secondly, it develops as a complex, chaotic network at the growing edge of the tumor with irregular and winding branches penetrating the nodule with a radial shape. The number of vessels within the tumor is often, but not always, increased, so that hyper vascularity is a common feature anastomosis between adjacent arteries and veins, mainly at the periphery of the nodule, are frequently observed [7,8].
Portal vein inflow 2/3, arterial inflow 1/3.90% of oxygen supply is via the hepatic artery. The artery supplies the disease process. Hepatic Artery is solely responsible for this increased blood supply. In The author’s experience, the use of highly sensitive color flow demonstrates neovascularization in virtually all hepatocellular carcinomas. For the reasons stated above, color flow is not optimal for demonstrating this neovascularization, and, in practice, Pulse-Doppler must be used to interrogate any vascular areas seen on the periphery of a tumor. Utilizing transducer angulations to optimize the Doppler shift, a Doppler shift greater than 2.5kHz (at an insinuating frequency of 3MHz) or with an angle corrected velocity greater than main hepatic artery is highly suggestive of malignancy [9]. The hepatic artery typically shows a splanchnic waveform, with a normal maximum velocity of 55.2+-12.0cm /sec. In cirrhotic patients, especially when portal vein thrombosis may occur, this value can increase up to 64.4+- 21.8cm/sec Peak systolic velocity of hepatic artery 30-60cm /sec2. In cirrhotic it rises to 70cm /sec.
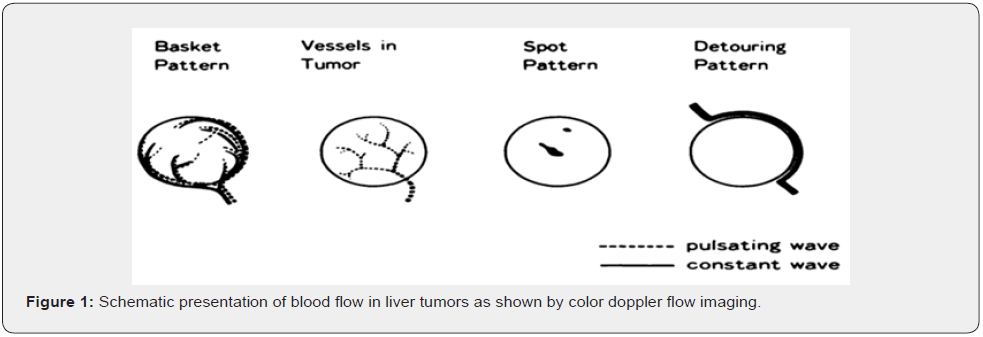
Taylor et al reported that a high-velocity Doppler signal was detected in hepatocellular carcinoma tumors when pulsed-wave Doppler sonography was used; they suggested that this signal was associated with large pressure gradients due to arteriovenous shunting. In our study, we also observed a fast-pulsating blood flow of 70-90cm/sec in maximal velocity in feeding arteries entering the tumor, which form part of the basket pattern. Furthermore, in addition to the pulsating wave, a constant wave could be detected in the periphery in hepatocellular carcinoma. Comparing the blood flows shown on the color image with angiographic findings, we found that the blood flow that creates the basket pattern is the portal vein displaced around mass lesions and feeding arteries surrounding tumor nodules. Also, the blood flow within the tumor displayed by color imaging is the pulsating tumor vessel running within the tumor (Figure 1).
Knowledge of the Doppler shift produced by RBCs but in the form of a frequency shift, it is not easily used. For example, the researchers at a particular lab may determine that a 5kHz shift is generated by hemodynamically significant stenosis. Given this information, the first question we must ask is “what Doppler frequency are you using and what Doppler angle did you use? “Clearly, without providing these two important parameters the determination of a 5kHz shift is useless information. For this reason, although the pioneering researchers often related their data in terms of the kilohertz shift. It soon became apparent that if the data was converted into velocities much of this ambiguity could be removed. Today, almost all spectral displays generate velocity-time spectra rather than frequency-time spectra [10].
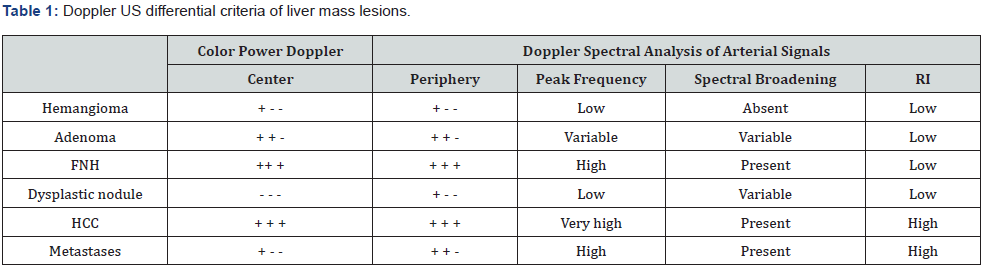
Although CT is considered the technique of choice in the initial evaluation and subsequent follow-up of hepatic masses, its accuracy is highly dependent on proper technique. The specificity of CT is limited, particularly in the setting of a solitary small lesion. Furthermore, features considered diagnostic of hematoma on CT occur with reduced frequency in the non-Asian population. The diagnostic accuracy of MR imaging in distinguishing hemangiomas from metastases can vary depending on the histologic type of the primary tumor, the strength of the magnetic field and the size of hemangiomas studied. In addition, the high cost and limited availability of MR imaging currently make it impractical as a primary method for diagnosing hepatic lesions (Table 1).
Equipment
B-scan, color Doppler, and duplex evaluation were done on soundscape S20 and later on logic 7. The insolating frequency of 3-5Hz was used for greyscale image & for color Doppler frequencies of 2.0, 2.4, and 3.3 were used, PRF of Doppler was 4, increased to 6, and a few times to 8 where Doppler aliasing occurs.
The Doppler of the hepatic artery was seldom taken in the head of the pancreas due to the need for angle correction, it was taken in the intrahepatic portion where it was almost perpendicular to insolating beam making an angle of less than 30. Where multiple HCC lesions were present, only the lesion with the highest PSV of basket vessels was recorded and mentioned.
Subject & method
The study comprises more than 120 patients with almost equal females & males of age 40 to 70 years. It began in April 2013 and was completed at the end of February 2021. Doppler signal of hepatic artery was measured along with Doppler signal of basket and feeding vessel. Any other important finding for example BCS, SMV thrombus, and gut ischemia was searched for and mentioned. In patients with more than one mass in the liver, only the mass with the highest PSV was considered and analyzed with color and spectral Doppler. Therefore, for purpose of data analysis, only one lesion was considered. All patients present them for ultrasound examination after the appointment. Verbal consent was taken to include in this study.
Objective
It has been studied in past qualitatively but not quantitatively. In this study, quantification is made of PSV of hepatic artery Doppler and circumferential arteries (basket vessels). Portal vein inflow 2/3 arterial inflow 1/3.90% of oxygen supply is via the hepatic artery. The artery supplies the disease process [11-13].
Hepatic Artery is solely responsible for this increased blood supply. In The author’s experience, the use of highly sensitive color flow demonstrates neovascularization in virtually all hepatocellular carcinomas. For the reasons stated above, color flow is not optimal for demonstrating this neovascularization, and, in practice, Pulse-Doppler must be used to interrogate any vascular areas seen on the periphery of a tumor. Utilizing transducer angulations to optimize the Doppler shift, a Doppler shift greater than 2.5kHz (at an insulating frequency of 3MHz) or with an angle corrected velocity greater than main hepatic artery is highly suggestive of malignancy [14] (Figures 2-4).
Results
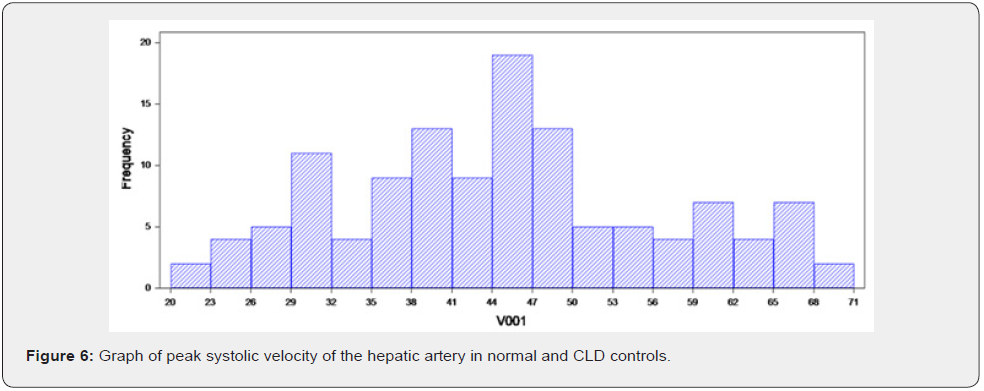
PSV of hepatic artery in normal and CLD controls, 126 subjects were used as control
Average 45.31cm/sec
Minimum of 22cm/sec
Maximum of 70cm/sec
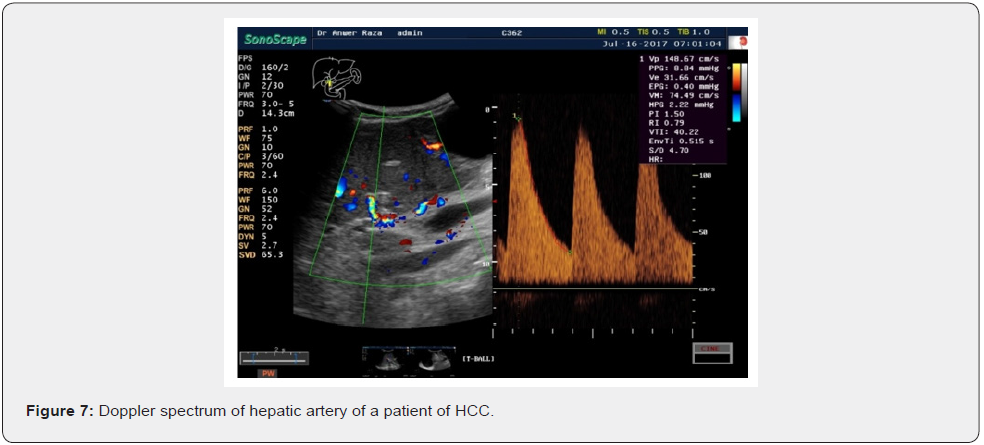
In all liver carcinomas especially HCC
Average 155cm/sec.
Minimum 80cm /sec.
Maximum 343cm/sec.
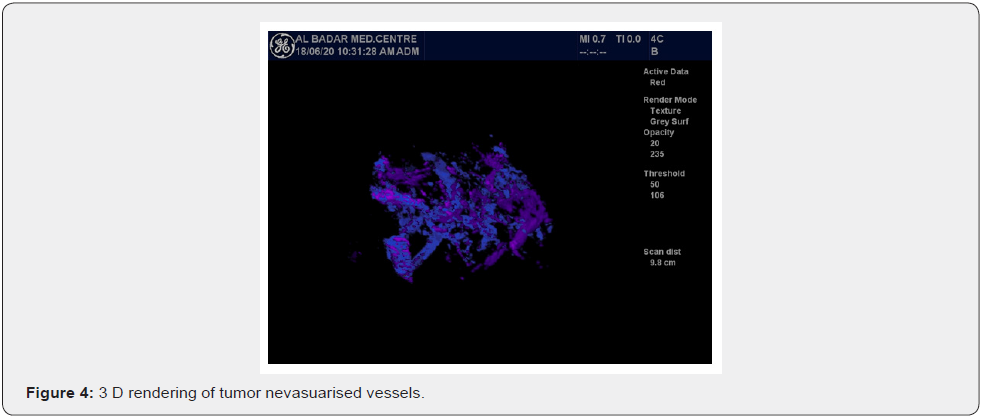
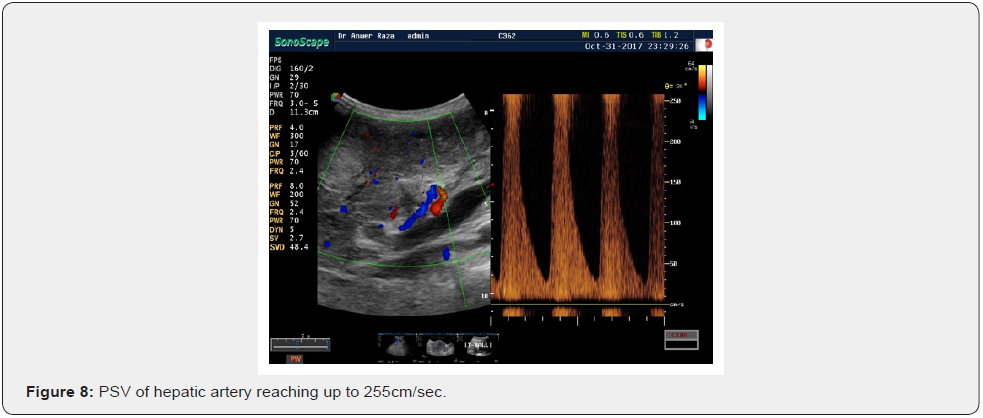
The most interesting phenomenon is of increased velocity around the tumor itself, whether it is the velocity of Basket Pattern or some penetrating or feeding artery. They all are not present in the normal liver. They had developed anew and show increased PSV even higher than the corresponding hepatic artery. Here the average PSV is 141 cm/sec, minimum being 95 cm/sec and maximum falling in the range of 266 cm/sec. Some intratumoral arteries show flow away from the probe which they should show as per rule. All basket vessels show aliasing due to high flow (Figures 5-12).
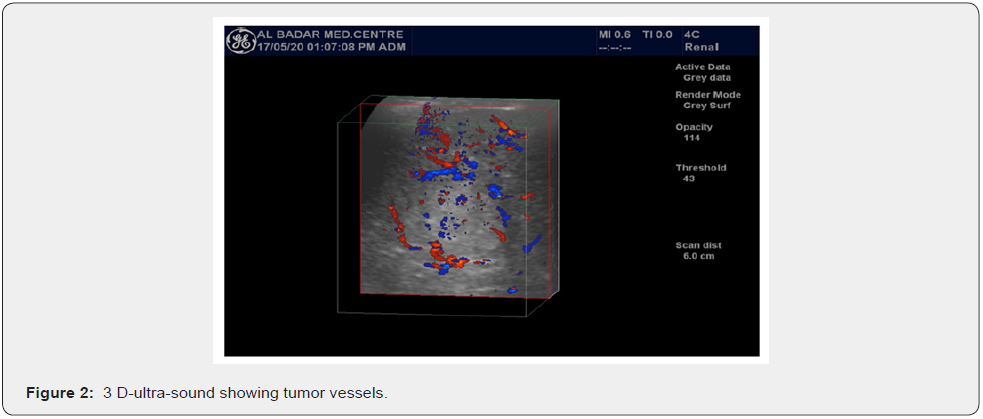
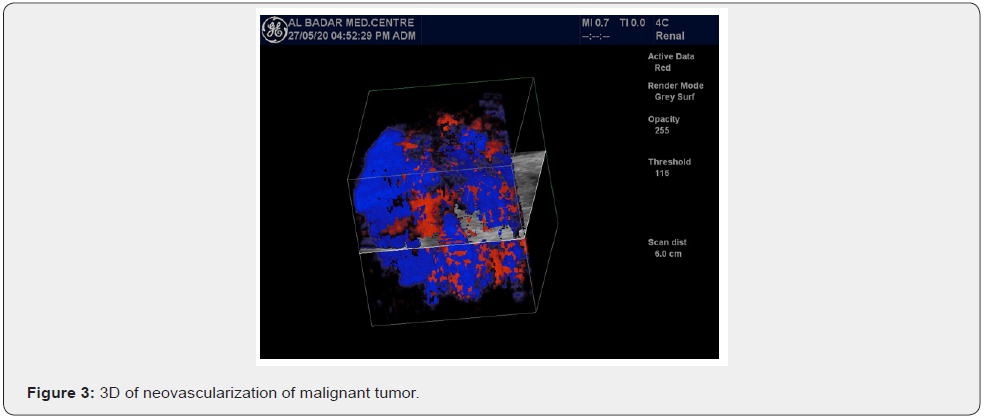

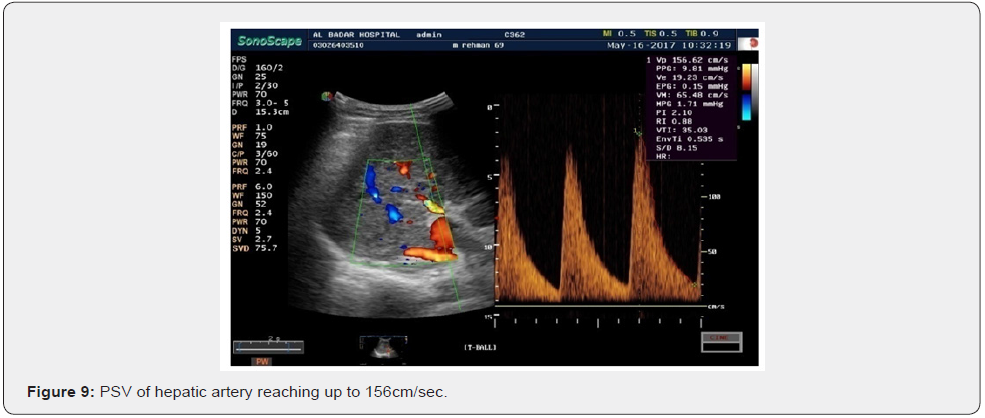
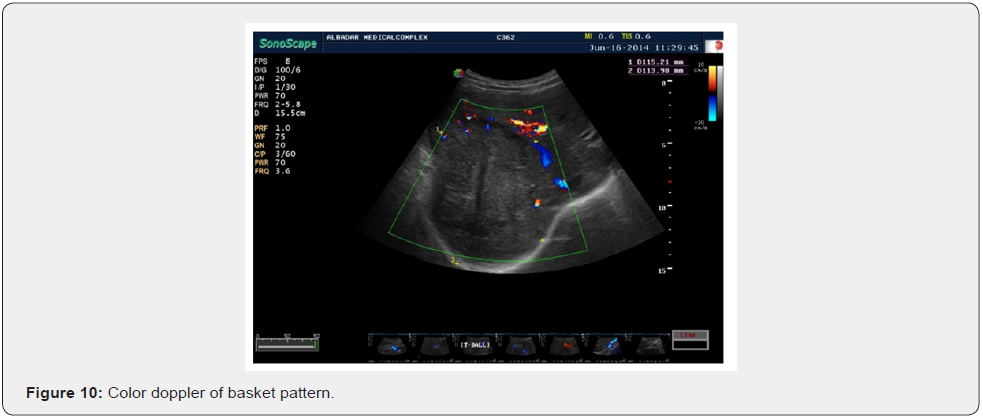

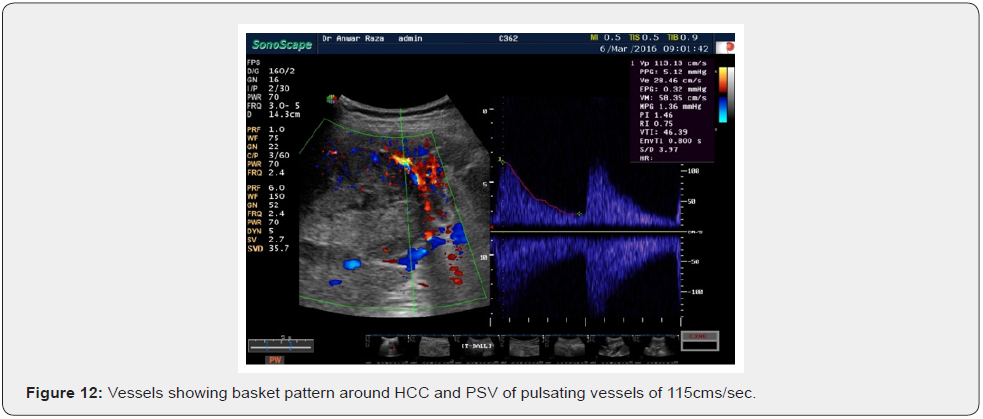

Minimum….65cm/sec.
Maximum……311cm/sec
Average….135cm/sec
A high-velocity Doppler signal was detected in hepatocellular carcinoma tumors when pulsed-wave Doppler sonography was used; they suggested that this signal was associated with large pressure gradients due to arteriovenous shunting. In our study, we also observed a fast-pulsating blood flow of 70-90 cm/sec in maximal velocity in feeding arteries entering the tumor, which form part of the basket pattern. Furthermore, in addition to the pulsating wave, a constant wave could be detected in the periphery in hepatocellular carcinoma. Comparing the blood flows shown on the color image with angiographic findings, we found that the blood flow that creates the basket pattern is the portal vein displaced around mass lesions and feeding arteries surrounding tumor nodules. In our study, we found this velocity of feeding pulsating artery about (Figures 13-19).
266cm/sec.
Minimum…..20cm/sec,
Maximum.…266cm/sec
Average……108cm/sec.
Maximum of feeding vessels 286cm/sec
Minimum PSV of feeding vessels 20cm/sec
Average PSV of feeding vessels 108cm/sec.
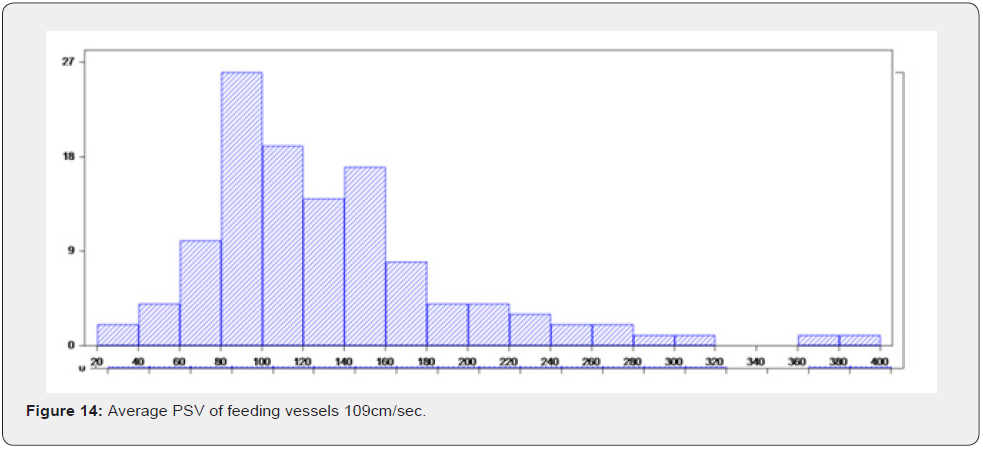
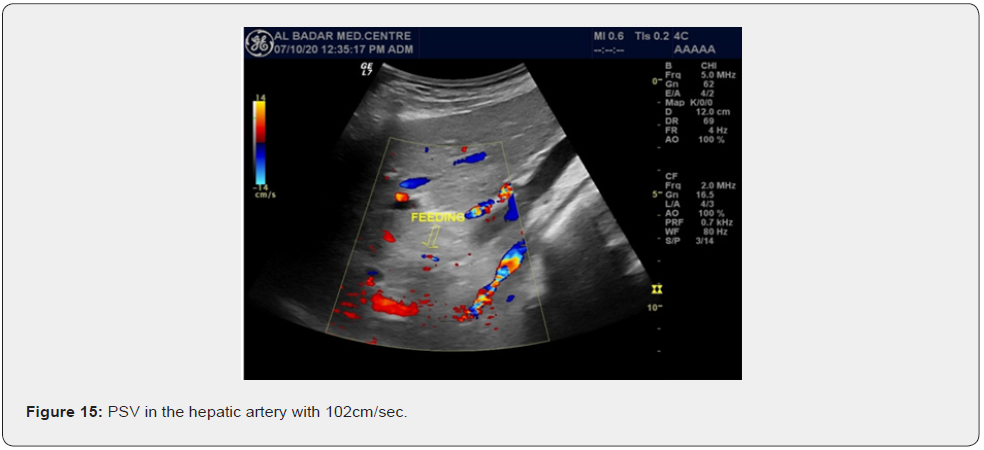
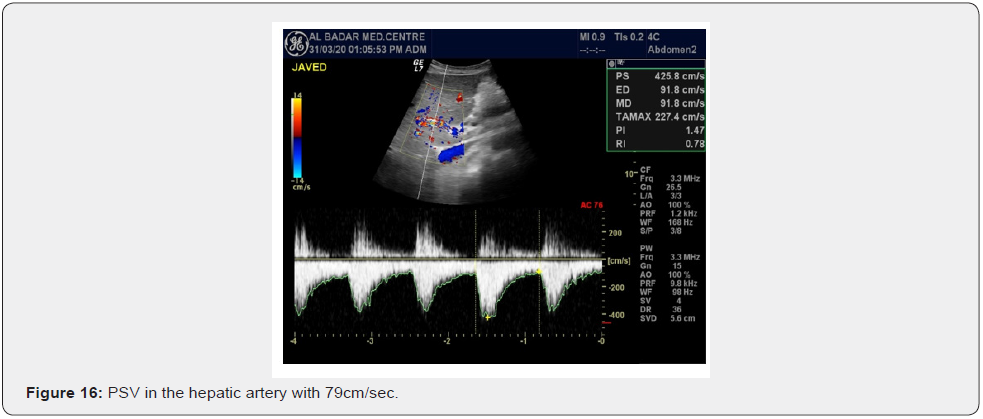
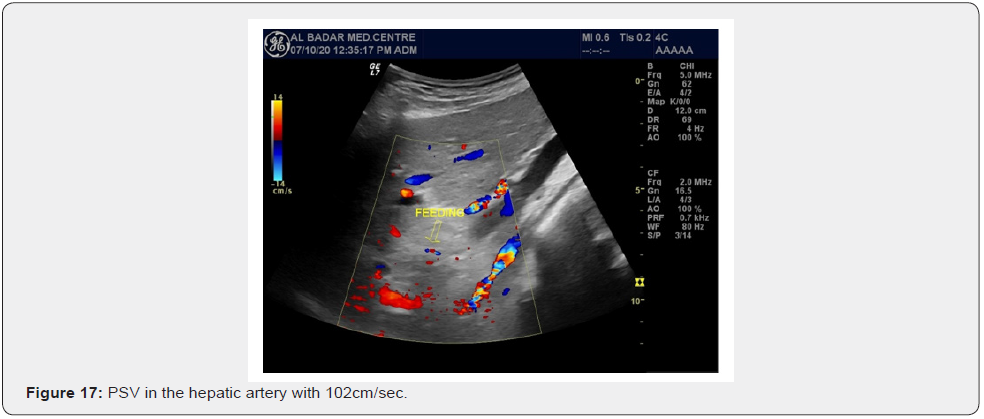
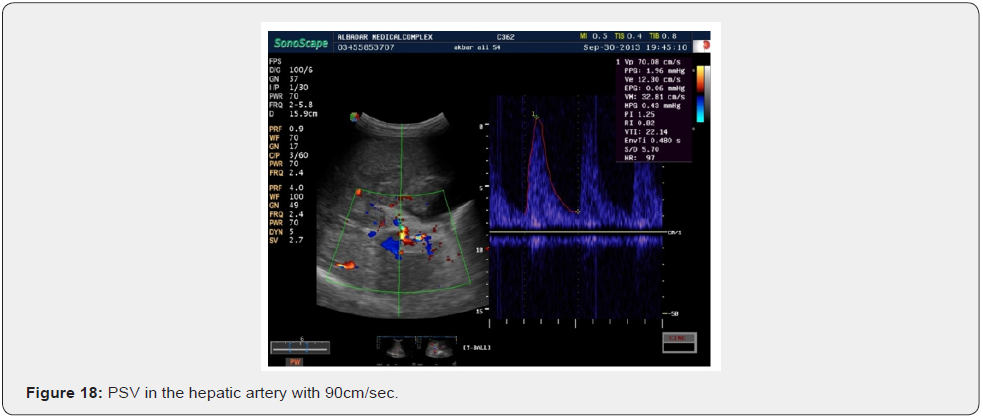
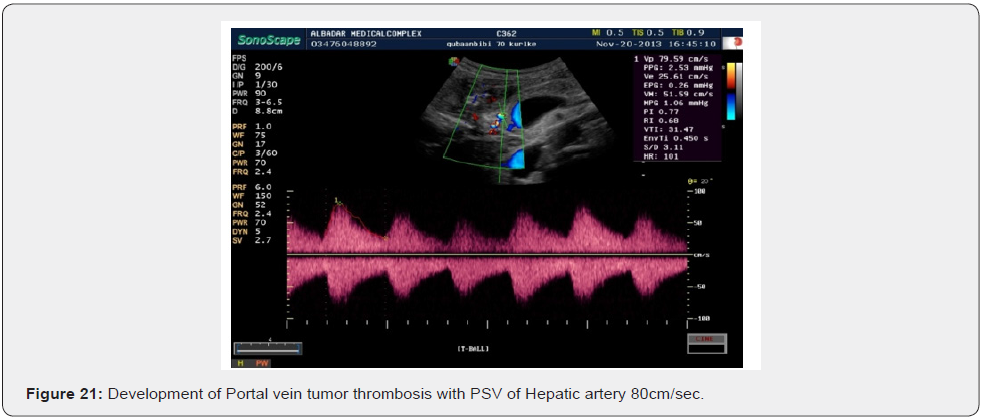
Follow up Scan of two patients scan was done. A female patient was scanned on 20th November 2013. She had compensated cirrhosis and PSV in the hepatic artery was 79cm/sec. She again presented for Doppler on 22nd December 2014. She developed partial portal vein tumor thrombosis.PS V of hepatic artery increased to 102cm/sec.
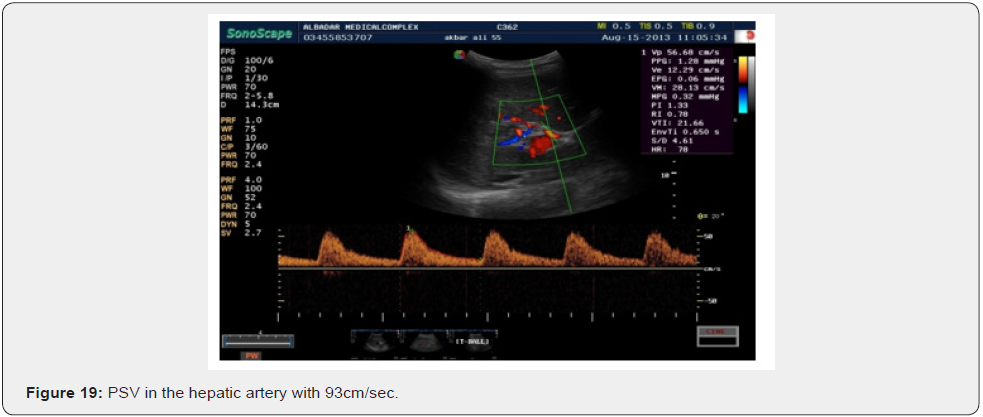
The second patient was a male of 55 years of age. He had partial portal vein tumor thrombosis and the PSV of the hepatic artery was 56cm/sec. on August 15, 2013. He again came back after 2 months back on Sep 30th. His PSV was 90cm/sec. patient (Figures 20-22).
Third patient
The third patient female of 50 years with chronic HBV infection. PSV of the hepatic artery was 38 cm/sec. in September 2023, with the development of HCC in December 2014 PSV of hepatic artery raised to 93 cm /sec.
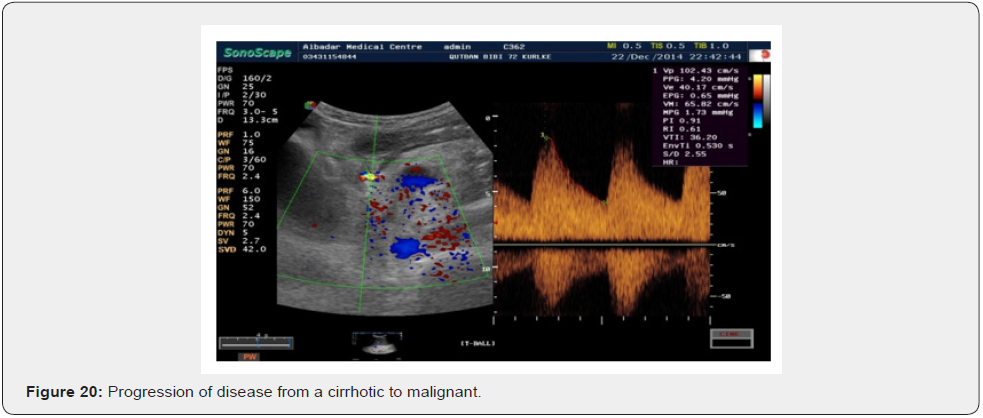
This clearly indicates that with the progression of disease from a cirrhotic to malignant, or a malignant to increased severity of malignancy, we find an increase in PSV of the hepatic artery [15].
HCC at the periphery of liver
A special trend of HCC in the periphery of Segments of V, VI,VII, and VIII. HCC developing at the periphery of these segments increase in size slowly and in some instances, patients survive some 1,5 years after their first appearance
a) Patient A
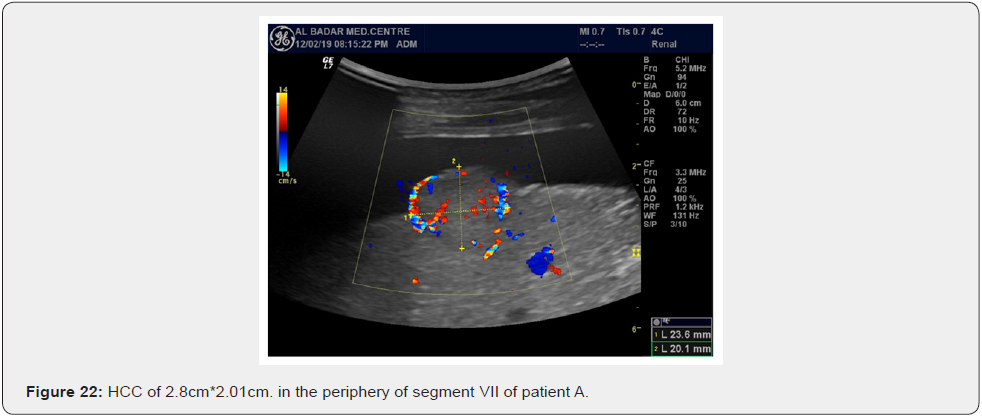
Patient A shows its first use appearance in our clinic of HCC of 2.8 comes*2.01 comes in the periphery of segment VII. He was referred to a tertiary care hospital for resection where doctors refused its presence and continued the line of antiviral treatment of HCV (Figure 23).

Patient was called for follow up 25th June 2019.At this date its size increased by almost to double and on January 2020 it was almost tripled. After second scan she was again referred there they refused to treat saying that she had HCC and could not be respected and traced. He was again referred to tertiary care hospital. They found it and declared it undertake now after diagnosing it as a case of HCC and portal vein tumor thrombosis. The followings are size and Doppler parameters at given dates of this patient. The patient died soon after (Tables 2-4).


b) Patient B
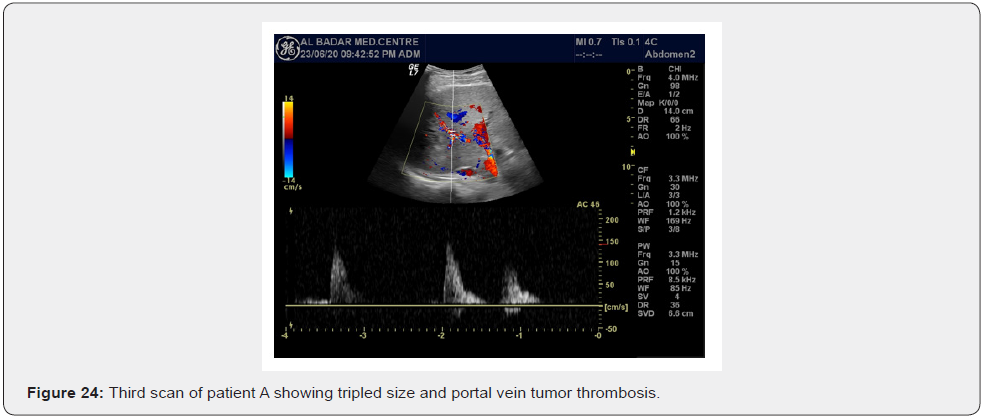
A middle-aged male patient having HC + ve with sudden loss of weight and increasing ascites. The HCC was located in segment VI of the liver. It developed from 2.3 cm to 5.6 cm over 8 months, Further more tumour thrombosis in portal vein had developed (Figure 24).
c) Patient C
A male of 55 having CLD and HCV presented on 18 10 18 with a SOL in segment vi of liver .it measured 5.06*4 6 cm. on 18 3 20, he was again scanned almost doubled the size. on 29 6 20 it increased rapidly and portal vein was blocked with tumor.
Conclusion
All liver malignant tumors, primary or secondary, need an increased blood supply, hence PSV of the hepatic artery increases more than 80 cm/sec. this we can use as a gold standard in a limited resource population, as a confirmatory tool for HCC and other malignant tumors.
a) HCC is a specific tumor in which basket pattern vessels or circumferential vessels around the big HCC show more velocity than the hepatic artery and this rises even up to 235 cm/sec. in our study,
b) Feeding or penetrating vessels show pulsatile flow and this sometimes reach more than basket pattern vessels and this is often below the baseline.
c) With the increase in the size of the tumor the PSV of the hepatic artery increases.
d) HCC presenting at the periphery of segments V, VI, VII, and VIII increase in size slowly and perhaps have better treatment options.
e) Malignant tumors having developed portal vein tumor thrombosis show poor prognosis. It’s open for future researchers to further explore this topic of increased blood supply and its various indices.
References
- Shubik P (1982) Vascularization of tumors: a review. J Cancer Res Clin Oncol 103: 211-222.
- Schor AM, Schor SL (1983) Tumor angiogenesis. J Pathol 141: 385-413.
- Moore JV, West DC (1991) Vasculature as a target for anticancer therapy. Taylor and Francis, London.
- Folkman J, Merler E, Abernathy C, Williams G (1971) Isolation of a tumor factor responsible for angiogenesis. J Exp Med 33(2): 275-288.
- Park YN, Yang CP, Fernandez GJ, Cubukcu O, Thung SN, et al. (1998) Neoangiogenesis and sinusoidal capillarization in dysplastic nodules of the liver. Am J Surg Pathol 22(6): 656-662.
- Roncalli M, Roz E, Coggi G, Di Rocco MG, Bossi P, et al. (1999) The vascular profile of regenerative and dysplastic nodules of the cirrhotic liver: implication for diagnosis and classification. Hepatology 30(5): 1174-1178.
- Strickland B (1959) The value of arteriography in the diagnosis of bone tumors. Br J Radiol 32: 705-713.
- Gammil SL, Shipkey RB, Himmelfarb EH, Parvey LS, Rabinowitz JG (1976) Roentgenology - pathology correlative study of neovascularity. Am J Roentgenol 126(2): 376-385.
- Current Medical (2009) lmaging Review 5(1).
- Johnson G, Nix L (1987) Clinical applications of Doppler Ultrasond. In: Taylor KJW, (2nd edition), Chapter 17.
- (2010) The Burwin institute of diagnostic medical ultrasound, ultrasound physics and instrumentation, module two-page p. 2-78.
- Choi BI, Kim TK, Han JK, Chung JW, Park JH, et al. (1996) Power versus conventional color Doppler sonography: comparison in the depiction of vasculature in liver tumors. Radiology 200(1): 55-58.
- Young LK, Yang WT, Chan KW, Metreweli C (1998) Hepatic hemangioma: quantitative color power US angiography - facts and fallacies. Radiology 207: 51-57.
- Kim TK, Han JK, Kim AY, Choi BI (1999) Limitations of characterization of hepatic hemangiomas using a sonographic contrast agent (Levovist) and power Doppler ultrasonography. J Ultrasound Med 18(11): 737-743.
- Choi BI, Kim TK, Han JK, Kim AY, Seong CK, et al. (2000) Vascularity of hepatocellular carcinoma: assessment with contrast-enhanced second harmonic versus conventional power Doppler US. Radiology 214(2): 381-386.






























