Aesthetic Management in Direct Composite of a Patient with an Oligodontia
Carrié A*, Fournier B, Colon P, De La Dure Molla M, Vifane B and Apap F
Department of Odontology, University of Paris, Rothschild Hospital APHP, France
Submission: January 26, 2022; Published: February 03, 2022
*Corresponding author: Carrié A, Department of Odontology, University of Paris, Rothschild Hospital APHP, France
How to cite this article: Carrié A, Apap F, Deladure Molla M, Vi-fane B, Colon P, et al. Aesthetic Management in Direct Composite of a Patient with an Oligodontia. Adv Dent & Oral Health. 2022; 15(2): 555908. DOI: 10.19080/ADOH.2022.15.555908
Abstract
Taking care of patients with rare diseases challenges our daily practice. It confronts us at exceptional clinical situations with patients presenting specific oral phenotype and an altered dental capital. The objectives of the treatment are to preserve the present teeth, to improve the masticatory and phonatory function, the aesthetics, and to promote the emotional and psychological well-being of the patient. Therefore, the management of these patients is based on a multidisciplinary cooperation between the treating dentist, the dentists of the specialized centers (experts in pediatric dentistry, prosthetic rehabilitation, implantology, periodontology, specialists in oral medicine, dentofacial orthopedics, oral surgery), maxillofacial surgeon, the attending physician and geneticist. In a societal context where appearance is becoming increasingly important, aesthetic treatment are essential. However, genetic rare diseases impact young children and it is necessary to treat them and to plan the next steps, meaning without damaging the future possibilities. With the use of contemporary bonding techniques and new composite resins, it is possible to restore anterior teeth in the direct technique in the most conservative way possible while achieving good esthetic and functional results at a lower cost. These types of restorations, unlike indirect restorations, require very little or no excessive preparation of the teeth and have the advantage of being scalable. However, these techniques are still subject to rigorous clinical rules and procedures in order to obtain the expected results. In this article we illustrate the anterior maxillary aesthetic management of a 22-year-old patient treated at the Reference Center for oral and dental rare diseases (O’RARES Rothschild Hospital, AP-HP, Paris) for oligodontia associated with dental morphology anomalies. Oligodontia is a rare anomaly of dental development characterized by the absence of 6 or more teeth. The objective of this article is to show the application of current bonding techniques in a patient with a rare pathology: an isolated oligodontia.
Keywords:Oligodontia; PAX9 mutation; Morphology anomalies
Introduction
Taking care of patients with rare diseases challenges our daily practice. It confronts us at exceptional clinical situations with patients presenting specific oral phenotype and an altered dental capital. However, the aesthetic and functional objectives remain the same as every patient: preserve the present teeth, improve the masticatory and phonatory function, the aesthetics, and promote the emotional and psychological well-being of the patient. A supplemental difficulty arises from taking care of patients from a young age until adulthood. Genetic rare diseases impact young children and it is necessary to treat them and to plan the next steps, meaning without damaging the future possibilities. Oligodontia is a rare anomaly of dental development characterized by the absence of six or more teeth. The prevalence of oligodontia is 0.14% [1]. It is a genetic anomaly, which can be transmitted to patient’s children. These mutations disrupt the mechanisms regulating the pattern of odontogenesis or the progression of dental development. Many genes may be involved. The mutated genes also impact the nature of the agenesis teeth [2], for example a PAX9 mutation will associate with posterior teeth agenesis.
Clinical signs include the absence of 6 or more teeth, lack of development of maxillary or mandibular alveolar bone height, and a reduction in lower facial height. Oligodontia may also associates with dental morphologies anomalies of size (smaller teeth) and shape (conical teeth, taurodontism) [3,4]. Exfoliation delays of primary teeth are frequently associated with the agenesis teeth. To make the diagnosis, clinical examination and panoramic radiographs are required. Late eruption of teeth, persistence of temporary teeth, alveolar bone hypotrophy, and the presence of diastemas also associate with oligodontia [4]. With the use of contemporary bonding techniques and new composite resins, it is possible to restore anterior teeth in the direct technique in the most conservative way possible while achieving good esthetic and functional results at a lower cost. These types of restorations, unlike indirect restorations, require very little or no excessive preparation of the teeth and have the advantage of being scalable. The objective of this article is to show the application of current bonding techniques in a patient with a rare pathology: an isolated oligodontia.
Case Report
Medical History
A 22-year-old patient, with no relevant medical history, is treated at the Reference Center for oral and dental rare diseases (O’RARES Rothschild Hospital, AP-HP, Paris) for oligodontia associated with dental morphology anomalies. He is referred by his orthodontist to complete the oral rehabilitation. The maxillary orthodontic treatment is completed but still ongoing at the mandible. The orthodontist would like the maxillary teeth to be restored before refining the lower arch. At the orthodontist’s level, the movements start to become limited and complicated so the orthodontist would like an ideally restored maxillary arch to have a reference for the mandibular arch. On his side, the patient wants to improve his smile aesthetics.
Analysis of the initial situation
The initial situation shows long and thin teeth, misshaped (coronoid) canines, visible diastemas and a deviation of the midline. We note the absence of the teeth number 15, 41, 44, 47, 34, 37 with persistence of temporary teeth: 55,75,85,73 (Figure 1a
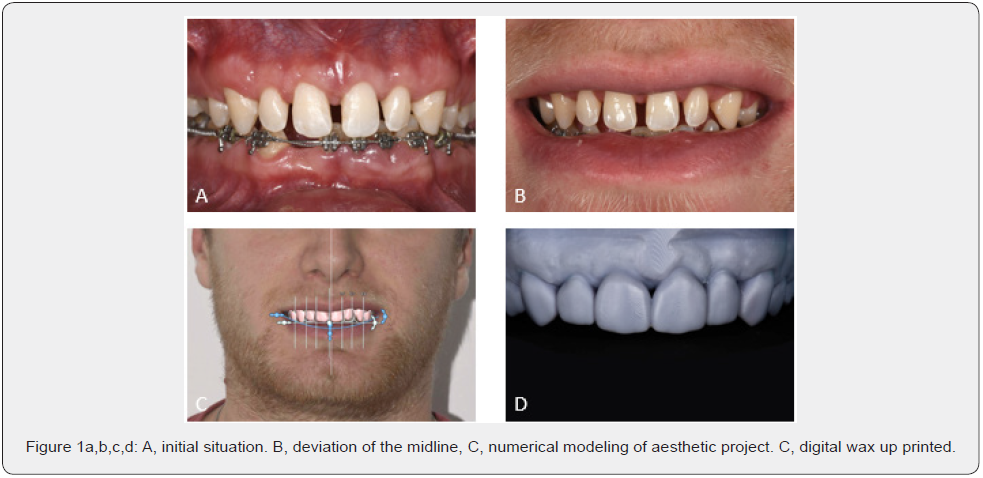
Therapeutic decision [5] Table 1

In this case report, composite resins can be used to improve the esthetics of the smile at a low cost and with relatively high clinical performance[6]. The survival rates of anterior composites were >90% and 50% at 2 5 and 5 years, respectively [7]. The presence of an effective posterior wedge influences the success rate [7]. However, the success of free-hand bonding in anterior teeth depends on a harmonious integration of various elements, including a thorough understanding of natural function, aesthetics, characteristics of current materials, and restorative techniques [8].
Clinical implementation
Realization and validation of an aesthetic project
The initial step consisted in the elaboration of an esthetic project. Digital impressions, photography from the face were taken and a digital wax up was generated using a CAD-CAM software (Figure 1c) and a model was obtained by stereolithography (Figure 1d)]. A digital preview is a multi-use tool that can assist the restorative team throughout treatment, improving the dental team’s understanding of the esthetic issues and increasing patient acceptance of the final result [9]. In order to validate the function and esthetics, an acrylic mock-up is bonded to the teeth and left in place for one week. The mockup will help us to validate the aesthetic project on the aesthetic, functional and psychological levels. The mockup will help us to validate the aesthetic project on the aesthetic, functional and psychological levels. This last point is fundamental because it allows the patient to try and to decide. The patient then participates fully in the decision-making process.
Realization of composites
First, we have to choose the shade [10], before the dam step. The dentin shade is selected in the cervical region. Here, the enamel is thinned or even absent. Then, the enamel shade is selected at the incisal edge. (Figure 2a).

The superposition of these samples allows us to verify the choice is correct.
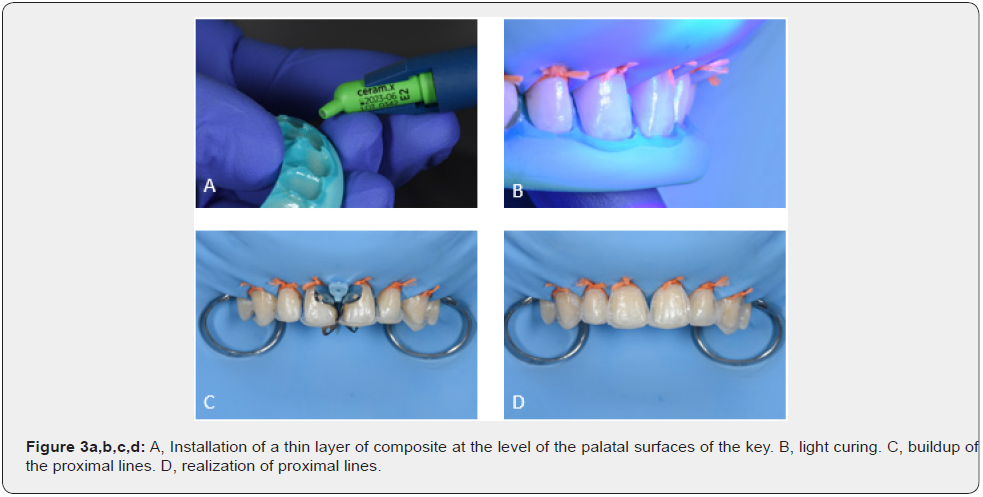
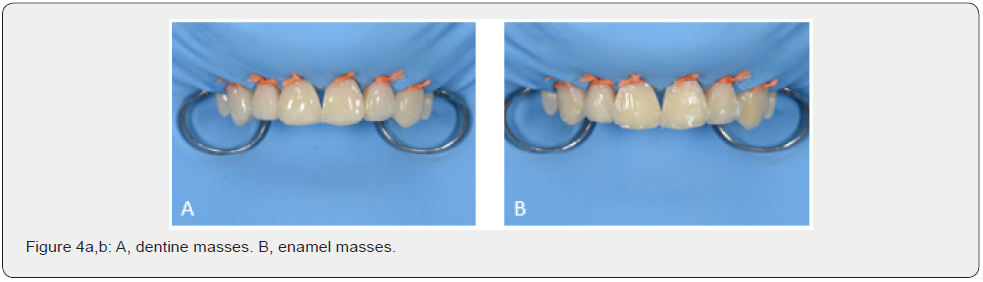
The enamel surfaces are left unprepared, sandblasted with small-grit alumina oxide (Figure 2b), and etched [11]. with DeTrey® Conditioner 36 for 30 seconds (Figure 2c). The enamel surfaces are rinsed profusely, and air-dried. A universal adhesive (Prime Bond active™) is applied for 20 seconds, dried and lightcured (Figure 2d). The palatal walls are built with enamel-shaded composite (ceram.x® duo E2) with the help of a silicone index (Figure 3a,b). A Palodent® V3 Sectional Matrix System is then used to build the proximal surfaces (Figure 3c,d). The layering of the vestibular surfaces is done with a D1-shaded composite for the dentinal core (Figure 4a), and the enamel mass is sculpted with E2-shaded composite (Figure 4b). Due to the high number of surfaces to restore, a particular attention is given to the shape, symmetry and harmonic variations of each individual tooth. The
The excess removal and shape refinement are made with multiblade high-speed tungstene carbide burs (Figure 5a). Surfaces are then polished using Enhance® (Figure 5b) & Enhance® PoGo® Finishing Systems (Figure 5c) under irrigation. The Enhance® system is defined by its manufacturer as a 1-step finishing instrument. It comes in the form of discs, tips, cups, mini-discs, mini-points, and mini-cups, made of dimethacrylate urethane resin, polymerized with 40 μm aluminum oxide particles. They are connected to a plastic mandrel and intended for single use. The PoGo® system designed for final polishing, is in the same form, also in 1 step, but is impregnated with diamond particles with a particle size of 2 to 4 μm. Then, we finished the interporximal polishing with abrasive strip (Figure 5d).

Then a follow-up at 1 week, 3 months and then every 6 months was set up to control the integrity of restorations.
Conclusion and Discussion
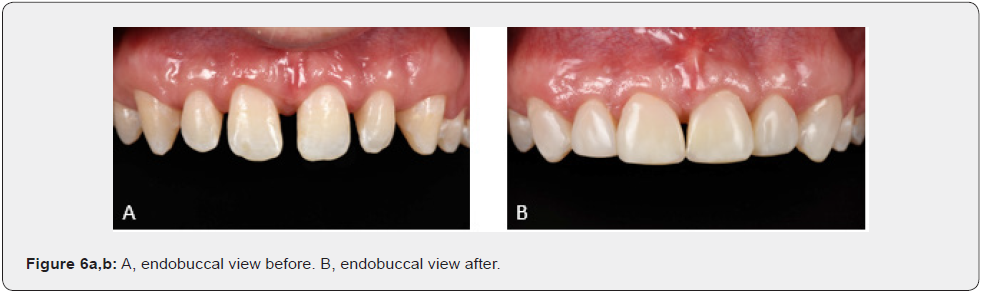
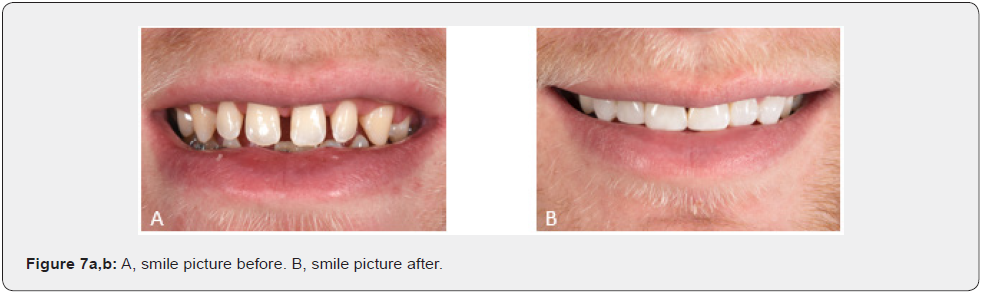
The clinical management of patients with rare diseases affecting the shape of the permanent dentition is a real challenge. The phenotypic peculiarities are unfavorable elements to overcome with minimally invasive restorations. Nevertheless,the functional, aesthetic, and biological requirements remain the same. In this case, a direct technique allowed us to restore the patient smile, although this demanding technique requires clinical time and a good patient cooperation. Since the patient is young and the orthodontic treatment is still ongoing, these restorations give us the frame to facilitate future refinements, if required. Moreover, the patient is satisfied with his new smile (Figure 6a,b) & (Figure 7a,b].
References
- Polder BJ, Van’t Hof MA, Van der Linden FPGM, Kuijpers-Jagtman AM (2004) A meta-analysis of the prevalence of dental agenesis of permanent teeth. Community Dent Oral Epidemiol 32(3): 217-226.
- Fournier BP, Bruneau MH, Toupenay S, Kerner S, Berdal A, et al. (2018). Patterns of Dental Agenesis Highlight the Nature of the Causative Mutated Genes. J Dent Res 97(12): 1306-1316.
- Dure-Molla M, Fournier BP, Manzanares MC, Ana Carolina Acevedo, Raoul C Hennekam, et al. (2019) Elements of morphology: Standard terminology for the teeth and classifying genetic dental disorders. American Journal of Medical Genetics Part A 179(10): 1913-1981.
- Haute Autorité de Santé (HAS) (novembre 2021): Protocole national de diagnostic et de soins (PNDS) : agénésies dentaires multiples : oligodontie et anodontie, synthèse à destination du chirurgien dentiste et du médecin traitant.
- Toupenay S, Fournier BP, Manière MC, Ifi-Naulin C, Berdal A, at al. (2018) Amelogenesis imperfecta: therapeutic strategy from primary to permanent dentition across case reports. BMC Oral Health 18(1): 108.
- Pontons-Melo JC, Furuse AY, Mondelli J (2011) A direct composite resin stratification technique for restoration of the smile. Quintessence Int 42(3): 205-211.
- Ahmed KE, Murbay S (2016) Survival rates of anterior composites in managing tooth wear: systematic review. J Oral Rehabil 43(2): 145-153.
- Dietschi D (1995) Free-hand composite resin restorations: a key to anterior aesthetics. Pract Periodontics Aesthet Dent 7(7): 15-25.
- Coachman C, Calamita M (2012) Digital Smile Design: A Tool for Treatment Planning and Communication in Esthetic Dentistry.
- Baratieri LN, Araujo E, Monteiro S (2007) Color in natural teeth and direct resin composite restorations: essential aspects. Eur J Esthet Dent 2(2): 172-186.
- Buonocore MG (1955) A simple method of increasing the adhesion of acrylic filling materials to enamel surfaces. J Dent Res 34(6): 849-853.
- Dietschi D (1997) Free-Hand Bonding in the Esthetic Treatment of Anterior Teeth: Creating the Illusion. J Esthet Restor Dent 9(4): 156-164.






























