Impact of Human Papilloma Virus (HPV) Status on Well Established Risk Profile of Oral Cancer in Sri Lanka
Manosha Lakmali Perera1,2 and Irosha Rukmali Perera3*
1School of Dentistry and Oral Health, Griffith University, Australia
2Menzies Health Institute Queensland, Griffith University, Australia
3Preventive Oral Health Unit, The National Dental Hospital (Teaching), Sri Lanka
Submission: April 06, 2021; Published: April 15, 2021
*Corresponding author: Irosha Rukmali Perera, Preventive Oral Health Unit, The National Dental Hospital, Teaching, Colombo, Sri Lanka
How to cite this article: Manosha Lakmali P, Irosha Rukmali P. Impact of Human Papilloma Virus (HPV) Status on Well Established Risk Profile of Oral Cancer in Sri Lanka. Adv Dent & Oral Health. 2021; 14(1): 555880. DOI: 10.19080/ADOH.2021.14.555880
Abstract
Background: There is a calamitous need to explore the impact of HPV on well-established risk profile of oral cancer which is poorly understood. Aim: Prioritizing this situation, we aimed to investigate the impact of HPV on well-established risk profile of oral cancer in Sri Lanka, using a representative sub sample consisted of 29 oral squamous cell carcinoma cases(OSCC) and 25 fibro epithelial polyps (FEP), from a large case control study conducted in Sri Lanka.
Methodology: Incisional biopsies of cases and excisional biopsies of controls were collected, transported, stored at =800C and dispatched as frozen tissues. DNA was extracted from frozen specimens, using the Gentra Puregene Tissue kit (Qiagen, Germany), solid tissue protocol according to the manufacturer’s instructions. Nested PCR was performed to detect HPV and HPV geno types were discovered by sequencing. Results: HPV was detected in 4/54 (7.4 %) of overall samples. Upon sequencing, high risk HPV α9 and HPV 31 were detected in controls and not in the HPV positive OSCC case. between cases and controls*. Moreover, statistically significant difference was obtained in mean ages of cases and controls. (p= 0.0001)*. Cases were older than controls. Conclusion: There was no impact of HPV on established risk profile of oral cancer in Sri Lanka. This high light the emerging importance of investigating the HPV status of young OSCC cases without known aetiology.Keywords: Aetiology; Agencourt bioscience; Heterogeneity; Human keratinocytes
Abbreviations: OSCC: Oral Squamous Cell Carcinoma Cases; FEP: Fibro Epithelial Polyps; OMF: Oro-Maxillo Facial; HNSCC: Head and Neck Squamous Cell Carcinoma
Introduction
In the global scenario, there are 13 other main cancer types, thus oral cancer dominated by oral squamous cell carcinoma (OSCC) ranking 14th [1]. Conspicuously, Indian subcontinent, especially Sri Lanka, India, Bangladesh and Pakistan alone accounts for one- third [2] of the global burden and oral cancer represents the commonest cancer type among men in Sri Lanka, ranking 1st [3]. Unfortunately, 3-4 people die every day due to one of the most preventable diseases [3]. This non communicable disease is multifactorial with an array of population and geographic specific risk factors [4]. Risk can be easily minimized by habit intervention, as known carcinogens are acquired or transmitted by life-style related-risk habits [4]. Older males indulging in betel quid chewing, alcohol consumption and smoking make the main risk profile of Sri Lankan oral cancer patients [4]. The global prevalence of HPV in OSCC, ranged from 0% to 85% [4-6], varying by geographic/population specificity as well as anatomical site, gender, age and method of detection but more prevalent in younger males without known aetiology [6,7]. In humans, plethora of HPV genotypes have been identified, exceeding 80 and some of them are categorized as ‘high risk’ due to their carcinogenic potential to cause genital cancers [6,7]. Among high risk types: HPV 18 and HPV 16 gained much attention of the scientific community as the aetiological agent of cervical cancer and a subset of head and neck squamous cell carcinoma (HNSCC).
The HPV prevalence in Sri Lankan OSCC patients ranged from 30.0 % to 39.4% without consensus among studies [7-9]. The oral carcinogenesis process caused by HPV defines a different entity, that is caused by well-established risk factors [10], however the exact events of integration of HPV DNA into the genome of the human keratinocyte needed to be fully understood [6]. At the moment, a lot to go to experience the influence of HPV in the wellestablished risk profile of oral cancer, not only in global context [11], or regional context [16] but also in Sri Lankan context [7,9]. Thus, the objective of this study was to investigate the impact of HPV status on well-established risk profile of oral cancer in Sri Lanka.
Materials and Methods
A sub sample representing the vast majority of OSCC cases, to detect the HPV status was selected from a large case control field study conducted in nine Oro-Maxillo Facial (OMF units), representing six provinces in Sri Lanka, while adhering to stringent exclusion and inclusion criteria. Study design, setting, subjects, data collection using pretested interviewer administered questioner, were described in detail previously [4,12]. Sample collection by incisional biopsies for Oral Squamous Cell Carcinoma (OSCC) cases and excisional biopsies of clinically diagnosed fibro epithelial polyps (FEP) controls, sample preservation as frozen biopsies, transport, storage in Sri Lanka, dispatch from Sri Lanka to Australia and storage at = 800C in the Griffith University, Australia were performed from April 2015 to August 2015 as described in detail previously [4,12]. The study cohort consisted of 29 Sinhala males with histologically confirmed OSCC cases involving the buccal mucosa or tongue (cases) and 25 Sinhala males with FEP from the same anatomic sites (controls). Ethical approval for this study was obtained from the University of Peradeniya (FRC/FDS/ UOP/E/2014/32) and the Griffith University Human Research Ethics Committee, Australia (DOH/18/14/HREC). Written consent was obtained from each participant.
DNA extraction, processing and quality assessment, amplification of target DNA, identification of amplimers and HPV type determination
Extraction of DNA: Deep tissue samples (~100 mg each) were dissected from frozen incisional biopsies of OSCC cases and excisional biopsies of FEP controls, preventing contamination from the tumor surface as much as possible [4,13]. DNA extraction was performed using Gentra Puregene Tissue kit (Qiagen, Germany) according to the manufacturer’s instructions (solid tissue protocol) [Cat no. 158689]as described previously [4].
Processing of target DNA for amplification by PCR: This was done by well-established Nested MY/GP+PCR. This PCR consisted of twosteps as two different pairs of degenerated oligonucleotide consensus primers MY09/MY11 and GP+/GP6+ were used for L1 region [14]. Firstly, (MY+) PCR was conducted using MY 09+ and MY 11+ primers. Details of master mix preparation and setting up of PCR assay were described previously [4]. Secondly, Nested (GP+) PCR was performed using the products of former PCR (MY+} PCR. Technical information related to master mix preparation and setting up of PCR assay was provided previously [4].
Quality assessment of target DNA by an indicator DNA: This was done to assess the quality of HPV DNA in samples by confirming the absence of PCR inhibiting agents and sheered or fragmented DNA. These might prevent the smooth amplification process if present. Hence, it is assumed that the presence of β-globin PCR products or specific bands in 2% agarose gel would indicate the quality of DNA extraction, amplification, separation, visualization procedures to obtain accurate and précised results on presence or absence of HPV DNA, in samples subjected to nested PCR, one of the conventional PCR techniques. Processing of extracted DNA, for amplification of β-globin gene by PCO3 and PCO4 [15] consensus primers, was described previously [4].
Amplification of processed target DNA and indicator DNA by PCR: This was done using Eppendorf Master- cycler Gradient PCR machine. Each PCR thermos cycler programme consisted of initial denaturation followed by 40 cycles. Each cycle consisted of denaturation (at 940C), primer annealing (occurs at 50–58°C, depending on the type of specific primers), elongation/extension (at 720C) and final elongation (at 720C).
a) (MY+) PCR: Using Eppendorf Master- cycler Gradient PCR machine as described previously [4].
b) (GP+) PCR: Using Eppendorf Master- cycler Gradient PCR machine as described previously [4].
c) PCO PCR 110417: Using Eppendorf Master- cycler Gradient PCR machine as described previously [4].
Identification of amplimers (PCR products) by gel electrophoresis: Separation of PCR products was done by gel electrophoresis (1.5% agarose gel containing ethidium bromide; SeaKem, FMC bioproducts and Sigma), visualization of separated bands was done under UV light and identification of HPV positive bands were identified using the suitable DNA ladder as described previously [4].
HPV type determination: HPV- positive PCR products were subjected to purification with the Agencourt AMpure PCR purification kit (Agencourt Bioscience) in a magnetic 96 ring SPRI plate and the thermal protocol as described previously [15]. After purifying the HPV- positive PCR product. Further purification was done to facilitate the sequencing by the Agencourt CleanSEQ dye-terminator removal kit (Agencourt Bioscience). in a magnetic
96-ring SPRIplate. Subsequently, purified sequences in reaction mixtures were analysed with an automated DNA sequencing machine (ABI model 3100). The DNA sequences obtained were compared with available reference sequences in GenBank through the BLAST server as described previously [15].
Statistical analysis: Descriptive statistics, t-test was used to compare means of independent samples. Fisher’s Exact test was used to find out statistical significance among two groups on risk habits: betel quid chewing, smoking and alcohol consumption.
Results
The tables and bar charts summarize the socio-demographic and laboratory data on HPV status.
Distribution of OSCC cases and FEP controls by mean age and well-established risk profile of OSCC
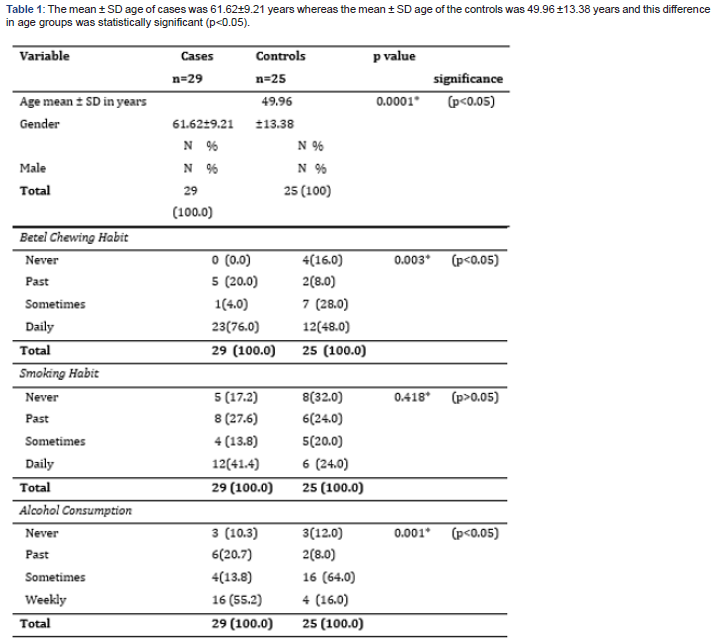
According to Table 1, the mean ± SD age of cases was 61.62±9.21 years whereas the mean ± SD age of the controls was 49.96 ±13.38 years and this difference in age groups was statistically significant (p<0.05).
The distribution of Cases and Controls by HPV Status (Table 2)
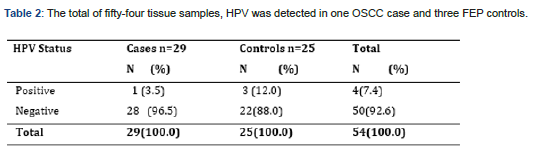

As said by Table 3, of the total of fifty-four tissue samples, HPV was detected in one OSCC case and three FEP controls.
Pie chart representation of HPV status in overall samples
In accordance with 3.3 pie chart of fifty-four subjects, only four subjects were detected with HPV (Figure 1).

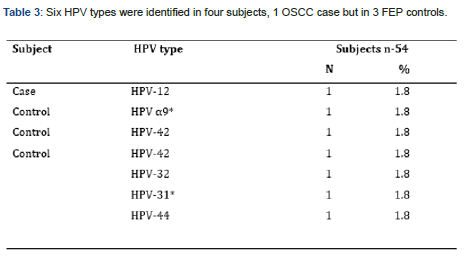
HPV types associated with subjects of oral cancer in Sri Lanka (Table 3)
As per Table 3, six HPV types were identified in four subjects, 1 OSCC case but in 3 FEP controls.
Discussion
To the authors’ knowledge this is one of the three publishable studies conducted to assess the impact of HPV status [7-9] on well-established risk profile of oral cancer in Sri Lanka. In the present study, the overall prevalence of HPV was 7%. In contrast, Sri Lankan oral cancer related HPV prevalence was reported as 37.2%, 30.0 % and 39.4% by Jayasooriya et al. [7]; Jalouli et al. [8] & Gunasekera et al. [10] respectively. This variation may be due to the heterogeneity in anatomical site, gender, mean age, sample size, type of specimen as well as inherent limitations in methodologies [7-9]. The subjects of the present study consisted of OSCC cases of older males indulging life-style related risk habits of betel chewing, smoking and alcohol consumption. On the contrary, younger males, yet indulging in risk habits to a lesser extent, compared to their oral cancer counterpart included in the FEP control group. Hence, there was a statistically significant difference on betel quid chewing (p = 0.003) and heavy alcohol consumption (p = 0.001) among two groups. In the present study, only one OSCC case was infected with HPV. Thus, it was not possible to find out significant association of HPV with wellestablished risk profile of oral cancer in Sri Lanka.
This finding is lined up with previous findings: inability of obtaining, significant association of HPV with well-known risk profile of oral cancer: tobacco use [16], addiction to smokeless tobacco preparations such as (shammah/moist snuff) and khat (Catha edulis) [11] betel quid chewing [7,9], heavy alcohol consumption [7,9] and smoking [7,9], in epidemiological studies conducted in India [16], Yamen [11]and Sri Lanka [7,9]. respectively. These findings confirm, the higher prevalence of HPV in oropharyngeal cancers than the oral cavity cancers [6]. Furthermore, OSCC cases infected with HPV were more frequently found among nonsmokers, nondrinkers and those with high risk oral sexual behaviours [17-22]. Obviously, tonsils and oro pharynx were encountered as the most affected anatomical sub sites than buccal mucosa and tongue. These findings corroborate the insignificant prevalence of HPV in OSCC cases comprising buccal mucosa (65.5%) and tongue (34.5%) sites of the present study. Contradictory to these findings, both synergistic [23] and additional [24] effects of HPV with the well-established risk profile were noted but poorly understood [6] in previous epidemiological studies.
Interestingly,15 out of 100 geno types of HPV considered as ‘high risk’ due to their oncogenic possibility to cause cervical and anogenital cancers [25,26]. Thus, geno typing of HPV is of utmost importance to identify the high-risk types rather stating the presence or absence of HPV-DNA in OSCC cases. Upon sequencing high risk HPV species α-9 [26] was identified in one control and high-risk type 31 [27] was identified in another control. Both got used to substance abuse betel quid and alcohol for more than a decade. Previously, Jayasooriya et al. [7] were able to identify HPV 16 in Sri Lankan OSCC cases. Besides, Gunasekera et al. [9] reported HPV 16 seropositivity in Sri Lankan OSCC patients. It has been suggested that the higher prevalence of high-risk HPV types, exclusively HPV 16, might be a contributing factor for oral carcinogenesis, mainly in younger individuals without known aetiology [7,9]. Undoubtedly, HPV 18 and HPV 16, established as causative agents of at least 70% of cancers of the uterine cervix [28] and significantly associated with oro-pharyngeal cancers [6].
Unanimously, HPV 16 is being considered as the commonest HPV type, overall 90% detected in head and neck cancers (HNSCCs) in the Asia Pacific region, not only in 75-95% of oropharyngeal cancers also in 50-68% of oral cavity cancers [6]. HPV species α-9, was found in one FEP control is known to made up of seven geno types, including well known HPV 16 [26]. Furthermore, HPV 31 was reported to be associated with cervical cancer [29] was found in another control. In the present study the difference of mean age between OSCC cases and FEP controls was statistically significant (p= 0.0001). Thus, the two controls infected with high risk HPV, but none of the case, support the notion, “the HPV association is higher in younger OSCC male patients than the elderly OSCC male patients without known aetiology” [4]. Last but not least, the presence, of HPV 12, which is a skin commensal in one and only OSCC case, concludes the findings of the present study, after stating the limitations.
Small sample size is a limitation of the present study. Thus, cohort studies with large sample sizes and rigorous methodology for controlling for confounders are much in need to investigate the emerging role of HPV in increased risk of OSCC in patients with known risk habit to establish any association or correlation. Moreover, dispatch of tissue samples from Colombo to Gold Coast as frozen could be considered as another unavoidable limitation, especially in maintaining the cold chain throughout to avoid the degradation of HPV- DNA. Besides, it is not known about the sexual practices of those two groups, which was beyond the scope of this study due to the fact that Sri Lanka is a conservative country with strong cultural values. Inquiring such information from patients is strictly prohibited and this can be considered as another obvious limitation of this study.
Conclusion
There was no impact or influence of HPV on established risk profile of OSCC in Sri Lanka, as per with present study conducted using histologically confirmed 29 OSCC cases and clinically diagnosed 25 FEP controls. It is essential to conduct studies with large sample size, clear sub site classification, age, gender and risk habits to minimize the in-consensus findings. Best affordable technique is needed to use after considering the inherent limitations of all available techniques for detection as well as genotyping of HPV, to maintain the accuracy and reproducibility of HPV laboratory data. This study states the emerging role of oncogenic HPV in oral carcinogenesis with special reference to high-risk groups with lifestyle related modifiable risk habits which might facilitate the transmission of HPV from one individual to another. Furthermore, investigation of oncogenic potential of high-risk HPV types (other than HPV 18 and HPV 16) using in vitro experiments, probably with OSCC cancer cell lines (BHY, HSC-3 and HN) and in vivo experiments with suitable animal models are recommended to widen the horrizons of existing knowledge on carcinogenic mechanisms of high risk HPV on human keratinocytes.
References
- Ferlay J, Soerjomataram I, Ervik M, Dikshit R, Eser S, et al. (2013) Globocan 2012, cancer incidence and mortality worldwide: IARC cancer base no. 11. Lyon (France): International Agency for Research on Cancer 10.
- Gupta B, Ariyawardana, Johnson NW (2013) Oral cancer in India continues in epidemic proportions: evidence base and policy initiatives. International dental journal 63(1): 12-25.
- (2014) Sri Lanka National Cancer Control Program, Cancer incidence data Sri Lanka 2014, Government Cancer Institute, Ministry of Health, Sri Lanka.
- Perera ML (2017) The Microbiome Profile of Oral Squamous Cell Carcinoma Tissues in a group of Sri Lankan Male Patients, Griffith University, Queensland, Australia.
- Fakhry C, Westra WH, Li S, Anthony Cmelak, John A Ridge, et al. (2008) Improved survival of patients with human papillomavirus-positive head and neck squamous cell carcinoma in a prospective clinical trial. J Natl Cancer Inst 100(4): 261-269.
- Shaikh MH, McMillan NAJ, Johnson NW (2015) HPV-associated head and neck cancers in the Asia Pacific: a critical literature review & meta-analysis. Cancer epidemiol 39(6): 923-938.
- Jayasooriya PR, Kurose K, Teraj M, Sivaganan K, Siriwardane S, et al. (2003) Human Papillomavirus in Oral Cancer from Sri Lanka: Prevalence and relationship with clinico-pathological parameters. Oral Medicine & Pathology 8(2): 45-50.
- Jalouli J, Jalouli MM, Sapkota D, Ibrahim SO, Larsson PA, et al. (2012) Human papilloma virus, herpes simplex virus and epstein barr virus in oral squamous cell carcinoma from eight different countries. Anticancer research 32(2): 571-580.
- Gunasekera SK, Perera KA, Fernando C, Udagama PV (2015) A shifting paradigm in the aetiology of oral and pharyngeal cancer in Sri Lanka: a case-control study providing serologic evidence for the role of oncogenic HPV types 16 and 18. Infectious agents and cancer 10(1): 1-9.
- Fakhry C, Westra WH, Li S, Cmelak A, Ridge JA, et al. (2008) Improved survival of patients with human papillomavirus-positive head and neck squamous cell carcinoma in a prospective clinical trial. J Natl Cancer Inst 100(4): 261-269.
- Nasher AT, Al-hebshi NN, Almoayad EE, Suleiman AM (2014) Viral infection and oral habits as risk factors for oral squamous cell carcinoma in Yemen: a case-control study. Oral surgery, oral medicine, oral pathology and oral radiology 118(5): 566-572.e1.
- Perera M, Al-hebshi NN, Perera I, Ipe D, Ulett GC, et al. (2017) A dysbiotic mycobiome dominated by Candida albicans is identified within oral squamous-cell carcinomas. J oral microbiol 9(1): 1385369.
- Perera M, Al-hebshi NN, Perera I, Ipe D, Ulet GC, et al. (2018) Inflammatory bacteriome and oral squamous cell carcinoma. J dent res 97(6): 725-732.
- Venceslau EM, Bezerra MM, Lopes ACM, Souza EV, Onofre ASC, et al. (2014) HPV detection using primers MY09/MY11 and GP5+/GP6+ in patients with cytologic and/or colposcopic changes. Jornal brasileiro de patologia e medicina laboratorial 50(4): 280-285.
- Antonsson A, Nancarrow DJ, Brown IS, Green AC, Drew PA, et al. (2010) High-risk human papillomavirus in esophageal squamous cell carcinoma. Cancer Epidemiology and Prevention Biomarkers 19(8): 2080-2087.
- Murthy V, Swain M, Teni T, Pawar S, Kalkar P, et al. (2016) Human papillomavirus/p16 positive head and neck cancer in India: Prevalence, clinical impact, and influence of tobacco use. Indian journal of cancer 53(3): 387-393.
- Gillison ML, D’Souza G, Westra W, Sugar E, Xiao W, et al. (2008) Distinct risk factor profiles for human papillomavirus type 16-positive and human papillomavirus type 16-negative head and neck cancers. J Natl Cancer Inst 100(6): 407-20.
- D’Souza G, Agrawal Y, Halpern J, Bodison S, Gillison ML (2009) Oral sexual behaviors associated with prevalent oral human papilloma virus infection. J Infect Dis 199(9): 1263-1239.
- Schiffman M, Rodriguez AC, Chen Z, Wacholder S, Herrero R, et al. (2010) Apopulation-based prospective study of carcinogenic human papillomavirus variant lineages, viral persistence, and cervical neoplasia. Cancer research 70(8): 3159-3169.
- Arteaga CL, Adamson PC, Engelman JA, Foti M, Gaynor RB, et al. (2014) AACR cancer progress report 2014. Clinical Cancer Research 20(19Supplement): S1-S112.
- Ryerson AB, Peters ES, Coughlin SS, Chen VW, Gillison ML, et al, (2008) Burden of potentially human papillomavirus-associated cancers of the oropharynx and oral cavity in the US, 1998–2003, Cancer 113(Suppl 10): 2901-2909.
- Maden C, Beckmann AM, Thomas DB, McKnight B, Sherman KJ, et al. (1992) Human papillomaviruses, herpes simplex viruses, and the risk of oral cancer in men. American journal of epidemiology 135(10): 1093-1102.
- Herrero R, Castelsague X, Pawlita M (2000) Human papilloma virus and oral cancer: The international agency for research on cancer multicentre study. J Natl Cancer Inst 92: 709-720.
- Jamaly S, Khanehkenari MR, Rao R, Patil G, Thakur S, et al. (2012) Relationship between p53 overexpression, human papillomavirus infection, and lifestyle in Indian patients with head and neck cancers. Tumour Biol 33(2): 543-550.
- Muñoz N, Bosch FX, Sanjose SD, Herrero R, Castellsague X, et al. (2003) Epidemiologic classification of human papillomavirus types associated with cervical cancer. New England Journal of Medicine 348(6): 518-527.
- Schiffman M, Rodriguez AC, Chen Z, Wacholder S, Herrero R, et al. (2010) A population-based prospective study of carcinogenic human papillomavirus variant lineages viral persistence, and cervical neoplasia. Cancer research 70(8): 3159-3169.
- Zur Hausen H (2002) Papillomaviruses and cancer: from basic studies to clinical application. Nature Reviews Cancer 2(5): 342-350.
- Elasbali AM, Hussein ARA, Gadelkarim AH (2012) Cervical and oral screening for HR-HPV types 16 and 18 among Sudanese women cervical lesions. Infectious agents and cancer 7(1): 17.
- Forslund O, Antonsson A, Nordin P, Stenquist B, Hansson BG (1999) A broad range of human papillomavirus types detected with a general PCR method suitable for analysis of cutaneous tumours and normal skin. Journal of General Virology 80(9): 2437-2443.






























