Gelatamp: A New Promising Hemostatic Agent
Babitha GA1, Shiva Charan Yadav K1, Sunil Dutt Christopher2, Nirmala Singh2 and Shobha Prakash1
1Department of Periodontics, College of Dental Sciences, India
2Department of Oral Implantology, College of Dental Sciences, India
Submission: May 05, 2017; Published: December 15, 2017
*Corresponding author: Shiva Charan Yadav K, Post graduate student, Dept of Periodontics, College Of Dental Sciences, Davangere, Karnataka, India, Email: shivacharan08@gmail.com
How to cite this article: Babitha GA, Shiva C Y K, Sunil D C, Nirmala S, Shobha P. Gelatamp: A New Promising Hemostatic Agent. Adv Dent & Oral Health: 2017; 7(1): 555707.DOI: 10.19080/ADOH.2017.07.555707
Abstract
Dentists perform a variety of surgical procedures frequently requiring the need for a hemostatic agent. Hemorrhage is a leading cause of preventable morbidity and mortality in and out of the operating room. Surgical bleeding can have a significant impact on both patient outcomes and health care costs. Of the importance of bleeding-related complications has resulted in an explosive use of topical hemostatic adjuncts throughout the health care environment.
Unlike other circumstances in which there are a plethora of evidence-based recommendations and guidelines, the use of topical hemostatic agents in the operating room principally reflects local practice and physician preference. This article is a review on a new hemostatic agent with the good potential for application in the oral cavity.
Keywords: Bite block; Cementation
Introduction
Dentists perform a variety of surgical procedures frequently requiring the need for a hemostatic agent. Hemorrhage is a leading cause of preventable morbidity and mortality in and out of the operating room. Surgical bleeding can have a significant impact on both patient outcomes and health care costs. Poor hemorrhage control is strongly linked with untoward outcomes and drives clinicians to use treatment methods that may further lead to increased morbidity and mortality [1,2].
At least 3 factors have an impact on bleeding-related complications: progressively widespread use of anticoagulant and antiplatelet therapeutics; technologic advances that enable complex and lengthy surgical procedures; and the advancing age of the general population, with associated comorbidities that predispose to bleeding-related complications. Recognition of the importance of bleeding-related complications has resulted in an explosive use of topical hemostatic adjuncts throughout the health care environment. Available preparations of topical hemostatic adjuncts include a host of formulations and significant differences between products. Products vary with regard to efficacy, reproducibility of action, and safety. As a result, a bewildering array of products confronts clinicians faced with hemorrhage in and out of the operating room. Unlike other circumstances in which there are a plethora of evidence-based recommendations and guidelines, the use of topical hemostatic agents in the operating room principally reflects local practice and physician preference. Moreover, the true scope of practice is likely unclear because topical hemostats may be stocked in multiple locations including the operating room, central supply, pharmacy, or the blood bank depending on local practice and product type. Therefore, obtaining a reliable evaluation of current practice to glean data from which to make evidence-based recommendations is a significant challenge.
Properties of the ideal topical hemostatic agent
Although the precise properties of the ideal topical hemostatic agent will vary according to surgical specialty as a result of the varying requirements, some features are universally valued, including:
1. Rapid and effective in control/cessation of bleeding;
2. Ability to make effective contact with the bleeding surface;
3. An acceptable adverse event profile;
4. Reliable and easy to handle;
5. Simple to prepare;
6. Available in multiple, versatile delivery options appropriate for different types of bleeding; and
7. Active and compatible with the patients' own physiology [3].
Gelatin foams date back to 1945 when they were introduced as hemostatic agents by Correll and Wise. Gelatin foam is manufactured from animal skin gelatin whipped and baked into its sponge form. It provides a physical matrix for clotting to be initiated and is available as Gelfilm and Gelfoam from Pharmacia and Upjohn Company (a subsidiary of Pharmacia Corporation, Pfizer). It can be applied as a film, sponge, or powder. Gelfoam (Pharmacia) is one of the more commonly employed agents for the control of minor bleeding. It is a porous, pliable sponge made from dried and sterilized porcine skin gelatin. This sponge holds many times its weight in blood and provides a stable scaffold for clot formation, thus, the mode of action of the Gelfoam is believed to be related to the formation of a mechanical matrix that facilitates clotting. Gelfoam is thought to act intrinsically by promoting the disintegration of platelets causing a subsequent release of thromboplastin, this is, in turn, stimulates the formation of thrombin in the interstices of the sponge. It may be soaked in thrombin or epinephrine solution to enhance its hemostatic properties. It is important to note that Gelfoam swells more than collagen or cellulose products and can double its volume. Although this provides a good mechanical hemostatic action, it can cause compressive complications, especially when used near nerves or in confined spaces. The surgeon may take advantage of this characteristic with penetrating trauma. Gelatin foam is absorbed within 4 to 6 weeks and is largely non-antigenic, although it is derived from animal products. Unlike oxidized cellulose, the pH of gelatin foams is neutral and therefore can be used in conjunction with thrombin or another pH neutral Biologics to enhance the hemostatic action [4].
Gelatamp (gelatine sponge with colloidal silver); is similar to Gelfoam which is absorbable gelatin sponge available as a sterile sponge-like dressing. Gelatamp colloidal silver gelatin sponge is the hemostatic and antibacterial which has the dual advantage. It stabilizes the blood clots, promotes coagulation and hemostasis. Gelatin sponge porous foam structure so that it can absorb many times more than the blood of weight (about 55-75 times its own weight, but not volume expansion). The huge surface area can promote platelet aggregation while packing the wound, forming a solid clot embolism fixed, prevent blood clots that may arise due to contraction of the secondary cracks, or due to bacterial infection caused by contaminated saliva.
Silver element is an inert element, in a wet environment can be free of traces of silver ions, which play a long-lasting bactericidal effect from ancient to modern times. Hippocrates, the "father of medicine”, wrote that silver had beneficial healing and antidisease properties. Silver also has proven antimicrobial activity that includes antibiotic-resistant bacteria. It has a broad spectrum of antimicrobial activity, with minimal toxicity toward mammalian cells at low concentrations, and has a less likely tendency than antibiotics to induce resistance due to its activity at multiple bacterial target sites [5].
Silver is promoted within alternative medicine in the form of colloidal silver, though it has never been proven safe and effective. The silver ion (Ag+) is bioactive and in sufficient concentration readily kills bacteria in vitro. Silver also kills bacteria in external wounds in living tissue and therefore physicians use wound dressings containing silver sulfadiazine (Ag-SD) or silver nanomaterials to treat external infections [6,7].
Wound dressings containing silver are increasing in importance due to the increase of antibiotic-resistant bacteria, which has imposed clinical limits on the use of antibiotics. Chopra states that topical silver is regaining popularity in the management of open wounds, "due largely to the spread of methicillin-resistant Staphylococcus aureus and the resultant reduction in the first-line antibiotic prescribing”. He does, however, conclude that "Some silver-based dressings appear to provide an effective alternative to antibiotics in the management of wound infection [7]. William suggested that addition of an antibacterial medium to the gelatin sponge is essential. He found that topical antimicrobial agents can significantly reduce the incidence of dry socket [8]. Gelatamp is made of 95% foam gelatin sponge and 5% finely dispersed colloidal silver. The small quantities of these ions are antimicrobial without developing resistance. Gelatamp is effective against wide range of micro-organisms which are found in the oral cavity. It has been found to be very effective against bacteria which are resistant to antibiotics. The finely dispersed colloidal silver provides a large active surface for the continuous release of silver ions. As silver does not dissolve easily it is not washed out of the gelatin sponge but is continually released as the sponge is resorbed. This gives Gelatamp a depot antimicrobial effect throughout the resorption process.
The particular property of colloidal silver-its long-lasting depot effect the finely dispersed colloidal silver provides a large, active surface for the continuous release of silver ions (Figure 1,2). As silver does not dissolve easily it is not washed out of the gelatine sponge but is continually released as the sponge is resorbed. This gives Gelatamp a depot effect-the product has an antimicrobial effect throughout the resorption process. Further medications are not required therefore treatment with Gelatamp is time-saving and very compatible with the patient [8].

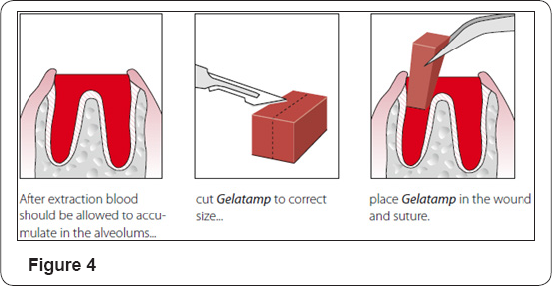
Gelatamp is effective against wide range of microrganisms, which are found in the oral cavity. It has been found to be very effective against bacteria, which are resistant to antibiotics. The finely dispersed colloidal silver provides a large active surface for the continuous release of silver ions. As silver does not dissolve easily it is not washed out of the gelatin sponge but is continually released as the sponge is resorbed (Figure 3,4). This gives Gelatamp a depot antimicrobial effect throughout the resorption process. Gelatamp has the great advantages of both hemostatic and bactericidal effect. It remains in the alveolus and completely resorbed within 4 weeks [9].


Composition [10]
One Gelatamp gelatine sponge (14 x 7 x 7 mm)
Contains:
Hardened gelatine Ph. Eur. 9.5 mg
Colloid silver Ph. Franc. 0.5 mg
Indications [10]
The treatment of alveoli and wound cavities,
E.g. after
1. Extractions
2. Apical amputations
3. Maxillary sinus perforations
4. Other surgical treatments (removal of tumors or retained teeth)
5. Prophylaxis of
6. Secondary cavity formation
7. Wound infections
8. Secondary hemorrhage prophylaxis
As well as a dressing after gingivectomy and in periodontopathic.
Contra-indications [10]
Infected, secretory and purulent wounds; hypersensitivity to silver or gelatin.
Instructions for use [10]
After opening the aluminum seal, Gelatamp is removed under aseptic conditions and is immediately ready for use. The size of the small sponge can be adjusted to fit the wound cavity if need be, without squeezing. Two Gelatamp plugs can be used for larger wounds.
The sponge is immediately placed dry and un squeezed in the fresh, blood-filled wound cavity and should be allowed to absorb as much blood as possible (visual inspection). The sponge must not protrude over the inner gingival margin so as not to adversely affect the desired epithelisation. This constitutes definitive treatment of the alveolus and there is no need for subsequent rinsing.
Sterility [10]
Gelatamp is supplied gamma-sterilized. The sterility of undamaged, unopened packs is guaranteed until the first application. Damaged packages should be discarded prior to use. Given the antimicrobial effect of this product, safe application is guaranteed until the product is used or up to the expiry date once the package had been opened, provided that Gelatamp is removed under aseptic conditions.
Side effects [10]
Recovery may be delayed if used incorrectly, especially in the case of contaminated alveolar spaces.
Interactions with other drugs [10]
Concomitant application of alveolar pastes, wound plugs or other inserts apart from thrombin preparations as a dry powder, and moistening with liquid substances or medication such as anion-active surfactants, antiseptics containing phenol, ethacridine lactate, dilute mineral acids and concentrated saline solutions can hinder wound recovery and should, therefore, be avoided. Please avoid contact with hydrogen peroxide as this will bleach the sponge.
Storage instructions [10]
Gelatamp possesses moisture-absorbing properties. The package must, therefore, be closed immediately after use and stored dry, protected from light. Keep all medicines out of the reach of children. Gelatamp has a shelf-life of 3 years. It can be used unopened and after opening up to the expiry date.
The product should no longer be used once the date on the packaging and label has elapsed. Unused sponges can easily be disposed of with laboratory waste whereas; the plastic container, lids and aluminum foil, etc. can be recycled.
Clinical studies using gelatamp
1. Yong et al. [10] has conducted a study to study the clinical effect of Gelatamp colloidal silver gelatin sponge on preventing the complication of teeth extraction and concluded that incidence rate of bleeding, infection, pain, swelling and dry socket after teeth extraction in experimental group was lower than those of control group, and the difference between them was statistically significant [10].
2. Wang et al. [11] conducted a study the clinical effect of "gelatamp” colloidal silver gelatin sponge on preventing dry socket after extracting the mandibular impacted teeth and concluded that that "gelatamp” colloidal silver gelatin sponge can prevent the occurrence of dry socket after teeth extraction, which is of wide clinical use [11].
3. Maani et al. [12] conducted a study to evaluate clinically the use of Gelatamp to avoid postoperative dry socket and bleeding in patients receiving anticoagulant therapy without altering the medication dosage and concluded that Gelatamp is an effective material as local hemostatic agent after extraction for anticoagulant patients (within the therapeutic range of INR) without interruption of their medicine [12].
Conclusion
Intraoperative bleeding can be life threatening in some cases; therefore, a fast and effective blood management plan incorporating topical hemostatic agents may be essential for achieving optimal patient outcomes. The use of topical hemostatic agents may improve blood conservation, avoid potential adverse events of systemic hemostatic medications, reduce overall procedure time, and contribute to faster patient recovery times. A Newer hemostatic agent like gelatamp has the great advantages of both hemostatic and bactericidal effect with promising results and further studies are needed .
References
- Rady MT, Ryan T, Starr NJ (1998) Perioperative determinants of morbidity and mortality in elderly patients undergoing cardiacsurgery. Crit Care Med 26(2): 225-235.
- Marietta M, Facchini L, Pedrazzi P, Busani S, Torelli G (2006) Pathophysiology of bleeding in surgery. Transplant Proc 38(3): 812814.
- Morikawa T (2001) Tissue sealing. Am J Surg 182(2 Suppl): 29S-35S.
- Achneck HE, Sileshi B, Jamiolkowski RM, Albala DM, Shapiro ML (2010) A Comprehensive Review of Topical Hemostatic Agents: Efficacy and Recommendations for use Ann Surg 251(2): 217-228.
- Grammaticos PC, Diamantis A (2008) Useful known and unknown views of the father of modern medicine, Hippocrates and his teacher Democritus. Hell J Nucl Med 11(1): 2-4.
- Qin Y (2005) Silver-containing alginate fibres and dressings. Int Wound J 2(2): 172-176.
- Hermans MH (2006) Silver-containing dressings and the need for evidence. Am J Nurs 106(12): 60-68.
- Chopra I (2007) The increasing use of silver-based products as antimicrobial agents: a useful development or a cause for concern? J Antimicrob Chemother 59(4): 587-590.
- Cai YH, Lu CS (2008) A clinical study of gelatamp colloidal silver gelatin sponge on preventing the complication of teeth extraction. 26(5): 519-521.
- http://www.dent.cz/navody/Colt%E9ne/Gelatamp.pdf.
- Wang YZ, Guan QL, Li YX, Guo JL, Jiang L et al. (2013) Use of "gelatamp” colloidal silver gelatin sponge to prevent dry socket after extracting mandibular impacted teeth. Shanghai Kou Qiang Yi Xue 22(1): 108110.
- Maani S, Saleh M, Melek L, Sadaka P(2015) Evaluation of colloidal silver gelatin sponge (gelatamp) in patients receiving anticoagulant after tooth extraction. Alexandria Dental Journal 40: 101-106.






























