Maternal Health-Seeking Behaviours in Preventing Preterm Delivery: A Case Control Study in Selangor
Rosnah Sutan*, Norsafinaz Mohamed and Azmi Mohd Tamil
Department of Community Health, Universiti Kebangsaan Malaysia Medical Centre, Malaysia
Submission: December 20, 2016; Published: March 27, 2017
*Corresponding author: Rosnah Sutan, Department of Community Health, Universiti Kebangsaan Malaysia Medical Centre, Jalan Yaakob Latif, Bandar Tun Razak, Cheras, 56000 Kuala Lumpur, Malaysia, Tel: +60193212256; Fax: +603-91456670; Email: rosnah_sutan@yahoo.com
How to cite this article: Sutan R, Norsafinaz M, Azmi M T. Maternal Health-Seeking Behaviours in Preventing Preterm Delivery: A Case Control Study in Selangor. J Gynecol Women's Health. 2017; 3(4): 555621. DOI: 10.19080/JGWH.2017.03.555621.
Abstract
Preterm delivery is a leading cause of new born death especially in the developing country. It is one of the perinatal outcome predictors of growth and survival of baby. The objective of this study is to identify the relationship between mother's health seeking behaviour during stages of pregnancy and preterm delivery. An unmatched case control study was conducted at 34 selected primary care centres (PHC) in Selangor from Mac to September 2013. Selection for case and control groups from PHC was done using multistage random sampling based on criteria set. All respondents were interviewed face-to-face by an interviewer. A validated structured interviewed questionnaire was used covering socio demographic, obstetric history, diet intake, stress handling and physical activity. A total of 424 samples were obtained. There were 212 of the postnatal mothers with preterm babies (cases) and 311 postnatal mothers with term babies (controls). This study found that the Indian mother (aOR=2.54, 95% CI 1.30-4.98), young aged less than 20 years (aOR=4.89, 95% CI 1.07-22.29), primigravida (aOR=1.84, 95% CI 1.212.78), unplanned pregnancy (aOR=1.74, 95% CI 1.14-2.66) and not taken folic acid during pre-pregnancy (aOR=2.21, 95% CI 1.01-4.84) was found have higher risk for preterm delivery. Promoting reproductive women to practice good health seeking behaviour by having regular folic acid intake pre pregnancy and family planning, need to be strengthening for further reduction of poor perinatal outcomes. Mothers need to educate on self-monitoring and regular follow up to ensure safe motherhood.
Keywords: Preterm delivery; Maternal health seeking behaviour; Pre pregnancy care
Introduction
Preterm birth is defined as the birth of a baby of less than 37 weeks gestation [1]. It is a major contributor (75%) to perinatal mortality and morbidity in the world, as well as the primary risk factor for neurological damage and disability [2]. The number of perinatal deaths is high and scientifically evidence showed that it was due to preterm birth complications caused by infection, asphyxia, hypothermia and hyper bilirubinemia [1]. Globally, an estimated 13 million babies are born premature every year, with a premature birth rate of 5-7% in developed countries and a premature birth rate of 9% in Asia [2]. The majority of premature incidences (85%) occurred in Africa and Asia and this contributed to almost 11 million premature births [3].
Maternal health behaviours vary with the different stages of pregnancy stages. It has an impact on pregnancy outcomes as direct and indirectly. Research has proven poor maternal health behaviours can cause low birth weight, premature birth, Sudden Infant Death Syndrome (SIDS), and an increased risk of spontaneous abortion [4]. Most researches were carried out using existing clinical data from patients' records in assessing the relationship between maternal health behaviours and pregnancy outcomes. Many factors related to maternal behaviour is unable to explore in depth using record data.
The main key challenges recorded in the Millennium Development Goals 2015 of Malaysia 15 years achievement review has recommended that the quality of care received by women before, during and after pregnancy is the important elements for better child health .this report has stated that the vast majority of child deaths in Malaysia occur in the first year of life. A series of annual report from Family Health Development Division of Malaysia has stated that between 1990 and 2007, neonatal mortality rates were halved to 3.8 per 1,000 live births but it increased slightly to 4.0 as of 2012. The leading causes of under-five deaths in Malaysia by the ICD-10 classification are conditions from perinatal period and mostly were due toimmaturity or prematurity (36.5 per cent) [5]. Between 2008 and 2012, about 60- 65 per cent of deaths due to prematurity had birth weights of less than 1000 grams. Between 54.5-63.7 per cent of these deaths occurred amongst the extreme preterm when the period of gestation was less than 28 weeks. In order to improve maternal health including perinatal health concerted effort to cover all reproductive health women screening is highlighted and it should be screen during pre-marital, pre-pregnancy care and all stages of pregnancy care This care needs to incorporate aspects such as reproductive health, family planning spacing and contraceptive use, healthy diet and physical activity, optimal psychological and psychosocial health [5].
The 11th Malaysia Plan and the transformative 2030 global development agenda have been planned to cover the Sustainable Development Goals to ensure that policies and programmes are sustainable, resilient and inclusive to build a foundation for improved quality of life for all in the country [5]. The important of awareness on health seeking behaviour for own health has been emphasised in that plan. The aim of present study is to identify the relationship between maternal health seeking behaviour at pre pregnancy and during pregnancy stage with preterm delivery including family planning practice, mother's intention on pregnancy, folic acid intake pre pregnancy, stress handling, and physical activity using face to face guided interviewed.
Materials and Methods
The methodology of present study has been described in an article published recently [6] using same dataset but with different sub-analysis according to outcome variable studied. In summary, this study was conducted in Selangor which is located at the centre of west coast of Peninsular Malaysia. Based on 2010 census, the state had a total population of 5.46 million and was the second highest population growth in Malaysia [7]. The average population density in 2010 was 674 people per square kilometre. The study was conducted in 34 randomly selected Primary Healthcare Centres (PHC) out of 75 PHC in five selected districts with highest populations in Selangor. An unmatched case-control study was conducted. The study subjects were identified from the list of postnatal mothers who had antenatal check-up in the selected PHC in Selangor. The postnatal mothers with preterm babies (cases) and postnatal mothers with normal term babies (controls) were recruited after met the inclusion criteria: Malaysian, singleton, mothers with not known chronic medical diseases or previous bad obstetric history, received antenatal check-up at selected clinic and was recruited within 1 month post-delivery. Pre term was defined as babies born alive at delivery with estimated gestational age less than 37 weeks. Babies with no gestational age recorded were not recruited for case group. Cases were postnatal mothers who had preterm babies which were identified from maternal home-based record registry at the clinics. Controls were selected by systematic sampling using the list of postnatal mothers who attended the same PHC as the case with gestational age at delivery ≥37 weeks recorded in the home-based record. The sample size was determined based on previous study [8], which was related to maternal occupation among preterm delivery. It was calculated by Power and Sample Size 2 (PS2) based on Fleiss JL formulae [9]. The calculation used the value of alpha=0.05, power of 80%, probability of exposure in the control (P0=71.9), probability of exposure in case (P.^52.7) and the ratio of controls to cases as 1:1. Fifteen percent was added for the expected non-response, making the final sample size was 424 respondents. From the seven districts in the Selangor, five districts were purposively selected as they have the highest populations. The respondents were selected from 34 out of 75 PHC that shown highest antenatal attendance. The study was conducted from March to September 2013. A validated structured questionnaire was developed and administered to the participants through an interview. The consistency of the content was controlled by using only one interviewer. The questionnaire was developed by combining different set of questionnaires from various sources with permission. At present there in not known any specific questionnaire that can be used to assess maternal health seeking behaviour along the pregnancy stages. The questionnaire on nutritional domain and handling stress was adapted from Health Promoting Lifestyle II [10] while the physical activity assessment was adapted from the Pregnancy Physical Activity Questionnaire (PPAQ) [11]. The questionnaire was first developed in English, and then translated into Malay language. The questionnaire was pre-tested on ten postnatal mothers in Universiti Kebangsaan Malaysia Medical Centre (UKMMC) who were not included in the study.
The aim is to assess the face validity. A pilot study was done among 100 postnatal mothers to examine the reliability and construct validity of the questionnaire. The questionnaire contained two sections. The first section covers the sociodemographic characteristics, clinical data and delivery process as well as child's health description. Data for the first section was obtained from the maternal home-based record while the second section covers the maternal health seeking behaviour across the pregnancy stages were collected through an interview. The reliability (internal consistency) source of information was tested using Cronbach's alpha reliability coefficients. Cronbach's alpha coefficient was more than 0.7, an adequate level of internal consistency of instruments. Data were entered using SPSS version 21.0 for statistical analysis. Data exploration was done to visualize the general feature of the data. After exploration, frequency and percentages were used to assess the sociodemographic characteristics, obstetric profile and pre-pregnancy and antenatal behaviour. A logistic regression model was used to determine the association between different factors and preterm delivery. All variables were entered into bivariate analysis. In the multivariate analysis, variables which p value was more than 0.2 were fitted into multiple logistic regressions to predict factors of preterm delivery. The strength of association was interpreted using the adjusted odds ratio and 95% confidence interval (CI).
Ethical clearance was obtained from Medical Research Etiquette Committee, Faculty of Medicine, UKMMC and National Medical Research Register. Written consent through e-mail from the original authors of the questionnaires used was obtained and modification was done to accommodate with local people. Written consent was obtained from the participants before the research. Moreover, the participants were assured on the voluntarily and confidentiality of the information given.
Results
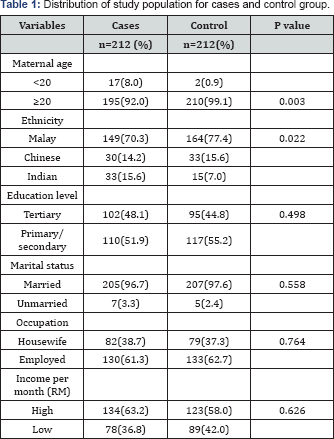
The total number of respondents participated were 424 postnatal mothers with 212 cases and 212 controls. The demographic characteristic of respondents was summarized in Table 1 Both groups the cases and controls were found not significant for education, marital status, occupation and income per month. However, a significant difference was noted for maternal age and ethnicity. Younger maternal age group (8.0% cases and 0.9% controls) and the Indian (15.6 % cases and 7.0% controls) were commonest among the preterm group.
Pre pregnancy stage
Majority of respondents from both groups had birth spacing of less than 2 years (69.5% cases and 72.2% controls). The result depicted that the majority of respondents have unplanned or mistimed pregnancies (72.2% cases and 58.0% of controls). Mistimed pregnancy is defines as wanted pregnancy but get pregnant not at suitable time. Majority of the respondents do not seek pre-pregnancy consultation, either from the government nor private sector and only low percentage (4-5%) for both groups received pre-pregnancy care counselling. Taken folic acid supplement during pre-pregnancy is not commonly practice. The finding showed a high percentage of not taken folic acid supplement in both groups (94.8% cases and 89.2% controls). Bivariate analysis revealed that family planning and taking folic acid supplement at prep regency stage has a direct and meaningful link to preterm birth. Mothers who have unplanned or mistimed pregnancies have a crude odds ratio of 1.88 (95% CI: 1.25-2.82) to experience a preterm birth, compared to mothers who planned their pregnancies. Mothers who practiced taking folic acid supplementation at pre-pregnancy have a crude odds ratio of 2.22 (95% CI: 0.21-0.95) for preterm births compared to mothers of controls group (Table 2).

Antenatal stage
During pregnancy, there are 3 variables that have a meaningful link to preterm delivery: primigravida, poor nutrition, and handling unhealthy stress (Table 3). A mother who is primigravida has a crude odds ratio of as much as 1.87 (95% SK 1.26-2.76) more likely to experience a preterm delivery as compared to a mother who is not primigravida (p value 0.002). Mothers who practice poor nutritional habits have a crude odds ratio of as much as 1.52(95% SK 1.04-2.22) with the p value=0.032. Mothers who passively deal with stress have a crude odds ratio of as much as 1.43 (95% SK 1.03-1.97) (Table 2).
Predicted factors for preterm delivery
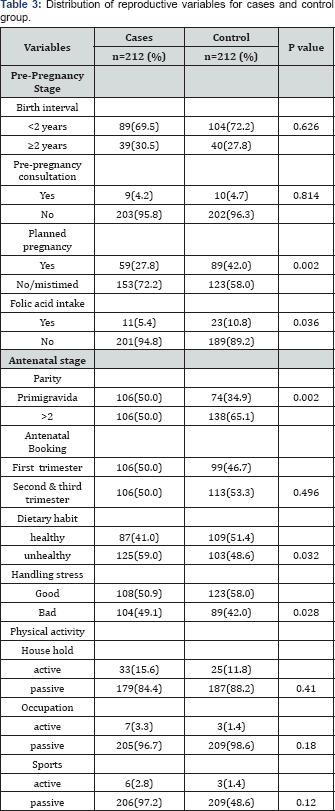
Multivariate logistic regression was conducted to predict the final determinant of preterm delivery All variables with p<0.25 in simple logistic regression were analysed. The following factors are predictive of preterm delivery: mothers of Indian ethnicity, primipara, unplanned pregnancy, not taking folic acid during pre-pregnancy and younger mother. Table 3 shows the multivariate analysis and it reveals that the group of mothers who are pregnant for the first time, are 1.84 times more likely to experience preterm delivery, as compared to mothers who are pregnant the second time or more (adjusted odds ratio=1.84, 95% SK1.21-2.78). Mothers of Indian ethnicity are more likely to experience preterm delivery 2.54 times when compared to mothers of other ethnicities (adjusted odds ratio=2.54, 95% SK 1.30-4.98). The third factor is family planning, where analysis shows that mothers who do not plan their pregnancies are 1.74 times more likely to experience preterm delivery as compared to those who plan their pregnancies (adjusted odds ratio=1.74, 95% SK 1.14-2.66). The fourth predictor of preterm delivery is the age factor. Mothers age <20 years are 4.89 times more likely to have preterm delivery as compared to mothers aged 20 and above (adjusted odds ratio=4.89, 95% SK 1.07-22.29). The fifth predictor is not taking folic acid during pre-pregnancy stage whereby the result shows that mothers who do not taken folic acid at pre pregnancy stage are at 2.21 times risk of more likely to experience preterm delivery when compared otherwise (adjusted odds ratio=2.21, 95% SK1.01-4.84).
Discussion
Mother's health seeking behaviour during pre-pregnancy and antenatal stages has an influence on perinatal outcome. Majority of research reveals that poor maternal health seeking behaviour results in poor perinatal outcomes, such as premature birth and low birth weight. This research differs from other researches because the researcher interviewed every respondent, as compared to other researches that use available data from hospitals. The main objective of this research is to identify the link between the behaviour in receiving maternal health care and preterm delivery. Results of the research reveals five predictive factors contributing to preterm delivery in Selangor that is: mothers of Indian ethnicity, mothers below 20 years of age, primigravida, not planned for the pregnancy and not taken folic acid pre-pregnancy stage. The result of this research is parallel to the research carried out at Hospital Seremban, which also discovered that mothers of Indian ethnicity are most at risk when compared to mothers of Chinese or Malay ethnicity [12].
Mothers below 20 years of age are 4.89 times more at risk compared to a mother age ≥20 years. The outcome of this research is supported by the meta-analysis of research done by Gibbs et al. [13] that states, a young mother has a risk of 1.68 times [13]. There are many theories that are often said to be linked to the risk of young mothers and the perinatal outcomes, such as preterm delivery. A popular theory is the competition for nutrients between mother and the foetus in pregnancy [14].Other theories explain that young mothers (aged 19 and below) have just experienced puberty, therefore there is a biological impact on a mother's growth, in which the mother's pelvic bone and height are insufficient and interferes with the growth of the foetus she is carrying. This causes the baby to be born earlier that date as compared to a mother who is an adult [13]. There are also views that say mothers aged 19 and below normally lack sufficient knowledge in preparing for pregnancy and the maternal behaviour regarding health care pre-pregnancy and during pregnancy [15].
This research outcome is similar to earlier research outcomes that say primigravida have a higher risk compared to mothers with a multi para status [15-17]. Meta-analysis outcomes are used to research simultaneously the parity effect and mother's age and find that these two factors are linked to preterm delivery, that is mothers who are 18 years of age and nulliparous, prove to be the group that has the highest risk compared to other ages and parities. Therefore, present research finding is parallel to the outcome of the meta-analysis outcome research that finds both factors which are below 20 years of age and primigravida have a high risk of premature birth [18].
Family planning status is one of the important predictive factors to determine the likelihood of a preterm delivery, that is, mothers who are not plan to be pregnant have higher risk of 1.74 times as compared to a mother who planned to be pregnant. The outcome of this research is parallel to earlier researches which use population data from PRAMS (Pregnancy Risk Assessment Monitoring Surveillance) in the United States of America which also found that mothers who do not intend or do not plan to be pregnant have a risk of as much as 1.16 times as compared otherwise [19].
The outcome of the multivariate analysis reveals that the practice of taking folic acid pre pregnancy has a meaningful link to preterm delivery. Mothers who do not practice this have a risk of as much as 2.21 of having preterm delivery as compared otherwise. There are various researches that have different outcomes in relation to the practice of taking folic acid during pre-pregnancy, that is, there are researches carried out in Holland revealing that this practice only has a meaningful link to low birth weight and not to preterm delivery [20]. The Sweden cohort research also found that there is no protective effect of folic acid against preterm delivery [21]. However, the dosage and duration of folic acid taken by the mothers before pregnant, geographical conditions (home), as well as the mother's own daily nutrition may need to be explore further as a micro increment or decrease on a human body may play different role. Generally up to this point, there still is no research that proves the practice of taking folic acid during pre-pregnancy has any positive link in preventing premature birth, but it has a weak correlation to the increase in a baby's average birth weight, which is in tandem with the latest meta-analysis of research [2223]. However, present study has proven it beneficial in Selangor Malaysia mothers who plan for future pregnancy
Conclusion and Recommendation
The present research reveals that 5 predictive maternal health seeking behaviour such as family planning practice, taking folic acid during pre-pregnancy, younger maternal age; Indian ethnicity and primiparity are higher risk of preterm delivery. This reveals that mother's health seeking behaviour during pre-pregnancy is very important as it also has an effect in preventing preterm delivery. Therefore, knowledge related to maternal behaviour in getting the right health care during prepregnancy, especially in family planning, needs to be emphasised among all groups of reproductive women especially the first time pregnancy, younger age and Indian minority group through health promotion that needs to be carried out in the community based and further emphasizing at clinic based. As been recommended by WHO [24] which stated that the important of bottlenecks faced identification by countries in implementation of effective new born health interventions at scale and their possible solutions. Therefore based on present study findings, Malaysia must emphasize on pre-pregnancy care services targeted to all reproductive age couple for screening and gain knowledge in preventing bad maternal and perinatal outcomes.
This research has limitations, in which, it was only carried out in Selangor, which was purposive. Therefore, it can only be generalised to the population in Selangor. The data that was collected, may also be subject to recall bias as the interviews were conducted retrospectively, and there is a possibility past information may not be remembered fully. In the future, this research may be carried out with matched control group for age and ethnicity.
Acknowledgement
We acknowledge our respondents participation, healthcare workers who helped during data collection process. We thank to the UKM who granted for this study
Declaration
Author(s) declare that there is no conflict of interest. All authors are responsible for the content and writing of the paper.
References
- WHO (2012) The worldwide incidence of preterm birth: a systematic review of maternal mortality and morbidity (Internet). World Helath Organisations, Geneva, Switerzland.
- Tucker J, McGuire W ( 2004) Epidemiology of preterm birth. BMJ 329(7467): 675-678.
- Beck S, Wojdyla D, Say L, Betran AP, Merialdi M, Requejo JH, et al. (2010) The worldwide incidence of preterm birth: a systematic review of maternal mortality and morbidity. Bulletin of the World Health Organization 88(1): 31-38.
- Lin YH, Tsai EM, Chan TF, Chou FH, Lin YL (2009) Health promoting lifestyles and related factors in pregnant women. Chang Gung Med J 32(6): 650-661.
- United Nations Malaysia (2016) Millennium Development Goals Report 2015.
- Sutan R, Norsafinaz M, Tamil AM, Areena Y (2016) A Case Control Study on Maternal Health-Seeking Behavior at Pre-Pregnancy Stage among Mothers with Low Birth Weight Babies. Womens Health Gynecol, Volume 2(7).
- Department of Statistics Malaysia (2014) Report On Characteristics of Household 2010.
- Gungor I, Oskay U, Beji NK (2011) Biopsychosocial risk factors for preterm birth and postpartum emotional well-being: a case-control study on Turkish women without chronic illnesses. Journal of clinical nursing 20(5-6): 653-665.
- Fleiss JL, Levin B, Cho Paik M (1981) Statistical Methods for Rates and Proportions. In: Shewart WA, Wilks SS, Wiley Series in Probability and Statistics. (3rd Edn), John Wiley & Sons, USA.
- Walker SN, Sechrist KR, Pender NJ (1987) The Health-Promoting Lifestyle Profile: development and psychometric characteristics. Nursing Research 36(2): 76-81.
- Chasan-Taber L, Schmidt MD, Roberts DE, Hosneo D, Markenson G, et al. (2004) Development and validation of PPA Questionaire. Journal of American College of Sports Medicine, pp. 1750-1760.
- Yadav H, Lee N (2013) Maternal factors in predicting low birth weight babies. The Medical Journal of Malaysia 68(1): 44-47.
- Gibbs CM, Wendt A, Peters S, Hogue CJ (2012) The impact of early age at first childbirth on maternal and infant health. Paediatric and Perinatal Epidemiology 26(Suppl 1): 259-284.
- King JC (2003) Life and Fitness The Risk of Maternal Nutritional Depletion and Poor Outcomes Increases in Early or Closely Spaced Pregnancies 1. The Journal of Nutrition Supplement 1732-1736.
- Nazari M, Zainiyah SYS, Lye MS, Zalilah MS, Heidarzadeh M (2013) Comparison of maternal characteristics in low birth weight and normal birth weight infants. Eastern Mediterranean Health Journal 19(9): 775781.
- Majoko FM, Nystrom L, Munjanja SP, Mason E, Lindmark G (2004) Relation of parity to pregnancy outcome in a rural community in Zimbabwe. African journal of reproductive health 8(3): 198-206.
- VelosoHJ, Selva AA,Bettio lH, Goldane M, Fernado (2014) Low birth weight in Sao Luis, northeastern Brazil: trends & associated factors. BMC pregnancy & Childbirth 14: 155.
- Kozuki N, Lee AC, Silveira MF, Sania A, Vogel JP, et al. ( 2013) The associations of parity and maternal age with small-for-gestational- age, preterm, and neonatal and infant mortality: a meta-analysis. BMC Public Health 13(Suppl 3): S2.
- Mohllajee AP, Curtis KM, Morrow B, Marchbanks PA (2007) Pregnancy intention and its relationship to birth and maternal outcomes. Obstetrics and gynecology 109(3): 678-686.
- Timmermans S, Jaddoe VWV, Hofman A, Steegers-Theunissen RPM, Steegers EP (2009) Periconception folic acid supplementation, fetal growth and the risks of low birth weight and preterm birth: the Generation R Study. The British journal of nutrition 102(5): 777-785.
- Sengpiel V, Bacelis J, Myhre R, Myking S, Pay AD, Haugen M, et al. ( 2013) Folic acid supplementation, dietary folate intake during pregnancy and risk for spontaneous preterm delivery: a prospective observational cohort study. BMC Pregnancy and Childbirth 13: 160.
- Lassi ZS, Salam RA, Haidar RA, Bhutta Za (2013) Folic acid supplemtation during pregnancy for maternal health & pregnancy outcomes.The Cochrane Library issue 3: CD006896.
- Montavani E, Filippini F, Bortolus R, Franchi M (2014) Folic acid supplementation and preterm birth : Results from observationals studies. Biomed Reserach International p. 8.
- WHO UNICEF (2014) Every Newborn: an action plan to end preventable deaths: Executive summary. World Health Organization, Geneva, Switzerland.






