Osteonecrosis of the Maxilla Associated With Conjugated Oral Pamidronate and Alendronate Usage for Breast Cancer Metastasis Prevention
Eduardo Azoubel1, Pedro Pinto Berenguer1, Neiana Carolina Rios Ribeiro2, Maria Cecilia Fonseca Azoubel2 and Eber Luis de Lima Stevao3
1Oral and Maxillofacial surgeon, State University of Feira de Santana, Brazil
2Bahiana School of Medicine and Public Health, Brazil
3Baylor University Medical Center, USA
Submission: June 27, 2017; Published: December 13, 2017
*Corresponding author: Eduardo Azoubel DDS, MS, Avenida Antonio Carlos Magalhaes 771 sala 501 Ed. Torre do Parque- Itaigara, Salvador - Bahia, Brazil, Email: azoubel.eduardo@gmail.com
How to cite this article: Eduardo A, Pedro P Be, Neiana C R R, Maria C F A, Eber L L S. Osteonecrosis of the Maxilla Associated With Conjugated Oral Pamidronate and Alendronate Usage for Breast Cancer Metastasis Prevention. Adv Dent & Oral Health: 2017; 7(2): 555706. DOI: 10.19080/ADOH.2017.07.555706
Abstract
Bisphosphonates are a class of medicines which have been used for almost two decades now for management of various healths conditions such as but not limitedto:
a. Osteoporosis,
b. Paget's disease,
c. Multiple myeloma,
d. Hypercalcemia associated with malignancy,
e. Breast, prostate, and lung cancer.
Currently it has been advocated these drugs are causative factors for osteonecrosis of the jaws which can be associated or not to dental intervention during patient's medication intake. Its occurrence has been frequently reported since the first case published in the early 2000s and with the increasing number of patients receiving these therapy dentists must be aware of possible side effects that may occur in the jaws due to long term use of these drugs. Also dental professionals must be able to help preventing osteonecrosis of the jaws occurrence by discussing with oncologists and endocrinologists the best therapy for their common patient, recognizing its signs and symptoms when present, and establishing a correct treatment for osteonecrosis of the jaws linked to bisphosphonates. The aim of this article is to describe an aggressive case of hemimaxilla osteonecrosis in a patient treated by bisphosphonates due to breast cancer, presenting its clinical and imaginological characteristics, as well as the surgical and prosthetic rehabilitation delivered treatment.
Keywords: Bisphosphonate; Osteonecrosis of jaw; Breast cancer
Introduction
Osteonecrosis of the jaws (ONJs) associated with the use of bisphosphonates (BPs) has become one of the most prominent puzzles not only in the dental community but also in the medical field as a whole [1]. ONJs are a clinically defined condition in which necrotic lesions of the mandible and/or maxilla develop and persist after a course of therapy with BPs [2].
The introduction of BPs has effectively helped the treatment of patients with cancer and disseminated bone disease; however, this evidence links its use with the occurrence of ONJs. Studies of large populations using such drugs provoking inflammatory conditions of the jaws have shown that patients who undergone surgical procedures have an increased risk of developing ONJs [3,4].
With the increasing number of patients receiving BPs therapy in current day's dental surgeons must be aware of possible side effects that may occur in the jaws due to prolonged use of such drugs, becoming able to recognize its signs and symptoms, prevent its complications as well as treat possible resulting pathologic processes.
Literature Review
Bisphosphonates are bone resorption inhibitors - osteoclast- mediated bone loss - used in treating a variety of diseases, such as osteoporosis, metabolic and metastatic bone diseases, hypercalcemia, Paget's disease, and multiple myeloma [5].
The ability of BPs to reduce tumor burden in the pre-clinical models of bone, has led to further studies on the potential benefits of using BPs to prevent or retard bone metastases, particularly in women with primary operable breast cancer [6].
The BPs suppress osteoclast-mediated bone remodeling for the purpose of preventing pathologic fractures, having a differential effect on different levels on the tissue [1,5]. Bisphosphonates are mainly concentrated in the jaws, as these have a greater blood supply compared to other bones and a more rapid bone remodeling that is related to the presence of teeth which determine bone remodeling daily around the periodontal ligament [7].
It is well known that patients treated with BPs can develop ONJs associated with the use of these drugs and this has been widespread among dentists since its first description in 2003 [8]. The differential diagnosis of ONJs should specifically exclude other common intraoral conditions including:
a. Periodontal disease,
b. Gingivitis or mucositis,
c. Osteomyelitis,
d. Bone tumors and metastases among others [9].
To distinguish ONJs from other conditions the following definition of ONJs was adopted by the American Association of Oral and Maxillofacial Surgeons (AAOMS) where patients can be considered as having all the three following ONJs characteristics present, as seen in Table 1 below.


Risk patients are those who are using BPs but do not have ONJs with bone exposure. When there is an exposure the ONJs can be classified accordingly to their clinical characteristics [10], as shown in Table 2 below
When bone exposed is identified by the dentist or oncologist, even if it is minimal exposure, the patient should be referred to an oral maxillofacial (OMF) surgeon who can better inform this patient about the nature of the disease and the bone exposure irreversibility without specific and indicated management, coordinating treatment in conjunction with the oncologist and endocrinologist [7].
With regard to the treatment of patients with ONJs priority should be given to eliminate pain if present, control soft and hard tissues infection, diminish the progression or the occurrence of bone necrosis [10]. Any or further dentoalveolar surgery increases the risk of developing osteonecrosis so dental procedures such as tooth extraction, bone grafting, implant placement must be avoided. Is essential for the periodontist to upholding a very good clinical oral health and patient's awareness of maintaining a good hygiene in order to prevent future problems [4].
Case report
A 64 y.o. white female in 2011 sought her dentist reporting severe pain in the right upper molars. On clinical evaluation bone exposure was found in the interproximal areas of teeth number 2 and 3 (American Dental Association Tooth Numbering System). X-ray of the region showed crestal alveolar bone loss supporting those teeth. The dentist proceeded to adjust dental occlusion, performed periodontal scaling and placement of surgical cement. Days followed with no change in the patient painful condition and the decision was made to extract tooth number 2 and 3 which surgical procedure subsequently caused an increase in bone exposure.
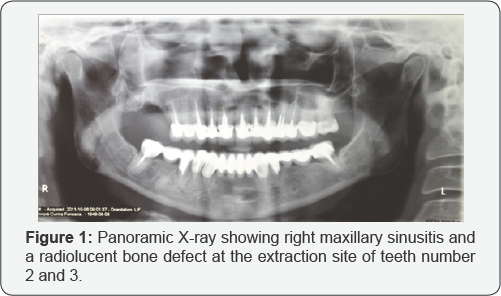
In the same year patient sought dental assistance consulting with other dentist. A Panoramic X-ray was obtained which showed abnormal right maxillary sinus transparency suggestive of sinusitis but normal radiolucency in the region of tooth number 3 evocative of bone healing after tooth extraction (Figure 1).
With the persistence of non-healing teeth extraction sites in 2012 patient sought dental care with an oral and maxillofacial surgeon who requested a CT scan of her face (Figure 2).

The CT revealed specific findings presenting an inflammatory and/or infectious process in the right maxillary sinus. Possible diagnosis for osteomyelitis was done but during her medical report review it was found that she had breast cancer in the past, also sustaining cancer therapy since 2005 and there were no medical authorization for her to be submitted to any dental surgical procedure.

After being examined by a periodontist in 2013 the patient was referred to an OMF surgeon for evaluation of an uncured maxillary osteomyelitis. After evaluating preexisting radiographs, CT scans, conducting an extensive interview about the specific medication she was taking, and intraorally analyzing the characteristics of the white-yellowish devitalized exposed bone, the diagnosis of ONJs induced by BPs affecting the right posterior maxilla was done (Figures 3A-3B).
In her medical history she reported fighting breast cancer for six years, hypertension, osteoporosis, and by indication of her oncologist she started systemic therapy with oral Pamidronate and Alendronate. Bone scintigraphy was requested, which showed intense uptake in the right hemimaxilla extending almost to the midline region.
Some initial measures were adopted by the OMF surgeon:
i. Discussed with her oncologist about BPs suspension for ninety days,
ii. Sent the patient for initial ten sessions of hyperbaric oxygen therapy, and

iii. Administration of antibiotics (metronidazole and amoxicillin) during six days prior surgery. During surgery careful but effective bone debridement was performed (Figure 4A-4D).
To remove all necrotic bone the whole right hemimaxilla was removed since it was already sequestrated and separated from supporting still vital bone (Figure 5).
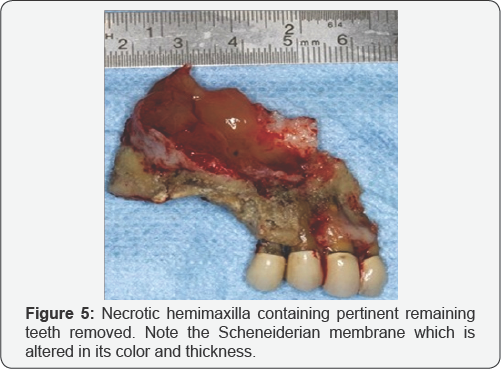

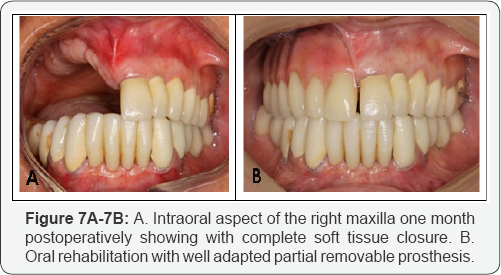
Right maxillary sinus curettage was performed and all remaining bone irregularities were smoothed off with a round bur. Non-interrupted suture with 3-0 poliglecaprone 25 monofilament was completed (Figures 6A-6C). There was a partial loss of the right nasal fossa floor as shown in Figure 4D, along with the anterior and lower wall of the right maxilla, and all ipsilateral teeth. Postoperative medication was conducted with clindamycin, analgesics and mouthwash with chlorhexidine during fourteen days. Again another ten sessions of hyperbaric oxygen therapy was completed. A removable partial denture was lab made for her one at forty five days after surgery (Figures 7A--7B). In subsequent clinical and radiological follow-ups the patient showed signs of complete healing. She is still under continuous supervision by her oral and maxillofacial surgeon.
Discussion
Osteonecrosis of the jaws (ONJs) is typically progressive leading to a subsequent involvement of adjacent teeth. The most common clinical finding in the ONJs is an ulcerated mucosa area and exposed devitalized bone, it has a whitish-yellow color and the surrounding areas of inflamed soft tissue present [11]. The characteristics presented in this clinical case resemble the exact description done by Zanata et al. [12].
The alveolar bone surgery in patients with chronic use of BPs highly increases the risk of developing osteonecrosis [11]. As reported here the patient had an spontaneous bone exposure which was aggravated by two surgical procedures. No specific cares were taken for the scaling neither for teeth extractions which consisted in a major fault.
Patients who have ONJs may present asymptomatically with bone exposure and no evidence of local erythema or may present with pain and evidence of local infection [10]. In this case the patient had painful symptomatology with bone exposure due to the chronic use of oral specific conjugated BPs, Pamidronate and Alendronate. Accordingly to the literature such drugs may increase the risk of developing ONJs since they are regarded as the most potent oral BPs [5].
There is still no consensus in the current literature about a treatment protocol for ONJs, but it is suggested a combination of lesion surgical treatment with antibiotic therapy which should be continued for at least ten days [10,12]. Regarding the specific treatment in this case described, antibiotic therapy, surgical removal of devitalized bone associated with varied sessions of hyperbaric oxygen therapy was clearly established.
The literature is conflicting regarding the use of hyperbaric oxygen and some authors claim that there is no clear benefit for those patients with the presence of exposed bone induced by BPs [8,11]. However, there are some findings in the scientific literature indicating that hyperbaric oxygen is an effective adjuvant therapy in situations where normal healing is impaired, improving wound repair, reducing edema, inflammation, bringing benefits to patients [2]. In this clinical case BPs were suspended for three months and subsequent twenty sessions of hyperbaric oxygenation were conducted which certainly helped in the healing process of the remaining parts of right maxilla and soft tissue repair
The literature shows that ONJs is a serious side effect of using BPs [3], which can be confirmed with this reported case. The patient was taking oral BPs for bone metastasis control for many years. Thus, when BPs therapy is initiated patients should be advised to be also followed by an OMF surgeon so as to ensure and encourage patient to maintain a good oral health in order to prevent or make an early diagnosis of ONJs.
In this report it was clearly noted that the patient underwent consultation and treatment in several dentists and it took about three years for her to get the correct diagnosis. It aggressively points to the extreme importance of further professional education and studies on the association between BPs and ONJs. It is indispensable general dentists and specialists to train in differential pathology diagnosis and multidisciplinary approach involving dental clinician, OMF surgeon, periodontist, prosthodontist, oncologist, endocrinologist, oncologic surgeon.
Conclusion
Bisphosphonates are associated with the development of osteonecrosis of mandible and maxilla with or without previous dental interventions, which is extremely important the interaction of dentists with the theme, assisting in the prevention and diagnosis of these injuries by recognizing the signs and symptoms, elucidating the diagnosis thus indicating an appropriate treatment for each situation. Regarding to this patient antibiotic therapy, surgical debridement, hyperbaric oxygen therapy, oral rehabilitation resulted in a satisfactory treatment.
References
- Allen MR, Burr, DB (2009) The Pathogenesis of Bisphosphonate-Relat- ed Osteonecrosis of the Jaw: So Many Hypotheses, So Few Data. J Oral Maxillofac Surg 67(5): 61-70.
- Freiberger JJ (2009) Utility of Hyperbaric Oxygen in Treatment of Bis- phosphonate-Related Osteonecrosis of the Jaws. J Oral Maxillofac Surg 67(5): 96-106.
- Kos M, Brusco D, Kuebler J, Engelke W (2010) Clinical comparison of patients with osteonecrosis of the jaws, with and without a history of bisphosphonates administration. Int J Oral Maxillofac Surg 39(11): 1097-102.
- Ruggiero SL, Fantasia J, Carlson E (2006) Bisphosphonate-related osteonecrosis of the jaw: background and guidelines for diagnosis, staging and management. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 102(4): 433-441.
- Woo SB, Hellstein JW, Kalmar JR (2006) Systematic Review: Bisphosphonates and Osteonecrosis of the Jaws. Ann Intern Med 144: 753-61.
- Coleman RE, Mccloskey EV (2011) Bisphosphonates in oncology. Bone 49 (1): 71-76.
- Marx RE, Sawatari Y, Fortin M, Broumand V (2005) Bisphospho- nate-Induced Exposed Bone (Osteonecrosis/Osteopetrosis) of the Jaws: Risk Factors, Recognition, Prevention, and Treatment. J Oral Maxillofac Surg 63(11): 1567-1575.
- Marx RE (2003) Pamidronate (aredia) and zoledronate (zometa) induced avascular necrosis of the jaws: a growing epidemic. J Oral Maxillofac Surg 61(9): 1115-1117.
- Khosla S, Burr D, Cauley J, Dempster DW, Ebeling PR, et al. (2007) Bi- sphosphonate-Associated Osteonecrosis of the Jaw: Report of a Task Force of the American Society for Bone and Mineral Research. Journal of Bone and Mineral Research 22(10): 1479-1491.
- Ruggiero SL, Dodson TB, Assael LA, Landesberg R, Marx RE, Mehro- tra B (2009) American Association of Oral and Maxillofacial Surgeons Position Paper on Bisphosphonate-Related Osteonecrosis of the Jaws- 2009 Update. J Oral Maxillofac Surg 67(5): 2-12.
- Migliorati CA, Schubert MM, Peterson DE, Seneda LM (2005) Bisphos- phonate-Associated Osteonecrosis of Mandibular and Maxillary Bone. Cancer 104(1): 83-93.
- Zanata A, Felin GC, Bona MC, Sawazaki R, Conto F (2014) Osteonecro- se mandibular associada ao uso debisfosfonato de sodio em paciente com mieloma multiplo. Rev port estomatol med dent cir maxilo fac 55(2): 115-120.






