Human Papilloma Virus in Women with Bad Obstetric History, Kirkuk, Iraq
Abdulghani Mohamed Alsamarai*1, Hala Mohamed Majeed2 and Amina Hamed Alobaidi3
1Tikrit University College of Medicine, Iraq
2Tikrit University College of Veterinary Medicine, Iraq
33Kirkuk University College of Veterinary Medicine, Iraq
Submission: November 22, 2016; Published: December 13, 2016
*Corresponding author: Abdulghani Mohamed Alsamarai, Tikrit University College of Medicine, Tikrit, Iraq, E-mail:galsamarrai@yahoo.com
How to cite this article: Abdulghani M A, Hala M M, Amina H A. Human Papilloma Virus in Women with Bad Obstetric History, Kirkuk, Iraq. JOJ Immuno Virology. 2016;1(4):555566. DOI: 10.19080/JOJIV.2016.01.555566
Abstract
Background: Bad obstetric outcomes are considered as major health problem with social and medical impact on society, with multiple etiology.
Study Design: Descriptive Case Control Study
Aim: to evaluate the role of HPV-16 and HPV-18 in pregnancy loss in women in Kirkuk, Iraq.
Materials and Methods: The study included 60 women with BOH, of them 20 were pregnant and 20 were non-pregnant at time of enrolment in the study. In addition, 20 women with inevitable abortion were included in the study. Also the study included 28 women with normal pregnancy as control and 14 of them were pregnant and 14 were non-pregnant. Serological study carried out to determine HPV -16 IgG, and HPV -18 IgG antibodies using ELISA kits.
Results: the overall HPV seroprevalence was 3.4% for both HPV-16 and HPV-18. In women with BOH serprevalence was 7.5% and 2.5% for HPV-16 and HPV-18 respectively. While in control [normal pregnancy] none of the tested sera show a positive result. In women with inevitable abortion, HPV-18 detected in 10% of the tested samples. HPV-16 was with higher seroprevalence in non-pregnant (5.9%) as compared to pregnant (2.9%) women, however, not reach a significant level.
Conclusions: Although, HPV-16 and HPV-18 infections were detected in low rate in women with BOH and not in women with normal pregnancy, however, a large scale study warranted.
Keywords: BOH; HPV; Human Papilloma virus; IgG
Introduction
Human Papilloma virus is one of the tumor viruses and studies suggested a link between some HPV types and development of tumors such as oropharyngeal [1], and cervical cancer [2]. Bad obstetric outcome is one of the major social problems in Iraqi population with a wide range of etiology. Infections are implicated as an important cause of bad pregnancy outcomes [3,4]. Recent studies in Iraq suggest that Toxoplasma gondi, Cytomegalovirus, Rubella virus, and Herpes Simplex Virus infections were with positive association with BOH [5-14]. In addition, abnormal immunological responses may play a role in the pathogenesis of bad pregnancy outcomes [15,16]. Human papillomavirus is viral infection that may affect the pregnancy outcome [17]. Forty-eight studies provided HPV- type specific prevalence data in women with normal cytology. The five most common types of HPV were HPV 16 (2.5%), HPV 18 (0.9%), HPV 31 (0.7%), HPV 58 (0.6%) and HPV 52 (0.6%). The authors estimated that the overall burden of HPV infection from the age-specific adjusted prevalence in cytological normal women to be 291 million women infected with HPV of whom 23.3% were estimated to be infected with HPV 16 and 8.5% with HPV 18 [18]. BOH is still represent a medical and social problem and may microbiological infections reported to be associated with pregnancy loss [4].
Previous studies [19-29] outlining the prevalence of maternal HPV was identified. The seroprevalence of HPV-16 was with a range of 1.3% in China [22] to 97.71% in China [23]. While, HPV-18 seroprevalence was with a range of 0.5% in China [22] to 27.6% in Brazil [25]. Since we don’t find a study in literature that evaluates the association between HPV infection and bad pregnancy outcomes. Thus this study was conducted to clarify the risk assessment of HPV infection in women with bad obstetric history.
Materials and Methods
Study design and settings
The study design is a Descriptive Case Control Study and was performed in Kirkuk General Hospital. The study proposal was approved by Tikrit University College of Science ethical committee and Kirkuk Health Authority Research Committee. Informed consent taken from each woman included in the study.
Study Population
The study population is women with childbearing age. Study population was recruited from Kirkuk General Hospital. 88 women with age range from 14 to 48 were included in the study, of them 60 with history of bad pregnancy outcomes and 28 women with normal pregnancy as control. The study included 60 women with BOH, of them 20 were pregnant and 20 were non-pregnant at time of enrolment in the study. In addition, 20 women with inevitable abortion were included in the study. Also the study included 28 women with normal pregnancy as control and 14 of them were pregnant and 14 were non-pregnant. For serological analysis, 5-10 mL of venous blood was collected in a sterile container with strict aseptic precautions from each study subject. The serum was separated and stored in numbered aliquots at -20°C till assayed. All the serum samples collected from the study and control groups were tested for HPV-16 and HPV-18 IgG using commercially- available (ELISA) kits. The results read by a Microwell reader and compared in a parallel manner with controls; optical density read at 450 nm on an ELISA reader.
Collection of data
All recruited women were subject for clinical examination and laboratory investigations were carried out for the study subjects to exclude other causes of foetal wastage, such as hypertension, diabetes mellitus, syphilis, Rh (rhesus) incompatibility, physical causes of abortion, and consanguinity. Subjects with known causes of foetal wastage were excluded from the study. All of them were interviewed to ascertain age, medical and obstetric information.
Statistical analysis
The proportion and the mean value were computed in appropriate situations. The data analyzed using the SPSS (Version 16). The study finding data were presented as mean and student t test and ANOVA were used to determine significance of differences between groups.
Results
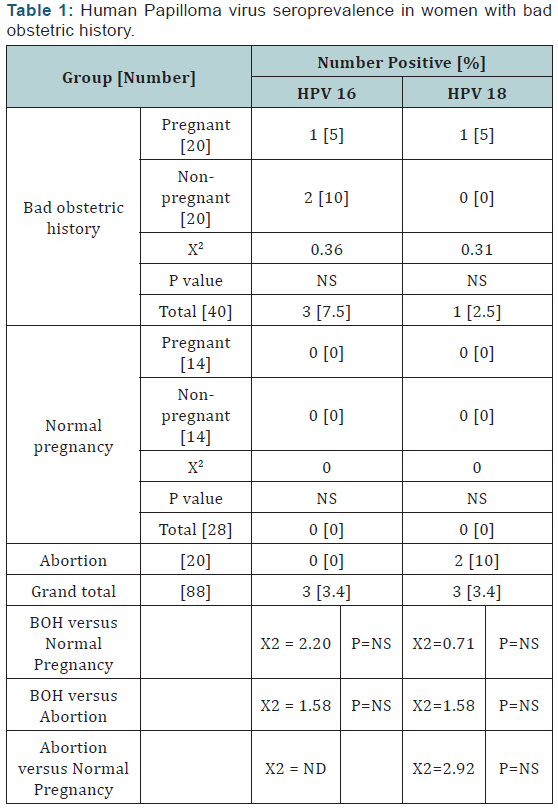
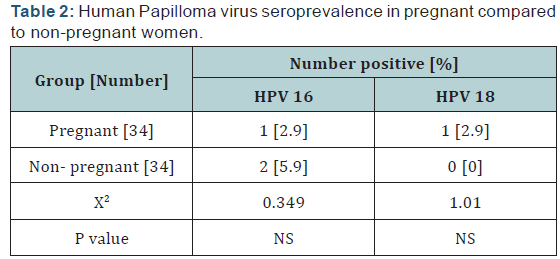
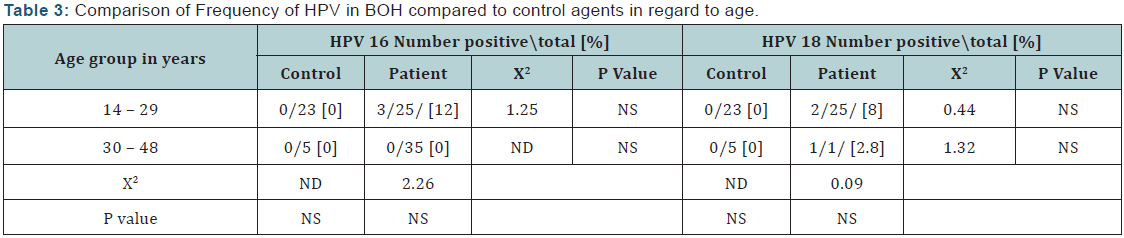
The overall HPV seroprevalence in our study population was 3.4% for both HPV 16 and HPV 18. In women with BOH seroprevalence was 7.5% and 2.5% for HPV 16 and HPV 18 respectively, as shown in (Table 1) while in the control group (normal pregnancy) none of the tested sera show a positive result. In women with inevitable abortion, HPV 18 detected in 10% of the tested samples.HPV 16 was with higher seroprevalence in non pregnant (5.9%) as compared to pregnant (2.9%) women, however, did not reach a significant level, as shown in (Table 2). HPV 16 seroprevalence was 12% in women with age of 14-29 years, while all were negative in the control group as shown in (Table 3). However, HPV 18 was seropositive in 8% of women in the age of 14-29 years, and in 2.8% in women with age of 30-48 years, but the difference was not significant. There was no significant difference in HPV 16 and HPV 18 seroprevalence between control and patients for age groups, as shown in (Table 3).
Discussion
In the present study HPV 16 and HPV 18 seroprevalence was 3.4% for each (3/88). In addition, HPV16 seroprevalence was higher in women with BOH (7.5%) as compared to those with normal pregnancy outcome (0%). However, this difference was not statistically significant. Furthermore, all women with inevitable abortion were negative for IgG HPV 16, while IgG HPV 18 was positive in 10% of women with inevitable abortion.
The present study seroprevalence of HPV 16 IgG in women with BOH (7.5%) was higher than that reported for other geographical areas using PCR technique, such as in China (1.3%) [22], Brazil (5.3%) [25] and Iran (5.8%) [19]. However, our finding was lower than that reported for Iran (10%, 73.9%) [28, 29], West Africa (17.6%) [27], Egypt (20%) [20], Morocco (42.5%) [21], Brazil (53.3%) [25], Saudi Arabia (71%) [24] and China (97.7%) [23].Thus the prevalence of HPV16 varies in different geographical areas and there may be wide a variation in its prevalence within the same country. For example, in China one research group reported the prevalence rate of 1.3%, while other study reported the prevalence of 97.7% [23]. In addition, the same pattern was reported for the Iran [28,29].
HPV 18 seroprevalence in women with BOH was 2.5%, which was higher than the prevalence reported for China (0.5%) [22] and Brazil (1.3%) [26]. However, the present study seroprevalence was lower than that reported for Iran (4-11.6%) [28], Egypt (10%) [20], China (14.2%) [23] West Africa (14.8%) [27], Saudi Arabia (15%) [24] and Brazil (27.6%) (476). The HPV 18 seroprevalence (2.5%) as this study indicated was lower than that of HPV 16 seroprevalence (7.5%). This finding was consistent to the studies reported globally which indicated a high prevalence of HPV 16 as compared to HPV 18.
In addition, HPV 18 seroprevalence was higher in women with inevitable abortion (10%) as compared to HPV 16 seroprevalence (0%). There was no reported data in literature to compare with. However, this finding may be influenced by the small size sample. Furthermore, both HPV 16 and HPV 18 seroprevalence was more in BOH women with age of <30 years, which may be a reflection of sexual activity. However, OR did not confirm an association between HPV 16 and HPV 18 infection age of < 30 years. Ampuhl et al. [30] in a recent review found that there was an association between HPV infection and spontaneous abortion or preterm delivery. Other study reported that HPV infection was associated with preterm rupture of membrane [31]. Genital HPV infection is the most common sexually transmitted infection in the world although detection of HPV types by polymerase chain reaction (PCR) assays varies greatly with age and by geography. Clifford et al [18] in a study that included women selected randomly from eleven countries found that age standardized prevalence varied nearly 20 times between different populations. The lower prevalence of 1.4% in Spain, while the higher prevalence of 25.6% in Nigeria. In addition, the overall, age standardized HPV prevalence was five times higher in sub-Saharan Africa than in Europe with intermediate prevalence in South America and Asia. Furthermore, HPV - 16 was the commonest type in all regions except in sub-Saharan Africa, where HPV-35 was equally as common. Sanjose, et al. [32] in a large scale meta-analysis study that included 157 879 women with normal cytology found that HPV global prevalence was 10.4% and was less in developed countries (10.6%) as compared to developing countries (15.5%). High prevalence was for Africa (22.1%), followed by Central America and Mexico 20.4%, Northern America 11.3%, Europe 8.1% and Asia 8.0%. HPV prevalence was highest in women younger than 34 years, with a decrease in the 35-44 year group. There was as second peak from age 45-54 years in all regions except Asia [18]. The predominant HPV type was HPV-16 (2.5%), followed by HPV 18 (0.9%), HPV 31 (0.7%), HPV 58 (0.6%) and HPV 52 (0.6%).
The present study shows that HPV 16 was with lower seroprevalence in pregnant women (2.9%) as compared to nonpregnant women (5.9%), but the difference was not statistically significant. However, HPV 18 seroprevalence was higher in pregnant (2.9%) than in non-pregnant (0%) women, but the difference was not statistically significant. In contrast, Salcedo, et al. [33] in Brazil found that HPV infection was higher in pregnant as compared to non-pregnant. Other study by Liu, et al. [34] in 2014 conducted on the frequency of HPV among 13640 pregnant and non pregnant women reported that frequency of HPV infection was 16 – 82% in pregnant and 12-25% in non pregnant. Immunological or hormonal changes may alter the prevalence of HPV and its clearance during pregnancy [35]. Some researchers reported decreased clearance of high-risk HPV types in the first two trimesters of pregnancy, contributing to a high prevalence of HPV during pregnancy [36]. The prevalence of HPV DNA among pregnant women that we observed (5.7%; 5 cases /88 samples) was lower than that in general female population of China (13.8%) [37] and BOH cases in Iran [28,29]. Other study in China not found a significant prevalence difference between the prevalence of HPV DNA and the pregnancy status [38].
The vertical transmission of HPV from mother to neonates represents a health problem with impact on child health. In 5.2% of neonates born to healthy women were infected with HPV and was associated with detection of HPV in mothers during any of the pregnancy trimester [39]. Thus vaccination is the best health care approach for the prevention and control of HPV infections. The two commercially available HPV vaccines are good in induction of antibody that was 7 fold higher than natural infection for at least twenty years post vaccination [40].
Conclusion
In conclusion, although, HPV-16 and HPV-18 infections were detected in low rate in women with BOH and not in women with normal pregnancy, however, a large scale study warranted.
References
- Kuo HK, Fujise K (2011) Human papillomavirus and cardiovascular disease among u.s. Women in the national health and nutrition examination survey, 2003 to 2006. J Am Coll Cardiol 58(19): 2001- 2006.
- Chaturvedi A, Maura L, Gillison A (2010) Human Papillomavirus and Head and Neck Cancer. (1st edn), Springer, New York, 978(1): 87-116.
- Alsamarai AGM, Aljumaily ZK (2013) Seroepidemiology of Toxoplasma, Rubella, Cytomegalovirus and Herpes Simplex Virus -2 in Women with Bad Obstetric History. Part-I: Toxoplasma and Rubella Infections. Our Dermatol Online 4(4): 522-535.
- Alsamarai AGM, Aljumaily ZK (2013) Seroepidemiology of Toxoplasma, Rubella, Cytomegalovirus and Herpes Simplex Virus -2 in Women with Bad Obstetric History. Part-II: Cytomegalovirus and Herpes Simplex Virus Infections. Our Dermatol Online 4(4): 536-544.
- Mohamed MHH, Abdulghani MA, Ferah GA, Aobaidi AH, Khalil MA (2016) Rubella seroprevalence in women with bad obstetric history. JOJ Immuno Virology 1(2): 555560.
- Aljumaili ZKM, Alsamarai AGM, Najem WS (2014) Cytomegalovirus seroprevalence in women with bad obstetric history in Kirkuk, Iraq. J Infection Public Health 7(4): 277-288.
- Aljumaili ZKM, Alsamarai AGM, Najem WS (2014) Rubella seroprevalence in women with bad obstetric history. Research Review Bioscience 8(6): 203-213.
- Hassan HMM, Alsamarai AGM, Aljumaili ZKM, Alsalihi FG (2014) Association between Herpes Simplex virus type 2 (HSV-2) and bad obstetric outcomes. Our Dermatol On line 5(1): 19-28.
- Aljumaily ZK, Alsamarai AGM, Najem WS (2013) Seroprevalence of herpes simplex type 2 (HSV-2) in women with bad obstetric history. Am J Derm Vener 2(3): 31-38.
- Hassan HM, Alsamarai AGM, Aljumaili ZK, Alobaidi AH, Alsalihi FG (2014) Association between cytomegalovirus infection and bad obstetric history in women from Kirkuk. Int J Public Health Sci 3(1): 29-42.
- Aljumaily ZK, Alsamarai AGM, Najem WS (2013) Seroepidemiology of toxoplasma, rubella, cytomegalovirus, and herpes simplex in women with bad obstetric history. Middle East J Intern Med 6(6): 21-33.
- Alsamarai AGM, Hassan HMM, Alsalihi FG, Alobaidi AH, Aljumaily ZK (2014) Toxoplasma gondii, Rubella and Cytomegalovirus coiunfections as a risk factors for abnormal pregnancy outcomes. Middle East J Fam Med 12(3): 16-23.
- Aljumaily ZKM, Alsamarai AGM (2013) Risk factors for bad obstetric history in Kirkuk women, Iraq. Int J Infect Microbiol 2(3): 70-77.
- Aljumaili ZKM, Alsamarai AGM, Najem WS (2014) Toxoplasma gondii seroprevalence in women with bad obstetric history. MEJIM 7(1): 32.
- Abdulghani MA, Hala MM, Amina HA (2016) Autoantibodies in Women with Bad Obstetric History. J Imm Cell Microbiology 1: 9-18.
- Alsamarai AGM, Majed HM, Alobaidi AH (2016) Interleukin-6 [IL-6], Interleukin-17 [IL-17] and Angiopoietin in Women with Bad Obstetric History, Kirkuk, Iraq. Am Res J Haematol 1: 1-11.
- Ferráez LC, Ade ACM, Martínez JRC, Talavera GA, Mdel RGL (2013) Human papillomavirus infection and spontaneous abortion: a casecontrol study performed in Mexico. Eur J Obstet Gynecol Reprod Biol 170(2): 468-473.
- Clifford GM, Gallus S, Herrero R, Muñoz N, Snijders PJ (2005) Worldwide distribution of human papillomavirus types in cytologically normal women in the International Agency for Research on Cancer HPV prevalence surveys: a pooled analysis. Lancet 366(9490): 991-998.
- Bakhshandeh NSMA, Beshart S (2011) Molecular epidemololgy of high -Risk Types ofhuman Papilloma Viruses (16,18) in Pap Smear, The North East of Iran. Iran J Cancer Prev 4(3): 135-140.
- Mona SE, Mohamed NGR, Nesrine FH, Orief YI, Sabaa BME (2013) Egypt,Acytololgical and Molecular study. Middle East FertilitySocietyJournal 8(4): 253-267.
- Bahia B, Sanae B, Chakib N, Honcine O, Moulay AM, et al. (2012) Correlates of high risk HPV:across-section study in women with normal cytololgy in north-centeral Morocco. J Infect Dev Ctries 96(7): 543-550.
- Chan PKS, Chang AR, Cheung JLK, Xu LY, Nelson LS Tang, et al. (2002) Determinants of Cervical Humen Papilloma infection: Differences between high- and Low-Oncogenic risk types. J Infect Dis 185(1): 28- 35.
- Rong S, Chen W, Wu L, Zhang X, Shen G (2002) Anlysis of risk facter cencer in Xiangy uan Country, Shanxi provine. Zhonghua Yu Fang Yi Xue Za Zhi 36(1): 41-43.
- Alsbeih G, Al-Harbi N, El-Sebaie M, Al-Badawi I (2013) HPV Prevalence and genetic to Cervical cancer in Saudia Arabia. Bio Med Centeral 8: 15.
- Pereira CR, Rosa ML, Vasconcelos GA, Faria PC, Cavalcanti SM (2013) Human Papilloma infection Prevalence and Predictors for Cervical cancer among high risk wonen from Rio de Janerio, Brazil. Int Gynecol Cancer 17(3): 651-660.
- Silva KC, Rosa ML, Moyse N, Afonso LA, Oliveira LH (2009) Risk factors associated with human papiulloma infection from Rio de Janero, Brazil Mem Inst Oswaldo Cruz 104(6): 74-76.
- Piras F, Piga M, Montis AD, Zannou AR, Minerba L, et al. (2011) Prevalence of human Papilloma virus infection in women in Bennin, West Africa. Virol J 8: 514-520.
- Mortazzavi SH, Zali MR, Raoufi M, Nadji M, Nowroozi A (2002) Thr prevalence of HPV in cervical cancer in Iran. Asian Pac J Cancer Prev 3: 69-72.
- Sharbatdaran M, Siadati S, Zeinalzadeh M, Shafaei S, Basirat Z, et al. (2013) The frequency of HPV 16/18 in cervical discharge by PCR in women with abnormal Pap smear or biopsy. Iranian J Pathol 8(1): 17- 20.
- Ambuhl LMM, Baandrup U, Dypkaer K, Blaakaer J, Uldbejerg N, et al. (2016) Human Papillomavirus infection as a possible cause of spontaneous abortion and spontaneous preterm delivery. Infec Dis Obstet Gynecol 19.
- Cho G, Min KJ, Hong HR, Kim S, Hong JH, et al. (2013) High risk human papillomavirus infection is associated with preterm rupture of membranes. BMC Pregnancy Childbirth 13: 173.
- de Sanjosé S, Diaz M, Castellsagué X, Clifford G, Bruni L, et al. Worldwide prevalence and genotype distribution of cervical human Papillomavirus DNA in women with normal cytology: a meta analysis . Lancet Infect Dis 7(7): 453-459.
- Salcedo SM, Damin APS, Agnes G, Pessini S, Beitune PE, et al. (2015) Prevalence of human papillomavirus infection in pregnant versus nonpregnant women in Brazil. Arch Gynecol Obstet 292(2): 1273-1278.
- Liu P, Xu L, Sun Y, Wang Z (2014) The prevalence and risk of human papillomavirus infection in a pregnant women. Epidemiol Infect 142(8): 1567-1578.
- Smith EM, Johnson SR, Jiang D, Zaleski S, Lynch CF, et al. (1991) The association between pregnancy and human papilloma virus prevalence. Cancer Detect Prev 15(5): 397-402.
- Nobbenhuis MAE, Helmerhorst TJM, Brule AJC, Rozendaal L, Bezemer PD, et al. (2002) High-risk human papillomavirus clearance in pregnant women: trends for lower clearance during pregnancy with a catch-up postpartum. Br J Cancer 87(1): 75-80.
- Hong Y, Li SQ, Hu YL, Wang ZQ (2013) Survey of human papillomavirus types and their vertical transmission in pregnant women. BMC Infect Dis 13: 109.
- Zhang Y, Li Y, Gao Z (2009) HR-HPV Infection in Pregnant or Postpartum Women. Chin J Nosocomiol 11(10): 1199-1201.
- Lee SM, Park JS, Norwitz ER, Koo JN, Oh IH, et al. (2013) Risk of vertical transmission of Human Papillomavirus throughout pregnancy: a prospective study. PLoS ONE 8(6): e66368.
- Vincenzo RD, Conte C, Ricci C, Scambia G, Capelli G (2014) Long-term efficacy and safety of human papillomavirus vaccination. Int J Womens Health 6: 999-1010.






























