Seroprevalence of Hepatitis C Virus in Iraqi Population
Abdulghani Mohamed Alsamarai1*, Gailan Abdulrazaq2 and Amina Hamed Alobaidi3
1Tikrit University College of Medicine, Iraq
2College of Science. Tikrit University.
2College of Science. Tikrit University.
3College of Veterinary Medicine. Kirkuk University
Submission: October 14, 2016; Published: December 13, 2016
*Corresponding author: Abdulghani Mohamed Alsamarai, Tikrit University College of Medicine, Tikrit, Iraq, E-mail:galsamarrai@yahoo.com
How to cite this article: Abdulghani M A, Gailan A, Amina H A. Seroprevalence of Hepatitis C Virus in Iraqi Population. JOJ Immuno Virology.2016;1(3):555565. DOI: 10.19080/JOJIV.2016.01.555565
Abstract
Background: Hepatitis C is a major public health problem worldwide. In Eastern Mediterranean Region, two third of liver cirrhosis and HCC were attributed to HCV infections.
Aim of the Study: To determine the seroepidemiology of hepatitis C viral infections in Samara community.
Settings: Samara General Hospital and primary health care centers in Samara District.
Study Design: The study design of two parts, the first one is a retrospective study and the second part is a Descriptive Case Control Study.
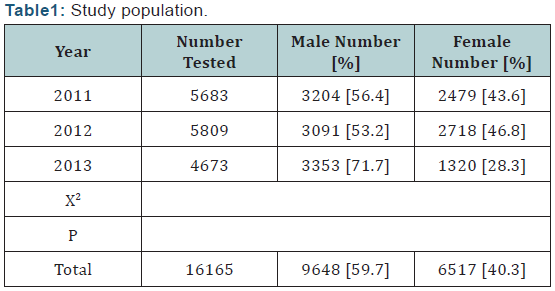
Study Population: The study conducted in Samara General Hospital and primary health care centers in Samara District. Records of subjects with hepatitis C during three years (2011, 2012 and 2013) were included in the study. Their age range from 1 to 59 years, with a mean age of 26.7 ± 4.9 years. The total number of tested serum samples was 16165, of them 5683 for 2011, 5809 for 2012 and 4673 for 2013. Of the total 9648 (60%) are male and 6517 (40%) are female.
Results: The overall Anti-HCV Ab Seroprevalence was 0.54% (87/16165) and the highest Seroprevalence was for 2013 which form 0.81% (38/4673), followed by 0.64% (37/5809) for 2012 and 0.21% for 2011. There was a highly significant (P=0.000) differences in Seroprevalence of Anti-HCV Ab between the three years of study. Anti-HC Ab Seroprevalence was significantly (P=0.009) higher in female (0.72%) as compared to male (0.41%), with male to female ration of 0.57:1.
Conclusions: The impact of HCV on health and medical care in Iraq is a major problem for the community and infectious disease physicians as this study illustrate evolving of new epidemiological characteristics.
Keywords:Hepatitis; HCV; HCC; Seroepidemiology; Samara
Introduction
Chronic hepatitis C prevalence was 3% in the global population [1] and 14% to 45% of the untreated cases of HCV infection develop chronic liver diseases and cirrhosis 20 years after acquisition of disease [2]. In Eastern Mediterranean Region, the prevalence of hepatitis C virus was variable and range from 1% to 2.5% in most countries, with a high prevalence reported in Egypt (>10%) [1], and in Libya, Sudan and Yemen (2.5% - 10%) [3]. Worldwide the HCV prevalence was with a range of 0.4% in Germany to 22% in Egypt [3]. However, the range of HCV prevalence in 21 regions was 1.2% in Tropical Latin America to 3.8% in Central Asia, with overall mean prevalence of 2.8% [3]. HCV prevalence was with a range of 0.32% to 7.1% in Iraqi general population [4,5]. However, most of the reported studies for Iraq are performed on selected study population [6]. To our knowledge, no data was reported concerning Samara city and thus we conducted this study to determine the seroepidemiology of hepatitis C viral infections in Samara community.
Materials and Methods
Settings
Samara General Hospital and primary health care centers in Samara District.
Study design
Retrospective study
Study population
The study conducted in Samara General Hospital and primary health care centers in Samara District. Records of subjects with hepatitis C viral infections during three years (2011, 2012 and 2013) were included in the study. Their age range from 1 to 59 years, with a mean age of 26.7 ± 4.9 years. The total number of tested serum samples was 16165, of them 5683 for 2011, 5809 for 2012 and 4673 for 2013. Of the total 9648 (60%) are male and 6517 (40%) are female. Table1. All the serum samples was tested for HBsAg, using commercially- available (ELISA) kits. The results read by a Micro well reader and compared in a parallel manner with controls; optical density read at 450 nm on an ELISA reader.
Results
Prevalence of Hepatitis C virus
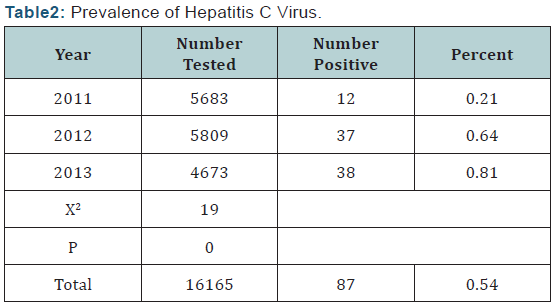
The overall Anti-HCV Ab seroprevalence was 0.54% (87/16165) and the highest seroprevalence was for 2013 which form 0.81% (38/4673), followed by 0.64% (37/5809) for 2012 and 0.21% (12/5683) for 2011. There was a highly significant (X2 =19, P=0.000) differences in seroprevalences of Anti-HCV Ab between the three years of study, (Table 2).
Gender influence on prevalence of Hepatitis C virus
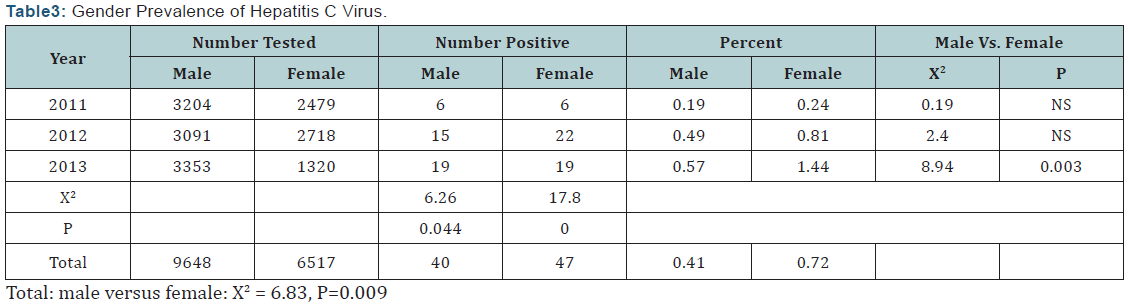
The Seroprevalence of Anti-HC Ab was not significantly different in female as compared to male for 2011 (X2 =0.19, P>0.05) and 2012 (X2 =2.4, P>0.05). However, Anti-HC Ab Seroprevalence was significantly (X2 =8.94, P=0.003) higher in female (1.44%) as compared to male (0.57%) for 2013. When the data of the 3 years pooled together, the Anti-HC Ab Seroprevalence was significantly (X2 =6.83, P=0.009) higher in female (47/6517; 0.72%) as compared to male (40/9648; 0.41%), with male to female ration of 0.57:1 (Table 3).
Age distribution of Hepatitis C virus
The overall Seroprevalence of Anti-HC Ab was significantly ((X2 =35.5, P=0.000) different between age groups, with higher prevalence (1.62%, 23/1421) in the age group >45 years, followed by age group of 1-4 years (1.22%, 3/246). In addition, for 2013, Anti-HC Ab Seroprevalence was significantly (X2 =37.6, P=0.000) different between the age groups, with higher prevalence in age group >45 years (3.46%, 12/347), followed by age group of 1-4 years (2.8%, 2/72). Furthermore, there was significant (X2 =9, P=0.029) difference for Anti-HC antibody Seroprevalence in age group of >45 years (1.62%,8/495), followed by age group of 1-4 years (1.25%,1/80) for 2012. However, in 2011, there was no significant (X2 =4.05, P>0.05) differences between the age groups, (Table 4).
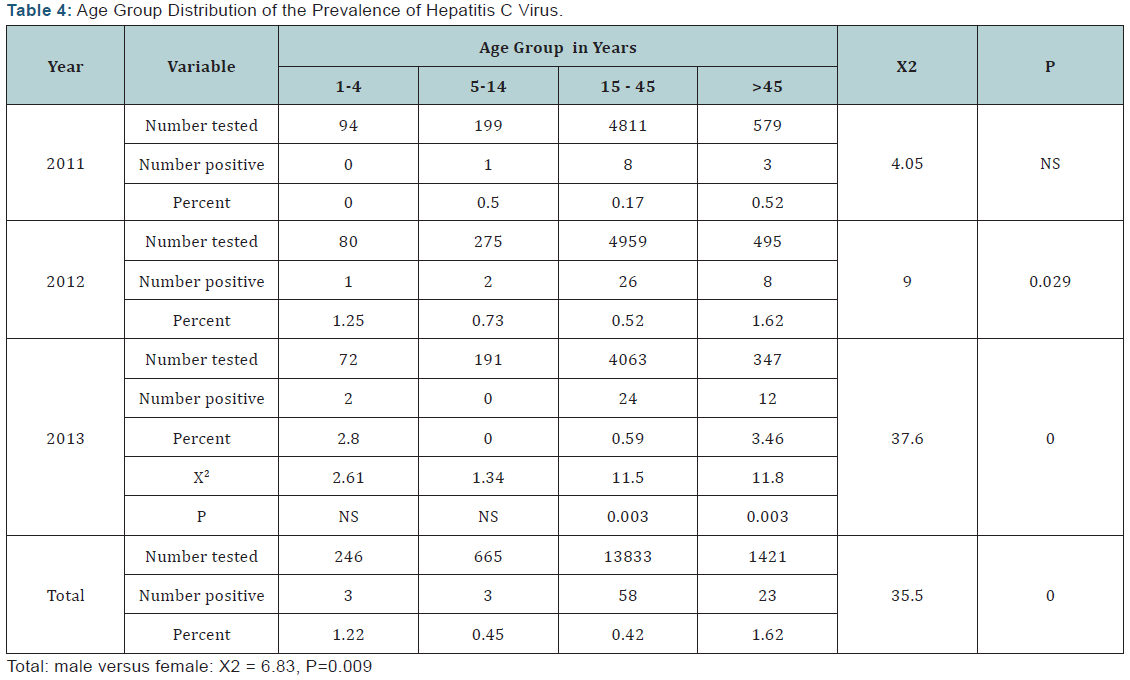
In the age group of 1-4 years there was no significant (X2 =2.61, P>0.05) differences in anti-hepatitis C virus antibody over the study years. In addition, the same pattern was demonstrated for the age group of 5-14 years. However, there was a significant difference in Anti-HC Ab between the study years in both age groups of 15-45 ((X2 =11.5, P=0.003) and >45 years (X2 =11.8, P=0.003), (Table 4).
Age group distribution of the prevalence of Hepatitis C virus in relation to gender
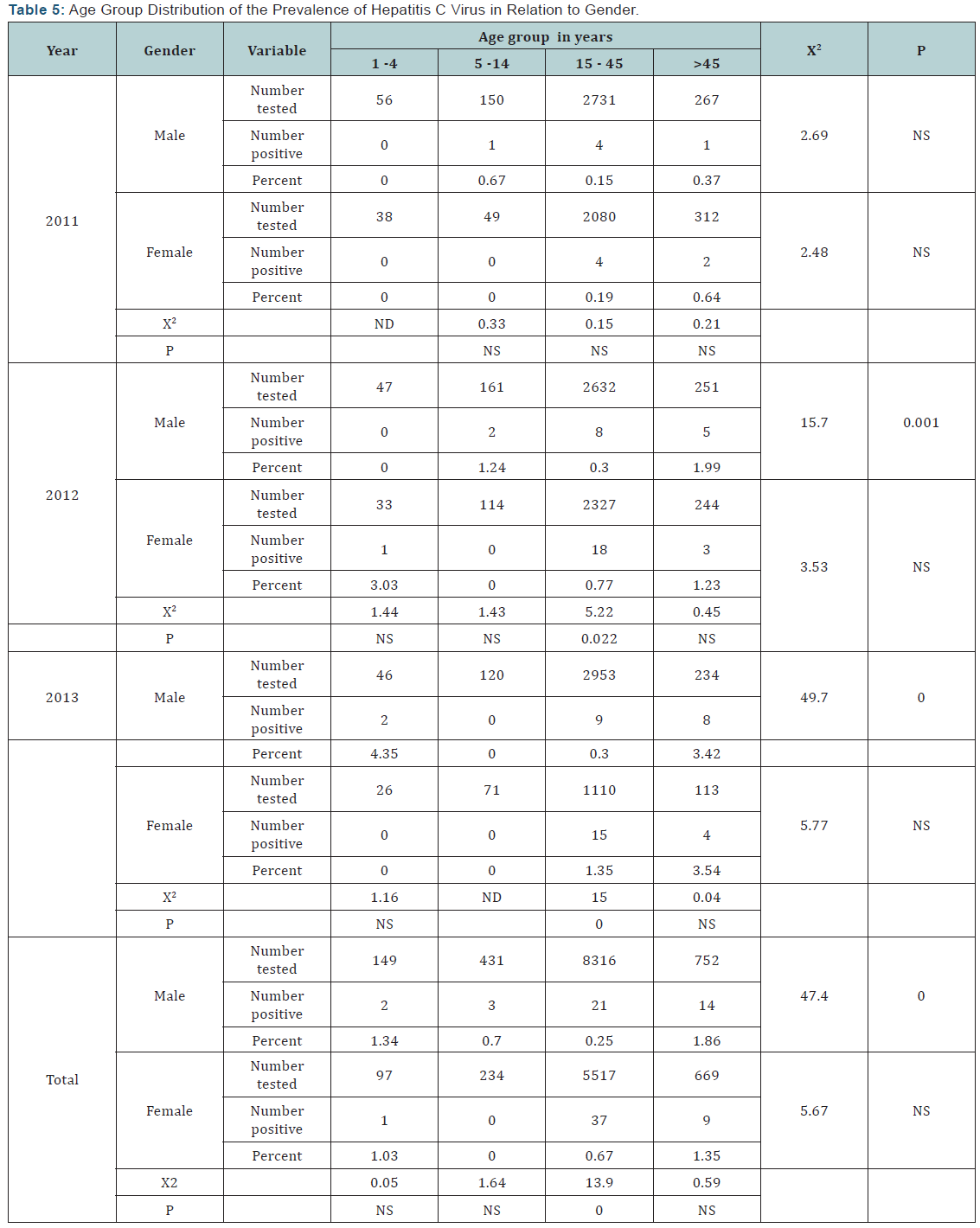
The age distribution of Anti-HC Ab is shown in Table 5. There was no significant differences in HCV antibody Seroprevalence between age groups in both male (X2 =2.69, P>0.05) and female (X2 =2.48, P>0.05) for the year 2011. However, in male individuals the higher HCV Seroprevalence (0.67%, 1/150) was in age group of 5-14 years, while in female (0.64%, 2/312) was in the >45 years age group. There were no significant differences in Seroprevalence of HCV within each age group between male and d female.
Regarding 2012, in male subjects there was a significant difference (X2= 15.7, P= 0.001) in HCV Seroprevalence between age groups, with a higher prevalence (1.99%, 5/251) in >45 years age group. However, in female there was no significant (X2 =3.53, P>0.05) difference in HCV Seroprevalence between the age groups, with a higher. Prevalence (3.03%, 1/33) in 1-4 years age group. Comparison between Seroprevalence between male and female within each age group indicated a significant (X2 =5.22, P=0.022) difference in age group 15-45 years only.
In male individuals, there was a highly significant (X2 =49.7, P=0.000) differences in HCV Seroprevalence between age groups, with a higher prevalence in the age of 1-4 years (4.35;2/46), followed by >45 years (3.42%; 8/234) age group. However, in female, there was no significant differences in HCV Seroprevalence between age groups, with a high prevalence (3.54%, 4/113) in >45 years age group. Male to female comparison. Within each age group demonstrated a significant (X2 =15, P=0.000) difference in 15-45 years age group.
When the data of the 3 years pooled together, the HCV Seroprevalence was significantly different between the age groups for male (X2 =47.4, P=0.000), but not female (X2 =5.67, P=0.000). In both male (1.86%,`4/752) and female (1.35%, 9/669) subjects, the higher HCV Seroprevalence was found in the >45 years age group. Within each age group, the comparison between male and female shows a significant (X2 =13.9, P=0.000) difference in HCV Seroprevalence in the 15-45 years age group, with a higher predominance in female (0.67%, 37/5517) than in male (0.25%; 21/8316).
Discussion
The present study indicated that HCV (Anti-HCV) prevalence was 0.54%, which was significantly higher (X2 =19, P=0.000) in 2013 (0.8%) as compared to 2012 (0.64%) and 2011 (0.21%). This Seroprevalence was about twice to that reported in blood donors (0.26%) in Baghdad [7], but slightly higher to that reported in a national normal population (0.4%) study [6]. The prevalence rate of Anti HCV was lowest in Erbil, Sulaymaniyah, Karbala, Al Qadisiyah, Al Muthanna, Al Basrah and Dahuk (<0.3%) and highest in Babylon, Al Najaf and Thi Qar (> 0.9%) [6].
The present study demonstrated an increase in anti-HCV with time which agreed to previously reported study in blood donors [7]. In Babylon, a higher anti-HCV was found in Iraqi patients with inherited blood disorders who received multiple blood transfusion [8], while it was 0.32% in general population, 0.17% in healthy blood donors, 0.8% in high risk groups [4]. Tawfeq, et al. [9] reported lower HBV prevalence in blood donors who reported 0.29% prevalence in Babylon. Al-Kubaisy, et al [10] found a very high prevalence of HCV infection among children with Thalassemia in Baghdad (67.3%). In contrast, Omer, et al. [11] reported low rate of hepatitis C infection among patients with leukemia who receive multiple blood transfusion in Baghdad.
Recent review reported significant differences in prevalence and epidemiology of hepatitis C virus infection exist among the Middle East countries or even inside the countries regions [12]. However, most of the included studies in this review were performed in risk group rather than general population. Depending on the available data it may be suggested that HCV transmission in the Eastern Mediterranean Region occurs in health care setting and primarily associated with unsafe injections [1]. Global hepatitis C prevalence are mostly based on hepatitis C virus Seroprevalence studies data [13] and data submitted from different countries and WHO regions [3].
The HCV prevalence was 0.4% in Germany, 0.8% in Canada, 1.1% in France and Australia, 5%- 1.5% in India, 1.5% -2.3% in Japan, 1.8% in USA, 2.1% in Indonesia, 3.2% in China, 4.9% in Pakistan, 2.5-10% in Italy and 18%-22% in Egypt [3]. However, the range of HCV prevalence in 21 regions was 1.2% in Tropical Latin America to 3.8% in Central Asia, with overall mean prevalence of 2.8% [3]. HCV prevalence was with a range of 0.32% to 7.1% in Iraqi general population [4,5]. Mohamed Hanafian, et al. [14] conducted a systematic review to estimated the HCV burden globally and their review included the data from 1990 to 2005 using Global Burden of Diseases that divided the world into 21 regions rather than 6 WHO regions, to achieve epidemiology homogenicity. Their review finds that globally the prevalence of anti-HCV increased from 2.3% to 2.8% between 1990 and 2005. Asia Pacific, Tropical Latin America and North America have low prevalence (<1.5%); Central and East Asia and North Africa/ Middle East are with high prevalence (>3.5%); whereas South and Southeast Asia, sub-Saharan Africa, Andean, Central and Southern Latin America, Caribbean, Oceania, Australasia, and Central, Eastern and Western Europe have moderate prevalence (1.5%-3.5%).
The present study HCV Seroprevalence was lower to that reported for Babylon but higher to that reported for general population national survey and in Baghdad in general population [4-6]. In addition, our study Seroprevalence was higher to that reported for Germany, similar to that of Canada, but lower to that reported for India, Japan, USA, Indonesia, China, Pakistan, Italy, and Egypt [3]. Furthermore, the present study HCV prevalence was lower to that reported for 21 regions [14].
In the Middle East countries, HCV prevalence was 0.2% in general population (<1%) [15], 0.12%-1.3% in blood donors, 10.6% -63.8% in patients with thalassemia [16,17], 24.8% in haemodialysis patients [15] in Iran. Among Bahrani, the HCV prevalence range was 9.24% in hemodialysis patients to 40% in those with haemolytic anaemia [18]. In Oman, HCV prevalence was 0%-1% in general population, 0.9%-1.5% in blood donors, 13.4% in kidney transplant patients and 26.5% in hemodialysis patients [19]. In Qatar, HCV prevalence was 6.3% in general population, and 44.6% in patients with dialysis [20,21]. In Jordan, the Seroprevalence in general population was 0.65% to 6.25%, 40% in multi-transfusion hereditary hemolytic anaemia, and 28% in hemodialysis patients [21]. In Kuwait, anti HCV was from 0.8% to 5.4% in blood donors [22].
In Saudi Arabia, the prevalence of HCV infection was low in general population, less in children than adults and intravenous drug use are the main modes of infections [23,24]. HCV prevalence was with 18% to 46% in patients with regular hemodialysis [25]. Anti-HCV detected in 41% of individuals screened recipients for preparation of renal transplantation [26]. In United Arab Emirates was reduced from 23% reported in 1995 [27] to 1.8% as reported in 2009 [1]. Anti-HCV was 0.46% among blood donors from Northern Cyprus, soldiers from Turkey and soldiers from Northern Cyprus [28]. In Syria, anti-HCV prevalence was 48.9% among hemodialysis patients [29], 60.5% among intravenous drug abusers, 1.96% among the prostitutes, and 0.95% among blood donors, [30], 3% among health care workers and 1% in the general population [30].
Ani-HCV was o.4% in health care workers and 0.6% in Lebanon [31] and higher in hemodialysis patients [32]. In Yemen, the anti-HCV was 1.7% in healthy population, 2.7 among blood donors, and 33.75 in patients with chronic liver diseases and in 33.8% in patients with regular hemodialysis [33]. In Turkey, anti- HCV was found in 1% to 2.1% in healthy individuals, and 4.5% in hemolytic anaemia [34,35]. In Sudan, anti-HCV prevalence was 2.2% to 3% in general population and 23.7% in hemodialysis patients [36,37].
In Egypt, the Seroprevalence of HCV in blood donors was 14.5%, 70.4% in hemodialysis patients, 7.7% in health care workers and 75.7% in children with thallasemia [38]. In addition, HCV prevalence was 12.1% of rural primary school children, 18.1 % of rural village residents, 22.1% of army recruits, 16.4% in children with hepatomegaly, 46.2% of hemodialysis adults, 47.2% in adults with hepatoma or chronic liver diseases, and 54.9% of multi-transfused children [39]. In Algeria, HCV antibodies found in 0.18% among blood donors and 0.19% of pregnant women [40].
Although the above summarized studies indicated varied prevalence of HCV, a newly reported review suggests a narrow prevalence scale [1]. The estimated anti-HCV prevalence in the Middle East Regions was with a range of 0.6%in Djibouti to 13.5% in Egypt; however, it was 3.21% in Iraq. In addition, it was 1-0.7% for Lebanon; 1-2% for Syria, Iran, Qatar, Yemen, Oman, Somalia, Libya, Bahrain, Kuwait, Saudi Arabia, Emirates; >2% -3% for Jordan, Sudan, Afghanistan, Morocco; and 4.9% for Pakistan [1]. Thus the present study HCV prevalence was lower (0.54%) to that reported by WHO regional office for Iraq and even less than the lower prevalence estimates (0.6%) for Djibouti.
Recent review [41] reported a summary of data extracted from 21 studies (from 1994 -2009) reporting prevalence of maternal HCV infection indicated a prevalence range from 0.04% in Pakistan [42] to 15.8% in India. In addition, 8 (38.1%) studies reported prevalence of HCV <1%, and 7 (33.3%) studies reporting prevalence of >2%. Furthermore, 5 studies performed in the last 5 years which indicated HCV prevalence of 0.15% to 1.4%, with exception of that performed in Egypt [43] was with 15.7% prevalence [41]. Gasim, et al. [44] in a regional review in Arab and African countries reported HCV prevalence for Arab countries ranged from 0.5% in Tunisia to 8.6% in Egypt. In addition, they reported HCV prevalence for African countries ranged from 1% in Ivory Coast to 16.5% in Malawi. In a systematic review [45], the epidemiology of HCV in Egypt, suggest that a massive hepatitis C virus epidemic at the national level must have occurred with substantial transmission still ongoing today. Overall hepatitis C virus prevalence was 5%-15% among pregnant women, 5% - 25% among blood donors, 10%- 55% among multi-transfused patients, 50%- 90% in dialysis patients, and 0% - 40% among general population. Recent review [46] concerning HCV prevalence which included the articles published after 1995, indicated that HCV prevalence in the general population in Africa was 0.1% to 17.5% depending on the country. Highest prevalence was found in Egypt (17.5%), Cameroon (13.8%) and Burundi (11.3%), while the lowest prevalence reported for Zambia , Kenya, Malawi and south Africa. Anwar, et al [47] using PCR for 4246 blood samples from general population found that 4.9% of the subjects were confirmed to harbor active hepatitis C virus infection. In a survey performed in Canada from 2007 t0 2011 as a nationally representative sample indicated that HCV seroprevalence was 0.5% [48]. A systematic review for Europe suggest that anti-HCV prevalence in general population ranged from 0.4% to 5.2% and varied widely between European countries and within the same country [49]. For example, 10 studies reviewed for Italy, and the anti-HCV ranged from 2.4% to 22.4%, in addition, one study performed at 2006 with a prevalence of 16.3% in community [50]. Flichman, et al. [51] retrospective study carried out in blood donors in Argentine for the period from 2004 to 2011 found that anti- HCV was reduced from 0.71% in 2004 to 0.46% in 2011. Ethnic disparities persist with regards to the prevalence of hepatitis C in the Central California Valley and the reported prevalence may be underestimating because the study population enrolled only healthy volunteers [52]. HCV high prevalence was found in Native American (2.8%), followed by Caucasians (0.59%), Hispanics (0.45%), African Americans (0.38%) and Asians (0.2%). The overall prevalence of HCV is on the decline, but the isolated pockets of very high prevalence in different districts within the same country (for e.g. Italy, Punjab, Iraq…) pose a serious health care problem [53]. The reported studies indicated that HCV Seroprevalence decreased over time [7,5,1], our study demonstrated an increase in anti-HCV in 2013 as compared to 2012 and 2011. This illustrates such increased pockets in Iraq, which represent a serious health impact and thus a regional and national survey is warranted. In a Polish nationwide survey anti- HCV detected in 2.93% in an elderly population [54].
The Seroprevalence of Anti-HC Ab was not significantly in female as compared to male for 2011 and 2012. However, Anti-HC Ab Seroprevalence was significantly (X2 =8.94, P=0.003) higher in female (1.44%) as compared to male (0.57%). When the data of the 3 years pooled together, the Anti-HC Ab Seroprevalence was significantly (X2 =6.83, P=0.009) higher in female (0.72%) as compared to male (0.41%), with male to female ratio of 0.57:1, however, Attalla, et al. [6] found higher prevalence of Anti-HCV in male (0.5%) than in female (0.3%) but the difference was not statistically significant in national population. The present study findings not agreed to that reported by others in Iran [55], Pakistan in blood donors, India in outpatients clinic visitors [56] and USA blood donors [52] as the prevalence was higher in male than female. In Egypt, higher HCV prevalence was detected in males compared to females among village residents [57] and blood donors [58]. In Pakistan, although the probability trends were slightly higher in males of all age groups than in females, the differences not statistically significant [47,59,60]. In a nationwide survey in Poland did not indicate a significant effect of gender on HCV prevalence [54].
The overall Seroprevalence of Anti-HC Ab was significantly (X2 =35.5, P=0.000) different between age groups, with higher prevalence (1.62%) in the age group >45 years, followed by age group of 1-4 years (1.22%). In addition, the same patterns were demonstrated for 2013 and 2012 but not 2011. Furthermore, there was a significant difference in Anti-HC Ab between the study years in both age groups of 15-45 and >45 years. Thus our results indicated that HCV Seroprevalence peak in 1-4 years (1.22%) then decline and peak again in >45 years (1.62%). In the national population survey, anti-HCV Seroprevalence was 0.3% in age 0f 1-10 years and increased gradually with age to pear at of >40 years [6]. Shakeri, et al. [55] from Iran found that HCV prevalence was higher in those with age of 50 – 59 years; however, the mean age of their population study was 39 years. Prevalence of HCV peak at 55-64 in Central, East and Southern sub-Saharan Africa; Americas; Eastern Mediterranean; Asia; and Eastern, and Western, Europe; however, West sub-Saharan African the curve have two peaks, 1st at 15-19 years and 2nd at 55- 64 years. In Western Pacific the pattern of Seroprevalence across age in Australasia exhibit a rapid increase in prevalence peaking 1st at 20-24 years and later in 55-64 years age. In addition, in Central Europe an early peak in ages 1-4 years is seen in Central Europe [14].
In a review for 2009 to 2011 in Canada reported that HCV Seroprevalence was higher in age of 50 to 79 as compared 14 to 49 years Rotermann, et al. [48]. In Egypt, the HCV prevalence increased dramatically with age with the highest rates observed among populations aged >40 years [45]. HCV prevalence of 4% to 7% was reported among Egyptian children from rural school children and attending outpatients clinics [60-62]. In a prospective study, maximum seropositivity of IgM anti HCV was in 10-20 years of age group of suspected cases of hepatitis and in 0-10 years of controls [63].
HCV prevalence was highest in the age group of 20-29and 30 -39 years among general population of Lahore, Pakistan [47]. In contrast to our findings HCV prevalence decreased in individuals with age of >40 years [59,64,65]. However, our study HCV prevalence was agreed to that reported by others [56]. The differences in HCV age related prevalence in different reported studies may be due to influence of the exposure to different risk factors, religious and social behaviors in different communities. For example, in Australasia, the estimated peak prevalence at ages 20-24 years may reflect the high incidence of HCV among persons who use injecting drugs reported recently [66,67].
Mother-to-infant transmission is the commonest route of transmission in children, with a vertical transmission rate of 5% [68]. Thus the higher HCV Seroprevalence in the ages of 1-4 years in our study population may be a reflect of high rate vertical transmission and an indicator of high infection in pregnant women. This finding could ascertain the need for a screening of pregnant women in antenatal period. This screening program is cost-effective, since the cost of HCV case treatment is more expensive [$15000] than performing HCV screening for > 6000 samples [1].
The present study higher HCV Seroprevalence was higher in older age group (>45 years) which it was twice to that reported for general population in Iraq [6], however, it is lower to the mean of the prevalence in North Africa and Middle East [69,3]. Those are in adult age when the HCV screening programs are founded in Iraq (1995), which means they are not included in the screening program and thus with increasing age the prevalence increased due to both vertical and horizontal infections. In addition, during this period Iraq was under economic sanction and after the American occupation of Iraq, the disrupt the health care system. The shortage of materials and equipment for blood screening lead to that blood and blood products given to patients without screening [8]. Furthermore, the possibility of transmission via tattooing, piercing, Hujama, and health care settings due to that these practices conducted by unsafe healthy practices. Sexual transmission also may be implicated as cause that leads to high rate of HCV transmission because of the loss of monitoring program for HCV in prostitutes.
The impact of HCV on health and medical care in Iraq is a major problem for the community and infectious disease physicians as this study illustrate evolving of new epidemiological characteristics. There are insufficient data about HCV prevalence and prevention methods in most of the Iraqi Governorates. In Iraq, information about the prevalence of HCV infections has generally been limited to laboratory data and personal interest of research projects in certain education institutes. There is no national routine surveillance which represents the sound data source in the Iraqi community. To establish public health strategies for Iraq, well-programmed, population based and certain HCV infections at risk survey are needed in Iraqi community. Thus because of such problem, a national screening community based program on the basis of regional and subregional sampling are warranted.
Health care setting need to implement and address primary prevention programs and a grassroots programs and support is an essential in control and prevention of HCV infections in health setting.
References
- WHO (2009) The growing threat of Hepatitis B and C in the Eastern Mediterranean region: a call for action. Regional office for Eastern Mediterranean, Geneva, Switzerland EM/RC56/3.
- WHO. Hepatitis B. 2013.
- WGO. Diagnosis, management and prevention of Hepatitis C. (2013).
- Abbas A, AL-Kiali KK, Hasan AS (2012) Is there any relationship between hepatitis C virus infection and skin diseases. Diyala J Med 3(1): 51-56.
- Khattab OS (2008) Prevalence and risk factors for hepatitis C virus infection in hemodialysis in an Iraq renal transplant center. Saudi J. Kidney Dis Transp 19(1): 110-105.
- Ataallah MT, Akram W, AL-Naaimi AS, Omer AR (2013) Epidemiology of viral hepatitis B and C in Ragi national survey 2005-2006. Zanco J Med Sci 17(1).
- Ataallah TM, Hanan KA, Maysoun KS, Sadoon AA (2011) Prevalence of Hepatitis B and C among blood donors attending the National Blood Transfusion Center in Baghdad from 2006-2009. Saudi Med J 32(10): 1046-1050.
- Alawady NB (2014) Prevalence of Hepatitis C virus infections among Iraqi patients registered to Babylon center for inherited blood disorders. International J. of Advanced Research 2(1): 383-388.
- Tawfeeq WF, Al-Aouadi RA, Al-Yousif AM (2013) Detection of Hepatitis C virus infection and genotypes among seropositive blood donors by polymerase chain reaction in Babylon governorate/Iraq. Medical journal of Babylon 10(1): 25-38.
- Al-Kubaisy WA, Al-Naib KT, Habib MA (2006) Prevalence of HCV/HIV co-infection among hemophilia patients in Baghdad. East Mediator Health J 12(3-4): 264-269.
- Omer AR, Al-Salmani AM (2007) Prevalence of Viral Hepatitis in Iraq. Research between Iraqi MOH (CDC) and WHO (2006-2007).
- Fallahian F, Najafi A (2011) Epidemiology of Hepatitis C in Middle East. Saudi J Kidney Dis Transplant 22(1): 1-9.
- Shepard CW, Finelli L, Alter MJ (2005) Global epidemiology of Hepatitis C virus infection. Lancet Infect Dis 5(9): 558-567.
- Mohd Hanafiah K, Groeger J, Flaxman AD, Wiersm ST (2013) Global epidemiology of Hepatitis C virus infection: new estimates age-specific antibody to HCV seroprevalence. Hepatology 57(4): 1333-1342.
- Shakeri MT, Nomani H, Mobarhan MG, Sima HR, Gerayli S, et al. (2013) The prevalence of Hepatitis C virus in Mashhad, Iran: a populationbased study. Hepatitis Mon 13(3): e7723.
- Tamaddoni A, Mohammadzadeh I, Ziaei O (2007) Seroprevalence of HCV antibody among patients with beta-thalassemia major in Amirkola Thalassemia Center, Iran. Iran J Allergy Asthma Immunol 6(1): 41.
- Alavian SM (2007) Control of Hepatitis C in Iran: vision and missions. Hepat Mon 7(2): 57-58.
- Al-Mahroos FT, Ebrahim A (1995) Prevalence of Hepatitis B, Hepatitis C and human immune deficiency virus markers among patients with hereditary hemolytic anemias. Ann Trop Paediatr 15(2): 121-128.
- Al-Dhahry SH, Aghanashinikar PN, al-Hasani MK, Buhl MR, Daar AS (1993) Prevalence of antibodies to hepatitis C virus among Omani patients with renal disease. Infection 21(3): 164-167.
- Bener A, AL-Kaabi S, Derbala M, AL-Marri A, Rikabi A (2009) The epidemiology of viral hepatitis in Qut. Saudi J Kidney Dis Transpl 20(2): 300-306.
- Al-Jamal M, Al-Qudah A, Al-Shishi KF, Al- Sarayreh A, Al-Quraan L (2009) Hepatitis C virus (HCV) infection in hemodialysis patients in the south of Jordan. Saudi J Kidney Dis Transpl 20(3): 488-492.
- Ameen R, Sanad N, Al-Shemmari S, Siddique I, Chowdhury RI, et al. (2005) Prevalence of viral markers among first-time Arab blood donors in Kuwait. Transfusion 45(12): 1973-1980. 136.">Simons RRL, Gale P, Horigan V, Snary EL, Breed AC (2014) Potential
- Simons RRL, Gale P, Horigan V, Snary EL, Breed AC (2014) Potential for introduction of bat-borne zoonotic viruses into the EU: A review. Viruses 6(5): 2084-2121.
- Bashawri LA (2002) Pattern of blood procurement, ordering and utilization in a University Hospital in Eastern Saudi Arabia. Saudi Med J 23(5): 555-561.
- Karkar A (2007) Hepatitis C in dialysis units: The Saudi experience. Hemodial Int 11(3): 354-367.
- Bernieh B, Mohamed AO, Sirwal IA, Wafa A, Abbade MA, et al. (1999) Viral Hepatitis in renal transplant patients. Saudi J Kidney Dis Transpl 10(2): 157-160.
- El Shahat YI, Varma S, Bari MZ, Shah Nawaz M, Abdulrahman S, et al. (1995) Hepatitis C virus infection among dialysis patients in United Arab Emirates. Saudi J Kidney Dis Transpl 6(2): 157-162.
- Altindis M, Yilmaz S, Dikengil T, Acemoglu H, Hosoglu S (2006) Seroprevalence and genotyping of Hepatitis B, Hepatitis C and HIV among healthy population and Turkish soldiers in Northern Cyprus. World J Gastroenterol 12(42): 6792-6796.
- Othman BM, Monem FS (2001) Prevalence of Hepatitis C virus antibodies among health care workers in Damascus, Syria. Saudi Medical Journal 22(7): 603-605.
- Othman BM, Monem FS (2002) Prevalence of Hepatitis C virus antibodies among intravenous drug abusers and prostitutes in Damascus, Syria. Saudi Medical Journal 23(4): 393-395.
- Irani-Hakime N, Aoun J, Khoury S, Samaha HR, Tamim H, et al. (2001) Seroprevalence of Hepatitis C infection among health care personnel in Beirut, Lebanon. Am J Infect Control 29(1): 20-23.
- Naman RE, Mansour I, Klayme S, Khalil G (1996) Hepatitis C virus in hemodialysis patients and blood donors in Lebanon. J Med Liban 44(1): 4-9.
- Bajubair MA, Elrub AA, Bather G (2008) Hepatic viral infections in Yemen between 2000-2005. Saudi Med J 29(6): 871-874.
- Yildirim B, Barut S, Bulut Y, Yenişehirli G, Ozdemir M, et al. (2009) Seropre- valence of Hepatitis B and C viruses in the pro- vince of Tokat in the Black Sea region of Turkey: A population-based study. Turk J Gastroenterol 20(1): 27-30.
- Akcam FZ, Uskun E, Avsar K, Songur Y (2009) Hepatitis B virus and Hepatitis C virus sero- prevalence in rural areas of the southwestern region of Turkey. Int J Infect Dis 13(2): 274-284.
- Mudawi HM, Smith HM, Rahoud SA, Fletcher IA, Babikir AM, et al. (2007) Epidemiology of HCV infection in Gezira state of central Sudan. J Med Virol 79(4): 383-385.
- El-Amin HH, Osman EM, Mekki MO, Abdelraheem MB, Ismail MO, et al. (2007) Hepatitis C virus infection in hemodialysis patients in Sudan: two centers’ report. Saudi J Kidney Dis Transpl 18(1): 101-106.
- el Gohary A, Hassan A, Nooman Z, Lavanchy D, Mayerat C, et al. (1995) High prevalence of Hepatitis C virus among urban and rural population groups in Egypt. Acta Trop 59(2): 155-161.
- Mohamed MK, Hussein MH, Massoud AA, Rakhaa MM, Shoeir S, et al. (1996) Study of the risk factors for viral Hepatitis C infection among Egyptians applying for work abroad. J Egypt Public Health Assoc 71(1- 2): 113-147.
- Spinella PC, Perkins JG, Grathwohl KW, Repine T, Beekley AC, et al. (2007) Risks associated with fresh whole blood and red blood cell transfusions in a combat support hospital. Crit Care Med 35(11): 2576- 2581.
- Helm JJVD, Prins M, del Amo J, Bucher HC, Chêne G, et al. (2011) The hepatitis C epidemic among HIV-positive MSM: incidence estimates from 1990-2007. AIDS 25(8): 1083-1091.
- Jafri W, Jafri N, Yakoob J, Islam M, Tirmizi SF, et al. (2006) Hepatitis B and C: prevalence and risk fac- tors associated with seropositivity among children in Karachi, Pakistan. BMC Infect Dis 6: 101.
- Shebl FM, El-Kamary SS, Saleh DA, Abdel-Hamid M, Mikhail N, et al. (2009) prospective cohort study of mother to infant infection and clearance of Hepatitis C in rural Egyptian villages. J med viral 81(6): 1024-1031.
- Gasim GI, Murad IA, Adam I (2012) Hepatitis B and C virus infections among pregnant women in Arab and African countries. J Infect Dev Ctries 7(8): 566-578.
- Mohmamoud YM, Mumtaz GR, Riome S, Miller D, Abu-Raddad LJ (2013) The epidemiology of Hepatitis C virus in Egypt: a systematic review and data analysis. BMC Infectious Diseases 13: 288.
- Karoney MJ, Siika AM (2013) Hepatitis C virus (HCV) infection in Africa: a review. Pan African Medical J 14: 44.
- Anwar MI, Rahman M, Hassan MU, Iqbal M (2013) Prevalence of Hepatitis C virus infections among general public of Lahour Pakistan. Virol J 10: 351.
- Rotermann M, Langlois K, Andonov A, Trubnikov M (2013) Seroprevalence of Hepatitis B and C virus infections: results from the 2007-2009 to 2011 Canadian health measures survey. Health Rep 24(11): 3-13.
- Hahne SJM, Veldhuijzen IK, Wiessing L, Lim TA, Salminen, et al. (2013) Infection with Hepatitis B and C virus in Europe: a systematic review of prevalence and cost-effectiveness of screening. BMC infectious Diseases 13: 181.
- Petti S, Divizia M, Donia DD, Arca AS, Tarsitani G, et al. (2006) Analysis of shift of the transmission pattern for Hepatitis C in a community in central Italy. New Microbial 29(3): 207-209.
- Flichman DM, Blejer JL, Livellara BI, Re VE, Bartoli S, et al. (2014) Prevalence and trends to markers of Hepatitis B virus, Hepatitis C virus and human immunodeficiency virus in Argentine blood donors. BMC Infectious Diseases 14: 218.
- Sheikh MY, Atla PR, Ameer A , Sadiq H, Sadler PC (2013) Seroprevalence Hepatitis B and C infections among healthy volunteer blood donors in the central California Valley. Gut and Liver 7(1): 66-73.
- Hafeez-ud-din, Usman RJ (2009) Prevalence of HBV and HCV in young healthy adult males seeking recruitment in Pakistan Rangers (Punjab). Pak J Pathol 20(3): 74-77.
- Hartleb M, Gutkowski K, Zejda JE, Chudek J, Więcek A (2012) Serological prevalence of Hepatitis B virus and C virus infection in the elderly populating: Polish nationwide survey - PolSenior. European Journal of Gastroenterology and Hepatology 24(11): 1288-1295.
- Shakeri MT, Nomani H, Mobarhan MG, Sima HR, Gerayli S. et al. (2013) The prevalence of Hepatitis C virus in Mashhad, Iran: a populationbased study. Hepatitis Mol 13(3): e7723.
- Sood S, Malvankar S (2010) Seroprevalence of Hepatitis B surface antige, antibodies to the Hepatitis C virus, and human immunodeficiency virus in a hospital-based population in Jaipur, Rajasthan. Indian J Community Med 35(1): 165-169.
- Sharaf-Eldin S, Salama K, Eldemedresh S, Hassan HMS, Semsem M (2007) Hepatitis B and C viruses in Egyptian children with malignancy. J Med Sci 7(6): 1003-1008.
- Rushdy O, Moftah F, Zakarya S (2009) Transmitted transfused viral infection among blood donors during years 2006 and 2007 in Suez canal area Egypt. Vax Sang 96: 86-87.
- Ahmad W, Ijaz B, Javed FT, Jahan S, Shahid I, et al. (2010) HCV genotype distribution and possible transmission risks in Lahore, Pakistan. World J Gatroenterol 16(34): 4321-4328.
- El-Raziky MS, El-Hawary M, Esmat G, Abouzied AM, El-Koofy N, et al. (2007) prevalence and risk factors of asymptomatic Hepatitis C virus infection in Egyptian children. World J Gastroenterol 13(12): 1828- 1832.
- Kandil ME, Rasheed MA, Saad NE (2007) Hepatitis C and B viruses among some high risk groups of Egyptian children. J Med Sci 7(8): 1259-1267.
- El-Sherbini A, Mohsen SA, Seleem Z, Ghany AA, Moneib A, et al. (2006) Hepatitis B virus among schoolchildren in an endemic area in Egypt over a decade: impact of hepatitis B vaccine. Am J Infect Control 34(9): 600-602.
- Rajani M, Jais M (2014)Age-wise seroprevalence Hepatitis C virus infection in clinically suspected infectious Hepatitis patients attending a tertiary care hospital in Delhi. International J of Medicine and Public Health. 4(1): 78-81.
- Inamullah M, Idrees M, Ahmad H, Sajid UG, Ali M, et al. (2011) Hepatitis C virus genotypes circulating in district Swat of Khyber Pakhtoonkhaw, Pakitan. Virol J 8: 16.
- Masood Z, Jawaid M, Khan RA, Rehman S (2011) Screening for Hepatitis B and C a routine pre-opertive investagations. Park J Med Sci 21(4): 455-459.
- Maher L, Li J, Jalaludin B, Chant KG, Kaldor JM (2007) Big Hepatitis C incidence in new injecting drug users: a policy failure. Aust N Z J Public Health 31(1): 30-35.
- Iversen J, Wand H, Gonnermann A, Maher L (2010) Gender differences in Hepatitis C antibody prevalence and risk behaviours amongst people who inject drugs in Australia 1998-2008. Int J Drug Policy 21(6): 471-476.
- McIntyre PG, Tosh K, McGuire W (2006) Caesarean section versus vaginal delivery for preventing mother to infant Hepatitis C virus transmission. Cochrane Database Syst Revs (4): CD005546.






























